Neural Networks in Alzheimer’s
Larry H. Bernstein, MD, FCAP, Curator
LPBI
SfN 2015 Recap: The Role of Synapses, Neural Networks in Alzheimer’s
Stephanie Guzowski, Editor
http://www.dddmag.com/articles/2015/11/sfn-2015-recap-role-synapses-neural-networks-alzheimers
http://www.dddmag.com/sites/dddmag.com/files/perineuronal%20nets_SfN.jpg
Perineuronal nets, shown in green, in three regions of the mouse brain. Credit: S.F. Palida et al.
Cognition and behavior rely on communication between individual neurons and extensive interactions between neural networks. But when synaptic dysfunction occurs, the results can be dire, leading to neurodegenerative symptoms in Alzheimer’s disease.
“The brain is the seed of our personal identity,” said Valina Dawson, Ph.D., director of neurogeneration and stem cell programs at Johns Hopkins University in Baltimore, Maryland. “It allows us to interact with our world but when things go wrong in the brain, it’s disastrous for the individual as well as the family.
“Our ability to treat these diseases is limited at the moment. We need new insight into what goes wrong.”
A lesser-known protein
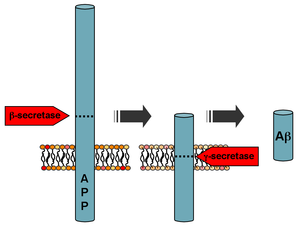
Researchers, for years, have targeted amyloid beta (Aβ) in attempts to halt the progression of Alzheimer’s disease, and have recently, shown increased interest in the protein, tau.
But Paula Pousinha, Ph.D., at the French National Centre for Scientific Research, has focused her research on a lesser-known protein fragment: amyloid precursor protein intracellular domain (AICD). AICD is a fragment of amyloid precursor protein (APP), which is formed at the same time as Aβ in the brain. New evidence suggests that in addition to Aβ, AICD also disrupts communication between neurons during the progression of Alzheimer’s disease. Pousinha presented thesepublished findings at this year’s Society for Neuroscience (SfN) conference, which took place from October 17 to 21 in Chicago.
“Although AICD has been known for more than 10 years, it has been poorly studied,” said Pousinha.
Pousinha’s research team demonstrated that overexpressing AICD levels with AAV vector in rats’ brains “perturbs neuronal communication in the hippocampus,” a key structure necessary in forming memories and an area earliest affected in Alzheimer’s disease.
“In normal animals, if we apply to these neurons a high-frequency stimulation, afterward the neurons are stronger,” said Pousinha. “Neurons where we overexpressed AICD failed to have this potentization.”
Pousinha doesn’t negate the importance of Aβ in the development of neurodegenerative diseases. “Our study doesn’t exclude the pathological effects of Aβ,” she said. “We believe that Alzheimer’s disease is much more complex and has more than one candidate that has implications.
“It’s very important for the scientific community to understand the role of all these APP fragments of neuroinflammation — different pieces of the puzzle of how we can stop the disease progression.”
How do memories persist in the brain long term?
New research, also presented at this year’s SfN, has implications for understanding memory to develop treatments for Alzheimer’s disease and dementias. Sakina Palida, a graduate student at the University of California, San Diego found that localized modifications in the perineuronal net (PNN) at synapses could be a mechanism by which information is stably encoded and preserved in the brain over time.
“We still don’t understand how we stably encode and store memories in our brains for up to our entire lifetimes,” said Palida. The prevailing idea on how memories are maintained over time generally focus on postsynaptic proteins, said Palida. “But the problem with looking at intracellular synaptic proteins is that the majority turn over rapidly, of hours to at most a few days. So they’re very unstable.”
So, Palida and her team identified PNN as an ideal substrate for long-term memory. “Kind of like how you carve into stone — stone is a stable substrate — you retain the information regardless of what comes and goes over it.” They demonstrated that individual PNN proteins are highly stable, and that the PNN is locally degraded when synapses are strengthened.
And the team also demonstrated that mice lacking enzymes that degrade the PNN have deficient long-term, but not short-term, memory. “Which is a really exciting new result,” said Palida.
To track the PNN in live animals, Palida and her team fused a fluorescent protein to a small link protein in the PNN to allow tracking of PNN dynamics in real time. They also monitored PNN degradation in live cells after stimulating neurons with brain-derived neurotrophic factor (BDNF), a chemical secreted in the nervous system to enhance signaling — and observed localized degradation of the PNN at some newly formed synapses.
Crtl 1-Venus. Fusion of a fluorescent protein to small link proteins in the PNN allows tracking of PNN dynamics over time. Credit: S.F. Palida et al. Crtl1-Venus Neurons. Tracking PNN dynamics in live cells, in mouse brain tissue. Credit: S.F. Palida et al.
What’s next? “We’re currently making transgenic animals to express this protein, which would allow us to monitor PNN dynamics simultaneously with synaptic dynamics in a live animal brain, and really investigate this hypothesis further,” said Palida.
Increased APP intracellular domain (AICD) production perturbs synaptic signal integration via increased NMDAR function
*Paula A Pousinha1PubmedElisabeth Raymond1PubmedXavier Mouska1PubmedMichael Willem2PubmedHélène Marie1Pubmed
1660 Route de Lucioles, CNRS IPMC UMR 7275, Valbonne, France; 2Ludwig-Maximilians-University Munich, Munich, Germany
Alzheimer’s disease (AD) is a neurodegenerative disease that begins as mild short-term memory deficits and culminates in total loss of cognition and executive functions. The main culprit of the disease, resulting from Amyloid-Precursor Protein (APP) processing, has been thought to be amyloid-b peptide (Ab). However, despite the genetic and cell biological evidence that supports the amyloid cascade hypothesis, it is becoming clear that AD etiology is complex and that Ab alone is unable to account for all aspects of AD [Pimplikar et al. J Neurosci.30: 14946. 2010]. Gamma-secretase not only liberates Ab, but also its C-terminal intracellular counterpart called APP intracellular domain (AICD) [Passer. et al. JAlzheimers Dis.2: 289-301. 2000], which is known to also accumulate in AD patient’s brain [Ghosal et al. PNAS.106:18367. 2009], but surprisingly little is known about its functions in the hippocampus. To address this crucial issue, we increased AICD production in vivo in adult CA1 pyramidal neurons, mimicking the human pathological condition. Different ex-vivo electrophysiological and pharmacological approaches, including double- patch of neighbor neurons were used. We clearly demonstrate that in vivo AICD production increases synaptic NMDA receptor currents. This causes a frequency-dependent disruption of synaptic signal integration, leading to impaired long-term potentiation, which we were able to rescue by different pharmacological approaches. Our results provide convincing and entirely novel evidence that increased in vivo production of AICD is enough, per se, to cause synaptic dysfunction in CA1 hippocampal neurons.
131.21P2X2R-FE65 interaction induces synaptic failure and neuronal dyshomeostasis after treatments with soluble oligomers of amyloid beta peptide
300.15Early synaptic deficits in Alzheimer’s disease involve neuronal adenosine A2A receptors
215.08Homeostatic coupling between surface trafficking and cleavage of amyloid precursor protein
280.11A novel mechanism for lowering Abeta
383.22Impact of intracellular soluble oligomers of amyloid-β peptide on glutamatergic synaptic transmission
Society for Neuroscience Annual Meeting Showcases Strides in Brain Research
10/23/2015 – Stephanie Guzowski, Editor
CHICAGO – Nearly 30,000 researchers from more than 80 countries gathered this week at the annual Society for Neuroscience (SfN) meeting, the world’s largest conference focused on scientific discovery related to the brain and nervous system.
The 45th annual SfN meeting at McCormick Place convention center showcased more than 15,000 scientific presentations on advances in technologies and new research about brain structure, disease and treatments, and 517 exhibitors, according to event organizers.
Presentations covered a wide variety of topics including new technologies to study the brain, the science behind addiction, potential treatments for spinal cord injuries, and the role of synapses in neurological conditions.
Of particular focus was the Brain Research through Advancing Innovative Neurotechnologies (BRAIN) Initiative, the large collaborative quest to develop technologies for a dynamic view of the brain. In early October, the National Institutes of Health announced its second round of funding to support goals, bringing the NIH investment to $85 million in fiscal year 2015.
Toxic Tau Could be Key to Alzheimer’s Treatment
01/06/2015 – Stephanie Guzowski, Editor
http://www.dddmag.com/articles/2015/01/toxic-tau-could-be-key-alzheimers-treatment
http://www.dddmag.com/sites/dddmag.com/files/tangles_Alz2.jpg
“But now, we know that tau is not simply a bystander but also a player,” Li said. “Both proteins work together to damage cell functions as the disease unfolds.”
Targeting tau
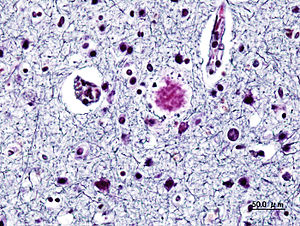
In the healthy brain, tau protein helps with the building and functioning of neurons. But when tau malfunctions, it creates abnormal clumps of protein fibers—neurofibrillary tangles—which spread rapidly throughout the brain. This highly toxic and altered form of the brain protein tau is called “tau oligomer.”
“There’s growing evidence that tau oligomers, not tau protein in general, are responsible for the development of neurodegenerative diseases, like Alzheimer’s,” said Julia Gerson, a graduate student in neuroscience at the University of Texas Medical Branch.
In Gerson’s research, which she presented at this year’s Society for Neuroscience meeting in Washington, D.C., Gerson and her team injected tau oligomers from people with Alzheimer’s into the brains of healthy mice. Subsequent testing revealed that the mice had developed memory loss.
“When we inject mice with tau oligomers, we see that they spend the same amount of time exploring a familiar object as an unfamiliar object,” said Gerson. “So they’re incapable of remembering that they’ve already seen this familiar object.”
What’s more, the molecules had multiplied throughout the animals’ brains. “This suggests that tau oligomers may spread from the injection site to other unaffected regions,” said Gerson.
Future treatments
Understanding tau’s connection to Alzheimer’s could have implications for potential therapies. “If we can stop the spread of these toxic tau oligomers, we may be capable of either preventing, or reversing, symptoms,” said Gerson. Gerson’s lab is currently investigating antibodies, which specifically fight tau oligomers.
Click to Enlarge. Normal brain vs. Alzheimer’s brain (Credit: Garrondo)
Erik Roberson, M.D., Ph.D., at the University of Alabama at Birmingham, and colleagues looked at how boosting the function of a specific type of neurotransmitter receptor, the NMDA receptor, provided benefit to people with the second most common type of dementia: frontotemporal dementia (FTD), a disease in which people experience rapid and dramatic changes in behavior, personality and social skills. People often quickly deteriorate and usually die about three years after diagnosis; there is also no effective treatment for FTD.
Since mutated tau impairs synapses—the connections between neurons—by reducing the size of NMDA receptors, “boosting the function of remaining NMDA receptors may help restore synaptic firing, and reverse behavioral abnormalities,” said Roberson.
Roberson’s, along with others’ work presented at the Society of Neuroscience meeting, focused on using animal models that mimic developing tau pathology. “These new mouse models, which contain both tau tangles and amyloid plaques” said Dr. Li, “offer the possibility of more accurately testing therapies directed at delaying the onset of amyloid beta plaques, tau accumulation and neuronal loss, all characteristic features of Alzheimer’s.”
Are clinical trials next?
Potentially, yes. “This arena of academic research has been ongoing for several years—it’s a younger area in terms of involvement of drug discovery,” said Sangram Sisodia, Ph.D., director of the Center for Molecular Neurobiology at the University of Chicago. “But I believe there is growing interest in pharma companies about targeting tau.
“The tau protein plays an incredibly complex role in the development of Alzheimer’s and other neurodegenerative diseases,” said Sisodia. “We are in the early stages of understanding that role, which will be crucial for developing effective preventions or treatments.”
Read Full Post »