Genomic Promise for Neurodegenerative Diseases, Dementias, Autism Spectrum, Schizophrenia, and Serious Depression
Reporter and writer: Larry H Bernstein, MD, FCAP
There has been an considerable success in the current state of expanding our knowledge in genomics and therapeutic targets in cancer (although clinical remission targets and relapse are a concern), cardiovascular disease, and infectious disease. Our knowledge of prenatal and perinatal events is still at an early stage. The neurology front is by no means unattended. Here there are two prominent drivers of progress –
- genomic control of cellular apoptosis by ubiquitin pathways, and
- epigenetic investigations,
among a complex sea of sequence-changes. I indicate some of the current status in this. However, as much as we have know, there is an incredible barrier to formulate working models because:
- ligand binding between DNA short-sequences is not predictable over time
- binding between proteins and DNA is still largely unknown
- specific regulatory roles between nucleotide-sequences and histone proeins are still unclear
- the relationship between intracellular as well as extracellular cations and the equilibria between cations and anions in intertitial fluid that bathes the cell and between organelles is virgin territory
Consequently, it is quite an accomplishment to have come as far as we have come, and yet, even with the huge compuational power at our disposal, there is insuficient data to unravel the complexity. This may be especially true in the pathway to understanding of neurological and behavioral disorders.
Broad Map of Brain
John Markoff reports in the Feb 18 front-page of New York Times (Project would construct a broad map of the brain) that the Obama administration envisions a decade-long effort to examine the workings of the human brain and construct a map, comparable to what the Human Genome Project did for genetics. It will be a collaboration between universities, the federal government, private foundations, and teams of scientists (neuro-, nano- and whoever else). The goal is to break through the barrier to understanding the brain’s billions of neurons and gain greater insight into
- perception
- actions
- and consciousness.
Essentially, it holds great promise for understanding
Alzheimer’s disease and Parkinson’s, as well as finding therapies for a variety of mental illnesses. An open-ended question is whether it will also advance artificial intelligence research. It is termed the Brain Activity Map project.
http://NYTimes/broad-map-of-brain/
Schizophrenia Genomics
Scientists Reveal Genomic Explanation for Schizophrenia
July 11, 2011
http://GenWeb.com/Exome Sequences Reveal Role for De Novo Mutations in Schizophrenia/
http://NatureGenetics.com/Exome Sequences Reveal Role for De Novo Mutations in Schizophrenia/
http://SchizophreniaResearch.com/INFS integrates diverse neurological signals that control the development of embryonic stem cell and neural progenitor cells/
Buffalo, NY (Scicast) (GenomeWeb News) –
Two new studies, published in Schizophrenia Research and in Nature Genetics, propose hypotheses in a new mouse model of schizophrenia that demonstrates how gestational brain changes cause behavioural problems later in life.
The first study implicates
A fibroblast growth factor receptor protein, (FGFR1), targets diverse genes implicated in schizophrenia. The research demonstrates how defects in an important neurological pathway in early development
- may be responsible for the onset of schizophrenia later in life.
Individuals with sporadic schizophrenia tend to carry more deleterious genetic changes than found in the general population, according to an exome sequencing study that appeared online in Nature Genetics yesterday. “The occurrence of de novo mutations may in part explain the high worldwide incidence of schizophrenia,” according to co-senior author Guy Rouleau, CHU Sainte-Justine Research Center of University of Montreal.
Researchers from Canada and France did exome sequencing on individuals from 14 parent-child trios, each comprised of an individual with schizophrenia and his or her unaffected parents. In the process, they found
- 15 de novo mutations in coding sequences from eight individuals with the psychiatric condition, including
- four nonsense mutations predicted to abbreviate protein sequences.
“They surmise that [de novo mutations] may account for some of the heritability reported for schizophrenia. Recent exome sequencing studies involving parent-child trios have implicated de novo mutations in other brain-related conditions, including
- autism spectrum disorder and
- mental retardation.
To detect de novo genetic changes specific to schizophrenia, the team compared coding sequences from affected individuals with
- the human reference genome, with
- both of his or her parents, and
- with 26 unrelated control individuals.
Of the 15 de-novo mutations verified by Sager sequencing,
- 11 were missense mutations predicted to alter the amino acid sequence of the resulting protein and
- four were nonsense mutations predicted to truncate it.
Among the genes containing nonsense mutations were the zinc finger protein-coding gene ZNF480, the karyopherin alpha 1 gene KPNA1, the low-density lipoprotein receptor-related gene LRP1, and the ALS-like protein-coding gene ALS2CL.
The 15 mutations were found in coding sequences from eight of the individuals with schizophrenia,
- hinting at a higher de novo mutation rate in individuals with sporadic schizophrenia than is predicted in the population overall.
This difference seems to be specific to exomes, and the researchers noted that
- de novo mutation rates across the entire genome are likely comparable in those with or without schizophrenia.
They conclude that the enrichment of [de novo mutations] within the coding sequence of individuals with schizophrenia may underlie the pathogenesis of many of these individual. Most of the genes identified in this study have not been previously linked to schizophrenia, thereby providing new potential therapeutic targets.
The second study
- identifies the Integrative Nuclear FGFR 1 Signaling (INFS) as a central intersection point for multiple pathways of
- as many as 160 different genes believed to be involved in the disorder.
The lead author Dr. Michal Stachowiakthis (UB School of Medicine and Biomedical Sciences) suggests this is the first model that explains schizophrenia
- from genes
- to development
- to brain structure and
- finally to behaviour .
A key challenge has been that patients with schizophrenia exhibit mutations in different genes. It is possible to have 100 patients with schizophrenia and each one has a different genetic mutation that causes the disorder. The explanation is possibly because INFS integrates diverse neurological signals that control the development of embryonic stem cell and neural progenitor cells, and
- links pathways involving schizophrenia-linked genes.
“INFS functions like the conductor of an orchestra,” explains Stachowiak. “It doesn’t matter which musician is playing the wrong note,
- it brings down the conductor and the whole orchestra.
With INFS, we propose that
- when there is an alteration or mutation in a single schizophrenia-linked gene,
- the INFS system that controls development of the whole brain becomes untuned.
Using embryonic stem cells, Stachowiak and colleagues at UB and other institutions found that
- some of the genes implicated in schizophrenia bind the FGFR1 (fibroblast growth factor receptor) protein,
- which in turn, has a cascading effect on the entire INFS.
“We believe that FGFR1 is the conductor that physically interacts with all genes that affect schizophrenia,” he says. “We think that schizophrenia occurs
- when there is a malfunction in the transition from stem cell to neuron, particularly with dopamine neurons.”
The researchers tested their hypothesis by creating an FGFR1 mutation in mice, which produced the hallmarks of the human disease: altered brain anatomy,
- behavioural impacts and
- overloaded sensory processes.
The researchers would like to devise ways to arrest development of the disease before it presents fully in adolescence or adulthood. The UB work adds to existing evidence that nicotinic agonists, might help improve cognitive function in schizophrenics by acting on the INFS.

childhood-schizophrenia-symptoms (Photo credit: Life Mental Health)

English: Types of point mutations. With examples. (Photo credit: Wikipedia)
Parkinson’s Disease
http:// CMEcorner.com/file:///G:/neurodegenerative_disease/Parkinson’s_disease.htm
PINK1 and Parkin and Parkinson’s Disease
Studies of the familial Parkinson disease-related proteins PINK1 and Parkin have demonstrated that these factors promote the fragmentation and turnover of mitochondria following treatment of cultured cells with mitochondrial depolarizing agents. Whether PINK1 or Parkin influence mitochondrial quality control under normal physiological conditions in dopaminergic neurons, a principal cell type that degenerates in Parkinson disease, remains unclear. To address this matter, we developed a method to purify and characterize neural subtypes of interest from the adult Drosophila brain.
Using this method, we find that dopaminergic neurons from Drosophila parkin mutants accumulate enlarged, depolarized mitochondria, and that genetic perturbations that promote mitochondrial fragmentation and turnover rescue the mitochondrial depolarization and neurodegenerative phenotypes of parkin mutants. In contrast, cholinergic neurons from parkin mutants accumulate enlarged depolarized mitochondria to a lesser extent than dopaminergic neurons, suggesting that a higher rate of mitochondrial damage, or a deficiency in alternative mechanisms to repair or eliminate damaged mitochondria explains the selective vulnerability of dopaminergic neurons in Parkinson disease.
Our study validates key tenets of the model that PINK1 and Parkin promote the fragmentation and turnover of depolarized mitochondria in dopaminergic neurons. Moreover, our neural purification method provides a foundation to further explore the pathogenesis of Parkinson disease, and to address other neurobiological questions requiring the analysis of defined neural cell types.
Burmana JL, Yua S, Poole AC, Decala RB , Pallanck L. Analysis of neural subtypes reveals selective mitochondrial dysfunction in dopaminergic neurons from parkin mutants.
http://Burmana JL, Yua S, Poole AC, Decala RB , Pallanck L. Analysis of neural subtypes reveals selective mitochondrial dysfunction in dopaminergic neurons from parkin mutants./
Autophagy in Parkinson’s Disease.
Parkinson’s disease is a common neurodegenerative disease in the elderly. To explore the specific role of autophagy and the ubiquitin-proteasome pathway in apoptosis,
- a specific proteasome inhibitor and macroautophagy inhibitor and stimulator were selected to investigate
- pheochromocytoma (PC12) cell lines
- transfected with human mutant (A30P) and wildtype (WT) -synuclein.
- The apoptosis ratio was assessed by flow cytometry.
- LC3, heat shock protein 70 (hsp70) and caspase-3 expression in cell culture were determined by Western blot.
- The hallmarks of apoptosis and autophagy were assessed with transmission electron microscopy.
Compared to the control group or the rapamycin (autophagy stimulator) group, the apoptosis ratio in A30P and WT cells was significantly higher after treatment with inhibitors of the proteasome and macroautophagy.
- The results of Western blots for caspase-3 expression were similar to those of flow cytometry;
- hsp70 protein was significantly higher in the proteasome inhibitor group than in control, but
- in the autophagy inhibitor and stimulator groups, hsp70 was similar to control.
These findings show that
- inhibition of the proteasome and autophagy promotes apoptosis, and
- the macroautophagy stimulator rapamycin reduces the apoptosis ratio.
- And inhibiting or stimulating autophagy has less impact on hsp70 than the proteasome pathway.
In conclusion,
- either stimulation or inhibition of macroautophagy, has less impact on hsp70 than on the proteasome pathway.
- rapamycin decreased apoptotic cells in A30P cells independent of caspase-3 activity.
Although several lines of evidence recently demonstrated crosstalk between autophagy and caspase-independent apoptosis, we could not confirm that
- autophagy activation protects cells from caspase-independent cell death.
Undoubtedly, there are multiple connections between the apoptotic and autophagic processes. Inhibition of autophagy may
- subvert the capacity of cells to remove
- damaged organelles or to remove misfolded proteins, which
- would favor apoptosis.
However, proteasome inhibition activated macroautophagy and accelerated apoptosis. A likely explanation is inhibition of the proteasome favors oxidative reactions that trigger apoptosis, presumably through
- a direct effect on mitochondria, and
- the absence of NADPH2 and ATP which may
- deinhibit the activation of caspase-2 or MOMP.
Another possibility is that aggregated proteins induced by proteasome inhibition increase apoptosis.
Yang F, Yanga YP, Maoa CJ, Caoa BY, et al. Role of autophagy and proteasome degradation pathways in apoptosis of PC12 cells overexpressing human -synuclein. Neuroscience Letters 2009; 454:203–208. doi:10.1016/j.neulet.2009.03.027. www.elsevier.com/locate/neulet http://neurosciletters.com/ Role_of_autophagy_and_proteasome_degradation_pathways_in_apoptosis_of_PC12_cells_overexpressing_human –synuclein/
Parkin-dependent Ubiquitination of Endogenous Bax
Autosomal recessive loss-of-function mutations within the PARK2 gene functionally inactivate the E3 ubiquitin ligase parkin, resulting
- in neurodegeneration of catecholaminergic neurons and a familial form of Parkinson disease.
Current evidence suggests both
- a mitochondrial function for parkin and
- a neuroprotective role, which may in fact be interrelated.
The antiapoptotic effects of Parkin have been widely reported, and may involve
fundamental changes in the threshold for apoptotic cytochrome c release, but the substrate(s) involved in Parkin dependent protection had not been identified. This study demonstrates
- the Parkin-dependent ubiquitination of endogenous Bax
- comparing primary cultured neurons from WT and Parkin KO mice and
- using multiple Parkin-overexpressing cell culture systems.
The direct ubiquitination of purified Bax was also observed in vitro following incubation with recombinant parkin.
- Parkin prevented basal and apoptotic stress induced translocation of Bax to the mitochondria.
- an engineered ubiquitination-resistant form of Bax retained its apoptotic function,
- but Bax KO cells complemented with lysine-mutant Bax
- did not manifest the antiapoptotic effects of Parkin that were observed in cells expressing WT Bax.
The conclusion is that Bax is the primary substrate responsible for the antiapoptotic effects of Parkin, and provides mechanistic insight into at least a subset of the mitochondrial effects of Parkin.
Johnson BN, Berger AK, Cortese GP, and LaVoie MJ. The ubiquitin E3 ligase Parkin regulates the proapoptotic function of Bax. PNAS 2012, pp 6. www.pnas.org/cgi/doi/10.1073/pnas.1113248109
http://PNAS.org/ The_ubiquitin_E3_ligase_Parkin_regulates_the_proapoptotic_function_of_Bax


Parkin Promotes Mitochondrial Loss in Autophagy
Parkin, an E3 ubiquitin ligase implicated in Parkinson’s disease,
- promotes degradation of dysfunctional mitochondria by autophagy.
upon translocation to mitochondria, Parkin activates the ubiquitin–proteasome system (UPS) for
- widespread degradation of outer membrane proteins.
We observe
- an increase in K48-linked polyubiquitin on mitochondria,
- recruitment of the 26S proteasome and
- rapid degradation of multiple outer membrane proteins.
The degradation of proteins by the UPS occurs independently of the autophagy pathway, and
- inhibition of the 26S proteasome completely abrogates Parkin-mediated mitophagy in HeLa, SH-SY5Y and mouse cells.
Although the mitofusins Mfn1 and Mfn2 are rapid degradation targets of Parkin, degradation of additional targets is essential for mitophagy.
It appears that remodeling of the mitochondrial outer membrane proteome is important for mitophagy, and reveal
- a causal link between the UPS and autophagy, the major pathways for degradation of intracellular substrates.
Chan NC, Salazar AM, Pham AH, Sweredoski MJ, et al. Broad activation of the ubiquitin–proteasome system by Parkin is critical for mitophagy. Human Molecular Genetics 2011; 20(9): 1726–1737. doi:10.1093/hmg/ddr048. http://HumMolecGenetics.com/ Broad_activation_of_the_ubiquitin–proteasome_system_by_Parkin_is_critical_for_mitophagy/
Autophagy impairment: a crossroad
Nassif M and Hetz C. Autophagy impairment: a crossroad between neurodegeneration and tauopathies. BMC Biology 2012; 10:78. http://www.biomedcentral.com/1741-7007/10/78
http://BMC.com/Biology/Autophagy impairment: a crossroad between neurodegeneration and tauopathies/
http://Molecular Neurodegeneration/Nassif M and Hetz C/
Impairment of protein degradation pathways such as autophagy is emerging as
- a consistent and transversal pathological phenomenon in neurodegenerative diseases, including Alzheimer´s, Huntington´s, and Parkinson´s disease.
Genetic inactivation of autophagy in mice has demonstrated a key role of the pathway in maintaining protein homeostasis in the brain,
- triggering massive neuronal loss and
- the accumulation of abnormal protein inclusions.
This paper in Molecular Neurodegeneration from Abeliovich´s group now suggests a role for
- phosphorylation of Tau and
- the activation of glycogen synthase kinase 3β (GSK3β)
- in driving neurodegeneration in autophagy-deficient neurons.
This study illuminatess the factors driving neurofibrillary tangle formation in Alzheimer´s disease and tauopathies.





images: autophagy, stem cell remodeling, lysosome, exosome, epigenetics,
Alzheimer’s Disease
Alzheimer’s Linked To Rare Gene Mutation That Affects Immune System
Article Date: 15 Nov 2012 –
Two international studies published this week point to a link between Alzheimer’s disease and a rare gene mutation that affects the immune system’s inflammation response. The discovery supports an emerging theory about the role of the immune system in the development of Alzheimer’s disease. Both studies were published online this week in the New England Journal of Medicine, one led by John Hardy of University College London, and the other led by the Iceland-based global company deCode Genetics.
Alzheimer’s is a form of distressing brain-wasting disease that gradually robs people of their memories and their ability to lead independent lives. Its main characteristic is the build up of
- protein tangles and
- plaques inside and between brain cells, which eventually
- disrupts their ability to communicate with each other.
Both teams conclude that a rare mutation in a gene called TREM2, which helps trigger immune system responses, raises the risk for developing Alzheimer’s disease. One study suggests it raises it three-fold, the other, four-fold. The UCL-led study included researchers from 44 institutions around the world and data on a total of 25,000 people.
After homing in on the TREM2 gene using new sequencing techniques, they carried out further sequencing that identified a set of
- rare mutations that occurred more often in 1,092 Alzheimer’s disease patients than in a group of 1,107 healthy controls.
They evaluated the most common mutation, R47H, and confirmed that this variant of TREM2 substantially increases the risk for Alzheimer’s disease. R47H mutation was present in 1.9 percent of the Alzheimer’s patients and in only 0.37 percent of the controls. The researchers on the study led by deCode Genetics indicate that this strong effect is on a par with that of the well-established gene variant known as APOE4. Not all people who have the R47H variant will develop Alzheimer’s and in those who do, other genes and environmental factors will also play a role — but like APOE 4 it does substantially increase risk,” Carrasquillo explains.
The study led by
deCode Genetics involved collaborators from Iceland, Holland, Germany and the US, not only found a strong link between the
R47H variant and Alzheimer’s disease, but the variant also
- predicts poorer cognitive function in older people without Alzheimer’s.
In a statement, lead author Kari Stefánsson, CEO and co-founder of deCODE Genetics says:
The discovery of variant TREM2 is important because
- it confers high risk for Alzheimer’s and
- because the gene’s normal biological function has been shown to reduce immune response
He surmises that the combined factors make TREM2 an attractive target for drug development.
Using deCode’s genome sequencing and genotyping technology, Stefánsson and colleagues identified
- approximately 41 million markers, including 191,777 functional variants, from
- 2,261 Icelandic samples.
They further analyzed these variants against the genomes of
- 3,550 people with Alzheimer’s disease and
- a control group of over-85s who did not have a diagnosis of Alzheimer’s.
This led to them finding the TREM2 variant, and to make sure this was not just a feature of Icelandic people,
- they replicated the findings against other control populations in the United States, Germany, the Netherlands and Norway.
Stefánsson says that the results were enabled by having
- sophisticated research tools,
- access to expanded and high quality genomic data sets, and
- investigators with profound analytic skills,
Researching into genetic causes of disease can, thereby, be carried out using an approach that combines sequence data and biological knowledge to find new drug targets.
R47H Variant of TREM2 and Immune Response
Preclinical studies have found that
- TREM2 is important for clearing away cell debris and amyloid protein, the protein that is associated with the brain plaques
- that are characteristic of Alzheimer’s disease.
The gene helps control the
- inflammation response associated with Alzheimer’s and cognitive decline.
Rosa Rademakers, a co-author in the UCL-led study, runs a lab at the Mayo Clinic in Florida that helped to pinpoint the R47H variant of TREM2. Other studies also link the immune system to Alzheimer’s disease, but
- studies are needed to establish that R47H acts by altering immune function.
EPIGENETICS, HISTONE PROTEINS, AND ALZHEIMER’S DISEASE
12/10/12 · Emily Humphreys
Epigenetic effects were first described by Conrad Waddington in 1942 as phenotypic changes resulting from an organism interacting with its environment.1 Today, epigenetics is
- heritable effects in gene expression that are
- not based on the genetic sequence.
One known epigenetic mechanism includes posttranslational modifications of histones that are
- found in the nuclei of nearly all eukaryotes and
- function to package DNA into nucleosomes.
Histone proteins can be heavily decorated with posttranslational modifications (PTMs), such as
- acetyl-,
- methyl-, and
- phosphoryl- groups at distinct amino acid residues.
These modifications are mainly
- located in the N-terminal tails of the histone and
- protrude from the core nucleosome structure.
Gene regulation, and the downstream epigenetic effects, can also
- depend on the cis or trans orientation of the PTMs.2
One PTM, acetylation, is an important determinant of cell replication, differentiation, and death.3 Zhang, et al. investigated the acetylation of histone proteins in Alzheimer’s disease (AD) pathology found in postmortem human brain tissue compared to neurological controls. To study histone acetylation,
- histones were isolated from frozen temporal lobe samples of patients with advanced AD.
Histones were quantified using Selected-reaction-monitoring (SRM)-based targeted proteomics, an LC-MS/MS-based technique demonstrated by the Zhang lab.4 Histones were also analyzed using western blot analysis and LC-MS/MS-TMT (tandem-mass-tagging) quantitative proteomics. The results of these three experimental strategies agreed, further validating the specificity and sensitivity of the targeted proteomics methods. Histone acetylation was reduced throughout in the AD temporal lobe compared to matched controls.
- the histone H3 K18/K23 acetylation was significantly reduced.
Alzheimer’s disease and aging have also been associated with loss of histone acetylation in mouse model studies.5 In addition, Francis et al. found
- cognitively impaired mice had a 50% reduced H4 acetylation in APP/PS1 mice than wild-type littermates.6
In mice, histone deacetylase inhibitors heve restored histone acetylation and improved memory in mice with age-related impairments or in models for other neurodegenerative diseases.7
Further studies of histone acetylation in AD could lead to target therapies in the disease pathology of neurodegenerative diseases, and
- increase our understanding of how epigenetic mechanisms, such as histone acetylation, alter gene regulation.
References
1. Waddington, C.H., (1942). ‘The epigenotype‘, Endeavour, 1942 (1), (pp. 18-20)
2. Sidoli, S., Cheng, L., and Jensen O.N. (2012) ‘Proteomics in chromatin biology and epigenetics: Elucidation of post-translational modifications of histone proteins by mass spectrometry‘, Journal of Proteomics, 75 (12), (pp. 3419-3433)
3. Zhang. K., et al. (2012) ‘Targeted proteomics for quantification of histone acetylation in Alzheimer’s disease‘, Proteomics, 12 (8), (pp. 1261-1268)
4. Darwanto, A., et al., (2010) ‘A modified “cross-talk” between histone H2B Lys-120 ubiquitination and H3 Lys-K79 methylation‘, The Journal of Biological Chemistry, 285 (28), (pp. 21868-21876)
5. Govindarajan, N., et al. (2011) ‘Sodium butyrate improves memory function in an Alzheimer’s disease model when administered at an advanced stage of disease progression‘, Journal of Alzheimer’s Disease, 26 (1), (pp.187-197)
6. Francis, Y.I., et al., (2009) ‘Dysregulation of histone acetylation in the APP/PS1 mouse model of Alzheimer’s disease‘, Journal of Alzheimer’s Disease, 18 (1), (pp. 131-139)
7. Kilgore, M., et al., (2010) ‘Inhibitors of class 1 histone deacetylases reverse contextual memory deficits in a mouse model of Alzheimer’s disease‘, Neuropsychopharmacology, 35 (4), (pp. 870-880)
Tags: acetylation, alzheimers disease, epigenetics, histone, targeted proteomics
Tau amyloid
An Outcast Among Peers Gains Traction on Alzheimer’s Cure
By JEANNE WHALEN jeanne.whalen@wsj.com
Gareth Phillips for The Wall Street Journal
November 10, 2012, on page A1 in the U.S. edition of The Wall Street Journal
After years of effort, researcher Dr. Claude Wischik is awaiting the results of new clinical trials that will test his theory on the cause of Alzheimer’s.
Dr. Wischik, an Australian in his early 30s in the 1980s, was attempting to answer a riddle: What causes Alzheimer’s disease? He needed to examine brain tissue from Alzheimer’s patients soon after death, which required getting family approvals and enlisting mortuary technicians to extract the brains. He collected more than 300 over about a dozen years.
Alzheimer’s researcher Claude Wischik had a view that a brain protein called tau-not plaque is largely responsible. WSJ’s Shirley Wang spoke with Dr. Wischik about his work on a new drug to treat the devastating disease.
The 63-year-old researcher believes that a protein called tau
- forms twisted fibers known as tangles inside the brain cells of Alzheimer’s patients and is largely responsible for driving the disease.
For 20 years, billions of dollars of pharmaceutical investment has placed chief blame on a different protein, beta amyloid, which
- forms sticky plaques in the brains of sufferers.
A string of experimental drugs designed to attack beta amyloid have failed recently in clinical trials.
Wherefore Tau thy go?
Dr. Wischik, who now lives in Scotland, sees this as tau’s big moment. The company he co-founded 10 years ago, TauRx Pharmaceuticals Ltd., has developed an experimental Alzheimer’s drug that it will begin testing in the coming weeks in two large clinical trials. Other companies are also investing in tau research. Roche Holding bought the rights to a type of experimental tau drug from Switzerland’s closely held AC Immune SA.
Wischik is a scientist who has struggled against a prevailing orthodoxy. In 1854, British doctor John Snow traced a cholera outbreak in London to a contaminated water supply, but his discovery was rejected. A very infamous example is the discovery of the cause of child-bed fever in Rokitanski’s University of Vienna by Ignaz Semmelweis. In 1982, two Australian scientists declared that bacteria (H. pylori) caused peptic ulcers, later to be awarded the 2005 Nobel Prize in medicine for their discovery.
Dr. Wischik says he and other tau-focused scientists have been shouted down over the years by what he calls the “amyloid orthodoxy.” But Dr. Wischik has been hampered by inconclusive research. A small clinical trial of TauRx’s drug in 2008 produced mixed, results. Of course, influential scientists still think that beta amyloid plays a central role. Although Roche is investing in tau, Richard Scheller, head of drug research at Roche’s biotech unit, Genentech, says the company still has a strong interest in beta amyloid (hedging the bet). He thinks amyloid drugs may have better results if testing on Alzheimer’s patients occurs much earlier in the disease to prove effective; Roche recently announced plans to conduct such a trial. Simply put -“Drugs tied to conventional theories on Alzheimer’s causes haven’t so far been effective.” Scientists Dr. Wischik accuses of wrongly fixating on beta amyloid argue that the evidence for pursuing amyloid is strong. One view expressed is that drugs to attack both beta amyloid and tau will be necessary.
Alzheimer’s disease is the leading cause of dementia in the elderly, and according to the World Health Organization, the cost of caring for dementia sufferers totals about $600 billion each year world-wide. The disease was first identified in 1906 by German physician Alois Alzheimer, who found in the brain of a deceased woman who had suffered from dementia the plaques and tangles that riddled the tissue. In the 1960s, Dr. Martin Roth and colleagues showed that
- the degree of clinical dementia was worse for patients with more tangles in the brain.
In the 1980s, Dr. Wischik joined Dr. Roth’s research group at Cambridge University as a Ph.D student, and was quickly assigned the task of
- determining what tangles were made of, which launched his brain-collecting mission, and years of examining tissue.
Finally, in 1988, he and colleagues at Cambridge published a paper demonstrating for the first time that
- the tangles first observed by Alzheimer were made at least in part of the protein tau, which was supported by later research.
Like all of the body’s proteins, tau has a normal, helpful function—working inside neurons to help
- stabilize the fibers that connect nerve cells.
When it misfires, tau clumps together to form harmful tangles that kill brain cells.
Dr. Wischik’s discovery was important news in the Alzheimer’s field:
- identifying the makeup of tangles made it possible to start developing ways to stop their formation. But by the early 1990s, tau was overtaken by another protein: beta amyloid.
Signs of Decline
Several pieces of evidence convinced an influential group of scientists that beta amyloid was the primary cause of Alzheimer’s.
- the discovery of several genetic mutations that all but guaranteed a person would develop a hereditary type of the disease.
- these appeared to increase the production or accumulation of beta amyloid in the brain,
- which led scientists to believe that amyloid deposits were the main cause of the disease.
Athena Neurosciences, a biotech company whose founders included Harvard’s Dr. Selkoe, focused in earnest on developing drugs to attack amyloid. Meanwhile, tau researchers say they found it hard to get research funding or to publish papers in medical journals. It became difficult to have a good publication on tau, because the amyloid cascade was like a dogma. It became the case that if you were not working in the amyloid field you were not working on Alzheimer’s disease. Dr. Wischik and his colleagues fought to keep funding from the UK’s Medical Research Council for the repository of brain tissue they maintained at Cambridge, he says. The brain bank became an important tool. In the early 1990s, Dr. Wischik and his colleagues compared the postmortem brains of Alzheimer’s sufferers against those of people who had died without dementia, to see how their levels of amyloid and tau differed. They found that both healthy brains and Alzheimer’s brains could be filled with amyloid plaque, but only Alzheimer’s brains contained aggregated tau.
- as the levels of aggregated tau in a brain increased, so did the severity of dementia.
In the mid-1990s, Dr. Wischik discovered that
- a drug sometimes used to treat psychosis dissolved tangles
Nevertheless, American and British venture capitalists wanted to invest in amyloid projects, not tau.
By 2002, Dr. Wischik scraped together about $5 million from Asian investors with the help of a Singaporean physician who was the father of a classmate of Dr. Wischik’s son in Cambridge. TauRx is based in Singapore but conducts most of its research in Aberdeen, Scotland. As his tau effort launched, early tests of drugs designed to attack amyloid plaques were disappointing. To better understand these results, a team of British scientists largely unaffiliated with Athena or the failed clinical trial decided to examine the brains of patients who had participated in the study. They waited for the patients to die, and then, after probing the brains, concluded that
- the vaccine had indeed cleared amyloid plaque but hadn’t prevented further neurodegeneration.
Peter Davies, an Alzheimer’s researcher at the Feinstein Institute for Medical Research in Manhasset, NY, recalls hearing a researcher at a conference in the early 2000s concede that his amyloid research results “don’t fit the hypothesis, but we’ll continue until they do! “I just sat there with my mouth open,” he recalls.
In 2004, TauRx began a clinical trial of its drug, called methylene blue, in 332 Alzheimer’s patients. Around the same time, a drug maker called Elan Corp., which had bought Athena Neurosciences, began a trial of an amyloid-targeted drug called bapineuzumab in 234 patients. A key moment came in 2008, when Dr. Wischik and Elan presented results of their studies at an Alzheimer’s conference in Chicago. The Elan drug
- failed to improve cognition any better than a placebo pill, causing Elan shares to plummet by more than 60% over the next few days.
The TauRx results Dr. Wischik presented were more positive, though not unequivocal. The study showed that,
- after 50 weeks of treatment, Alzheimer’s patients taking a placebo had fallen 7.8 points on a test of cognitive function,
- while people taking 60 mg of TauRx’s drug three times a day had fallen one point—
- translating into an 87% reduction in the rate of decline for people taking the TauRx drug.
But TauRx didn’t publish a full set of data from the trial, causing some skepticism among researchers. (Dr. Wischik says it didn’t to protect the company’s commercial interests). What’s more,
- a higher, 100-mg dose of the drug didn’t produce the same positive effects in patients;
Dr. Wischik blames this on the way the 100-mg dose was formulated, and says the company is testing a tweaked version of the drug in its new clinical trials, which will begin enrolling patients late this year.
This summer, a trio of companies that now own the rights to bapineuzumab—Elan, Pfizer and Johnson & Johnson—
- scrapped development of the drug after it failed to work in two large clinical trials.
Then in August, Eli Lilly & Co. said its experimental medicine targeting beta amyloid,
- solanezumab, failed to slow the loss of memory or basic skills like bathing and dressing in two trials
- involving 2,050 patients with mild or moderate Alzheimer’s.
Lilly has disclosed that in one of the trials, when moderate patients were stripped away,
- the drug slowed cognitive decline only in patients with mild forms of the disease.
Still fervent believers assert that beta amyloid needs to be attacked very early in the disease cycle—
- perhaps before symptoms begin.
This spring, the U.S. government said it would help fund a $100 million trial of Roche’s amyloid-targeted drug, crenezumab, in 300 people
- who are genetically predisposed to develop early-onset Alzheimer’s but who don’t yet have symptoms.
This trial should help provide a “definitive” answer about the theory.
Scientists and investors are giving more attention to tau. Roche this year said it would pay Switzerland’s AC Immune an undisclosed upfront fee for the rights to a new type of tau-targeted drug, and up to CHF400 million in additional payments if any drugs make it to market.
Dr. Buee, the longtime tau researcher in France, says Johnson & Johnson asked him to provide advice on tau last year, and that he’s currently discussing a tau research contract with a big pharmaceutical company. (A Johnson & Johnson spokeswoman says the company invited Dr. Buee and other scientists to a meeting to discuss a range of approaches to fighting Alzheimer’s.)
With its new clinical trial program under way,
TauRx is the first company to test a
tau-targeted drug against Alzheimer’s in a large human study, known in the industry as a phase 3 trial. Dr. Wischik
- In the end…it’s down to the phase 3 trial.
Protein Degradation in Neurodegenerative Diseases
Cebollero E , Reggiori F and Kraft C. Ribophagy: Regulated Degradation of Protein Production Factories. Int J Cell Biol. 2012; 2012: 182834. doi: 10.1155/2012/182834 (online).
During autophagy, cytosol, protein aggregates, and organelles
- are sequestered into double-membrane vesicles called autophagosomes and delivered to the lysosome/vacuole for breakdown and recycling of their basic components.
In all eukaryotes this pathway is important for
- adaptation to stress conditions such as nutrient deprivation, as well as
- to regulate intracellular homeostasis by adjusting organelle number and clearing damaged structures.
Starvation-induced autophagy has been viewed as a nonselective transport pathway; but recent studies have revealed that
- autophagy is able to selectively engulf specific structures, ranging from proteins to entire organelles.
In this paper, we discuss recent findings on the mechanisms and physiological implications of two selective types of autophagy:
- ribophagy, the specific degradation of ribosomes, and
- reticulophagy, the selective elimination of portions of the ER.
Lee JH, Yu WH,…, Nixon RA. Lysosomal Proteolysis and Autophagy Require Presenilin 1 and Are Disrupted by Alzheimer-Related PS1 Mutations. Cell 2010; 141, 1146–1158. DOI 10.1016/j.cell.2010.05.008.
Macroautophagy is a lysosomal degradative pathway essential for neuron survival. Here, we show
- that macroautophagy requires the Alzheimer’s disease (AD)-related protein presenilin-1 (PS1).
In PS1 null blastocysts, neurons from mice hypomorphic for PS1 or conditionally depleted of PS1,
- substrate proteolysis and autophagosome clearance during macroautophagy are prevented
- as a result of a selective impairment of autolysosome acidification and cathepsin activation.
These deficits are caused by failed PS1-dependent targeting of the v-ATPase V0a1 subunit to lysosomes. N-glycosylation of the V0a1 subunit,
- essential for its efficient ER-to-lysosome delivery,
- requires the selective binding of PS1 holoprotein to the unglycosylated subunit and the sec61alpha/ oligosaccharyltransferase complex.
PS1 mutations causing early-onset AD produce a similar lysosomal/autophagy phenotype in fibroblasts from AD patients. PS1 is therefore essential for v-ATPase targeting to lysosomes, lysosome acidification, and proteolysis during autophagy. Defective lysosomal proteolysis represents a basis for pathogenic protein accumulations and neuronal cell death in AD and suggests previously unidentified therapeutic targets.
Hanai JI, Cao P, Tanksale P, Imamura S, et al. The muscle-specific ubiquitin ligase atrogin-1/MAFbx mediates statin-induced muscle toxicity. The Journal of Clinical Investigation 2007; 117(12):3930-3951. http://www.jci.org
Gene Wars Span Eons
Transposons have been barging into genomes and crossing species boundaries throughout evolution. Rapidly evolving bacterial species often use them to transmit antibiotic resistance to one another. Nearly half of the DNA in the human genome consists of transposons, and the percentage can potentially creep upward with every generation. That’s because nearly 20 percent of transposons are capable of replicating in a way that is unconstrained by the normal rules of DNA replication during cell division ― although through generations over time, most have become inactivated and no longer pose a threat.
While humans are riddled with transposons, compared to some organisms, they’ve gotten off easy, according to Madhani, a professor of biochemistry and biophysics at UCSF. The water lily’s genome is 99 percent derived from transposons. The lowly salamander has about the same number of genes as humans, but in some species the genome is nearly 40 times bigger, due to all the inserted, replicating transposons.
The scientists’ discovery of SCANR and how it targets transposons in the yeast Cryptococcus neoformans builds upon the Nobel-Prize-winning discovery of jumping genes by maize geneticist Barbara McClintock, and the Nobel-prize-winning discovery by molecular biologists Richard Roberts and Phillip Sharp that parts of a single gene may be separated along chromosomes by intervening bits of DNA, called introns. Introns are transcribed into RNA from DNA but then are spliced out of the instructions for building proteins.
In the current study, the researchers discovered that the cell’s splicing machinery stalls when it gets to transposon introns. SCANR recognizes this glitch and
- prevents transposon replication by
- triggering the production of “small interfering RNA” molecules, which
- neutralize the transposon RNA.
The earlier discovery by biologists Andrew Fire and Craig Mello of the phenomenon of RNA interference, a feature of this newly identified transposon targeting, also led to a Nobel Prize. “Scientists might find that many of the peculiar ways in which genes are expressed differently in higher organisms are, like
- intron splicing in the case of SCANR, useful
- in distinguishing and defending ‘self’ genes from ‘non-self’ genes,” Madhani said.
Researchers at UCSF ( Phillip Dumesic, an MD/PhD student and first author of the study, graduate students Prashanthi Natarajan and Benjamin Schiller, and postdoctoral fellow Changbin Chen, PhD.) and collaborators at the Whitehead Institute of Medical Research in Cambridge, Mass., and from the Scripps Research Institute in La Jolla, Calif., contributed to the research.
Researchers Discover Gene Invaders Are Stymied by a Cell’s Genome Defense
If unrestrained, transposons replicate and insert themselves randomly throughout the genome.
San Francisco, CA (Scicasts) – Gene wars rage inside our cells, with invading DNA regularly threatening to subvert our human blueprint. Now, building on Nobel-Prize-winning findings, UC San Francisco researchers have discovered a molecular machine that helps protect a cell’s genes against these DNA interlopers.
The machine, named SCANR, recognizes and targets foreign DNA. The UCSF team identified it in yeast, but comparable mechanisms might also be found in humans. The targets of SCANR are
- small stretches of DNA called transposons, a name that conjures images of alien scourges.
But transposons are real, and to some newborns, life threatening. Found inside the genomes
- of organisms as simple as bacteria and
- as complex as humans,
they are in a way alien ― at some point,
- each was imported into its host’s genome from another species.
Unlike an organism’s native genes, which are reproduced a single time during cell division, transposons ― also called jumping genes ― replicate multiple times, and
- insert themselves at random places within the DNA of the host cell.
When transposons insert themselves in the middle of an important gene, they may cause malfunction, disease or birth defects.
But just as the immune system has ways of distinguishing what is part of the body and what is foreign and does not belong, researchers led by UCSF’s Dr. Hiten Madhani, discovered in
- SCANR a novel way through which the genetic machinery within a cell’s nucleus recognizes and targets transposons.
“We’ve known that only a fraction of human-inherited diseases are caused by these mobile genetic elements,” Madhani said. “Now we’ve found that cells use a step in gene expression to distinguish ‘self’ from ‘non-self’ and to halt the spread of transposons.” The study was published online Feb. 13 in the journal Cell (http://www.cell.com/abstract/S0092-8674%2813%2900138-4).
Epigenetics of brain and brawn
Study Shows Epigenetics Shapes Fate of Brain vs. Brawn Castes in Carpenter Ants
Philadelphia, PA (Scicasts) – The recently published genome sequences of seven well-studied ant species are opening up new vistas for biology and medicine. A detailed look at molecular mechanisms that underlie the complex behavioural differences in two worker castes in the Florida carpenter ant, Camponotus floridanus, has revealed a link to epigenetics. This is the study of how the expression or suppression of particular genes by chemical modifications affects an organism’s
- physical characteristics,
- development, and
- behaviour.
Epigenetic processes not only play a significant role in many diseases, but are also involved in longevity and aging. Interdisciplinary research teams led by Dr. Shelley Berger, from the Perelman School of Medicine at the University of Pennsylvania, in collaboration with teams led by Danny Reinberg from New York University and Juergen Liebig from Arizona State University, describe their work in Genome Research. The group found that epigenetic regulation is key to
- distinguishing one caste, the “majors”, as brawny Amazons of the carpenter ant colony,
- compared to the “minors”, their smaller, brainier sisters.
These two castes have the same genes, but strikingly distinct behaviours and shape.
Ants, as well as termites and some bees and wasps, are eusocial species that organize themselves into rigid caste-based societies, or colonies, in which only one queen and a small contingent of male ants are usually fertile and reproduce. The rest of a colony is composed of functionally sterile females that are divided into worker castes that perform specialized roles such as
- foragers,
- soldiers, and
- caretakers.
In Camponotus floridanus, there are two worker castes that are physically and behaviourally different, yet genetically very similar. “For all intents and purposes, those two castes are identical when it comes to their gene sequences,” notes senior author Berger, professor of Cell and Developmental Biology. “The two castes are a perfect situation to understand
- how epigenetics,
- how regulation ‘above’ genes,
plays a role in establishing these dramatic differences in a whole organism.”
To understand how caste differences arise, the team examined the role of modifications of histones throughout the genome. They produced the first genome-wide epigenetic maps of genome structure in a social insect. Histones can be altered by the addition of small chemical groups, which affect the expression of genes. Therefore, specific histone modifications can create dramatic differences between genetically similar individuals, such as the physical and behavioural differences between ant castes. “These chemical modifications of histones alter how compact the genome is in a certain region,” Simola explains. “Certain modifications allow DNA to open up more, and some of them to close DNA more. This, in turn, affects how genes get expressed, or turned on, to make proteins.
In examining several different histone modifications, the team found a number of distinct differences between the major and minor castes. Simola states that the most notable modification,
- discriminates the two castes from each other and
- correlates well with the expression levels of different genes between the castes.
And if you look at which genes are being expressed between these two castes, these genes correspond very nicely to the brainy versus brawny idea. In the majors we find that genes that are involved in muscle development are expressed at a higher level, whereas in the minors, many genes involved in brain development and neurotransmission are expressed at a higher level.”
These changes in histone modifications between ant castes are likely caused by a regulator gene, called CBP, that has “already been implicated in aspects of learning and behaviour by genetic studies in mice and in certain human diseases,” Berger says. “The idea is that the same CBP regulator and histone modification are involved in a learned behaviour in ants – foraging – mainly in the brainy minor caste, to establish a pattern of gene regulation that leads to neuronal patterning for figuring out where food is and being able to bring the food back to the nest.” Simola notes that “we know from mouse studies that if you inactivate or delete the CBP regulator, it actually leads to significant learning deficits in addition to craniofacial muscular malformations. So from mammalian studies, it’s clear this is an important protein involved in learning and memory.”
The research team is looking ahead to expand the work by manipulating the expression of the CBP regulator in ants to observe effects on caste development and behaviour. Berger observes that all of the genes known to be major epigenetic regulators in mammals are conserved in ants, which makes them a good model for studying behaviour and longevity.
Research Reveals Mechanism of Epigenetic Reprogramming
Cambridge, UK (Scicasts) – New research reveals a potential way for how parents’ experiences could be passed to their offspring’s genes.
Epigenetics is a system that turns our genes on and off. The process works by chemical tags, known as epigenetic marks, attaching to DNA and telling a cell to either use or ignore a particular gene. The most common epigenetic mark is a methyl group.
- When these groups fasten to DNA through a process called methylation
- they block the attachment of proteins which normally turn the genes on.
As a result, the gene is turned off.
Scientists have witnessed epigenetic inheritance, the observation that offspring may inherit altered traits due to their parents’ past experiences. For example, historical incidences of famine have resulted in health effects on the children and grandchildren of individuals who had restricted diets,
- possibly because of inheritance of altered epigenetic marks caused by a restricted diet.
However, it is thought that between each generation
- the epigenetic marks are erased in cells called primordial gene cells (PGC), the precursors to sperm and eggs.
This ‘reprogramming’ allows all genes to be read afresh for each new person – leaving scientists to question how epigenetic inheritance could occur.
The new Cambridge study initially discovered how the DNA methylation marks are erased in PGCs. The methylation marks are converted to hydroxymethylation which is then
- progressively diluted out as the cells divide.
This process turns out to be remarkably efficient and seems to reset the genes for each new generation.
The researchers, also found that some rare methylation can ‘escape’ the reprogramming process and can thus be passed on to offspring – revealing how epigenetic inheritance could occur. This is important because aberrant methylation could accumulate at genes during a lifetime in response to environmental factors, such as chemical exposure or nutrition, and can cause abnormal use of genes, leading to disease. If these marks are then inherited by offspring, their genes could also be affected. The research demonstrates how genes could retain some memory of their past experiences, indicating that the idea that epigenetic information is erased between generations – should be reassessed. The precursors to sperm and eggs are very effective in erasing most methylation marks, but they are fallible and at a low frequency may allow some epigenetic information to be transmitted to subsequent generations.
Professor Azim Surani from the University of Cambridge, principal investigator of the research, said: “The new study has the potential to be exploited in two distinct ways.
- how to erase aberrant epigenetic marks that may underlie some diseases in adults.
- address whether germ cells can acquire new epigenetic marks through environmental or dietary influences on parents that may evade erasure and be transmitted to subsequent generations
The research was published 25 January, in the journal Science. Story adapted from the University of Cambridge.
Study Suggests Expanding the Genetic Alphabet May Be Easier than Previously Thought
Featured In: Academia News | Genomics
Monday, June 4, 2012
A new study led by scientists at The Scripps Research Institute suggests that the replication process for DNA—the genetic instructions for living organisms that is composed of four bases (C, G, A and T)—is more open to unnatural letters than had previously been thought. An expanded “DNA alphabet” could carry more information than natural DNA, potentially coding for a much wider range of molecules and enabling a variety of powerful applications, from precise molecular probes and nanomachines to useful new life forms.
The new study, which appears in the June 3, 2012 issue of Nature Chemical Biology, solves the mystery of how a previously identified pair of artificial DNA bases can go through the DNA replication process almost as efficiently as the four natural bases.
“We now know that the efficient replication of our unnatural base pair isn’t a fluke, and also that the replication process is more flexible than had been assumed,” said Floyd E. Romesberg, associate professor at Scripps Research, principal developer of the new DNA bases, and a senior author of the new study. The Romesberg laboratory collaborated on the new study with the laboratory of co-senior author Andreas Marx at the University of Konstanz in Germany, and the laboratory of Tammy J. Dwyer at the University of San Diego.
Adding to the DNA Alphabet
Romesberg and his lab have been trying to find a way to extend the DNA alphabet since the late 1990s. In 2008, they developed the efficiently replicating bases NaM and 5SICS, which come together as a complementary base pair within the DNA helix, much as, in normal DNA, the base adenine (A) pairs with thymine (T), and cytosine (C) pairs with guanine (G).
The following year, Romesberg and colleagues showed that NaM and 5SICS could be efficiently transcribed into RNA in the lab dish. But these bases’ success in mimicking the functionality of natural bases was a bit mysterious. They had been found simply by screening thousands of synthetic nucleotide-like molecules for the ones that were replicated most efficiently. And it had been clear immediately that their chemical structures lack the ability to form the hydrogen bonds that join natural base pairs in DNA. Such bonds had been thought to be an absolute requirement for successful DNA replication‑—a process in which a large enzyme, DNA polymerase, moves along a single, unwrapped DNA strand and stitches together the opposing strand, one complementary base at a time.
An early structural study of a very similar base pair in double-helix DNA added to Romesberg’s concerns. The data strongly suggested that NaM and 5SICS do not even approximate the edge-to-edge geometry of natural base pairs—termed the Watson-Crick geometry, after the co-discoverers of the DNA double-helix. Instead, they join in a looser, overlapping, “intercalated” fashion. “Their pairing resembles a ‘mispair,’ such as two identical bases together, which normally wouldn’t be recognized as a valid base pair by the DNA polymerase,” said Denis Malyshev, a graduate student in Romesberg’s lab who was lead author along with Karin Betz of Marx’s lab.
Yet in test after test, the NaM-5SICS pair was efficiently replicable. “We wondered whether we were somehow tricking the DNA polymerase into recognizing it,” said Romesberg. “I didn’t want to pursue the development of applications until we had a clearer picture of what was going on during replication.”
Edge to Edge
To get that clearer picture, Romesberg and his lab turned to Dwyer’s and Marx’s laboratories, which have expertise in finding the atomic structures of DNA in complex with DNA polymerase. Their structural data showed plainly that the NaM-5SICS pair maintain an abnormal, intercalated structure within double-helix DNA—but remarkably adopt the normal, edge-to-edge, “Watson-Crick” positioning when gripped by the polymerase during the crucial moments of DNA replication.
“The DNA polymerase apparently induces this unnatural base pair to form a structure that’s virtually indistinguishable from that of a natural base pair,” said Malyshev.
NaM and 5SICS, lacking hydrogen bonds, are held together in the DNA double-helix by “hydrophobic” forces, which cause certain molecular structures (like those found in oil) to be repelled by water molecules, and thus to cling together in a watery medium. “It’s very possible that these hydrophobic forces have characteristics that enable the flexibility and thus the replicability of the NaM-5SICS base pair,” said Romesberg. “Certainly if their aberrant structure in the double helix were held together by more rigid covalent bonds, they wouldn’t have been able to pop into the correct structure during DNA replication.”
An Arbitrary Choice?
The finding suggests that NaM-5SICS and potentially other, hydrophobically bound base pairs could some day be used to extend the DNA alphabet. It also hints that Evolution’s choice of the existing four-letter DNA alphabet—on this planet—may have been somewhat arbitrary. “It seems that life could have been based on many other genetic systems,” said Romesberg.
He and his laboratory colleagues are now trying to optimize the basic functionality of NaM and 5SICS, and to show that these new bases can work alongside natural bases in the DNA of a living cell.
“If we can get this new base pair to replicate with high efficiency and fidelity in vivo, we’ll have a semi-synthetic organism,” Romesberg said. “The things that one could do with that are pretty mind blowing.”
The other contributors to the paper, “KlenTaq polymerase replicates unnatural base pairs by inducing a Watson-Crick geometry,” are Thomas Lavergne of the Romesberg lab, Wolfram Welte and Kay Diederichs of the Marx lab, and Phillip Ordoukhanian of the Center for Protein and Nucleic Acid Research at The Scripps Research Institute.
Source: The Scripps Research Institute
Like this:
Like Loading...
Read Full Post »
 worms, that reducing the activity of the signaling mechanism conveyed through insulin and the growth hormone IGF1, a major aging regulating pathway, constituted a defense against the aggregation of the Aβ protein which is mechanistically-linked with
worms, that reducing the activity of the signaling mechanism conveyed through insulin and the growth hormone IGF1, a major aging regulating pathway, constituted a defense against the aggregation of the Aβ protein which is mechanistically-linked with 

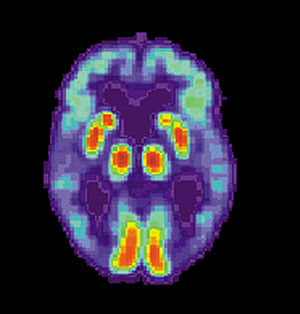
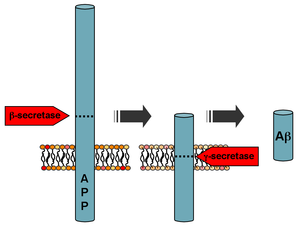

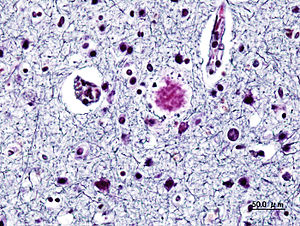
 One of the primary culprits in the neurobiological development of Alzheimer’s disease is a protein called amyloid beta, which can build up and form plaques in the brain. Now European scientists are reporting that a common psoriasis drug could stop these plaques from forming by targeting a natural inflammatory response in our brains — lending credence to the idea of Alzheimer’s as an auto-immune disease.
One of the primary culprits in the neurobiological development of Alzheimer’s disease is a protein called amyloid beta, which can build up and form plaques in the brain. Now European scientists are reporting that a common psoriasis drug could stop these plaques from forming by targeting a natural inflammatory response in our brains — lending credence to the idea of Alzheimer’s as an auto-immune disease.








![A Pot[age] to Die For A Pot[age] to Die For](https://i0.wp.com/farm5.static.flickr.com/4102/4874343314_6aa1f56fd4_m.jpg?resize=240%2C180)



