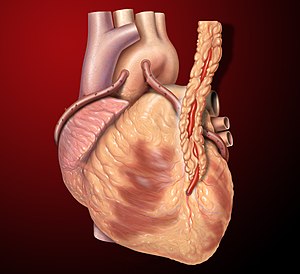
An American designed Artificial Heart by ABIOMED, the Symphony model, assists in remodeling of heart tissue cells by design, as described in
Mechanical Circulatory Assist Devices as a Bridge to Heart Transplantation or as “Destination Therapy“: Options for Patients in Advanced Heart Failure
By Larry H Bernstein, MD, FCAP
A total artificial heart (TAH) is a device that replaces the two ventricles of the heart. Those who benefit from a TAH usually have end-stage heart failure. Since the condition is so severe that the heart can’t pump enough blood to meet the body’s needs, all treatments, except heart transplant, have failed.
The TAH is attached the atria, and mechanical valves are between the TAH and the atria functioning like the heart’s valves, controlling the flow of blood in pulmonary and systemic circulation.
Currently, the two types of TAHs are the CardioWest and the AbioCor. The main difference between these TAHs is that the CardioWest is connected to an outside power source. The CardioWest has tubes that, through holes in the abdomen, run from inside the chest to an outside power source.
CardioWest Total Artificial Heart
Figure A shows a CardioWest TAH. Tubes exit the body and connect to a machine that powers the TAH and controls how it works.

The AbioCor TAH is completely contained inside the chest. A battery powers this TAH, and the battery is charged through the skin with a special magnetic charger. Energy from the external charger reaches the internal battery through an energy transfer device called transcutaneous energy transmission, or TET. An implanted TET device is connected to the implanted battery. An external TET coil is connected to the external charger. Also, an implanted controller monitors and controls the pumping speed of the heart.
AbioCor Total Artificial Heart
Figure B shows an AbioCor TAH and the internal devices that control how it works.

A TAH usually extends life for months beyond what is expected with end-stage heart failure. It can keep one alive while waiting for a donor heart. It is a challenge for surgeons to implant, and it can cause complications. TAHs are devices used only in a small number of people.
There is a Difference Between Artificial Heart & Ventricular Assist Device
(see Michael Paul Maupin, eHow Contributor)
http://www.ehow.com/facts_6713118_difference-_amp_-ventricular-assist-devices.html#ixzz2a5BH465n
A ventricular assist device (VAD) utilizes the patient’s own heart, and it operates as a bridge device until a donor heart is procured for transplant. A TAH replaces a patient’s explanted heart. The VAD is grafted onto a patient’s left ventricle, boosting the impaired ventricular function. A VAD is either continuous or pulsatile in function. In a continuous VAD, blood is circulated through the heart like water through a hose. A pulsatile VAD more mimics the expulsion of blood in rhythmic patterns.
http://www.ehow.com/facts_6713118_difference-_amp_-ventricular-assist-devices.html#ixzz2a5Bcbszh
On the other hand, an artificial heart completely replaces the human heart. The device functions in every way a healthy human heart would in the absence of cardiac disease. The TAH creates the same pattern of squeeze-and-release seen in a real heart.
http://www.ehow.com/facts_6713118_difference-_amp_-ventricular-assist-devices.html#ixzz2a5Bn6xaR
As of 2010, the longest any human being has lived with an artificial heart is 21 months. In comparison, documentation exists in which a VAD recipient was still enjoying a vigorous quality of life after seven years.
Read more: http://www.ehow.com/facts_6713118_difference-_amp_-ventricular-assist-devices.html#ixzz2a5C1cPFV
The SynCardia temporary Total Artificial Heart
(An artificial heart displayed at the London Science Museum)

http://www.wikipedia.com/Artificial Heart
An artificial heart is a device is typically used to bridge the time to heart transplantation, or to permanently replace the heart in case heart transplantation is impossible. The first artificial heart to be successfully implanted in a human was the Jarvik-7, designed and implemented by Robert Jarvik in 1982, but the first two patients to receive these hearts survived 112 (4 m) and 620 (21 m) days beyond their surgeries, respectively.[1]
Jarvik-7
It has already been stated that a TAH is distinct from a VAD, both used to support a failing heart. It is also distinct from a cardiopulmonary bypass machine, which is an external device used to provide the functions of both the heart and lungs, and it is used for only a few hours during cardiac bypass surgery.
Origin and Development of the Heart-Lung Bypass
A synthetic replacement for the severely failing heart would be expected to lower the need for heart transplants, because the demand for organs always greatly exceeds supply. However, the first devices had problems with reactivity to synthetic materials and power supplies. For example, the Jarvik models were not created of a material that the human body would accept. This problem was improved when Dayton, Ohio’s Ival O. Salyer, along with various colleagues, developed a polymer material that the human body would not necessarily reject.
Prior to Jarvik-7, 41-year-old Henry Opitek made medical history in 1952 at Harper Hospital, Wayne State University in Detroit, Michigan when Dr. Forest Dewey Dodrill used the Dodrill-GMR heart machine to bypass Henry Opitek’s left ventricle for 50 minutes while he repaired the mitral valve. [2][3] In this case In Dr. Dodrill’s post-operative report, he notes, “To our knowledge, this is the first instance of survival of a patient when a mechanical heart mechanism was used to take over the complete body function of maintaining the blood supply of the body while the heart was open and operated on.”[4] A heart-lung machine was used in 1953 during a successful open heart surgery by Dr. John Heysham Gibbon, the inventor, who performed the operation with the heart-lung substitute (distinct from an artificial heart substitute).
Designs of total artificial hearts
A precursor to the modern artificial heart pump was built by doctors William Sewell and William Glenn of the Yale School of Medicine in 1949 using an assortment of parts, and successfully bypassed the heart of a dog for more than an hour.[5]
The first patent for an artificial heart was held by Paul Winchell invented and Dr. Henry Heimlich (of the Heimlich Maneuver), which preceded the Jarvik heart. On December 12, 1957, Dr. Willem Johan Kolff, the world’s most prolific inventor of artificial organs, implanted an artificial heart into a dog at Cleveland Clinic before he relocated to Salt Lake City, Utah, where there was established an Institute for artificial organs. There, more than 200 physicians, engineers, students and faculty at the University of Utah Division of Artificial Organs developed, tested and improved Dr. Kolff’s artificial heart. To help manage his many endeavors, Dr. Kolff assigned project managers. Each project was named after its manager. Graduate student Robert Jarvik was the project manager for the artificial heart, which was subsequently renamed the Jarvik 7.
In 1958, Domingo Liotta initiated the studies of TAH replacement at Lyon, France, and in 1959–60 at the National University of Córdoba, Argentina. He presented his work at the meeting of the American Society for Artificial Internal Organs held in Atlantic City in March 1961. At that meeting, Dr. Liotta described the implantation of three types of orthotopic (inside the pericardial sac) TAHs in dogs, each of which used a different source of external energy: an implantable electric motor, an implantable rotating pump with an external electric motor, and a pneumatic pump.[6][7]
In 1964, the National Institutes of Health started the Artificial Heart Program, with the goal of putting a man-made organ into a human by the end of the decade.[8] The first success followed in February 1966, when Dr. Adrian Kantrowitz performed the world’s first permanent implantation of a partial mechanical heart (left ventricular assist device) at Maimonides Medical Center, Brooklyn, NY.[9] He relocated to Detroit’s Sinai and Wayne Stae University.
In 1981, Dr. William DeVries submitted a request to the FDA to implant the Jarvik 7 into a human being. On December 2, 1982, Dr. Kolff implanted the Jarvik 7 artificial heart into Barney Clark, who was suffering from severe congestive heart failure. With Clark tethered to an external 400 lb pneumatic compressor, he suffered prolonged periods of confusion, a number of instances of bleeding, and asked several times to be allowed to die.[10]
Total Artificial Heart (TAH)
On April 4, 1969, Domingo Liotta and Denton A. Cooley replaced a dying man’s heart with a mechanical heart inside the chest at The Texas Heart Institute in Houston as a bridge for a transplant. The patient woke up and recovered well. After 64 hours, the pneumatic-powered artificial heart was removed and replaced by a donor heart. However thirty-two hours after transplantation, the patient died of what was later proved to be an acute pulmonary infection, extended to both lungs, caused by fungi, most likely caused by an immunosuppressive drug complication.[11]
The original prototype of Liotta-Cooley artificial heart used in this historic operation is prominently displayed in the Smithsonian Institution’s National Museum of American History “Treasures of American History” exhibit in Washington, D.C..[12]
Permanent Pneumatic Total Artificial Heart (TAH)
The eighty-fifth clinical use of an artificial heart designed for permanent implantation rather than a bridge to transplant occurred in 1982 at the University of Utah. Artificial kidney pioneer Dr. Willem Johan Kolff started the Utah artificial organs program in 1967.[13] There, physician-engineer Dr. Clifford Kwan-Gett invented two components of an integrated pneumatic artificial heart system: a ventricle with hemispherical diaphragms that did not crush red blood cells (a problem with previous artificial hearts) and an external heart driver that inherently regulated blood flow without needing complex control systems.[14] Dr. Robert Jarvik combined several modifications of the original: an ovoid shape to fit inside the human chest, a more blood-compatible polyurethane developed by biomedical engineer Dr. Donald Lyman, and a fabrication method by Kwan-Gett that made the inside of the ventricles smooth and seamless to reduce dangerous stroke-causing blood clots.[16]
Today, the modern version of the Jarvik 7 is known as the SynCardia temporary CardioWest Total Artificial Heart. It has been implanted in more than 800 people as a bridge to transplantation.

In the mid-1980s, artificial hearts were powered by dishwasher-sized pneumatic power sources whose lineage went back to Alpha-Laval milking machines and required two catheters to cross the abdominal wall to carry the pneumatic pulses to the implanted heart. The National Heart, Lung, and Blood Institute opened a competition for implantable electrically powered artificial hearts funding Cleveland Clinic in Cleveland, Ohio; the College of Medicine of Pennsylvania State University (Penn State Hershey Medical Center) in Hershey, Pennsylvania; and AbioMed, Inc. of Danvers, Massachusetts.

Polymeric trileaflet valves ensure unidirectional blood flow with a low pressure gradient and good longevity. State-of-the-art transcutaneous energy transfer eliminates the need for electric wires crossing the chest wall.
AbioCor
The first AbioCor to be surgically implanted in a patient was on July 3, 2001.[17] The AbioCor is made of titanium and plastic with a weight of two pounds, and its internal battery can be recharged with a transduction device that sends power through the skin.[17] The internal battery lasts for a half hour, and a wearable external battery pack lasts for four hours.[18] The FDA announced on September 5, 2006, that the AbioCor, intended for critically ill patients who can not receive a heart transplant[19] could be implanted after the device had been tested on 15 patients.[19] But limitations of the current AbioCor are that its size makes it suitable for only about 50% of the male population, and its useful life is only 1–2 years.[20] AbioMed designed a smaller, more stable heart, the AbioCor II, by combining its valved ventricles with the control technology and roller screw developed at Penn State. This pump, which should be implantable in most men and 50% of women with a life span of up to five years,[20] had animal trials in 2005, and the company hoped to get FDA approval for human use in 2008.[21]
Intrathoracic Pump (LVAD)
On July 19, 1963, E. Stanley Crawford and Domingo Liotta implanted the first clinical Left Ventricular Assist Device (LVAD) at The Methodist Hospital in Houston, Texas, in a patient who had a cardiac arrest after surgery. The patient survived for four days under mechanical support but did not recover from the complications of the cardiac arrest.
On April 21, 1966, Michael DeBakey and Liotta implanted the first clinical LVAD in a paracorporeal position (where the external pump rests at the side of the patient) at The Methodist Hospital in Houston, in a patient experiencing cardiogenic shock after heart surgery. The patient developed neurological and pulmonary complications and died after few days of mechanical support. In October 1966, DeBakey and Liotta implanted the paracorporeal Liotta-DeBakey LVAD in a new patient who recovered well and was discharged from the hospital after 10 days, marking the first successful use of an LVAD for postcardiotomy shock.
Recent developments
In June 1996, a 46-year-old Taiwanese American Mr. Yao ST received the world’s first total artificial heart implantation done by Dr. Jeng Wei at Cheng-Hsin General Hospital[26] in the Republic of China (Taiwan). This technologically advanced pneumatic Phoenix-7 Total Artificial Heart was manufactured by a Taiwanese dentist Kelvin K. Cheng, a Chinese physican T. M. Kao and colleagues at the Taiwan TAH Research Center in Tainan, Republic of China (Taiwan). With this experimental artificial heart, the patient’s BP was maintained at 90-100/40-55 mmHg and cardiac output at 4.2-5.8 L/min. After 15 days of bridging, Mr. Yao received combined heart and kidney transplantation. As of March 2013, he is still very well and is currently living in San Francisco, USA. Mr. Yao ST is the world first successful combined heart and kidney transplantation patient after bridging with total artificial heart.[27]
In August 2006, an artificial heart was implanted into a 15-year-old girl at the Stollery Children’s Hospital in Edmonton, Alberta. It was intended to act as a temporary fixture until a donor heart could be found. Instead, the artificial heart (called a Berlin Heart) allowed for natural processes to occur and her heart healed on its own. After 146 days, the Berlin Heart was removed, and the girl’s heart was able to function properly on its own.[22]
On December 16, 2011 the Berlin Heart, a ventricular assist intended for children age 16 and under, gained U.S. FDA approval. The device has since been successfully implanted in several children including a 4-year-old Honduran girl at Children’s Hospital Boston.[23]
In 2012, a study published in the New England Journal of Medicine compared the Berlin Heart to extracorporeal membrane oxygenation (ECMO) and concluded that “a ventricular assist device available in several sizes for use in children as a bridge to heart transplantation [such as the Berlin Heart] was associated with a significantly higher rate of survival as compared with ECMO.”[24] The study’s primary author, Dr. Charles D. Fraser, Jr., surgeon in chief at Texas Children’s Hospital, explained: “With the Berlin Heart, we have a more effective therapy to offer patients earlier in the management of their heart failure. ..This is a giant step forward.” [25]
Total artificial heart (TAH) invention abroad
On October 27, 2008, French professor and leading heart transplant specialist Alain F. Carpentier announced that a fully implantable artificial heart will be ready for clinical trial by 2011 and for alternative transplant in 2013. It was developed and will be manufactured by him, biomedical firm CARMAT SA, and venture capital firm Truffle Capital. The prototype uses embedded electronic sensors and is made from chemically treated animal tissues, called “biomaterials”, or a “pseudo-skin” of biosynthetic, microporous materials.[28] According to an interview of the professor Alain Carpentier in Paris (2011), a number of leading cardiac clinics already conducted successful partial replacement of the organic components of the artificial heart, for example, replacing valves, large vessels, atria, ventricles. In addition to cardio-surgery, there is the medico-psychological aspect of an artificial heart. A quarter of patients in the postoperative period after prosthetic valvular surgery developed specific psychopathological symptoms, which later received the name Skumin syndrome in 1978. It is possible that a similar problem will be discovered when conducting large-scale operations to implant an artificial heart.[29]
Another U.S. team with a prototype called 2005 MagScrew Total Artificial Heart, including Japan and South Korea researchers are racing to produce similar projects.[30][31][32]
In August 2010, 50-year-old Angelo Tigano of Fairfield, New South Wales, Australia, had his failing heart removed in a five-hour operation and it was replaced with the SynCardia temporary Total Artificial Heart by surgeon Dr Phillip Spratt, head of the heart transplant unit at St Vincent’s Hospital, Sydney.[33]
On 12 March 2011, an experimental artificial heart was implanted in 55-year-old Craig Lewis at The Texas Heart Institute in Houston by Drs. O. H. Frazier and William Cohn. The device is a combination of two modified HeartMate II pumps that is currently undergoing bovine trials.[34]
On 9 June 2011, 40 year old Matthew Green was implanted with the SynCardia temporary Total Artificial Heart in a seven hour operation at Papworth Hospital. He was the first Briton to leave hospital supported by an artificial Heart on 2 August 2011.[35]
A centrifugal pump[36][37] or an axial-flow pump[38][39] can be used as an artificial heart, resulting in the patient being alive without a pulse.
Imachi et al. described a centrifugal artificial heart which alternately pumps the pulmonary circulation and the systemic circulation, causing a pulse.[40]
Heart Assist Devices
Patients who have some remaining heart function but who can no longer live normally may be candidates for ventricular assist devices (VAD), which do not replace the human heart but complement it by taking up much of the function.
The first Left Ventricular Assist Device (LVAD) system was created by Domingo Liotta at Baylor College of Medicine in Houston in 1962.[41]
Another VAD, the Kantrowitz CardioVad, designed by Adrian Kantrowitz boosts the native heart by taking up over 50% of its function.[42] Additionally, the VAD can help patients on the wait list for a heart transplant. In a young person, this device could delay the need for a transplant by 10–15 years, or even allow the heart to recover, in which case the VAD can be removed.[42] The artificial heart is powered by a battery that needs to be changed several times while still working.
The first heart assist device was approved by the FDA in 1994, and two more received approval in 1998.[43] While the original assist devices emulated the pulsating heart, newer versions, such as the Heartmate II,[44] developed by The Texas Heart Institute of Houston, provide continuous flow. These pumps (which may be centrifugal or axial flow) are smaller and potentially more durable and last longer than the current generation of total heart replacement pumps. A major advantage of a VAD is that the patient keeps the natural heart, which may provide enough support to keep the patient alive until a solution to the problem is implemented.

Suffering from end-stage heart failure, former Vice President Dick Cheney underwent a procedure in July 2010 to have a VAD implanted at INOVA Fairfax Hospital, in Fairfax Virginia. In 2012, he received a heart transplant at age 71 after 20 months on a waiting list.
REFERENCES
2^ Stephenson, Larry W, et al. “The Michigan Heart: The World’s First Successful Open Heart Operation?” Journal of Cardiac Surgery 17.3 (2002): 238–246.
3^ Lavietes, Stuart. William Glenn, 88, Surgeon Who Invented Heart Procedure, The New York Times, March 17, 2003. Accessed May 21, 2009.
4^ Artificial Heart in the chest: Preliminary report. Trans. Amer. Soc. Inter. Organs, 1961, 7:318
5^ Ablation experimentale et replacement du coeur par un coer artificial intra-thoracique. Lyon Cirurgical, 1961, 57:704
6^ Sandeep Jauhar, M.D., Ph.D.: The Artificial Heart. New England Journal of Medicine (2004): 542–544.
7^ http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2676518/, NCBI In Memoriam Dr. Adrian Kantrowitz
8^ Barron H. Lerner, MD, PhD (December 1, 2007). “The 25th Anniversary of Barney Clark’s Artificial Heart”. Celebrity Health. HealthDiaries.com. Retrieved 15 November 2010.
9^ Orthotopic cardiac prosthesis for two-staged cardiac replacement. Am J Cardio 1969; 24:723–730.
10^ “Treasures of American History”, National Museum of American History
11^ Spare Parts: Organ Replacement in American Society. Renee C. Fox and Judith P. Swazey. New York: Oxford University Press; 1992, pp. 102–104
12^ Kwan-Gett CS, Van Kampen KR, Kawai J, Eastwood N, Kolff WJ. “Results of total artificial heart implantation in calves.” Journal of Thoracic and Cardiovascular Surgery. 1971 Dec; 62(6):880–889.
13^ “Winchell’s Heart”. Time. March 12, 1973. Retrieved April 25, 2010.
14^ Kolff
15^ a b “Patient gets first totally implanted artificial heart”. CNN.com. 2001-07-03. Archived from the original on 7 June 2008. Retrieved 2008-07-13.
16^ “AbioCor FAQs”. AbioMed. Archived from the original on 3 July 2008. Retrieved 2008-07-13.
17^ a b “FDA Approves First Totally Implanted Permanent Artificial Heart for Humanitarian Uses”. FDA.gov. 2006-09-05. Retrieved 2008-07-13.
18^ a b “Will We Merge With Machines?”. popsci.com. 2005-08-01. Archived from the original on 19 July 2008. Retrieved 2008-07-13.
19^ “14th Artificial Heart Patient Dies: A Newsmaker Interview With Robert Kung, PhD”. medscape.com. 2004-11-11. Retrieved 2008-07-13.
20^ Capital Health: One year later: Berlin Heart bridges patient back to health (August 28, 2007), Capital Health, Edmonton (archived from [1] the original) on 2007-10-01).
21^ approved Berlin Heart helps patients waiting for a transplant (December 30, 2011), Children’s Hospital Boston.
22^ http://www.nejm.org/doi/pdf/10.1056/NEJMoa1014164
23^ http://www.texaschildrens.org/About-Us/News/Berlin-Heart-NEJM-2012/
24^ Cheng-Hsin General Hospital
25^ J. Wei, K. K. Cheng, D. Y. Tung, C. Y. Chang, W. M. Wan, Y. C. Chuang: Successful Use of Phoenix-7 Total Artificial Heart. Transplantation Proceedings, 1998, 30:3403-4
26^ The Carmat Heart,- The technology behind the prosthesis
27^ “About artificial heart”. Heart For Your Soul. Retrieved 2011-02-19.
28^ Total artificial heart to be ready by 2011: research team, news.yahoo.com
29^ Scientists develop artificial heart that beats like the real thing, timesonline.co.uk
30-^ Total artificial heart to be ready by 2011: research team, afp.google.com
31^ Sydney man receives Total Artificial Heart, dailyTelegraph.com.au
32^ Berger, Eric. “New artificial heart ‘a leap forward'”. Houston Chronicle. Retrieved 23 March 2011.
33^ “Plastic heart gives dad Matthew Green new lease of life”. BBC News. August 2, 2011.
34^ Black, Rosemary (January 5, 2011). “Former vice president Dick Cheney now has no pulse”. Daily News (New York).
35^ http://www.scribd.com/doc/21241693/Pulseless-Pumps-Artificial-Hearts
36^ The pulseless life
37^ Dan Baum: No Pulse: How Doctors Reinvented The Human Heart. 2012-02-29.
38^ ‘#A new pulsatile total artificial heart using a single centrifugal pump., K. Imachi, T. Chinzei, Y. Abe, K. Mabuchi, K. Imanishi, T. Yonezawa, A. Kouno, T. Ono, K. Atsumi, T. Isoyama, et al.. Institute of Medical Electronics, Faculty of Medicine, University of Tokyo, Japan.
39^ Prolonged Assisted circulation after cardiac or aortic surgery. Prolonged partial left ventricular bypass by means of intracorporeal circulation. This paper was finalist in The Young Investigators Award Contest of the American College of Cardiology. Denver, May 1962 Am. J. Cardiol. 1963, 12:399–404
40^ a b Mitka, Mike. “Midwest Trials of Heart-Assist Device.” Journal of the American Medical Association 286.21 (2001): 2661.
41^ FDA APPROVES TWO PORTABLE HEART-ASSIST DEVICES at FDA.gov
42^ An Artificial Heart That Doesn’t Beat at TechnologyReview.com
The development and operation of these life-saving devices requires understanding and application of a combination of biology, materials science and physics.
Institute of Physics website http://www.physics.org/article-questions.asp?id=74
The artficial heart
Image: Syncardia Systems
The right atrium collects blood and the right ventricle then pumps it to the lungs where it is oxygenated. The blood is then picked up by the left atrium and distributed around the body and brain by the left ventricle. Each side of the heart has a pair of valves – one pair per lung – controlling the flow of blood.
Artificial hearts can now completely, if temporarily, replace the ventricles and valves with a device made of plastic or other man-made materials, which does the job of pumping blood around.
The type of artificial heart made by Syncardia Systems, works by using a pump carried externally in a backpack – previously, patients would have to be connected to a large, immobile pump and would not have the freedom to move around.

The NHS Choices website explains that tubes connecting the heart to the pump “send pulses of air into two expandable, balloon-like sacs in the artificial ventricles, forcing out blood in much the same way that a beating heart would”.
Other models such as that produced by AbioMed use an internal pump and battery, which can be charged via transcutaneous energy transmission – a method of transferring power under the skin without having to penetrate it, thereby decreasing the chance of infection.
Energy transmission
In the artificial hearts produced by AbioMed, an electronics package is implanted in the abdomen of the recipient of the transplant to monitor and control the pumping of the heart.
Power is supplied from an external source to components under the skin, without penetrating it, using inductive electromagnetic coupling – the same principle as used by transformers to transfer electricity between different circuits, as in the national grid.
At their simplest, systems of transcutaneous energy transmission will use an external power supply connected to an external coil of wire, generating a magnetic field in it. This, in turn, produces an induced voltage in a second coil implanted under the skin, and a rectifier is used to change this alternating current into direct current that can be used to power the electronics of the heart and its controller.
Though simple in theory, in practice there are complications that arise from the need to keep the two coils aligned correctly as the patient moves, in delivering the correct level of power so that there is no excess dissipated as heat to potentially damage surrounding tissue in the patient’s body, and in making the components small enough to be carried around without too much discomfort.
Monitoring blood flow
A replacement heart needs to be able to monitor the flow of blood to regulate its pumping and ensure that the correct amount of blood is delivered around the body.
Quicker pumping is required when the transplant recipient is more active, whereas the opposite is true while he or she is resting.
Blood-flow monitors make use of ultrasound – they bounce high-frequency sound waves off blood cells coming out of the heart, the volume and speed can be measured using similar basic principles to those behind radar.
Ultrasound is used because it can monitor the flow of blood without having to be in contact with it.
Appropriate materials
Artificial hearts need to be made of light but durable materials – the Syncardia version is plastic whereas that made by AbioMed is a combination of titanium and a specially developed polyurethane, called ‘Angioflex’.
Although the Abiomed heart is designed to have as few moving parts as possible, those that it does have are made from Angioflex and are tested to ensure that they are safe for contact with blood and capable of withstanding beating 100 000 times a day for years on end.
Materials scientists can develop substances with specific properties by manipulating the constituent elements and the way in which they are processed. Materials are characterised using various techniques from condensed-matter physics including electron microscopy, x-ray diffraction and neutron diffraction.
Because they were still quite large, the first devices produced were limited to around half the male population – those with the largest chest cavities. A newer, smaller, model is intended to extend their availability to smaller people.
An artificial heart being produced by the French medical company Carmat and expected to be available by 2013 will use chemically treated animal tissue to help avoid rejection by the host’s immune system. Aerospace engineers from Airbus were also involved in its development.
Artificial hearts combine, and improve upon, many existing physics ideas to produce a piece of technology that saves lives – although they are currently only approved as a stopgap until a donor heart can be found.
Expressions of Experience: Heart Assist Devices
Video interview with O. H. “Bud” Frazier, MD; Chief, Center for Cardiac Support; Director, Cardiovascular Surgery Research; and Co-Director, Cullen Cardiovascular Research Laboratories, at Texas Heart Institute.
O. H. “Bud” Frazier, MD, on his inspiration for developing treatments for heart failure at the Texas Heart Institute.
The Texas Heart Institute is a world leader in the development, testing and application of heart assist devices. Our goal for the surgical research conducted here is to develop and determine the best assist device to use for each individual patient. Devices may be referred to as mechanical assist devices, ventricular assist devices (VAD), left ventricular assist devices (LVAD), total artificial hearts (TAH), or simply heart pumps.
January 23, 2013
Keeping hearts pumping Dr. Bud Frazier and Dr. Billy Cohn with heart pump BiVacor. [Photo credit Mayra Beltran, Houston Chronicle]
Doctors push the limits of heart-pump technology in an effort to save lives. Dr. Bud Frazier often tells a story about when he was a medical student in the 1960s . . . Frazier had this thought: If I can keep a man alive with my hand, why can’t we make a pump that we can pull off of the shelf to do the same thing? Dr. Billy Cohn, another physician who works at the cutting edge of heart pump technology, likes to use the history of human flight as an analogy for the evolution in his field. Experimenters in both domains had to give up the idea of bio-mimicry to advance the technology. “It is similar to when man first tried to build a flying machine with flapping wings that mimic the birds. It is obvious now that fixed wings were the way to go,” he says. “We think it is the same with the nonpulsatile pump, which, because it has only one moving part, is much more durable.” – Houston Chronicle [Photo credit Mayra Beltran]
January 13, 2013
BiVACOR artificial heart device
Australian engineer Daniel Timm’s revolutionary device to be developed at THI. “I think we’re beyond the Kitty Hawk stage with this,” – Drs. Bud Frazier and Billy Cohn. Read Eric Berger’s Houston Chronicle article.
November 20, 2012
FDA Approves HeartWare LVAD for HF
The FDA gave the green light for the HeartWare Ventricular Assist System as a bridge to heart transplantation in patients with heart failure. “The miniaturized device with an integrated inflow cannula is placed within the pericardial sac . . . simplifying the surgical insertion,” said O.H. “Bud” Frazier, MD, of Texas Heart Institute. Read the full story from medpagetoday.com.
Drs. Bud Frazier & Billy Cohn TEDMED 2012
Is this the future of artificial hearts?
At TEDMED 2012, Bud Frazier and Billy Cohn of the Texas Heart Institute preview a continuous-flow heart pump with minimal parts that works via a screw pump. Watch the VIDEO.
Cameron Engineers, THI researchers collaborate on heart pump
Engineers and scientists at Cameron Manufacturing & Engineering have worked with THI researchers in developing a new heart pump. On March 1, 2012, Cameron donated $500,000 to Texas Heart Institute at St. Luke’s Episcopal Hospital to develop a prototype heart pump which could save countless lives.
Can Tiny Heart Pump Limit Heart Muscle Damage after STEMI?
Interventional cardiologists affiliated with THI at St. Luke’s recently implanted the first two patients in the nation with a tiny heart pump in a feasibility trial to determine the pump’s potential to limit damage to heart muscle following a STEMI (ST-elevation myocardial infarction). Read the full news release to learn about the FDA-approved trial and the first enrolled patients. (November 2011)
Miniature Heart Pump: Smaller May Be Better!
Dr. William “Billy” Cohn discusses recent advances in left ventricular assist devices (LVADs) and other mechanical circulatory blood pumps as they get smaller and more adaptable to individual patients. View the video of his presentation at the Pumps & Pipes Conference (15 minutes, December 2010).
Video: Artificial hearts giving hope, saving lives. (August 19, 2011)

Companion 2 and Freedom Drivers
C2 Driver Supports Total Artificial Heart Patients in the Hospital Until They Are Stable and Eligible for the Freedom® Portable Driver
The Companion 2 Driver, which can be docked in the Hospital Cart or Caddy, powers the SynCardia Total Artificial Heart from implant until the patient’s condition stabilizes. Once stable, patients who are eligible can be switched to the smaller, wearable Freedom® portable driver. The Companion 2 Driver, which can be docked in the Hospital Cart or Caddy, powers the SynCardia Total Artificial Heart from implant until the patient’s condition stabilizes. Once stable, patients who are eligible can be switched to the smaller, wearable Freedom® portable driver.
The Companion 2 (C2) Driver System, which powers the SynCardia temporary Total Artificial Heart in the hospital, was selected as the Silver Winner in the Critical-Care and Emergency Medicine Products category of the Medical Design Excellence Awards (MDEA) held on June 19 in Philadelphia.
“It is a tremendous honor to have one of our products selected as a winner for the second consecutive year,” said Michael Garippa, SynCardia Chairman/CEO/President. “Our Freedom® portable driver, the world’s first wearable power supply for the Total Artificial Heart, was selected as the Bronze Winner in the same category last year. These drivers support Total Artificial Heart patients from implant with the C2 through discharge with the Freedom.”
Once stable, patients who are eligible can be switched to the 13.5-pound Freedom portable driver. Patients who meet discharge criteria can then leave the hospital and wait for a matching donor heart at home and in their communities.
The Medical Design Excellence Awards are the industry’s premier design awards competition and is the only awards program exclusively recognizing contributions and advances in the design of medical products. Entries were evaluated on the basis of their design and engineering features, including innovative use of materials, user-related functions that improve healthcare delivery and change traditional medical attitudes or practices, features that provide enhanced benefits to the patient, and the ability to overcome design and engineering challenges to meet clinical objectives.
About the SynCardia temporary Total Artificial Heart
The SynCardia Total Artificial Heart is currently approved as a bridge to transplant for people suffering from end-stage heart failure affecting both sides of the heart (biventricular failure). There have been more than 1,200 implants of the Total Artificial Heart, accounting for more than 315 patient years of life on the device. It is the only device that eliminates the symptoms and source of end-stage biventricular failure. The TAH provides immediate, safe blood flow of up to 9.5 liters per minute through each ventricle. This high volume of blood flow helps speed the recovery of vital organs, helping make the patient a better transplant candidate.
Artificial Heart Devices used at Barnes-Jewish Hospital Washington University, St. Louis
The cardiac surgeons at the Barnes-Jewish & Washington University Heart & Vascular Center are one of the leading heart surgery teams in the nation. Our permanent and temporary artificial heart devices can dramatically improve symptoms of late-stage heart failure, and sometimes even provide long-term treatment.
Mechanical Circulatory Support
The field of mechanical circulatory support in the management of patients with heart failure has seen significant advances over the past few years. The heart failure program at Washington University and Barnes-Jewish Hospital utilizes the latest technology for both temporary and long-term mechanical support of the heart failure patient.
Temporary Support
Patients that experience severe symptoms of heart failure that cannot be stabilized with medical therapy may require a temporary support device. These implantable devices are usually placed in a cardiac catheterization lab by interventional cardiologists and/or cardiac surgeons. Temporary support devices typically serve to stabilize the patient until long-term mechanical support can be introduced. These devices include:
- intra-aortic balloon pump
- Impella 2.5, 4.0 and 5.0
- TandemHeart
- Thoratec CentriMag
Long-Term Mechanical Support
Patients may require long-term circulatory support either as a bridge to a heart transplant (bridge-to-transplant, or BTT) or as long-term treatment of heart failure in non-transplant candidates (destination therapy, or DT). The mechanical assist device program at Barnes-Jewish & Washington University Heart & Vascular Center is one of the largest programs in the country. The program has a multidisciplinary group of dedicated specialists to ensure excellent outcomes in this patient population. Currently available devices include both left ventricular assist devices (LVAD) and the total artificial heart:
- HeartMate II
- HeartWare HVAD
- Syncardia Total Artificial Heart
The cardiac surgeons at the Barnes-Jewish & Washington University Heart & Vascular Center are one of only 13 surgical teams in the country to implant the CardioWest™ temporary Total Artificial Heart (TAH-t) as a bridge-to-transplantation in specific heart transplant candidates.
The CardioWest™ TAH-t is an improved version of the Jarvik-7 Artificial Heart, which was first implanted in 1982. This unique technology allows us to treat patients who would not survive without full circulatory support. The CardioWest™ TAH-t completely replaces the patient’s diseased heart with a goal of restoring normal blood pressure, increasing cardiac output and giving organs such as the kidney and liver a chance to recover. As a result, patients become better candidates for transplantation. The program is currently involved in testing the Freedom portable driver which will allow patients to leave the hospital following implantation of the TAH.

An American designed Artificial Heart by ABIOMED, the Symphony model, assists in remodeling of heart tissue cells by design, as described in

Heart Remodeling by Design – Implantable Synchronized Cardiac Assist Device:Abiomed’s Symphony

SOURCE
Heart Remodeling by Design – Implantable Synchronized Cardiac Assist Device:Abiomed’s Symphony
Part II
Comparison of the Cardiac Operations involved in an Organ Transplant of a Donor’s Heart vs Implantation of an Artificial Heart
By Justin D Pearlman, MD, PhD, FACC
A heart donor is a patient deemed brain dead who had forethought (a designation on the driver’s license) or a designated decision-maker (Healthcare Proxy) elected to make the heart available to help save another person’s life. Every tissue in the body has proteins that render a unique signature or “smell” and every patient has a limited set of markers it will accept without a fight (the histocompatibility complex, and in particular, the human leukocyte antigen). The immune system is a major part of the body’s defenses against infection and abnormal tissues (cancer) which consists of cells trained to attack foreign protein chemistry and/or mark it for destruction with anti-bodies.
I. Heart Transplant of a Human Donor
The steps for heart transplant include:
(1) demonstration of need,
(2) identification of suitable donors,
(3) surviving while waiting for a suitable donor,
(4) surviving the removal of the damaged heart or heart and lungs to make room for the replacement (accomplished with a bypass pump),
(5) survival of the donor heart (or heart and lungs) pending preparation of the patient for receipt of the transplant,
(6) inserting the donor heart (or heart and lungs),
(7) taking the patient off the bypass pump and directing circulation through the transplant,
(8) recovery and healing,
(9) establishing and maintaining sufficient immune suppression to avoid rejection of the transplant,
(10) monitoring for functional losses or rejection.
(11) monitoring for cancer or infection,
(12) resuming enjoyment of life. Each year in the United states 800 patients die waiting for a transplant, while 2300 receive transplants.
The first heart transplant is credited to Vladimer Demikhov when he transplanted dog hearts in 1946; Dr. Shumway reported successful transplantation of the heart in 1966, and Dr. Christiaan Barnard performed the operation successfully on humans in 1967 (that patient lived 18 days). Replacing the heart with a donor heart is called orthotopic (true location) heart transplantation. Durability of a transplant improved markedly with the approval of the immune suppression medication ciclosporine. NOVA has created a shockwave video demonstrating the heart transplant operation: view video.
The actual transplantation requires only five or six lines of sutures (stitches):
- inferior and superior vena cava (venous input to the right ventricle),
- the main (or left and right) pulmonary arteries (delivery of blood from right ventricle to the lungs),
- the upper half of the original left atrium to route the 3-5 pulmonary veins to the left ventricle (return of blood from the lungs), and the
- aorta (to route blood from the left ventricle to the brain and body).
The donor heart harvesting typically includes a segment of the superior and inferior vena cava which feed
- the right atrium,
- the four pulmonary veins which feed the left atrium, and
- a portion of the pulmonary artery, and
- the aorta.
The heart is chilled to minimized its metabolic demands while it is disconnected and transferred.
The recipient heart explantation (removal of the bad heart) after the patient is supported by a bypass pump involves:
- cannulation (tubing placement) into the aorta,
- the superior vena cava and
- the inferior vena cava, then
- explantation leaving the posterior aspect of the left atrium and the posterolateral aspect of the right atrium in the recipient patient.
The left and right pulmonary veins of the donor are divided and the veins are threaded into the retained portion of the recipient left atrium. The inferor vena cava, superior vena cava, pulmonary artery, and aorta are respectively anastomosed (sewed onto the truncated portion of the corresponding native vessels end-to-end). Clots and air are flushed out and the patient is taken off bypass pump.
II. Artificial Heart: Implant of an Assist Device
Implantation of ventricular assist device or an artificial heart is easier than a heart transplant, but it has been challenging to match nature’s ability to place the pump and keep it powered and regulated. Also durability is a major issue. The most common ventricular assist device, the intra-aortic balloon pump, is a temporizing tool to sustain a patient for just a few days while alternatives are evaluated and pursued.The steps for implanting a ventricular assist pump can be as simple as:
(1) cleaning and applying antiseptics to the skin,
(2) placing a needle in the femoral artery at the groin area,
(3) threading a wire into the artery,
(4) threading a series of hollow tubes over the wire (dilators) and leaving the largest in place (introducer),
(5) threading a catheter-pump through the introducer and up the aorta to the desired location,
(6) synchronizing the pump the the cardiac cycle by electrocardiogram.
If the device is an intra-aortic balloon pump (IABP) then the device is advanced to the aortic arch so that an inflatable balloon expands and contracts within the aorta from the aortic arch down to just above the renal arteries. The IABP is designed to deflate when the heart contracts (systole), to make space for blood ejecting from the failing heart ( afterload reduction), then inflate when the heart relaxes (diastole), effectively converting a blood pressure of 120/80 to 80/120. The coronary arteries are stressed during systole and receive their blood supply during diastole, so the diastolic augmentation (inflation of the balloon during heart relaxation) markedly improves blood delivery to the coronary arteries, which is very helpful when the coronary arteries are diseased and not well suited for immediate repair. The actions of the balloon damage blood cells and can rupture the aorta. The blood cell damage activates clotting, so full anticoagulation is required. If the device is an Impella catheter pump, then the distal end (farthest into the patient) crosses the aortic valve into the left ventricle to draw blood from there and deliver it beyond the heart in the descending aorta.
|
  IABP www.fda.gov/MedicalDevices/Safety Impella www.abiomed.com IABP www.fda.gov/MedicalDevices/Safety Impella www.abiomed.com |
Devices draw their input from
- arterial blood (aorta or femoral artery)
- venous blood (vena cava), or
- a puncture wound created in the apex of the left ventricle of the heart
The next example of a ventricular assist device to consider during open heart surgery, is the bypass pump that is used during most cardiovascular surgeries, and in particular during heart or heart-lung transplant. The bypass pump relies on a tube (cannula) placed in a large source of deoxygenated blood
- the right atrium,
- the inferior vena cava or
- the femoral vein
to draw its input blood from there (diverting it from the heart), and a second cannula placed in a large artery (the aorta or the femoral artery) for output. The blood passes out of the patient (extra-corporeal) to a very large mechanical pump, that typically consists of compressible tubing and rollers to minimize trauma to the blood, passing the red cells of the blood by membranes that enable uptake of oxygen. Despite the attempts not to damage the blood, blood does get damaged, so full anti-coagulation is required. The anti-coagulation consists of intravenous heparin to bind the coagulation factors. When the patient comes off the pump, the heparinization of the blood is counteracted by intravenous protamine sulfate. Also the blood is cooled because low temperatures slow down metabolism and make the cells of the body less needy during the sub-optimal circulation support. Cooled blood has increased viscosity, offset by dilution of the blood with saline (Normal Saline, isotonic solution, w/v of NaCl, about 300 mOsm/L or 9.0 g per liter). As the pump takes over circulation, the blood supply to the heart is clamped off (cross-clamp), at which point the surgeon can work to repair the heart (valve repair, valve replacement, aorta graft, coronary grafts) or replace the heart or heart and lungs.
Artificial hearts are extensions of the concepts above, and differ primarily in
- how the pump in energized and
- how the pump is regulated.
An artificial heart is designed for long term use so it must be more gentle on the blood. In Part I: Alternative Models of Artificial Hearts, US and Europe, in this article, we reported on the Latest Innovations in Alternative Models of Artificial Hearts, the Carmat Heart, it is unusual in its design, said Dr. Joseph Rogers, an associate professor at Duke University and medical director of its cardiac transplant and mechanical circulatory support program. Surfaces in the new heart that touch human blood are made from cow tissue instead of artificial materials like plastic that can cause problems like clotting, it will decrease the anticoagulation dependence by design.
Artificial hearts must accommodate changes in demands of the body, not just in the chilled low metabolic state imposed by cardiovascular surgeons. The demands of the heart are measured by oxygen consumption in units of metabolic equivalents (METS) where 1 MET represents basal metabolism (awake at rest). MET values of activities range from 0.9 (sleeping) to 23 or more (running at 14 miles/hour = 22.5 km/hour). Thus, the artificial heart should be capable of increasing its output 2300% without damage the blood cells or running out of power. The goal of long term use generally is met by linking to an external power supply that is considered portable (on wheels), or in some cases, wearable








 Carmat’s bioprosthetic device is designed to replace the real heart for as much as five years, mimicking nature’s work using biological materials and sensors. (Benoit Tessier/Reuters)
Carmat’s bioprosthetic device is designed to replace the real heart for as much as five years, mimicking nature’s work using biological materials and sensors. (Benoit Tessier/Reuters) PARIS (Reuters) – France’s Carmat said on Friday it had carried out the first human implantation of its artificial heart.The operation, performed on Wednesday at the Georges Pompidou European Hospital in Paris, went smoothly, Carmat said in a statement, adding that the patient was being monitored in the intensive care unit but was awake and talking.(Reporting by Natalie Huet; editing by Mark John)
PARIS (Reuters) – France’s Carmat said on Friday it had carried out the first human implantation of its artificial heart.The operation, performed on Wednesday at the Georges Pompidou European Hospital in Paris, went smoothly, Carmat said in a statement, adding that the patient was being monitored in the intensive care unit but was awake and talking.(Reporting by Natalie Huet; editing by Mark John)