Alternative Designs for the Human Artificial Heart: Patients in Heart Failure – Outcomes of Transplant (donor)/Implantation (artificial) and Monitoring Technologies for the Transplant/Implant Patient in the Community
Authors and Curators: Larry H Bernstein, MD, FCAP and Justin D Pearlman, MD, PhD, FACC
and
Article Curator and Reporter: Aviva Lev-Ari, PhD, RN

Article ID #74: Alternative Designs for the Human Artificial Heart: Patients in Heart Failure – Outcomes of Transplant (donor)/Implantation (artificial) and Monitoring Technologies for the Transplant/Implant Patient in the Community. Published on 8/5/2013
WordCloud Image Produced by Adam Tubman
When the heart fails to function adequately, whether from large or multiple myocardial infarctions (tissue death/scarring) or from permanent inflammatory, toxic, microvascular or infectious muscle injury, it has two modes of failure: forward failure = inadequate pumping of blood to tissues, and backward failure = inadequate withdrawal of blood from the lungs, resulting in pulmonary congestion and elevated back-pressures which cause fluid to seep into air spaces (pulmonary edema) interfering with oxygen uptake. When the heart cannot be repaired, replacement is considered. Additional pumps may be placed in parallel and/or in series with the heart to assist circulation of blood. A heart from another patient (usually a patient deemed brain dead from trauma) or from a baboon may be transplanted to replace the ailing heart, or may be placed in tandem with the ailing heart, or the heart and lungs may be replaced together (heart-lung transplant). Additional options include the intra-aortic balloon pump, the Impella catheter pump, other ventricular assist devices. There is far greater demand for heart transplants than there are available suitable organs, so work continues on alternatives. Additional reasons to seek alternatives include the complications of transplantation. Transplantation requires shutting down the body defenses against foreign materials, called immune suppression, but the immune defense system protects against cancer and infection, so a one in five of the transplant patients succomb to cancer or infection, while others die of rejection due to insufficient suppression of the autoimmune system. Artificial materials exist that do not trigger autoimmune defenses, thereby avoiding that major issue, but energizing the pump, providing sufficient circulatory support and avoiding damage to the blood have been major hurdles.
This article has the following FIVE Parts:
Part I. Alternative Models of Artificial Hearts, US and Europe
By Larry H Bernstein, MD, FCAP and Aviva Lev-Ari, PhD, RN
Part II. Comparison of the Cardiac Operations involved in an Organ Transplant of a Donor’s Heart vs Implantation of an Artificial Heart
By Justin D Pearlman, MD, PhD, FACC
Part III. Comparative Analysis of Transplant Clinical Outcomes based on Data in:
Heart Transplant (HT) Indication for Heart Failure (HF): Procedure Outcomes and Research on HF, HT @ Two Nation’s Leading HF & HT Centers
By Larry H Bernstein, MD, FCAP and Aviva Lev-Ari, PhD, RN
Part IV. Imaging Technologies in use for Clinical Monitoring of Patients with Heart Transplant: Donor Human Heart and Artificial Heart
By Justin D Pearlman, MD, PhD, FACC
Part V. The Failure of a Heart Transplant – Pathology and Autopsy Findings
by Larry H Bernstein, MD, FCAP
Conclusions
by Larry H Bernstein, MD, FCAP
Part I
Alternative Models of Artificial Hearts, US and Europe
By Larry H Bernstein, MD, FCAP and Aviva Lev-Ari, PhD, RN
Latest Innovations in Alternative Models of Artificial Hearts, US and Europe
by Aviva Lev-Ari, PhD, RN
UPDATED on 12/29/2013
Total Artificial Heart Manufacturer SynCardia Secures $14M in Growth Financing
Total Artificial Heart Manufacturer SynCardia Secures $14M in Growth Financing
$10M Financed by SWK of Dallas with $4M from Athyrium Opportunities Fund
A $14 million infusion of funding will allow SynCardia Systems, Inc. to respond to the rapid growth in the number of Total Artificial Heart implants and SynCardia Certified Centers that has occurred since 2010. As of Dec. 16, 2013, there were 155 implants of the SynCardia Total Artificial Heart, making 2013 another record-breaking year.
TUCSON, Ariz., Dec. 17, 2013 /PRNewswire/ — Privately held SynCardia Systems, Inc. announced today that it had raised $14 million to fund the rapid growth of the only approved medical device that eliminates the symptoms and source of end-stage heart failure, the SynCardia temporary Total Artificial Heart. The SynCardia Total Artificial Heart is the world’s first and only FDA, Health Canada and CE (Europe) approved Total Artificial Heart.
“SWK is very pleased to provide SynCardia this new capital in order to help further the growth of the company’s Total Artificial Heart,” Brett Pope, CEO of SWK Holdings Corporation, says of its $10-million financing. “We are very gratified to help expand the availability of this lifesaving device.”
“In 2013 we are setting another record for SynCardia Heart implants, nearly double what was then our 2011 record-breaking year of 81 implants,” says Michael Garippa, President and CEO of SynCardia. “As of Dec. 16, 155 SynCardia Total Artificial Hearts have been implanted this year.”
The financing positively affects the development of the new, smaller 50cc version of the approved 70cc SynCardia Total Artificial Heart, the availability of the Freedom portable driver and the use of SynCardia technology for destination therapy.
“We are pleased to support SynCardia’s continued clinical and commercial successes,” says Laurent Hermouet, a partner at Athyrium. “This latest financing will help reinforce SynCardia’s supply chain and manufacturing capabilities ahead of new product launches and increased production levels.”
The $4 million provided by Athyrium Capital Management in last week’s funding supplemented $15 million in long-term growth capital it provided to SynCardia in March 2013.
Wedbush PacGrow Life Sciences acted as exclusive placement agent for the offering.
The new financing allows SynCardia to accelerate the development and launch of its 50cc Total Artificial Heart* through an FDA-approved clinical study. Together, the 50cc and 70cc sizes of the Total Artificial Heart will fit almost all women and men, as well as many pediatric patients. With this expanded product line, SynCardia anticipates the tripling of the market size and sales potential for the SynCardia Total Artificial Heart.
The funds also will help the company meet the increasing demand for the Freedom portable drivers. In a letter dated Oct. 21, 2013, the FDA determined that the Freedom PMA supplement is approvable with the submission of additional information. The 13.5-pound wearable Freedom driver, which powers the SynCardia Heart while giving patients nearly unrestricted mobility, is already approved by Health Canada and has a CE Mark for Europe.
SynCardia is an innovative, 85-employee company focused on advanced medical technology targeting the NYHA Class IV heart failure market. There are 93 SynCardia Certified Centers worldwide where the SynCardia Heart is immediately available with an additional 35 hospitals undergoing the company’s four-phase certification program. As of Dec. 16, 2013, there have been 1,262 total implants of the SynCardia Total Artificial Heart worldwide.
SWK Holdings Corporation is a specialized finance company with a focus on the global healthcare sector. SWK partners with ethical product marketers and royalty holders to provide flexible financing solutions at an attractive cost of capital to create long-term value for both SWK’s business partners and its investors. SWK believes its financing structures achieve an optimal partnership for companies, institutions and inventors seeking capital for expansion or capital and estate planning by allowing its partners to monetize future cash flow with minimal dilution to their equity stakes. Additional information on the life science finance market is available on the company’s website at http://www.swkhold.com.
Athyrium Capital Management, LLC is an asset management company formed in 2008 to focus on investment opportunities in the global healthcare sector. Athyrium invests across all healthcare verticals including biopharma, medical devices and products and healthcare services, and partners with management teams to implement creative financing solutions to companies’ capital needs. The Athyrium team has substantial investment experience in the healthcare sector across a wide range of asset classes, including public equity, private equity, fixed income, royalties and other structured securities. Athyrium has over $600 million under management as of Sept. 30, 2013. The firm’s investors include public and corporate pension funds, charitable endowments, insurance companies, funds-of-funds, family offices and university endowments. For more information, please visit http://www.athyrium.com.
*The 50cc Total Artificial Heart is designed for use as a bridge to transplant in patients of smaller stature, including women and adolescents. It has been designated as a Humanitarian Use Device (HUD) by the FDA for destination therapy in adults and as a bridge to transplant in pediatric patients. Prior to clinical study, an Investigational Device Exemption (IDE) application that includes each indication must be approved by the FDA.
** CAUTION – The Freedom portable driver is an investigational device, limited by United States law to investigational use.
About the SynCardia temporary Total Artificial Heart
For additional information, please visit: http://www.syncardia.com
Like SynCardia on Facebook
Follow SynCardia on Twitter – @SynCardia
Connect with SynCardia on LinkedIn
SOURCE
SynCardia Systems, Inc.
Read more: Total Artificial Heart Manufacturer SynCardia Secures $14M in Growth Financing – FierceMedicalDevices http://www.fiercemedicaldevices.com/press-releases/total-artificial-heart-manufacturer-syncardia-secures-14m-growth-financing#ixzz2otlLCH8I
Subscribe at FierceMedicalDevices
UPDATED on 12/23/2013
First Carmat artificial heart implanted in human in France
http://medcitynews.com/2013/12/first-artificial-heart-implanted-human/
UPDATED on 3/27/2014
Carmat Investigates Death of First Artificial Heart Recipient
Posted in Cardiovascular by Stephen Levy on March 18, 2014
French artificial heart maker Carmat says it will not perform another human implant until it has determined the cause of death of the first patient fitted with the device.
That first patient, a 76-year-old man suffering from terminal heat failure, died March 2. He received the implanted artificial heart 75 days before, on December 18. The Georges Pompidou European Hospital in Paris, where the implantation was performed, announced the death.

Artificial heart internals (Courtesy Carmat)
Alain Carpentier, MD, the inventor of the heart, told the Journal du Dimanche on March 16 that the heart had stopped after a short circuit, although the exact reasons behind the death were still unknown.
“We are trying to understand where this electronic problem came from and why,” Carpentier told the French weekly. “Our engineers are working night and day to understand, and they will find (the reason).”
Velizy Villacoublay, France–based Carmat said in a news release on March 17 that it is continuing to analyze the data from the first implanted prosthesis. The company further stated that it will continue the clinical trial once it has obtained the results of the data from the first implantation.
Reuters reports that Philippe Pouletty, director general of Truffle Capital, one of Carmat’s main shareholders, told i>Tele television, “Patients are still being chosen, but of course we will wait to hear a little more on the causes of the death of the first patient before transplanting another artificial heart.”
The company explained that its detailed analysis of the data is still being carried out. More than 4000 pieces of data are recorded every second, it said. These include inputs from the artificial heart itself, its control console, and their respective power supplies.
Also of great interest are the very complex interactions between the weakened heart of the patient and the prosthesis. At the current time, Carmat says, there is no single explanation, only hypotheses that will be substantiated or not in the coming weeks by in-house and external experts. The results of the analyses of the first implantation, and the subsequent implantations, will be reviewed by the Data and Safety Monitoring Board (DSMB).
From the company’s point of view, the first implantation was a success. The patient survived for 74 days within the framework of a trial where the benchmark for success was 30 days. Carmat says that the approved medical centers are continuing to assess next patients for the ongoing clinical trial.
Pouletty said that the data analysis would be complete within “a few weeks.” The company has previously stated that if it passed this first safety test, it intends to fit the device into about 20 more patients with less severe heart failure later this year. It hopes to apply for CE Marking to market its device in Europe by 2015.
Stephen Levy is a contributor to Qmed and MPMN.
SOURCE
http://www.qmed.com/news/carmat-investigates-death-first-artificial-heart-recipient?cid=nl.qmed02
UPDATED on 3/6/2014
Artificial heart patient in France dies – Frenchman died 75 days after surgery
Thomson Reuters Posted: Mar 04, 2014 5:11 PM ET Last Updated: Mar 04, 2014 5:12 PM ET
The first patient fitted with an artificial heart made by the French company Carmat has died, the hospital that had performed the transplant in December has announced.
 Carmat’s bioprosthetic device is designed to replace the real heart for as much as five years, mimicking nature’s work using biological materials and sensors. (Benoit Tessier/Reuters)
Carmat’s bioprosthetic device is designed to replace the real heart for as much as five years, mimicking nature’s work using biological materials and sensors. (Benoit Tessier/Reuters)The 76-year-old man died on Sunday, 75 days after the operation, the Georges Pompidou European Hospital in Paris said in a statement, adding that the cause of his death could not be known for sure at this stage.
When he was fitted with the device, the man was suffering from terminal heart failure, when the sick heart can no longer pump enough blood to sustain the body, and was said to have only a few weeks, or even days, to live.
Carmat’s bioprosthetic device is designed to replace the real heart for as much as five years, mimicking nature’s work using biological materials and sensors. It aims to help the thousands of patients who die each year while awaiting a donor, and reducing the side-effects associated with transplants.
“Carmat wishes to pay tribute to the courage and the pioneering role of this patient and his family, as well as the medical team’s dedication,” a company spokeswoman said.
She stressed that it was premature to draw any conclusions on Carmat’s artificial heart at this stage.
Three more patients in France with terminal heart failure are due to be fitted with the device. The clinical trial will be considered a success if the patients survive with the implant for at least a month.
If it passes the test, Carmat has said it would fit the device into about 20 patients with less severe heart failure.
Extending life
“The doctors directly involved in the post-surgical care wish to highlight the value of the lessons learned from this first clinical trial, with regard to the selection of the patient, his surveillance, the prevention and treatment of difficulties encountered,” the hospital said in its statement.
An in-depth analysis of the medical and technical data gathered since the patient’s operation will be needed to establish the cause of his death, the hospital added.
Carmat estimates around 100,000 patients in the United States and Europe could benefit from its artificial heart, a market worth more than $12 billion.
Among Carmat’s competitors for artificial heart implants are privately-held SynCardia Systems and Abiomed, both of the United States.
SynCardia’s artificial heart is the only one approved both in the United States and the European Union and has been implanted in more than 1,200 patients to keep them waiting for a heart from a matching donor. The longest a patient has lived with the device is just under four years prior to a transplant.
Carmat’s heart is designed to serve not as a bridge to transplant but as a permanent implant, extending life for terminally ill patients who cannot hope for a real organ, generally because they are too old and donors too scarce.
Carmat’s shares, which have risen nearly five-fold since floating on the Paris stock market in 2010, closed at 95 euros before Monday’s news, giving the company a market capitalization of around 407 million euros
December 20, 2013 12:11 pm by Staff
 PARIS (Reuters) – France’s Carmat said on Friday it had carried out the first human implantation of its artificial heart.The operation, performed on Wednesday at the Georges Pompidou European Hospital in Paris, went smoothly, Carmat said in a statement, adding that the patient was being monitored in the intensive care unit but was awake and talking.(Reporting by Natalie Huet; editing by Mark John)
PARIS (Reuters) – France’s Carmat said on Friday it had carried out the first human implantation of its artificial heart.The operation, performed on Wednesday at the Georges Pompidou European Hospital in Paris, went smoothly, Carmat said in a statement, adding that the patient was being monitored in the intensive care unit but was awake and talking.(Reporting by Natalie Huet; editing by Mark John)
Read more: http://medcitynews.com/2013/12/first-artificial-heart-implanted-human/#ixzz2oLlFRyDG
An artificial heart from a French company is to be tested in patients in four countries.
By ANNE EISENBERG
Published: July 13, 2013 – The New York Times, Novelties
SCIENTISTS have long searched for a durable artificial heart that can work as efficiently as the one supplied by nature.
Carmat
Cow tissue will be used on surfaces of membranes — represented by elliptical shapes in this rendering — that touch the blood.
Now Carmat, a company based in Paris, has designed an artificial heart fashioned in part from cow tissue. The device, soon to be tested in patients with heart failure, is regulated by sensors, software and microelectronics. Its power will come from two external, wearable lithium-ion batteries.
Fifteen years in development, the heart has been approved for clinical trials at cardiac surgery centers in Belgium, Poland, Saudi Arabia and Slovenia, where staff members are receiving training and patients are being screened, said Dr. Piet Jansen, medical director at Carmat.
In France, where the device is not yet cleared for human implantation, regulators have requested more animal tests, Dr. Jansen said; those tests are continuing.
Artificial hearts aren’t new, of course, but the Carmat heart is unusual in its design, said Dr. Joseph Rogers, an associate professor at Duke University and medical director of its cardiac transplant and mechanical circulatory support program. Surfaces in the new heart that touch human blood are made from cow tissue instead of artificial materials like plastic that can cause problems like clotting.
“The way they’ve incorporated biological surfaces for any place that contacts blood is a really nice advantage,” Dr. Rogers said. “If they have this design right, this could be a game changer.” He added that it could lessen the need for anticoagulation medicines. (Dr. Rogers has no financial connections to Carmat.)
This is the first artificial heart to use cow-derived materials — specifically, tissue from the pericardial sac that surrounds the heart. Biological tissue has been used in earlier mechanical blood pumps only in valves, Dr. Rogers said.
Thousands of people in the United States need a replacement heart, said Dr. Lynne Warner Stevenson, a professor at Harvard Medical School and director of the cardiomyopathy and heart-failure program at Brigham and Women’s Hospital in Boston. “It’s estimated that if we had enough donor hearts to go around, 100,000 to 150,000 people in the United States with heart failure would benefit,” she said. “Transplants work best, but we have only 2,000 or so adult hearts” that are available each year, she said. “It’s a huge problem.”
There are long-established options for patients while they await transplants, Dr. Stevenson said, including installing an artificial heart made by SynCardia until a donor heart is available.
When the natural heart is partly damaged or diseased, patients might keep it and have a mechanical aid implanted to bolster blood flow. Such pumps — especially those that aid the left side of the heart (LVAD)— are in wide use both as a bridge to a transplant and for lifetime therapy.
A totally artificial heart for extended use would be of great value, but it’s far too early to know if the Carmat heart, as yet untried in humans, will be that device. “The whole history of mechanical devices is that people thought they had devices where blood wouldn’t clot. But they didn’t,” Dr. Stevenson said.
Dr. Jansen said that the cost of the Carmat heart would be about $200,000 and that he did not expect it to be brought to market in Europe before the end of 2014. Once the company gains momentum with its European clinical studies, he said, it plans to start working through the regulatory process in the United States.
The Carmat heart has two chambers, each divided by a membrane. That membrane has cow tissue on one side — the side that is in contact with blood — and polyurethane on the other side, which touches the miniaturized pumping system of motors and hydraulic fluids that changes the membrane’s shape. (The motion of the membrane pushes the blood out to the body.) The embedded electronics and software adjust the rate of blood flow. Patients can wear the batteries under the arm in a holster, or in a belt, among other options.
Cow tissue is also used for the heart’s artificial valves, which were created by Dr. Alain Carpentier, a cardiac surgeon and a pioneer of heart valve repair who is also a co-founder of Carmat and its scientific director. Such valves have been used in heart-valve replacement surgery for decades. The cow tissue is chemically treated so that it is sterile and biologically inert.
The heart’s design and development relied heavily on aerospace testing strategies by EADS, the European Aeronautic Defense and Space Company, one of Carmat’s backers, Dr. Jansen said. Even so, duplicating the durability of a human heart will not be easy, said Dr. Robert Kormos, director of the artificial heart program at the University of Pittsburgh Medical Center and co-director of its heart transplant program.
“We can test these pumps on the bench in the laboratory, and in animals, but there is no true long-term data until you implant them in people for trials,” he said.
DR. JANSEN said that one design requirement for the heart was that it last five years. The company has been doing bench tests to see whether the new heart will stand up to that level of wear and tear. “Whether it lasts five years in the patient we will have to prove clinically,” he said.
Dr. Stevenson of Harvard is optimistic about the new device.
“Innovation is what we need,” she said. “This new device is exciting. I applaud the pioneers who developed it, and the patients and families who will go down this path for the first time.”
A version of this article appeared in print on July 14, 2013, on page BU3 of the New York edition with the headline: The Artificial Heart Is Getting a Bovine Boost.
Mechanical Circulatory Assist Devices as a Bridge to Heart Transplantation or as “Destination Therapy“: Options for Patients in Advanced Heart Failure
By Larry H Bernstein, MD, FCAP
A total artificial heart (TAH) is a device that replaces the two ventricles of the heart. Those who benefit from a TAH usually have end-stage heart failure. Since the condition is so severe that the heart can’t pump enough blood to meet the body’s needs, all treatments, except heart transplant, have failed.
The TAH is attached the atria, and mechanical valves are between the TAH and the atria functioning like the heart’s valves, controlling the flow of blood in pulmonary and systemic circulation.
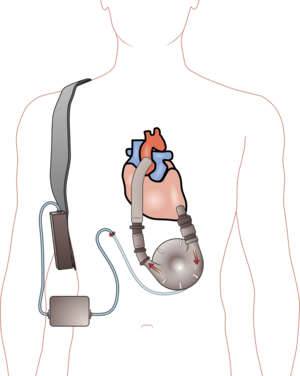
Currently, the two types of TAHs are the CardioWest and the AbioCor. The main difference between these TAHs is that the CardioWest is connected to an outside power source. The CardioWest has tubes that, through holes in the abdomen, run from inside the chest to an outside power source.
CardioWest Total Artificial Heart
Figure A shows a CardioWest TAH. Tubes exit the body and connect to a machine that powers the TAH and controls how it works.
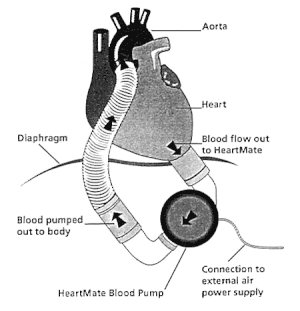
The AbioCor TAH is completely contained inside the chest. A battery powers this TAH, and the battery is charged through the skin with a special magnetic charger. Energy from the external charger reaches the internal battery through an energy transfer device called transcutaneous energy transmission, or TET. An implanted TET device is connected to the implanted battery. An external TET coil is connected to the external charger. Also, an implanted controller monitors and controls the pumping speed of the heart.
AbioCor Total Artificial Heart
Figure B shows an AbioCor TAH and the internal devices that control how it works.
A TAH usually extends life for months beyond what is expected with end-stage heart failure. It can keep one alive while waiting for a donor heart. It is a challenge for surgeons to implant, and it can cause complications. TAHs are devices used only in a small number of people.
There is a Difference Between Artificial Heart & Ventricular Assist Device
(see Michael Paul Maupin, eHow Contributor)
http://www.ehow.com/facts_6713118_difference-_amp_-ventricular-assist-devices.html#ixzz2a5BH465n
A ventricular assist device (VAD) utilizes the patient’s own heart, and it operates as a bridge device until a donor heart is procured for transplant. A TAH replaces a patient’s explanted heart. The VAD is grafted onto a patient’s left ventricle, boosting the impaired ventricular function. A VAD is either continuous or pulsatile in function. In a continuous VAD, blood is circulated through the heart like water through a hose. A pulsatile VAD more mimics the expulsion of blood in rhythmic patterns.
http://www.ehow.com/facts_6713118_difference-_amp_-ventricular-assist-devices.html#ixzz2a5Bcbszh
On the other hand, an artificial heart completely replaces the human heart. The device functions in every way a healthy human heart would in the absence of cardiac disease. The TAH creates the same pattern of squeeze-and-release seen in a real heart.
http://www.ehow.com/facts_6713118_difference-_amp_-ventricular-assist-devices.html#ixzz2a5Bn6xaR
As of 2010, the longest any human being has lived with an artificial heart is 21 months. In comparison, documentation exists in which a VAD recipient was still enjoying a vigorous quality of life after seven years.
Read more: http://www.ehow.com/facts_6713118_difference-_amp_-ventricular-assist-devices.html#ixzz2a5C1cPFV
The SynCardia temporary Total Artificial Heart
(An artificial heart displayed at the London Science Museum)
http://www.wikipedia.com/Artificial Heart
An artificial heart is a device is typically used to bridge the time to heart transplantation, or to permanently replace the heart in case heart transplantation is impossible. The first artificial heart to be successfully implanted in a human was the Jarvik-7, designed and implemented by Robert Jarvik in 1982, but the first two patients to receive these hearts survived 112 (4 m) and 620 (21 m) days beyond their surgeries, respectively.[1]
Jarvik-7
It has already been stated that a TAH is distinct from a VAD, both used to support a failing heart. It is also distinct from a cardiopulmonary bypass machine, which is an external device used to provide the functions of both the heart and lungs, and it is used for only a few hours during cardiac bypass surgery.
Origin and Development of the Heart-Lung Bypass
A synthetic replacement for the severely failing heart would be expected to lower the need for heart transplants, because the demand for organs always greatly exceeds supply. However, the first devices had problems with reactivity to synthetic materials and power supplies. For example, the Jarvik models were not created of a material that the human body would accept. This problem was improved when Dayton, Ohio’s Ival O. Salyer, along with various colleagues, developed a polymer material that the human body would not necessarily reject.
Prior to Jarvik-7, 41-year-old Henry Opitek made medical history in 1952 at Harper Hospital, Wayne State University in Detroit, Michigan when Dr. Forest Dewey Dodrill used the Dodrill-GMR heart machine to bypass Henry Opitek’s left ventricle for 50 minutes while he repaired the mitral valve. [2][3] In this case In Dr. Dodrill’s post-operative report, he notes, “To our knowledge, this is the first instance of survival of a patient when a mechanical heart mechanism was used to take over the complete body function of maintaining the blood supply of the body while the heart was open and operated on.”[4] A heart-lung machine was used in 1953 during a successful open heart surgery by Dr. John Heysham Gibbon, the inventor, who performed the operation with the heart-lung substitute (distinct from an artificial heart substitute).
Designs of total artificial hearts
A precursor to the modern artificial heart pump was built by doctors William Sewell and William Glenn of the Yale School of Medicine in 1949 using an assortment of parts, and successfully bypassed the heart of a dog for more than an hour.[5]
The first patent for an artificial heart was held by Paul Winchell invented and Dr. Henry Heimlich (of the Heimlich Maneuver), which preceded the Jarvik heart. On December 12, 1957, Dr. Willem Johan Kolff, the world’s most prolific inventor of artificial organs, implanted an artificial heart into a dog at Cleveland Clinic before he relocated to Salt Lake City, Utah, where there was established an Institute for artificial organs. There, more than 200 physicians, engineers, students and faculty at the University of Utah Division of Artificial Organs developed, tested and improved Dr. Kolff’s artificial heart. To help manage his many endeavors, Dr. Kolff assigned project managers. Each project was named after its manager. Graduate student Robert Jarvik was the project manager for the artificial heart, which was subsequently renamed the Jarvik 7.
In 1958, Domingo Liotta initiated the studies of TAH replacement at Lyon, France, and in 1959–60 at the National University of Córdoba, Argentina. He presented his work at the meeting of the American Society for Artificial Internal Organs held in Atlantic City in March 1961. At that meeting, Dr. Liotta described the implantation of three types of orthotopic (inside the pericardial sac) TAHs in dogs, each of which used a different source of external energy: an implantable electric motor, an implantable rotating pump with an external electric motor, and a pneumatic pump.[6][7]
In 1964, the National Institutes of Health started the Artificial Heart Program, with the goal of putting a man-made organ into a human by the end of the decade.[8] The first success followed in February 1966, when Dr. Adrian Kantrowitz performed the world’s first permanent implantation of a partial mechanical heart (left ventricular assist device) at Maimonides Medical Center, Brooklyn, NY.[9] He relocated to Detroit’s Sinai and Wayne Stae University.
In 1981, Dr. William DeVries submitted a request to the FDA to implant the Jarvik 7 into a human being. On December 2, 1982, Dr. Kolff implanted the Jarvik 7 artificial heart into Barney Clark, who was suffering from severe congestive heart failure. With Clark tethered to an external 400 lb pneumatic compressor, he suffered prolonged periods of confusion, a number of instances of bleeding, and asked several times to be allowed to die.[10]
Total Artificial Heart (TAH)
On April 4, 1969, Domingo Liotta and Denton A. Cooley replaced a dying man’s heart with a mechanical heart inside the chest at The Texas Heart Institute in Houston as a bridge for a transplant. The patient woke up and recovered well. After 64 hours, the pneumatic-powered artificial heart was removed and replaced by a donor heart. However thirty-two hours after transplantation, the patient died of what was later proved to be an acute pulmonary infection, extended to both lungs, caused by fungi, most likely caused by an immunosuppressive drug complication.[11]
The original prototype of Liotta-Cooley artificial heart used in this historic operation is prominently displayed in the Smithsonian Institution’s National Museum of American History “Treasures of American History” exhibit in Washington, D.C..[12]
Permanent Pneumatic Total Artificial Heart (TAH)
The eighty-fifth clinical use of an artificial heart designed for permanent implantation rather than a bridge to transplant occurred in 1982 at the University of Utah. Artificial kidney pioneer Dr. Willem Johan Kolff started the Utah artificial organs program in 1967.[13] There, physician-engineer Dr. Clifford Kwan-Gett invented two components of an integrated pneumatic artificial heart system: a ventricle with hemispherical diaphragms that did not crush red blood cells (a problem with previous artificial hearts) and an external heart driver that inherently regulated blood flow without needing complex control systems.[14] Dr. Robert Jarvik combined several modifications of the original: an ovoid shape to fit inside the human chest, a more blood-compatible polyurethane developed by biomedical engineer Dr. Donald Lyman, and a fabrication method by Kwan-Gett that made the inside of the ventricles smooth and seamless to reduce dangerous stroke-causing blood clots.[16]
Today, the modern version of the Jarvik 7 is known as the SynCardia temporary CardioWest Total Artificial Heart. It has been implanted in more than 800 people as a bridge to transplantation.
In the mid-1980s, artificial hearts were powered by dishwasher-sized pneumatic power sources whose lineage went back to Alpha-Laval milking machines and required two catheters to cross the abdominal wall to carry the pneumatic pulses to the implanted heart. The National Heart, Lung, and Blood Institute opened a competition for implantable electrically powered artificial hearts funding Cleveland Clinic in Cleveland, Ohio; the College of Medicine of Pennsylvania State University (Penn State Hershey Medical Center) in Hershey, Pennsylvania; and AbioMed, Inc. of Danvers, Massachusetts.
Polymeric trileaflet valves ensure unidirectional blood flow with a low pressure gradient and good longevity. State-of-the-art transcutaneous energy transfer eliminates the need for electric wires crossing the chest wall.
AbioCor
The first AbioCor to be surgically implanted in a patient was on July 3, 2001.[17] The AbioCor is made of titanium and plastic with a weight of two pounds, and its internal battery can be recharged with a transduction device that sends power through the skin.[17] The internal battery lasts for a half hour, and a wearable external battery pack lasts for four hours.[18] The FDA announced on September 5, 2006, that the AbioCor, intended for critically ill patients who can not receive a heart transplant[19] could be implanted after the device had been tested on 15 patients.[19] But limitations of the current AbioCor are that its size makes it suitable for only about 50% of the male population, and its useful life is only 1–2 years.[20] AbioMed designed a smaller, more stable heart, the AbioCor II, by combining its valved ventricles with the control technology and roller screw developed at Penn State. This pump, which should be implantable in most men and 50% of women with a life span of up to five years,[20] had animal trials in 2005, and the company hoped to get FDA approval for human use in 2008.[21]
Intrathoracic Pump (LVAD)
On July 19, 1963, E. Stanley Crawford and Domingo Liotta implanted the first clinical Left Ventricular Assist Device (LVAD) at The Methodist Hospital in Houston, Texas, in a patient who had a cardiac arrest after surgery. The patient survived for four days under mechanical support but did not recover from the complications of the cardiac arrest.
On April 21, 1966, Michael DeBakey and Liotta implanted the first clinical LVAD in a paracorporeal position (where the external pump rests at the side of the patient) at The Methodist Hospital in Houston, in a patient experiencing cardiogenic shock after heart surgery. The patient developed neurological and pulmonary complications and died after few days of mechanical support. In October 1966, DeBakey and Liotta implanted the paracorporeal Liotta-DeBakey LVAD in a new patient who recovered well and was discharged from the hospital after 10 days, marking the first successful use of an LVAD for postcardiotomy shock.
Recent developments
In June 1996, a 46-year-old Taiwanese American Mr. Yao ST received the world’s first total artificial heart implantation done by Dr. Jeng Wei at Cheng-Hsin General Hospital[26] in the Republic of China (Taiwan). This technologically advanced pneumatic Phoenix-7 Total Artificial Heart was manufactured by a Taiwanese dentist Kelvin K. Cheng, a Chinese physican T. M. Kao and colleagues at the Taiwan TAH Research Center in Tainan, Republic of China (Taiwan). With this experimental artificial heart, the patient’s BP was maintained at 90-100/40-55 mmHg and cardiac output at 4.2-5.8 L/min. After 15 days of bridging, Mr. Yao received combined heart and kidney transplantation. As of March 2013, he is still very well and is currently living in San Francisco, USA. Mr. Yao ST is the world first successful combined heart and kidney transplantation patient after bridging with total artificial heart.[27]
In August 2006, an artificial heart was implanted into a 15-year-old girl at the Stollery Children’s Hospital in Edmonton, Alberta. It was intended to act as a temporary fixture until a donor heart could be found. Instead, the artificial heart (called a Berlin Heart) allowed for natural processes to occur and her heart healed on its own. After 146 days, the Berlin Heart was removed, and the girl’s heart was able to function properly on its own.[22]
On December 16, 2011 the Berlin Heart, a ventricular assist intended for children age 16 and under, gained U.S. FDA approval. The device has since been successfully implanted in several children including a 4-year-old Honduran girl at Children’s Hospital Boston.[23]
In 2012, a study published in the New England Journal of Medicine compared the Berlin Heart to extracorporeal membrane oxygenation (ECMO) and concluded that “a ventricular assist device available in several sizes for use in children as a bridge to heart transplantation [such as the Berlin Heart] was associated with a significantly higher rate of survival as compared with ECMO.”[24] The study’s primary author, Dr. Charles D. Fraser, Jr., surgeon in chief at Texas Children’s Hospital, explained: “With the Berlin Heart, we have a more effective therapy to offer patients earlier in the management of their heart failure. ..This is a giant step forward.” [25]
Total artificial heart (TAH) invention abroad
On October 27, 2008, French professor and leading heart transplant specialist Alain F. Carpentier announced that a fully implantable artificial heart will be ready for clinical trial by 2011 and for alternative transplant in 2013. It was developed and will be manufactured by him, biomedical firm CARMAT SA, and venture capital firm Truffle Capital. The prototype uses embedded electronic sensors and is made from chemically treated animal tissues, called “biomaterials”, or a “pseudo-skin” of biosynthetic, microporous materials.[28] According to an interview of the professor Alain Carpentier in Paris (2011), a number of leading cardiac clinics already conducted successful partial replacement of the organic components of the artificial heart, for example, replacing valves, large vessels, atria, ventricles. In addition to cardio-surgery, there is the medico-psychological aspect of an artificial heart. A quarter of patients in the postoperative period after prosthetic valvular surgery developed specific psychopathological symptoms, which later received the name Skumin syndrome in 1978. It is possible that a similar problem will be discovered when conducting large-scale operations to implant an artificial heart.[29]
Another U.S. team with a prototype called 2005 MagScrew Total Artificial Heart, including Japan and South Korea researchers are racing to produce similar projects.[30][31][32]
In August 2010, 50-year-old Angelo Tigano of Fairfield, New South Wales, Australia, had his failing heart removed in a five-hour operation and it was replaced with the SynCardia temporary Total Artificial Heart by surgeon Dr Phillip Spratt, head of the heart transplant unit at St Vincent’s Hospital, Sydney.[33]
On 12 March 2011, an experimental artificial heart was implanted in 55-year-old Craig Lewis at The Texas Heart Institute in Houston by Drs. O. H. Frazier and William Cohn. The device is a combination of two modified HeartMate II pumps that is currently undergoing bovine trials.[34]
On 9 June 2011, 40 year old Matthew Green was implanted with the SynCardia temporary Total Artificial Heart in a seven hour operation at Papworth Hospital. He was the first Briton to leave hospital supported by an artificial Heart on 2 August 2011.[35]
A centrifugal pump[36][37] or an axial-flow pump[38][39] can be used as an artificial heart, resulting in the patient being alive without a pulse.
Imachi et al. described a centrifugal artificial heart which alternately pumps the pulmonary circulation and the systemic circulation, causing a pulse.[40]
Heart Assist Devices
Patients who have some remaining heart function but who can no longer live normally may be candidates for ventricular assist devices (VAD), which do not replace the human heart but complement it by taking up much of the function.
The first Left Ventricular Assist Device (LVAD) system was created by Domingo Liotta at Baylor College of Medicine in Houston in 1962.[41]
Another VAD, the Kantrowitz CardioVad, designed by Adrian Kantrowitz boosts the native heart by taking up over 50% of its function.[42] Additionally, the VAD can help patients on the wait list for a heart transplant. In a young person, this device could delay the need for a transplant by 10–15 years, or even allow the heart to recover, in which case the VAD can be removed.[42] The artificial heart is powered by a battery that needs to be changed several times while still working.
The first heart assist device was approved by the FDA in 1994, and two more received approval in 1998.[43] While the original assist devices emulated the pulsating heart, newer versions, such as the Heartmate II,[44] developed by The Texas Heart Institute of Houston, provide continuous flow. These pumps (which may be centrifugal or axial flow) are smaller and potentially more durable and last longer than the current generation of total heart replacement pumps. A major advantage of a VAD is that the patient keeps the natural heart, which may provide enough support to keep the patient alive until a solution to the problem is implemented.
Suffering from end-stage heart failure, former Vice President Dick Cheney underwent a procedure in July 2010 to have a VAD implanted at INOVA Fairfax Hospital, in Fairfax Virginia. In 2012, he received a heart transplant at age 71 after 20 months on a waiting list.
REFERENCES
1^ American Heart Association. The Mechanical Heart celebrates 50 lifesaving years. 22 10 2002. 9 Feb 2008 <http://www.americanheart.org/presenter.jhtml;jsessionid=EFNP3NSFUBXLICQFCXQCDSQ?identifier=3005888>
2^ Stephenson, Larry W, et al. “The Michigan Heart: The World’s First Successful Open Heart Operation?” Journal of Cardiac Surgery 17.3 (2002): 238–246.
3^ Lavietes, Stuart. William Glenn, 88, Surgeon Who Invented Heart Procedure, The New York Times, March 17, 2003. Accessed May 21, 2009.
4^ Artificial Heart in the chest: Preliminary report. Trans. Amer. Soc. Inter. Organs, 1961, 7:318
5^ Ablation experimentale et replacement du coeur par un coer artificial intra-thoracique. Lyon Cirurgical, 1961, 57:704
6^ Sandeep Jauhar, M.D., Ph.D.: The Artificial Heart. New England Journal of Medicine (2004): 542–544.
7^ http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2676518/, NCBI In Memoriam Dr. Adrian Kantrowitz
8^ Barron H. Lerner, MD, PhD (December 1, 2007). “The 25th Anniversary of Barney Clark’s Artificial Heart”. Celebrity Health. HealthDiaries.com. Retrieved 15 November 2010.
9^ Orthotopic cardiac prosthesis for two-staged cardiac replacement. Am J Cardio 1969; 24:723–730.
10^ “Treasures of American History”, National Museum of American History
11^ Spare Parts: Organ Replacement in American Society. Renee C. Fox and Judith P. Swazey. New York: Oxford University Press; 1992, pp. 102–104
12^ Kwan-Gett CS, Van Kampen KR, Kawai J, Eastwood N, Kolff WJ. “Results of total artificial heart implantation in calves.” Journal of Thoracic and Cardiovascular Surgery. 1971 Dec; 62(6):880–889.
13^ “Winchell’s Heart”. Time. March 12, 1973. Retrieved April 25, 2010.
14^ Kolff
15^ a b “Patient gets first totally implanted artificial heart”. CNN.com. 2001-07-03. Archived from the original on 7 June 2008. Retrieved 2008-07-13.
16^ “AbioCor FAQs”. AbioMed. Archived from the original on 3 July 2008. Retrieved 2008-07-13.
17^ a b “FDA Approves First Totally Implanted Permanent Artificial Heart for Humanitarian Uses”. FDA.gov. 2006-09-05. Retrieved 2008-07-13.
18^ a b “Will We Merge With Machines?”. popsci.com. 2005-08-01. Archived from the original on 19 July 2008. Retrieved 2008-07-13.
19^ “14th Artificial Heart Patient Dies: A Newsmaker Interview With Robert Kung, PhD”. medscape.com. 2004-11-11. Retrieved 2008-07-13.
20^ Capital Health: One year later: Berlin Heart bridges patient back to health (August 28, 2007), Capital Health, Edmonton (archived from [1] the original) on 2007-10-01).
21^ approved Berlin Heart helps patients waiting for a transplant (December 30, 2011), Children’s Hospital Boston.
22^ http://www.nejm.org/doi/pdf/10.1056/NEJMoa1014164
23^ http://www.texaschildrens.org/About-Us/News/Berlin-Heart-NEJM-2012/
24^ Cheng-Hsin General Hospital
25^ J. Wei, K. K. Cheng, D. Y. Tung, C. Y. Chang, W. M. Wan, Y. C. Chuang: Successful Use of Phoenix-7 Total Artificial Heart. Transplantation Proceedings, 1998, 30:3403-4
26^ The Carmat Heart,- The technology behind the prosthesis
27^ “About artificial heart”. Heart For Your Soul. Retrieved 2011-02-19.
28^ Total artificial heart to be ready by 2011: research team, news.yahoo.com
29^ Scientists develop artificial heart that beats like the real thing, timesonline.co.uk
30-^ Total artificial heart to be ready by 2011: research team, afp.google.com
31^ Sydney man receives Total Artificial Heart, dailyTelegraph.com.au
32^ Berger, Eric. “New artificial heart ‘a leap forward'”. Houston Chronicle. Retrieved 23 March 2011.
33^ “Plastic heart gives dad Matthew Green new lease of life”. BBC News. August 2, 2011.
34^ Black, Rosemary (January 5, 2011). “Former vice president Dick Cheney now has no pulse”. Daily News (New York).
35^ http://www.scribd.com/doc/21241693/Pulseless-Pumps-Artificial-Hearts
36^ The pulseless life
37^ Dan Baum: No Pulse: How Doctors Reinvented The Human Heart. 2012-02-29.
38^ ‘#A new pulsatile total artificial heart using a single centrifugal pump., K. Imachi, T. Chinzei, Y. Abe, K. Mabuchi, K. Imanishi, T. Yonezawa, A. Kouno, T. Ono, K. Atsumi, T. Isoyama, et al.. Institute of Medical Electronics, Faculty of Medicine, University of Tokyo, Japan.
39^ Prolonged Assisted circulation after cardiac or aortic surgery. Prolonged partial left ventricular bypass by means of intracorporeal circulation. This paper was finalist in The Young Investigators Award Contest of the American College of Cardiology. Denver, May 1962 Am. J. Cardiol. 1963, 12:399–404
40^ a b Mitka, Mike. “Midwest Trials of Heart-Assist Device.” Journal of the American Medical Association 286.21 (2001): 2661.
41^ FDA APPROVES TWO PORTABLE HEART-ASSIST DEVICES at FDA.gov
42^ An Artificial Heart That Doesn’t Beat at TechnologyReview.com
How does an artificial heart work?
The development and operation of these life-saving devices requires understanding and application of a combination of biology, materials science and physics.
Institute of Physics website http://www.physics.org/article-questions.asp?id=74
The artficial heart
Image: Syncardia Systems
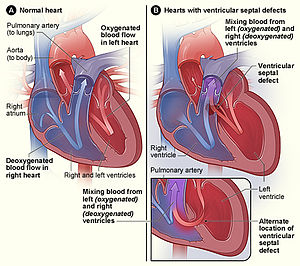
The right atrium collects blood and the right ventricle then pumps it to the lungs where it is oxygenated. The blood is then picked up by the left atrium and distributed around the body and brain by the left ventricle. Each side of the heart has a pair of valves – one pair per lung – controlling the flow of blood.
Artificial hearts can now completely, if temporarily, replace the ventricles and valves with a device made of plastic or other man-made materials, which does the job of pumping blood around.
The type of artificial heart made by Syncardia Systems, works by using a pump carried externally in a backpack – previously, patients would have to be connected to a large, immobile pump and would not have the freedom to move around.
The NHS Choices website explains that tubes connecting the heart to the pump “send pulses of air into two expandable, balloon-like sacs in the artificial ventricles, forcing out blood in much the same way that a beating heart would”.
Other models such as that produced by AbioMed use an internal pump and battery, which can be charged via transcutaneous energy transmission – a method of transferring power under the skin without having to penetrate it, thereby decreasing the chance of infection.
Energy transmission
In the artificial hearts produced by AbioMed, an electronics package is implanted in the abdomen of the recipient of the transplant to monitor and control the pumping of the heart.
Power is supplied from an external source to components under the skin, without penetrating it, using inductive electromagnetic coupling – the same principle as used by transformers to transfer electricity between different circuits, as in the national grid.
At their simplest, systems of transcutaneous energy transmission will use an external power supply connected to an external coil of wire, generating a magnetic field in it. This, in turn, produces an induced voltage in a second coil implanted under the skin, and a rectifier is used to change this alternating current into direct current that can be used to power the electronics of the heart and its controller.
Though simple in theory, in practice there are complications that arise from the need to keep the two coils aligned correctly as the patient moves, in delivering the correct level of power so that there is no excess dissipated as heat to potentially damage surrounding tissue in the patient’s body, and in making the components small enough to be carried around without too much discomfort.
Monitoring blood flow
A replacement heart needs to be able to monitor the flow of blood to regulate its pumping and ensure that the correct amount of blood is delivered around the body.
Quicker pumping is required when the transplant recipient is more active, whereas the opposite is true while he or she is resting.
Blood-flow monitors make use of ultrasound – they bounce high-frequency sound waves off blood cells coming out of the heart, the volume and speed can be measured using similar basic principles to those behind radar.
Ultrasound is used because it can monitor the flow of blood without having to be in contact with it.
Appropriate materials
Artificial hearts need to be made of light but durable materials – the Syncardia version is plastic whereas that made by AbioMed is a combination of titanium and a specially developed polyurethane, called ‘Angioflex’.
Although the Abiomed heart is designed to have as few moving parts as possible, those that it does have are made from Angioflex and are tested to ensure that they are safe for contact with blood and capable of withstanding beating 100 000 times a day for years on end.
Materials scientists can develop substances with specific properties by manipulating the constituent elements and the way in which they are processed. Materials are characterised using various techniques from condensed-matter physics including electron microscopy, x-ray diffraction and neutron diffraction.
Because they were still quite large, the first devices produced were limited to around half the male population – those with the largest chest cavities. A newer, smaller, model is intended to extend their availability to smaller people.
An artificial heart being produced by the French medical company Carmat and expected to be available by 2013 will use chemically treated animal tissue to help avoid rejection by the host’s immune system. Aerospace engineers from Airbus were also involved in its development.
Artificial hearts combine, and improve upon, many existing physics ideas to produce a piece of technology that saves lives – although they are currently only approved as a stopgap until a donor heart can be found.
Expressions of Experience: Heart Assist Devices
Video interview with O. H. “Bud” Frazier, MD; Chief, Center for Cardiac Support; Director, Cardiovascular Surgery Research; and Co-Director, Cullen Cardiovascular Research Laboratories, at Texas Heart Institute.
O. H. “Bud” Frazier, MD, on his inspiration for developing treatments for heart failure at the Texas Heart Institute.
The Texas Heart Institute is a world leader in the development, testing and application of heart assist devices. Our goal for the surgical research conducted here is to develop and determine the best assist device to use for each individual patient. Devices may be referred to as mechanical assist devices, ventricular assist devices (VAD), left ventricular assist devices (LVAD), total artificial hearts (TAH), or simply heart pumps.
January 23, 2013
Keeping hearts pumping Dr. Bud Frazier and Dr. Billy Cohn with heart pump BiVacor. [Photo credit Mayra Beltran, Houston Chronicle]
Doctors push the limits of heart-pump technology in an effort to save lives. Dr. Bud Frazier often tells a story about when he was a medical student in the 1960s . . . Frazier had this thought: If I can keep a man alive with my hand, why can’t we make a pump that we can pull off of the shelf to do the same thing? Dr. Billy Cohn, another physician who works at the cutting edge of heart pump technology, likes to use the history of human flight as an analogy for the evolution in his field. Experimenters in both domains had to give up the idea of bio-mimicry to advance the technology. “It is similar to when man first tried to build a flying machine with flapping wings that mimic the birds. It is obvious now that fixed wings were the way to go,” he says. “We think it is the same with the nonpulsatile pump, which, because it has only one moving part, is much more durable.” – Houston Chronicle [Photo credit Mayra Beltran]
January 13, 2013
BiVACOR artificial heart device
Australian engineer Daniel Timm’s revolutionary device to be developed at THI. “I think we’re beyond the Kitty Hawk stage with this,” – Drs. Bud Frazier and Billy Cohn. Read Eric Berger’s Houston Chronicle article.
November 20, 2012
FDA Approves HeartWare LVAD for HF
The FDA gave the green light for the HeartWare Ventricular Assist System as a bridge to heart transplantation in patients with heart failure. “The miniaturized device with an integrated inflow cannula is placed within the pericardial sac . . . simplifying the surgical insertion,” said O.H. “Bud” Frazier, MD, of Texas Heart Institute. Read the full story from medpagetoday.com.
Drs. Bud Frazier & Billy Cohn TEDMED 2012
Is this the future of artificial hearts?
At TEDMED 2012, Bud Frazier and Billy Cohn of the Texas Heart Institute preview a continuous-flow heart pump with minimal parts that works via a screw pump. Watch the VIDEO.
Cameron Engineers, THI researchers collaborate on heart pump
Engineers and scientists at Cameron Manufacturing & Engineering have worked with THI researchers in developing a new heart pump. On March 1, 2012, Cameron donated $500,000 to Texas Heart Institute at St. Luke’s Episcopal Hospital to develop a prototype heart pump which could save countless lives.
Can Tiny Heart Pump Limit Heart Muscle Damage after STEMI?
Interventional cardiologists affiliated with THI at St. Luke’s recently implanted the first two patients in the nation with a tiny heart pump in a feasibility trial to determine the pump’s potential to limit damage to heart muscle following a STEMI (ST-elevation myocardial infarction). Read the full news release to learn about the FDA-approved trial and the first enrolled patients. (November 2011)
Miniature Heart Pump: Smaller May Be Better!
Dr. William “Billy” Cohn discusses recent advances in left ventricular assist devices (LVADs) and other mechanical circulatory blood pumps as they get smaller and more adaptable to individual patients. View the video of his presentation at the Pumps & Pipes Conference (15 minutes, December 2010).
Video: Artificial hearts giving hope, saving lives. (August 19, 2011)
Companion 2 and Freedom Drivers
C2 Driver Supports Total Artificial Heart Patients in the Hospital Until They Are Stable and Eligible for the Freedom® Portable Driver
The Companion 2 Driver, which can be docked in the Hospital Cart or Caddy, powers the SynCardia Total Artificial Heart from implant until the patient’s condition stabilizes. Once stable, patients who are eligible can be switched to the smaller, wearable Freedom® portable driver. The Companion 2 Driver, which can be docked in the Hospital Cart or Caddy, powers the SynCardia Total Artificial Heart from implant until the patient’s condition stabilizes. Once stable, patients who are eligible can be switched to the smaller, wearable Freedom® portable driver.
The Companion 2 (C2) Driver System, which powers the SynCardia temporary Total Artificial Heart in the hospital, was selected as the Silver Winner in the Critical-Care and Emergency Medicine Products category of the Medical Design Excellence Awards (MDEA) held on June 19 in Philadelphia.
“It is a tremendous honor to have one of our products selected as a winner for the second consecutive year,” said Michael Garippa, SynCardia Chairman/CEO/President. “Our Freedom® portable driver, the world’s first wearable power supply for the Total Artificial Heart, was selected as the Bronze Winner in the same category last year. These drivers support Total Artificial Heart patients from implant with the C2 through discharge with the Freedom.”
Once stable, patients who are eligible can be switched to the 13.5-pound Freedom portable driver. Patients who meet discharge criteria can then leave the hospital and wait for a matching donor heart at home and in their communities.
The Medical Design Excellence Awards are the industry’s premier design awards competition and is the only awards program exclusively recognizing contributions and advances in the design of medical products. Entries were evaluated on the basis of their design and engineering features, including innovative use of materials, user-related functions that improve healthcare delivery and change traditional medical attitudes or practices, features that provide enhanced benefits to the patient, and the ability to overcome design and engineering challenges to meet clinical objectives.
About the SynCardia temporary Total Artificial Heart
The SynCardia Total Artificial Heart is currently approved as a bridge to transplant for people suffering from end-stage heart failure affecting both sides of the heart (biventricular failure). There have been more than 1,200 implants of the Total Artificial Heart, accounting for more than 315 patient years of life on the device. It is the only device that eliminates the symptoms and source of end-stage biventricular failure. The TAH provides immediate, safe blood flow of up to 9.5 liters per minute through each ventricle. This high volume of blood flow helps speed the recovery of vital organs, helping make the patient a better transplant candidate.
Artificial Heart Devices used at Barnes-Jewish Hospital Washington University, St. Louis
The cardiac surgeons at the Barnes-Jewish & Washington University Heart & Vascular Center are one of the leading heart surgery teams in the nation. Our permanent and temporary artificial heart devices can dramatically improve symptoms of late-stage heart failure, and sometimes even provide long-term treatment.
Mechanical Circulatory Support
The field of mechanical circulatory support in the management of patients with heart failure has seen significant advances over the past few years. The heart failure program at Washington University and Barnes-Jewish Hospital utilizes the latest technology for both temporary and long-term mechanical support of the heart failure patient.
Temporary Support
Patients that experience severe symptoms of heart failure that cannot be stabilized with medical therapy may require a temporary support device. These implantable devices are usually placed in a cardiac catheterization lab by interventional cardiologists and/or cardiac surgeons. Temporary support devices typically serve to stabilize the patient until long-term mechanical support can be introduced. These devices include:
- intra-aortic balloon pump
- Impella 2.5, 4.0 and 5.0
- TandemHeart
- Thoratec CentriMag
Long-Term Mechanical Support
Patients may require long-term circulatory support either as a bridge to a heart transplant (bridge-to-transplant, or BTT) or as long-term treatment of heart failure in non-transplant candidates (destination therapy, or DT). The mechanical assist device program at Barnes-Jewish & Washington University Heart & Vascular Center is one of the largest programs in the country. The program has a multidisciplinary group of dedicated specialists to ensure excellent outcomes in this patient population. Currently available devices include both left ventricular assist devices (LVAD) and the total artificial heart:
- HeartMate II
- HeartWare HVAD
- Syncardia Total Artificial Heart
The cardiac surgeons at the Barnes-Jewish & Washington University Heart & Vascular Center are one of only 13 surgical teams in the country to implant the CardioWest™ temporary Total Artificial Heart (TAH-t) as a bridge-to-transplantation in specific heart transplant candidates.
The CardioWest™ TAH-t is an improved version of the Jarvik-7 Artificial Heart, which was first implanted in 1982. This unique technology allows us to treat patients who would not survive without full circulatory support. The CardioWest™ TAH-t completely replaces the patient’s diseased heart with a goal of restoring normal blood pressure, increasing cardiac output and giving organs such as the kidney and liver a chance to recover. As a result, patients become better candidates for transplantation. The program is currently involved in testing the Freedom portable driver which will allow patients to leave the hospital following implantation of the TAH.
An American designed Artificial Heart by ABIOMED, the Symphony model, assists in remodeling of heart tissue cells by design, as described in
Heart Remodeling by Design – Implantable Synchronized Cardiac Assist Device:Abiomed’s Symphony
SOURCE
Heart Remodeling by Design – Implantable Synchronized Cardiac Assist Device:Abiomed’s Symphony
Part II
Comparison of the Cardiac Operations involved in an Organ Transplant of a Donor’s Heart vs Implantation of an Artificial Heart
By Justin D Pearlman, MD, PhD, FACC
A heart donor is a patient deemed brain dead who had forethought (a designation on the driver’s license) or a designated decision-maker (Healthcare Proxy) elected to make the heart available to help save another person’s life. Every tissue in the body has proteins that render a unique signature or “smell” and every patient has a limited set of markers it will accept without a fight (the histocompatibility complex, and in particular, the human leukocyte antigen). The immune system is a major part of the body’s defenses against infection and abnormal tissues (cancer) which consists of cells trained to attack foreign protein chemistry and/or mark it for destruction with anti-bodies.
I. Heart Transplant of a Human Donor
The steps for heart transplant include:
(1) demonstration of need,
(2) identification of suitable donors,
(3) surviving while waiting for a suitable donor,
(4) surviving the removal of the damaged heart or heart and lungs to make room for the replacement (accomplished with a bypass pump),
(5) survival of the donor heart (or heart and lungs) pending preparation of the patient for receipt of the transplant,
(6) inserting the donor heart (or heart and lungs),
(7) taking the patient off the bypass pump and directing circulation through the transplant,
(8) recovery and healing,
(9) establishing and maintaining sufficient immune suppression to avoid rejection of the transplant,
(10) monitoring for functional losses or rejection.
(11) monitoring for cancer or infection,
(12) resuming enjoyment of life. Each year in the United states 800 patients die waiting for a transplant, while 2300 receive transplants.
The first heart transplant is credited to Vladimer Demikhov when he transplanted dog hearts in 1946; Dr. Shumway reported successful transplantation of the heart in 1966, and Dr. Christiaan Barnard performed the operation successfully on humans in 1967 (that patient lived 18 days). Replacing the heart with a donor heart is called orthotopic (true location) heart transplantation. Durability of a transplant improved markedly with the approval of the immune suppression medication ciclosporine. NOVA has created a shockwave video demonstrating the heart transplant operation: view video.
The actual transplantation requires only five or six lines of sutures (stitches):
- inferior and superior vena cava (venous input to the right ventricle),
- the main (or left and right) pulmonary arteries (delivery of blood from right ventricle to the lungs),
- the upper half of the original left atrium to route the 3-5 pulmonary veins to the left ventricle (return of blood from the lungs), and the
- aorta (to route blood from the left ventricle to the brain and body).
The donor heart harvesting typically includes a segment of the superior and inferior vena cava which feed
- the right atrium,
- the four pulmonary veins which feed the left atrium, and
- a portion of the pulmonary artery, and
- the aorta.
The heart is chilled to minimized its metabolic demands while it is disconnected and transferred.
The recipient heart explantation (removal of the bad heart) after the patient is supported by a bypass pump involves:
- cannulation (tubing placement) into the aorta,
- the superior vena cava and
- the inferior vena cava, then
- explantation leaving the posterior aspect of the left atrium and the posterolateral aspect of the right atrium in the recipient patient.
The left and right pulmonary veins of the donor are divided and the veins are threaded into the retained portion of the recipient left atrium. The inferor vena cava, superior vena cava, pulmonary artery, and aorta are respectively anastomosed (sewed onto the truncated portion of the corresponding native vessels end-to-end). Clots and air are flushed out and the patient is taken off bypass pump.
II. Artificial Heart: Implant of an Assist Device
Implantation of ventricular assist device or an artificial heart is easier than a heart transplant, but it has been challenging to match nature’s ability to place the pump and keep it powered and regulated. Also durability is a major issue. The most common ventricular assist device, the intra-aortic balloon pump, is a temporizing tool to sustain a patient for just a few days while alternatives are evaluated and pursued.The steps for implanting a ventricular assist pump can be as simple as:
(1) cleaning and applying antiseptics to the skin,
(2) placing a needle in the femoral artery at the groin area,
(3) threading a wire into the artery,
(4) threading a series of hollow tubes over the wire (dilators) and leaving the largest in place (introducer),
(5) threading a catheter-pump through the introducer and up the aorta to the desired location,
(6) synchronizing the pump the the cardiac cycle by electrocardiogram.
|
If the device is an intra-aortic balloon pump (IABP) then the device is advanced to the aortic arch so that an inflatable balloon expands and contracts within the aorta from the aortic arch down to just above the renal arteries. The IABP is designed to deflate when the heart contracts (systole), to make space for blood ejecting from the failing heart (afterload reduction), then inflate when the heart relaxes (diastole), effectively converting a blood pressure of 120/80 to 80/120. The coronary arteries are stressed during systole and receive their blood supply during diastole, so the diastolic augmentation (inflation of the balloon during heart relaxation) markedly improves blood delivery to the coronary arteries, which is very helpful when the coronary arteries are diseased and not well suited for immediate repair. The actions of the balloon damage blood cells and can rupture the aorta. The blood cell damage activates clotting, so full anticoagulation is required.
If the device is an Impella catheter pump, then the distal end (farthest into the patient) crosses the aortic valve into the left ventricle to draw blood from there and deliver it beyond the heart in the descending aorta.
|
  IABP www.fda.gov/MedicalDevices/Safety Impella www.abiomed.com IABP www.fda.gov/MedicalDevices/Safety Impella www.abiomed.com |
Devices draw their input from
- arterial blood (aorta or femoral artery)
- venous blood (vena cava), or
- a puncture wound created in the apex of the left ventricle of the heart
The next example of a ventricular assist device to consider during open heart surgery, is the bypass pump that is used during most cardiovascular surgeries, and in particular during heart or heart-lung transplant. The bypass pump relies on a tube (cannula) placed in a large source of deoxygenated blood
- the right atrium,
- the inferior vena cava or
- the femoral vein
to draw its input blood from there (diverting it from the heart), and a second cannula placed in a large artery (the aorta or the femoral artery) for output. The blood passes out of the patient (extra-corporeal) to a very large mechanical pump, that typically consists of compressible tubing and rollers to minimize trauma to the blood, passing the red cells of the blood by membranes that enable uptake of oxygen. Despite the attempts not to damage the blood, blood does get damaged, so full anti-coagulation is required. The anti-coagulation consists of intravenous heparin to bind the coagulation factors. When the patient comes off the pump, the heparinization of the blood is counteracted by intravenous protamine sulfate. Also the blood is cooled because low temperatures slow down metabolism and make the cells of the body less needy during the sub-optimal circulation support. Cooled blood has increased viscosity, offset by dilution of the blood with saline (Normal Saline, isotonic solution, w/v of NaCl, about 300 mOsm/L or 9.0 g per liter). As the pump takes over circulation, the blood supply to the heart is clamped off (cross-clamp), at which point the surgeon can work to repair the heart (valve repair, valve replacement, aorta graft, coronary grafts) or replace the heart or heart and lungs.
Artificial hearts are extensions of the concepts above, and differ primarily in
- how the pump in energized and
- how the pump is regulated.
An artificial heart is designed for long term use so it must be more gentle on the blood. In Part I: Alternative Models of Artificial Hearts, US and Europe, in this article, we reported on the Latest Innovations in Alternative Models of Artificial Hearts, the Carmat Heart, it is unusual in its design, said Dr. Joseph Rogers, an associate professor at Duke University and medical director of its cardiac transplant and mechanical circulatory support program. Surfaces in the new heart that touch human blood are made from cow tissue instead of artificial materials like plastic that can cause problems like clotting, it will decrease the anticoagulation dependence by design.
Artificial hearts must accommodate changes in demands of the body, not just in the chilled low metabolic state imposed by cardiovascular surgeons. The demands of the heart are measured by oxygen consumption in units of metabolic equivalents (METS) where 1 MET represents basal metabolism (awake at rest). MET values of activities range from 0.9 (sleeping) to 23 or more (running at 14 miles/hour = 22.5 km/hour). Thus, the artificial heart should be capable of increasing its output 2300% without damage the blood cells or running out of power. The goal of long term use generally is met by linking to an external power supply that is considered portable (on wheels), or in some cases, wearable
In contrast to Transplant of a human donor’s heart, described above, we present below the procedure for implantation of:
|
  Heartmate II (Thoratec, Pleasanton, CA). http://thenatureofhiking.com/heartless-man.html#.UiPybNKsh8E Heartmate II (Thoratec, Pleasanton, CA). http://thenatureofhiking.com/heartless-man.html#.UiPybNKsh8E |
Complications related to Open Heart Surgery
- perioperative hemorrhage,
- air embolism, and
- ventricular failure.
- infection,
- thromboembolism, and
- device failure. If the power drive is connected to a power line, the patient is tethered. Alternatively, the power may be provided by a battery pack that the patient may wear or wheel alongside.
Open Heart Surgery and Reoperative Sternotomy
Pearlman, JD and A. Lev-Ari 7/23/2013 Cardiovascular Complications: Death from Reoperative Sternotomy after prior CABG, MVR, AVR, or Radiation; Complications of PCI; Sepsis from Cardiovascular Interventions
- perfusion of the heart and
- promotion of circulation
III. Implant of a Total Artificial Heart
- A total artificial heart is similar to a BiVAD except for the option that it can replace most of the native heart instead of connecting in tandem to it
- If a total artificial heart is placed in tandem, the procedure is basically the same as for an RVAD plus and LVAD.
- If the total artificial heart replaces the native heart, the surgery is very similar to the heart transplant procedure explained above, plus handling for
- the native right atrium connects to the right intake of the total artificial heart,
- the main pulmonary artery connects to the right output,
- the native left atrium connects to the left input, and
- the aorta connects to the left output.
REFERENCES
- Shumway NE, Lower RR, Stofer RC. Transplantation of the heart. Adv Surg 1966;2:265-84.
- Gilles Dreyfus G, Jebara V, Mihaileanu S, Carpentier AF. Total orthotopic heart transplantation: An alternative to the standard technique. The Annals of Thoracic Surgery Volume 52, Issue 5 , Pages 1181-1184, November 1991
- Angermann CE, Spes CH, Tammew A, et al. Anatomic characteristics and valvular function of the transplanted heart:
transthoracic versus transoesophageal echocardiographic findings. J Heart Transplant 1990;9:331-8. - Griepp RB, Ergin MA. The history of experimental heart transplantation. J Heart Transplant. 1984;3:145.
- Copeland JG, Emery RW, Levinson MM, et al. Selection of patients for cardiac transplantation. Circulation. Jan 1987;75(1):2-9. [Medline].
- Ramakrishna H, Jaroszewski DE, Arabia FA. Adult cardiac transplantation: A review of perioperative management Part – I. Ann Card Anaesth. Jan-Jun 2009;12(1):71-8. [Medline]
- Hill JD. Bridging to cardiac transplantation. Ann Thorac Surg. Jan 1989;47(1):167-71. [Medline].
- Portner PM, Oyer PE, Pennington DG, et al. Implantable electrical left ventricular assist system: bridge to transplantation and the future. Ann Thorac Surg. Jan 1989;47(1):142-50. [Medline].
- Holman WL, Kormos RL, Naftel DC, Miller MA, Pagani FD, Blume E, et al. Predictors of death and transplant in patients with a mechanical circulatory support device: a multi-institutional study. J Heart Lung Transplant. Jan 2009;28(1):44-50. [Medline].
- Overcast TD, Evans RW, Bowen LE, et al. Problems in the identification of potential organ donors. Misconceptions and fallacies associated with donor cards. JAMA. Mar 23-30 1984;251(12):1559-62.[Medline].
- Reichart B, Brandl U. 40 years of heart transplantation and the DFG-Transregio Research Group Xenotransplantation. Xenotransplantation. Sep 2008;15(5):293-294. [Medline].
- Moriguchi J, Davis S, Jocson R, Esmailian F, Ardehali A, Laks H, et al. Successful use of a pneumatic biventricular assist device as a bridge to transplantation in cardiogenic shock. J Heart Lung Transplant. Oct 2011;30(10):1143-7. [Medline].
- Kilic A, Conte JV, Shah AS, Yuh DD. Orthotopic Heart Transplantation in Patients With Metabolic Risk Factors. Ann Thorac Surg. Feb 2 2012;[Medline].
- Arnaoutakis GJ, George TJ, Allen JG, Russell SD, Shah AS, Conte JV, et al. Institutional volume and the effect of recipient risk on short-term mortality after orthotopic heart transplant. J Thorac Cardiovasc Surg. Jan 2012;143(1):157-67, 167.e1. [Medline].
- Lee I, Localio R, Brensinger CM, Blumberg EA, Lautenbach E, Gasink L, et al. Decreased post-transplant survival among heart transplant recipients with pre-transplant hepatitis C virus positivity. J Heart Lung Transplant. Nov 2011;30(11):1266-74. [Medline].
- Caves PK, Stinson EB, Billingham M, Shumway NE. Percutaneous transvenous endomyocardial biopsy in human heart recipients. Experience with a new technique. Ann Thorac Surg. Oct 1973;16(4):325-36.[Medline].
- Hunt J, Lerman M, Magee MJ, et al. Improvement of renal dysfunction by conversion from calcineurin inhibitors to sirolimus after heart transplantation. J Heart Lung Transplant. Nov 2005;24(11):1863-7.[Medline].
- Pedotti P, Mattucci DA, Gabbrielli F, Venettoni S, Costa AN, Taioli E. Analysis of the complex effect of donor’s age on survival of subjects who underwent heart transplantation. Transplantation. Oct 27 2005;80(8):1026-32. [Medline].
- Griffith BP, Hardesty RL, Deeb GM, et al. Cardiac transplantation with cyclosporin A and prednisone. Ann Surg. Sep 1982;196(3):324-9. [Medline].
- Ye F, Ying-Bin X, Yu-Guo W, Hetzer R. Tacrolimus versus cyclosporine microemulsion for heart transplant recipients: a meta-analysis. J Heart Lung Transplant. Jan 2009;28(1):58-66. [Medline].
- Khan MS, Mery CM, Zafar F, Adachi I, Heinle JS, Cabrera AG, et al. Is mechanically bridging patients with a failing cardiac graft to retransplantation an effective therapy? Analysis of the United Network of Organ Sharing database. J Heart Lung Transplant. Aug 17 2012;[Medline].
- Hofflin JM, Potasman I, Baldwin JC, et al. Infectious complications in heart transplant recipients receiving cyclosporine and corticosteroids. Ann Intern Med. Feb 1987;106(2):209-16. [Medline].
- Tambur AR, Pamboukian SV, Costanzo MR, et al. The presence of HLA-directed antibodies after heart transplantation is associated with poor allograft outcome. Transplantation. Oct 27 2005;80(8):1019-25.[Medline].
- Kfoury AG, Renlund DG, Snow GL, Stehlik J, Folsom JW, Fisher PW, et al. A clinical correlation study of severity of antibody-mediated rejection and cardiovascular mortality in heart transplantation. J Heart Lung Transplant. Jan 2009;28(1):51-7. [Medline].
- Sweeney MS, Macris MP, Frazier OH, et al. The treatment of advanced cardiac allograft rejection. Ann Thorac Surg. Oct 1988;46(4):378-81. [Medline].
- Ford MA, Almond CS, Gauvreau K, Piercey G, Blume ED, Smoot LB, et al. Association of graft ischemic time with survival after heart transplant among children in the United States. J Heart Lung Transplant. Nov 2011;30(11):1244-9. [Medline].
Part III
Comparative Analysis of Transplant Clinical Outcomes based on Data in: Heart Transplant (HT) Indication for Heart Failure (HF): Procedure Outcomes and Research on HF, HT @ Two Nation’s Leading HF & HT Centers
By Larry H Bernstein, MD, FCAP and Aviva Lev-Ari, PhD, RN
Procedures Outcomes of Heart Transplant (HT) Indication for Heart Failure (HF)Center for Heart Failure @Cleveland Clinic, and Transplant Center @Mayo Clinic
Center for Heart Failure @Cleveland Clinic: Institution Profile
The treatment of heart failure requires a specialized multidisciplinary approach to manage the overall patient care plan. The Kaufman Center for Heart Failure Team brings together clinicians that specialize in cardiomyopathies and ischemic heart failure for patients with:
- All types of heart failure
- Dilated Cardiomyopathy
- Restrictive Cardiomyopathy
- Arrhythmogenic Right Ventricular Dysplasia (ARVD)
Heart Failure – National Hospital Quality Measures
Cleveland Clinic, 2011 (N = 1,163) 96.9%
UHC Top Decile, 2011 99.2%
SOURCE
University Health System Consortium (UHC) Comparative Database, January through November 2011 discharges.
The Centers for Medicare and Medicaid Services (CMS) calculates two heart failure outcome measures:
- all-cause mortality and
- all-cause readmission rates,
each based on Medicare claims and enrollment information.
Heart Failure All-Cause 30-Day Mortality (N = 762) July 2008 – June 2011
Cleveland Clinic 9.2%
National Average 11.6%
Heart Failure All-Cause 30-Day Readmission (N = 1,) July 2008 – June 2011
Cleveland Clinic 27.3%
National Average 24.7%
SOURCE:
hospitalcompare.hhs.gov
The results for risk-adjusted all-cause mortality is 2% lower than the National Average and 30-day risk-adjuted readmission rates for 2008-2011 are 2% higher than the National Average. There is no definitive information provided to explain the higher readmission rate. One might consider that they take most difficult referrals. The heart failure risk-adjusted readmission rate is higher than the national average; and both differences are statistically significant. To further reduce this rate, a multidisciplinary team was tasked with improving transitions from hospital to home or post-acute care facility. Specific initiatives have been implemented in each of these focus areas: communication, education and follow-up. There is no data for comparing 1-month, 1-year, and 3-year survivals.
http://my.clevelandclinic.org/Documents/outcomes/2011/outcomes
Additional Cleveland Clinic Data is provided related to Pre- and Post-operative conditions
Preoperative patient characteristics |
Prob |
Diabetes mellitus 499 (21.5%) 61 (26.4%) |
0.084 |
Congestive heart failure 758 (32.6%) 89 (38.5%) |
0.069 |
III-IV 1830 (78.8%) 184 (84.0%) |
|
Previous operation No injury (2324) Injury (231) P |
|
CABG 1375 (59.2%) 162 (70.1%) |
0.001 |
Current operation No injury (2324) Injury (231) P |
|
CABG 897 (38.6%) 104 (45.0%) |
0.056 |
Aortic valve surgery 1020 (43.9%) 118 (51.1%) |
0.036 |
Tricuspid valve surgery 414 (17.8%) 52 (22.5%) |
0.078 |
Aortic surgery 232 (10.0%) 37 (16.0%) |
0.004 |
Postoperative results |
|
No injury (2324) — Injury (231) – P |
|
PRCs 4.5 7.2 6.5 8.9 |
0.046 |
ICU stay (h) 102.3 228.6 146.3 +/- 346.9 |
<.001 |
Reoperation for bleeding 127 (5.5%) 21 (9.1%) |
0.024 |
Sepsis 86 (3.7%) 16 (6.9%) |
0.017 |
Stroke 56 (2.4%) 11 (4.8%) |
0.033 |
Prolonged ventilation 505 (21.7%) 97 (42.0%) |
<.001 |
Pneumonia 123 (5.3%) 25 (10.8%) |
<.001 |
ARDS 32 (1.4%) 8 (3.5%) |
0.015 |
Postoperative renal failure 237 (10.2%) 51 (22.1%) |
<.001 |
Multisystem failure 45 (1.9%) 13 (5.6%) |
<.001 |
Hospital death 151 (6.5%) 43 (18.6%) |
<.001 |
| Cleveland Clinic |
| LVAD mortality 2007-2011 5% |
| VAD mortality 2011 Obs 10% Exp 17.5% N 56 |
| HF- NHQM |
| 2010 1194 93.9% |
| 2011 1163 96.9% |
| UHC Top decile, 2011 99.2% |
Transplant Center @ Mayo Clinic: Alternative Solutions to Treatment of Heart Failure. Mayo Clinic performs has pre-eminent adult and pediatric transplant programs.
| Success Measures 2009-2011 |
1 mo |
1 year |
3 year |
| Heart Transplant Patient Survival — Adult | |||
| Mayo – Phoenix, AZ (n=40) |
97.50% |
94.63% |
82.22% |
| Mayo – Jacksonville, FL (n=61) |
95.08% |
91.50% |
81.82% |
| Saint Marys Hospital – Rochester, MN (n=48) |
95.83% |
95.83% |
82.61% |
| National Average |
95.89% |
90.21% |
81.79% |
| Heart Transplant – Children | |||
| Saint Marys Hospital – Rochester, MN (n=5) |
100% |
100% |
60% |
| Adult Heart Organ (Graft) | |||
| Mayo – Phoenix, AZ (n=41) |
97.56% |
94.77% |
82.22% |
| Mayo – Jacksonville, FL (n=61) |
95.08% |
91.50% |
80.00% |
| Mayo -Rochester, MN (n=49) |
93.88% |
93.88% |
82.61% |
| National Average |
95.71% |
89.91% |
80.92% |
Standards for Comparison: SRTR function, data acquisition, analysis, and reporting.
http://srtr.transplant.hrsa.gov/
The Scientific Registry of Transplant Recipients
supports the ongoing evaluation of solid organ transplantation in the United States. SRTR designs and carries out data analyses and maintains two websites to disseminate organ transplant information.
This site is srtr.transplant.hrsa.gov. Here you will find the OPTN/SRTR Annual Data Report, which publishes organ transplant statistics and is produced each year by SRTR staff and staff of the national Organ Procurement and Transplantation Network (OPTN).
At www.srtr.org, you will find older (pre-2010) annual data reports, current and past reports on organ procurement organizations and transplant programs, and information for researchers (including additional data tables and information about SRTR data and statistical methods).
Both sites aim to inform transplant programs, organ procurement organizations, policy makers, transplant professionals, transplant recipients, organ donors and donor families, and the general public about the current state of solid organ transplantation in the US.
SRTR also helps facilitate transplant research by providing access to data for qualified researchers interested in studying various aspects of solid organ transplantation.
- Timeline and cohort selection.
- Patients who are lost to follow-up: censoring and extra ascertainment.
- Expected survival and risk-adjustment.
- Comparison points: norms versus targets.
- Range of other data here are incorporated either on a person-level matching basis or on an aggregate basis for comparison.
- Primary data source is the transplant center, submitting data through the OPTN system. Includes WL and organ allocation, tiedi, match runs.
- Range of other data here are incorporated either on a person-level matching basis or on an aggregate basis for comparison.
- Primary data source is the transplant center, submitting data through the OPTN system. Includes WL and organ allocation, tiedi, match runs.
- Range of other data here are incorporated either on a person-level matching basis or on an aggregate basis for comparison.
- National Death Index is not be used for analyses, but is used to evaluate completeness of extra ascertainment.
- Uniform methodology: The SRTR provides a uniform methodology of calculation. These methods are standard and accepted within the statistical and medical communities, however they are not the only ones available.
- Audited data collection: All data on which these statistics are based are audited by the OPTN. The United Network for Organ Sharing (UNOS), the contractor for the OPTN, works to ensure the accuracy and reliability of these data.
- Extra ascertainment of mortality: The SRTR helps find information about patients who become lost-to-follow-up that may be unavailable to transplanting centers, or very difficult to find.
- Risk adjustment: Comparison of outcomes should be based on risk-adjusted models that account for the types of patients treated. Without national data, it is impossible for centers to calculate risk-adjusted comparison points.
Program-Specific Reporting – different formats for different audiences: What we choose to focus on
Percent survival at one year, three years.
- What choices do our patients have?
- How well are we doing?
*Report Contents – Focus on patient outcomes
- Graft and patient survival rates compared with expected values
- Updated every 6 months (January, July).
- Patient and graft survival tables report 1-month, 1-year, and 3-year outcomes for 2.5-year cohorts of recipients.
Calculating Survival
| Transplant Month Follow-up | Group A: Transplant > 1 Y | Group B:Transplant 6-12 Mo | All | |
| Months 0-6 | Transplants Deaths |
100 10 |
100 14 |
200 24 |
| Survival | 90% | 86% | 88% | |
| Months 7-12 | At-Risk Deaths Survival |
90 18 80% |
Not yet observed, Use 80% |
.88*.80 = 70.4%or (72 + 68.8)/2 = 70.4 |
| 1 Year Survival | .90 * .80 = 72% | .86*.80 = 68.8% | ||
Incomplete Data and Loss to Follow-Up
- Censoring (Kaplan Meier/Cox) works only if “lost” patients have similar failure rates as followed patients (unbiased).
- Censoring can produce unstable estimates for small samples
- NDI study indicates that the SRTR identifies > 99% of deaths
- Observed rates are compared with rates that would be expected based on characteristics of recipients and donors at each center.
- Allows fair comparison among centers that treat different types of patients
- Is the difference we see between the observed survival of 87.78% and the expected rate of 89.41% large enough to be meaningful? The answer may depend perspective.
The percent surviving at one year is only 2% lower than expected, an apparently small difference. However, the same difference appears more consequential when comparing the percent died that implied by subtracting survival percents from 100: the percent of patients who had died by the end of the first year was a full 15% higher than expected. Finally, in our example center that performed 90 transplants during a 2.5-year period, the count of deaths observed during follow-up was 30% higher, accounting for 2.5 deaths more than we would expect during time these patients were followed.
The difference between each of these is stark. The first change from a 2% difference to a 15% difference reflects the change in denominator: a small percentage point difference is a much smaller fraction of survival (usually a large number at one year) than of mortality (usually a small number). Several years after transplant, when survival rates may be close to 50%, the contrast would not be as evident.
The difference between the percent died and death count is more subtle: the expected number of deaths is calculated according to the time that patients are followed after transplant, so a patient whose follow-up ends immediately after transplant – for any reason, including death — is smaller than the expected number of deaths for a patient who died after ten months. Therefore, this last statistic accounts for the difference between a patient who survives only briefly during follow-up, and one who survives nearly the entire period, despite the fact that they have both died in the end-of-period accounting of “percent died”.
Risk Adjustment
What rate would be expected for patients at this center if their outcomes were comparable to national outcomes for similar patients?
“Similar” defined by characteristics that affect the rate, such as:
- Demographics
- Etiology
- Severity of illness
Differences between observed and expected outcomes are not due to these adjustment factors.
*notion of a “similar” patient: have in-common characteristics that may influence the outcome –
include basic demographic factors such as age, etiology of disease, and the patient’s severity of illness.
Risk-Adjustment Models
Each risk-adjustment model is published one month in advance of the PSRs (Figure 5). These tables serve not only as a list of all characteristics incorporated, but also tell the reader:
- The beta, or calculated coefficient, tells what was the effect of that characteristic on expected risk of dying or failed transplant?
- The standard error and p-value tell how much random variance there was around this estimate, and how sure we are that there is a real effect of this characteristic.
- Models are repeated for a series of three different cohorts of transplants, allowing a comparison of how stable the coefficients are across time.
- The index of concordance, for each model, tells the percent of variation in the order of events (deaths or graft failures) that is accurately predicted by the model. A index of 100% would suggest that the model perfectly predicts the order of events; 50% would suggest that the order is random with regard to predictors.
*Odds Ratio >1 = Failure/Death More Likely = Lower Expected;
Odds Ratio <1 = Failure/Death Less Likely = Higher Expected
Adjusting for Age
Nationally: Average survival, 85%.
- 50% of patients are young with 95% survival.
- 50% of patients are old with 75% survival.
Center A treats only older patients, 80% survival:
Center survival of 80% worse than national average of 85%.
100% are older patients with expected 75% survival.
Center A patients have better expected survival compared with similar patients nationwide
Center X Treats More Older Recipients than the National Average
Adjustment: Account for Case Mix
Adjustment: Random Variation
Concepts: Actionable, Important, and Significant
- MPSC Criteria: Observed (O) – Expected (E) greater than 3, O – E > 3
- Interpretation: 3 excess deaths per 2-year transplant cohort
- MPSC Criteria: Standardized Mortality Ratio (SMR) > 1.5; O / E > 1.5
- Interpretation: 50% more deaths than expected
- MPSC Criteria: one-sided p-value less than .05
- Interpretation: there is less than a 5 percent chance that a poor outcome occurred by simple random variation
Important: More than 3 excess deaths
Actionable: More than 50% excess deaths
Part IV
Imaging Technologies in use for Clinical Monitoring of Patients with Heart Transplant: Donor Human Heart and Artificial Heart
By Justin D Pearlman, MD, PhD, FACC
Imaging of the heart monitors success and viability of the transplanted heart in terms of
what fraction of the contents of each ventricle moves out of the heart (ejection fraction),
- what volumes the heart sees
- end-diastolic volume, or EDV, and
- end-diastolic diameter, or
- LVIDd,
- end systolic volume or ESV),
- how well the walls move (wall motion) and
- wall thickening analysis,
- tissue character
- visual evidence for changes in the heart muscle,
- perfusion (delivery of nutrient blood supply to the heart muscle), and
- various means to detect coronary artery disease (obstructions to blood delivery to the heart muscle).
Clinical tools for imaging the heart include:
- The major tool – ultrasound (echocardiography),
- cardiac magnetic resonance (CMR),
- computed xray tomography (CT),
- catheterization with xray imaging (coronary angiography and ventriculography),
- metabolic marker distribution by positron emission tomography (PET), and
- radioactive marker distribution (nuclear imaging, SPECT).
Ultrasound applies alternating current to a piezoelectric crystal (lead zirconate) to produce compressions and expansions of material as a wave pattern that relies on tissue elastic properties to propagate into the tissue, reflecting back when the wave encounters a change of properties (acoustic impedance mismatch). Display of signal versus time on an oscilloscope (like an ECG monitor) constitutes “A-mode”(amplitude) display, whereby the distance between peaks corresponds to distances along the path that can report thickness of the left ventricle, and diameter of the left ventricular cavity. Time translates to distance because the speed of sound through tissue is fairely constant, ~1540 meters/second. Collapsing the peaks to bright dots represents the same data in “B-mode” (brightness) which reduces the data to a line of variable intensity with bright dots marking changes in tissue (e.g., muscle versus blood). Attaching a position sensor to the handle of the sound source (the transducer) enabled plotting the B-mode signal on a 2D screen to indicate the position of the sound beam. Gynecologists showed that a steady sweep of the transducer (C-mode, composite) then generated 2D images that delineated the shape of a fetal head, and as quality improved, the gender prior to birth. The invention of phased-array crystal sets (multiple sources electrically activated sequentially with specific timing) enabled generation of a composite beam that is electronically swept in an arc with no mechanically moving parts. That is now the main method of ultrasound imaging, called phased-array sector scanning. More advanced phased arrays sweep in a 2D pattern to generate 3D imaging (4D or dynamic 3D, when you include repeating over time).
The e-Reader is encourage to review Cardiovascular Imaging Chapters in each of the three volumes.
For new technological developments in achieving Optimal PCI Outcomes and for Visual Tools for Characterization of endovascular tissue affecting Coronary Circulation, review the following article:
Part V
The Failure of a Heart Transplant – Pathology and Autopsy Findings
by Larry H Bernstein, MD, FCAP
Section A. SRTR Graft and Patient Survival Data
Table 1. Transplant Survivals, 2011, and related conditions
| Activities 2011 | Numbers |
| Deceased donor transplants (n=number) | 2,322 |
| Adult graft survival (based on 4595 transplants) | 89.91 (%) |
| Adult patient survival (based on 4449 transplants) | 90.21 (%) |
| Pediatric graft survival (based on 886 transplants) | 90.74 (%) |
| Pediatric patient survival (based on 829 transplants) | 91.31 (%) |
| Primary Disease | (%) of Waitlist |
| Cardiomyopathy | 49.4 |
| Coronary Artery Disease | 34.7 |
| Retransplant/Graft Failure | 4.4 |
| Valvular Heart Disease | 1.7 |
| Congenital Heart Disease | 8.4 |
Table 2. Recipient Condition at Transplant (%)
| Not Hospitalized | 54.0 |
| Hospitalized | 14.6 |
| ICU | 31.0 |
| No Support Mechanism | 25.2 |
| Devices | 42.4 |
| Other Support Mechanism | 32.2 |
Table 3. Donor Characteristics
| Cause of Death | (%) |
| Stroke | 20.9 |
| MVA | 23.4 |
| Other | 55.7 |
| Age (years) | |
| 18-34 | 48.8 |
| 35-49 | 24.5 |
| 12-17 | 9.4 |
| Cold ischemic time 1.5-4.5 h | 85.3 |
Table 4. Graft and Patient Survival
| Survival by… | time since transplant | ||
| 1 mo | 1 yr | 3 yrs | |
| Adult (Age 18+) | |||
| Graft survival (%) | 95.7 | 89.9 | 80.9 |
| # failures |
197 |
442 |
847 |
| Patient survival (%) | 95.9 | 90.2 | 81.8 |
| # deaths |
183 |
415 |
783 |
| Pediatric (Age < 18) | |||
| Graft Survival (%) | 96.3 | 90.7 | 82.0 |
| Graft Failures |
33 |
80 |
151 |
| Patient Survival (%) |
96.4 |
91.3 |
82.93 |
| Deaths |
30 |
70 | 134 |
* 07/01/2006 and 12/31/2008 for the 3 Year Model
Table 4. Risk Model Documentation – Adult, Three−Year Graft Survival
| Characteristic | Level | Estimate | Std. Err. | P−Value |
| Bilirubin at Transplant | mg/dL | 0.0364 | 0.008 | <0.0001 |
| Dialysis at Transplant | Yes | 0.8026 | 0.169 | <0.0001 |
| Donor Age | 0−17 | −0.5789 | 0.140 | <0.0001 |
| 18−34 | −0.3098 | 0.074 | <0.0001 | |
| Ischemic Time | hrs | 0.1298 | 0.033 | <0.0001 |
| Previous Transplant | Yes | 0.4251 | 0.157 | 0.0069 |
| Recipient DX | Cardiomyopathy | −0.1933 | 0.078 | 0.0130 |
| Recipient Age | 18-34 | 0.2806 | 0.110 | 0.0107 |
| 65+ | 0.2694 | 0.101 | 0.0074 | |
| Recipient Race | Black | 0.4104 | 0.086 | <0.0001 |
| Recipient SCrea | >1 & <=1.5 mg/dL | 0.0115 | 0.086 | 0.8933 |
| >1.5 mg/dL | 0.4316 | 0.095 | <0.0001 | |
| Recipient on VAD | Yes | 0.2777 | 0.086 | 0.0013 |
| Recipient on Vent | Yes | 0.7014 | 0.169 | <0.0001 |
* SRTR Program−Specific Report July 12, 2012
Table 5. Risk Model Documentation Adult, Three−Year Patient Survival
| Characteristic | Level | Estimate | Std. Err. | P−Value |
| Donor Age | 0−17 | −0.4758 | 0.1452 | 0.0010 |
| 18−34 | −0.3066 | 0.0764 | 0.0001 | |
| Ischemic Time | hrs | 0.1400 | 0.0344 | <0.0001 |
| Most Recent CPRA/PRA% | 0.0039 | 0.0019 | 0.0359 | |
| Recipient Age | 18−34 | 0.3041 | 0.1157 | 0.0086 |
| 65+ | 0.3089 | 0.1013 | 0.0023 | |
| Recipient DX | Cardiomyopathy | −0.2151 | 0.0809 | 0.0078 |
| Congen Heart Dis | 0.5504 | 0.2085 | 0.0083 | |
| Recipient Race | Black | 0.4942 | 0.0895 | <0.0001 |
| Recipient SCrea | >1 and <=1.5 | 0.0245 | 0.0887 | 0.7827 |
| >1.5 mg/dL | 0.5053 | 0.0991 | <0.0001 | |
| Recipient on VAD | Yes | 0.2559 | 0.0816 | 0.0017 |
| Recipient on Vent | Yes | 0.7340 | 0.1852 | 0.0001 |
Note the following:
1. The most common transplant recipients in adults are cardiomyopathy and CAD, and congenital heart disease in children.
2. recipient on VAD or on vantilator is significant
3. ischemic time for donor heart is usually 1.5-4.5 hours, but longer time has an effect on graft and patient survival
4. Recipient serum creatinine exceeding 1.5 mg/dl is unfavorable, but considering BMI and age related renal nephron loss, eGFR would be a better measure.5. African-American has an effect, but it is not at all clear whether sickle cell trait or disease is a factor.
6. Half the recipients are not hospitalized, and they might coincide with no or other support.
Section B. Special Concerns
Topic 1
Cellular repopulation of myocardial infarction in patients with sex-mismatched heart transplantation
Source: Georg-August-University G€ottingen. c2004, Eur Soc Cardiol
Recent studies have suggested that human extracardiac progenitor cells are capable of differentiating into cardiomyocytes. In animal studies, myocardial infarction attracted bone marrow stem cells and enhanced their differentiation into cardiomyocytes.
Myocardial infarction enhances the invasion of extracardiac progenitor cells and their regeneration of endothelial cells. However, a significant differentiation into cardiomyocytes as a physiological mechanism of postischaemic regeneration does not occur in transplanted patients.
Topic 2
Five-year follow-up of hepatitis C-naïve heart transplant recipients who received hepatitis C-positive donor hearts.
G S Gudmundsson, K Malinowska, J A Robinson, B A Pisani, J C Mendez, B K Foy, G M Mullen
Advanced Heart Failure/Heart Transplant Program, Loyola University, Maywood, Illinois, USA.
Transplantation Proceedings (impact factor: 1). 07/2003; 35(4):1536-8.
Source: PubMed
Due to the risk of transmission of hepatitis C virus, the use of hepatitis C seropositive donors in heart transplantation is controversial. The transmission rate of hepatitis C in this patient population is estimated to range from 67% to 80%. Long-term clinical outcomes of heart transplant recipients of hepatitis C-positive donor hearts are not well described. We report the 5-year long-term outcome of seven hepatitis C-naïve heart transplant recipients who received hepatitis C-positive donor hearts.
Seven hearts transplant recipients, six men and one woman were included in our study. After a mean follow-up of 63.3 +/- 20.4 months (range 28.2 to 85.9), four of seven (57.1%) patients are hepatitis C-negative, have normal liver function tests, and no clinical evidence of hepatitis. Three of seven (43%) have been diagnosed with hepatitis C by liver biopsy or the HCV-RNA reverse transcriptase polymerase chain reaction at a mean follow-up of 35.1 months (18.8 months posttransplantation). One had an accelerated course of hepatitis that was ultimately fatal, one was successfully treated with interferon, and the third died from other causes than liver injury. Overall, the 5-year survival was 71.4%.
Topic 3
Cryptococcus neoformans Infection in Organ Transplant Recipients: Variables Influencing Clinical Characteristics and Outcome
Shahid Husain, Marilyn M. Wagener, and Nina Singh
Veterans Affairs Medical Center and University of Pittsburgh
Thomas E. Starzl Transplantation Institute, Pittsburgh, Pennsylvania, USA
Emerging Infectious Diseases 376 Vol. 7, No. 3, May–June 2001
Unique clinical characteristics and other variables influencing the outcome of Cryptococcus neoformans infection in organ transplant recipients have not been well defined. From a review of published reports, we found that C. neoformans infection was documented in 2.8% of organ transplant recipients (overall death rate 42%). The type of primary immunosuppressive agent used in transplantation influenced the predominant clinical manifestation of cryptococcosis. Patients receiving tacrolimus were significantly less likely to have central nervous system involvement (78% versus 11%, p =0.001) and more likely to have skin, soft-tissue, and osteoarticular involvement (66% versus 21%, p = 0.006) than patients receiving nontacrolimus-based immunosuppression. Renal failure at admission was the only independently significant predictor of death in these patients (odds ratio 16.4, 95% CI 1.9–143, p = 0.004). Hypotheses based on these data may elucidate the pathogenesis and may ultimately guide the management of C. neoformans infection in organ transplant recipients.
Patients were 12 to 67 years of age (median 44 years); 78% were male. The mean incidence of C. neoformans infection was 2.8 per 100 transplants (0.3 to 5.3 per 100). The overall incidence was 2.4% in liver, 2.0% in lung, 3.0% in heart, and 2.8% in renal transplant recipients. Of 127 transplant recipients who could be evaluated, 100 (79%) had azathioprine as the primary immunosuppressive agent, 9 (7%) had tacrolimus, 11 (9%) had cyclosporine, and 7 (6%) had cyclosporine and azathioprine. Of these 127 patients, 78 were also receiving prednisone in various dosages. The incidence of cryptococcosis was 4.5 per 100 transplants in patients who received tacrolimus, 2.4 per 100 transplants in patients who received cyclosporine, and 3.4 per 100 transplants in patients who received azathioprine. These rates did not differ significantly. Rejection episodes preceding cryptococcal infection were documented in 17 (25%) of 67 patients; rejection had occurred a median of 7 months (from 5 days to 49 months) before onset of infection.
Cryptococcosis occurred a median of 1.6 years (from 2 days to 12 years) after transplantation. Overall, 14 (15%) of 94 cases occurred within 3 months, 10 (11%) of 94 in 3 to 6 months, 15 (16%) of 94 in 6 to 12 months, and 55 (59%) of 94 >12 months after transplantation. The median time to onset after transplantation was 35 months for kidney, 25 months for heart, 8.8 months for liver, and 3 months for lung transplant recipients (p = 0.001). Overall, cryptococcosis developed in 100% of the lung, 75% of the liver, 33% of the heart, and 30% of the kidney transplant recipients within 12 months of transplantation (p = 0.002).
Topic 4
Diagnostic Accuracy of Mortality on a Population of Heart Transplant Patients
M AMUCHÁSTEGUI, AE CONTRERAS, O SALOMONE, A DILLER, et al.
Hospital Privado Centro Médico de Córdoba
REV ARGENT CARDIOL 2008;76:292-294.
Although morbidity and mortality rates in heart transplant have been extensively analyzed, most mortality studies and mortality registries in heart transplant patients are based on clinical data.
Between January 1990 and January 2005 all dead transplant patients were included. The final diagnosis of the cause of death was confirmed with necropsy or biopsy of a solid organ. The causes of death assessed were early graft failure, cellular rejection, graft vascular disease, neoplasms and others.
Seventy three patients underwent heart transplantation during the study period. Thirty one patients died. The cause of death was certified in 61% of cases by 12 necropsies and 7 solid organ biopsies.
- Cellular rejection greater than grade III was the most frequent cause of death.
- Histopathology studies differed from the clinically suspected cause of death in 12.9% of cases.
Clinical and pathological information derived from post mortem studies is an indicator of the reality of our practice and constitutes an underlying mainstay for understanding transplant patients and for their further management; in this sense, performing necropsies is of vital importance for these patients.
Topic 5
How do Heart Failure patients die?
S. Orn and K. Dickstein
Central Hospital in Rogaland, Stavanger, Norway
European Heart Journal Supplements (2002) 4 (Supplement D), D59-D65
http://eurheartjsupp.oxfordjournals.org/
Approximately 90% of heart failure patients die from cardiovascular causes. Fifty per cent die from progressive heart failure, and the remainder die suddenly from arrhythmias and ischaemic events. Autopsy reveals the presence of an acute ischaemic event inapproximately 50% of sudden deaths and in 35% of all deaths among patients with ischaemic heart failure.
An accurate description of the cause and mode of death is important if we are to elucidate the mechanisms that are operative in the heart failure population.
At present, the most accurate data on mode of death are obtained from large randomized heart failure trials. They indicate that current treatment strategies for heart failure prolong life expectancy, but have relatively little impact on the proportion of heart failure patients who die from cardiovascular causes. The ultimate goal of intervention is to shift the balance toward more deaths from non-cardiovascular causes. (Eur Heart J Supplements 2002; 4 (Suppl D): D59-D65)
The heterogeneity of the heart failure population is reflected in the different ways in which these patients die.
- Some deteriorate progressively, whereas others
- die after acute episodes of decompensation.
- Others die suddenly and unexpectedly, and some (relatively few)
- die from noncardiac causes.
Before the angiotensin-converting enzyme (ACE) inhibitor era, it was estimated that
- 90% of the total deaths in heart failure patients were from cardiovascular causes,
- 49% were related to worsening heart failure,
- 22% to arrhythmias and
- 11% to acute myocardial infarction[S].
It is conventional to categorise death according to mode and cause of death.
- Cause of death addresses the mechanisms by which death occurs, such as arrhythmia, acute myocardial infarction or progressive heart failure (Table 1).
- Mode of death is perhaps easier to categorise.
- Mode and cause of death are not the same, although they are often used interchangeably.
Sudden death has various underlying causes, such as
- arrhythmia,
- acute myocardial infarction,
- pulmonary embolism,
- myocardial or aortic rupture, and
- stroke.
Sudden cardiac death is defined as natural death due to cardiac causes, heralded by abrupt loss of consciousness within 1 h of the onset of acute symptoms[2].
In order to avoid confusion in terminology, some clinical trials subclassify death without using the term ’cause of death’ and end-point committees focus instead on mode and place of death (Table 1)[31]. However, although it is more difficult to classify cause of death than mode of death, it is nevertheless productive to examine the causes of death among heart failure patients. The cause of death reflects the underlying pathophysiology of the disease, and helps us to understand the mechanisms responsible for its progression. Unravelling the mechanisms that lead to death is clinically relevant and may reveal potential new treatment targets. Effective treatment may alter the cause of death, and should ideally shift the operative mechanism from cardiovascular to noncardiovascular. Most of our knowledge of the cause and mode of death in heart failure comes from the
- large randomized mortality trials and from
- official death registries.
However, both of these sources of information have their problems.
A simplified classification of heart failure deaths
- Cardiovascular
- Non-cardiovascular
- Cardiac
- Myocardial infarction
- Progressive heart failure
- Other cardiac
- Sudden death
- Non-cardiac
- Stroke
- Other
- Procedure-related
Conclusions
by Larry H Bernstein, MD, FCAP
Part I
Leading Causes of Death
Number of Deaths – Leading Causes |
|
| Heart disease |
597,689 |
| Cancer |
574,743 |
| Chronic Lung Disease |
138,080 |
| Stroke |
129,476 |
| Accidents |
120,859 |
| Alzheimer’s |
83,494 |
| Diabetes |
69,071 |
| Kidney disease |
50,476 |
| Influenza and Pneumonia |
50,097 |
| Suicide |
38,364 |
| *National Vital Statistics Report (NVSR) “Deaths: Final Data for 2010.” MortalityData@cdc.gov. | |
WHO Leading Causes of Death |
||
| Low income countries |
Deaths (mil) |
% of deaths |
| Lower respiratory infections |
1.05 |
11.3 |
| Diarrheal diseases |
0.76 |
8.2 |
| HIV/AIDS |
0.72 |
7.8 |
| Ischemic heart disease |
0.57 |
6.1 |
| Malaria |
0.48 |
5.2 |
| High-income countries |
Deaths (mil) |
% of deaths |
| Ischemic heart disease |
1.42 |
15.6 |
| Cerebrovascular disease |
0.79 |
8.7 |
| Bronchioepithelial cancers |
0.54 |
5.9 |
| Alzheimer and dementias |
0.37 |
4.1 |
| Pneumonias |
0.35 |
3.8 |
| High-income countries |
Deaths (mil) |
% of deaths |
| Ischemic heart disease |
5.27 |
13.7 |
| Stroke |
4.91 |
12.8 |
| COPD |
2.79 |
7.2 |
| Lower respiratory infections |
2.07 |
5.4 |
| Diarrheal diseases |
1.68 |
4.4 |
| World |
Deaths (mil) |
% of deaths |
| Ischaemic heart disease |
7.25 |
12.8 |
| Stroke |
6.15 |
10.8 |
| Pneumonias |
3.46 |
6.1 |
| COPD |
3.28 |
5.8 |
| Diarrheal diseases |
2.46 |
4.3 |
| HIV/AIDS |
1.78 |
3.1 |
Q: What is the number one cause of death throughout the world?
Cardiovascular diseases kill more people each year than any others. In 2008, 7.3 million people died of ischaemic heart disease, 6.2 million from stroke or another form of cerebrovascular disease.
Q: Isn’t smoking a top cause of death?
Tobacco use is a major cause of many of the world’s top killer diseases – including cardiovascular disease, chronic obstructive lung disease and lung cancer.
Deaths across the globe: an overview
Imagine a diverse international group of 1000 individuals representative of the women, men and children from all over the globe who died in 2008. Of those 1000 people,
- 159 would have come from high-income countries,
- 677 from middle-income countries and
- 163 from low-income countries.
What would be the top 10 causes of their deaths?
Low income countries
http://who.int/entity/mediacentre/factsheets/fs310_graph3.gif
Middle income countries
http://who.int/entity/mediacentre/factsheets/fs310_graph3.gif
High income countries
http://who.int/entity/mediacentre/factsheets/fs310_graph3.gif
Note: In this fact sheet, we use low-, middle- and high-income categories as defined by the World Bank. Countries are grouped based on their 2009 gross national income. See World health statistics 2011 for more information.
SOURCE
World health statistics 2011
Part II
Advances in Imaging Technology
This document discusses the advances in cardiac surgery assisted by rapid advances in cardiac imaging technology over the last 15 years. This portion concentrates on the treatments for advanced and disabling congestive heart failure as the age expectancy has increased to a range of early 8th and mid-9th decade, depending on patient related comorbidities, nutrition and activity status. Many of the patients who require a heart transplant have coincident metabolic syndrome, advanced coronary artery circulation compromise, and/or atherosclerotic disease at the aortic arch. The advances in cardiothoracic technique has enabled a parallel advance in ventricular assist devices and a total artificial heart, which has allowed the maintenance of patients on waitlists until a suitable donor can be found, which is usually under a 5 year period. The ventricular assist device is selected for those patients who have sufficient reserve of left ventricular function. The cardiac and cardiosurgical advances have been advanced by the development of vastly improved imaging for both diagnosis and for enabling safety of procedures.
Cardiac magnetic resonance imaging is a noninvasive technique for assessing heart structure and function without the need for ionizing radiation. Its ability to precisely outline regions of myocardial ischemia and infarction gives it an important role in guiding interventional cardiologists in revascularization. Its ability to characterize and precisely quantify abnormal regurgitant flow volumes or abnormal shunts also makes it a valuable tool for many noncoronary interventions. The evidence is sufficient to show that cardiac magnetic resonance in guiding complex therapies in the catheter laboratory, as well as practical issues that need to be addressed to allow the application of this powerful tool to an increasing number of patients. But this advantage extends as well to the transplantation arena.1 (Cardiac magnetic resonance imaging for the interventional cardiologist. GA Figtree, JLønborg, SM Grieve, MR Ward, RBhindi. University of Sydney, Sydney, Australia. PubMed 02/2011; 4(2):137-48. http://dx.doi.org/10.1016/j.jcin.2010.09.026.)
Further, A novel approach to three-dimensional (3D) visualization of high quality, respiratory compensated cardiac magnetic resonance (MR) data is presented with the purpose of assisting the cardiovascular surgeon and the invasive cardiologist in the pre-operative planning2. Developments included:
(1) optimization of 3D, MR scan protocols;
(2) dedicated segmentation software;
(3) optimization of model generation algorithms;
(4) interactive, virtual reality visualization.
The approach is based on a tool for interactive, real-time visualization of 3D cardiac MR datasets in the form of 3D heart models displayed on virtual reality equipment. This allows the cardiac surgeon and the cardiologist to examine the model as if they were actually holding it in their hands. To secure relevant examination of all details related to cardiac morphology, the model can be re-scaled and the viewpoint can be set to any point inside the heart. Finally, the original, raw MR images can be examined on line as textures in cut-planes through the heart models3. (A new virtual reality approach for planning of cardiac interventions. T S Sørensen, SV Therkildsen, P Makowski, JL Knudsen, EM Pedersen. University of Aarhus Abogade 34, 8200 N, Arhus, Denmark. PubMed 07/2001; 22(3):193-214.
In addition, TeraRecon, (www.terarecon.com), the largest dedicated provider of advanced visualization and decision support solutions for medical imaging, showcased iNtuitionREVIEW™, a powerful new multi-modality, multi-monitor review and collaboration tool at the 24th European Congress Of Radiology4, held at the Austria Center, Vienna, Austria, March 8th-11th 2013. iNtuitionREVIEW is part of the iNtuition™ solution suite for advanced image management and quantitative decision support.
iNtuition has always complemented PACS with advanced functionality to resolve specialized use cases and workflow challenges not adequately addressed by existing PACS solutions. Features relevant to this discussion are:
- Time-Volume Analysis – Enhanced support for Cardiac MRI image acquisitions
- 3D/4D Visualization – Enhanced TAVI (transcatheter valve implantation) analysis
- Lesion-Specific Analysis – Support for research into downstream impact of stenosis
Editorial5: Seeing the heart; the success story of cardiac imaging
European Heart Journal 2000; 21(16): 1281–1288
http://dx.doi.org/10.1053/euhj.2000.2299
In 1896 a large audience at the Wurzburg Physical Medical Society attended a lecture and a demonstration, published a paper in 1895 ‘Eine Neue Art von Strahlen’ in the Annals of the Society. He showed an image of the hand of the famous anatomist F. Von Kolliker (1817– 1905). He was awarded the first Nobel prize laureate in Physics in 1901. FH Williams (1852–1936) began lecturing on the use of X-rays in visualization of the heart. In his paper ‘A method for more fully determining the outline of the heart by means of a fluoroscope together with otheruses of this instrument in medicine, he laid the basis for quantitative cardiac measurements from the chest X-ray.
To make angiocardiography of the heart possible, the feasibility of human cardiac catheterization had to be demonstrated. In 1929 W. Forssman (1904–1979) introduced ‘. . . a well oiled 65 cm long ureteral catheter’ into his antecubital vein to reach the right atrium. Soon thereafter he performed the first cardiac angiocardiogram on himself using 20 cc of 25% sodium iodide. Forssman shared the Nobel Prize for Medicine with A. Cournard and D. Richards in 1956.
The modern era of cardiac X-ray imaging began after the Second World War. G. Hounsfield of EMI Ltd tested their mathematical solutions and constructed the first clinical CT, which was installed in the Atkinson Morle Hospital in London in 1971 for brain scanning. This instrument revolutionized radiological imaging. Electronic and computer developments resulted in the image intensifier in 1952, which was a critical tool for analysing internal cardiac anatomy and the performing of selective coronary arteriography. Cormack and Hounsfield received the Nobel Prize for Physiology in 1979. Subsequent major advances have been the dramatic increase in the speed of scanning and image reconstruction and improved image quality as a result of faster and more sophisticated computers. At the Mayo Clinic, dynamic volume scanning was achieved in 1975 with the dynamic spatial reconstructor which is based on multiple X-ray sources and multiplex detectors for scanning the heart using the mathematical principles of CT. Fast computed tomography, or electron beam tomography of the heart, was introduced by D. Boyd and co-workers in 1979 at Imatron. Contrary to the conventional CT scanner, this instrument has no moving parts and can acquire an image in as little as 50 ms, obviating the need for ECG-gating. By successively steering a small focal spot size electron beam at four tungsten target rings, producing a moving beam 180o about the patient, with a 180o ring of detectors, the heart is imaged virtually free of motion artifacts.
The existence of ultrasound was recognized by L. Spallanzani (1729–1799). He demonstrated that bats who are blind navigate by means of echo reflection using inaudible sound. In 1880, Jacques and Pierre Curie discovered the piezo-electric effect, a peculiar phenomenon observed in certain quartz crystals, which were the basis of early ultrasound systems and were later replaced by ferroelectric materials. The first suggestion that submerged objects could be located by echo-reflection probably came after theTitanic disaster in 1912. During World War I, P.Langevin (1872–1946) conceived the idea in 1917 of using a piezo-electric quartz crystal as both transmitter and receiver, and this ultimately led to the development of sonar which was completed with the invention of the cathode ray tube, extensively used in World War II for ship navigation and remote submarine detection. In 1950, the German W. D. Keidel, also using an echo-transmission technique, performed the first cardiac examinations in an attempt to measure cardiac output.
In the late 1960s, the fibreoptic recorder, a spin-off from space technology, was introduced allowing the M-mode recording of all structures along the ultrasound beam: this constituted the definitive breakthrough in echocardiography. Today, M-mode echocardiography remains an important part of a complete cardiac ultrasound examination because of its high temporal resolution. J Griffith and W Henry introduced the mechanical sector-scanner in 1974, in the same year that FL Thurstone and OT.von Ramm constructed their electronic phased-array scanner. Today, phased-array scanners are the most widely available tomographic imaging instruments with a tremendous impact on cardiac diagnosis. Recently, new computer technologies have enabled the development of volume-rendered data which display tissue information possible even in real-time. The mono- and biplane electronic phased-array probes developed by J. Souquet in 1982 and his multiplane probe in 1985 represented the definitive clinical breakthrough of transoesophageal echocardiography.
The pulsed-wave Doppler technique allowed depth selection for blood flow velocity interrogation, but the major step forward for its clinical acceptance was its combination with imaging: the duplex scanner, reported by F. E. Barber et al. in 1974[35]. This development ultimately led to the integration of pulsed-wave Doppler with two-dimensional phased-array systems and allowed blood flow to be studied at selected regions within the image plane. The Bernouilli equation is now the cornerstone for Doppler assessment of cardiac haemodynamics and was published by the Dutch born D. Bernouilli (1700–1782) in his treatise ‘Hydrodynamica’ in 1738. The rapid progress in interventional cardiology renewed the interest in imaging devices, allowing circumferential imaging of the arterial wall under the endothelial surface. Both mechanical single-element and multi-element electronic systems are now increasingly used.
De Hevesy introduced the red cell blood volume measurement and the1284 anniversary ‘dilution principle’ in humans using the first man-made radioisotope 32P produced by the cyclotron in Berkeley, a milestone invention by EO Lawrence in 1931 for which he received the Nobel Prize in 1939. With the cyclotron it was now possible to artificially produce radiopharmaceuticals and radionuclides, which became increasingly available for clinical research. Diagnostic nuclear imaging techniques can be divided into four general groups, depending on localization, dilution, flow or diffusion and biochemical and metabolic properties. Most of these basic principles were first demonstrated by de Hevesy using cyclotron-produced radioisotopes and techniques that he had described many years before—he should therefore be considered the ‘father of nuclear medicine’. It was the introduction of technetium-99m which spurred on the growth of nuclear medicine because of its ideal properties for gamma camera imaging, its short half life and the possibility of producing it in a hospital radiopharmacy. There are now radiopharmaceuticals labelled with 99mTc for almost every application in nuclear medicine. However, the clinical application of nuclear imaging required both counting and detection of radioisotope emissions. Modern counting equipment dates back to 1908 when H Geiger made his first electron counting tube, the precursor of the 1928 Geiger counter. The major breakthrough in radioisotope emission detection was the development of the scintillation scanner by B. Cassen in Los Angeles in 1949, an instrument rapidly followed by refinements. The scintillation camera was designed by Anger based on a concept proposed by DE Copeland and EW Benjamin and was followed by the electronic gamma camera in 1952, which is still the basis of the scintillation camera used today.
Single photon emission tomography (SPET) is based on the pioneering work of Kuhl and Edwards and the first clinical system became available in 1953. However, digital computer technology was necessary for emission tomography as we use it today and put the ‘C’ in SPECT. Tomographic capabilities have proved invaluable in the clinical use of nuclear imaging of the heart. Clinical application rapidly followed technical advances. Although Wren et al. laid the foundation of PET in 1951 it was Sweet and Brownell of Massachusetts General Hospital who conceived the idea of positron imaging which relies on the annihilation radiation emitted at 180o when positrons and electrons meet. PET has a clinical role in defining myocardial viability in patients with ischemic left ventricular dysfunction who may benefit from revascularization rather than transplantation. It allows the sympathetic nervous system to be studied as regards the development of a number of cardiac disorders by receptor imaging. Although PET was developed before SPECT, it is less accessible because it requires direct access to a cyclotron to produce the short-lived positron emitting tracers and a radiopharmaceutical laboratory, which is not required for SPECT.
F Bloch et al. at Stanford and E Purcell et al. at Harvard in 1946 published a paper on the nuclear magnetic resonance (NMR) phenomenon in bulk matter for which they received the Nobel Prize in Physics in 1952. Initially, the major limitation to NMR spectroscopy in intact living systems was the small bore of the superconducting magnets. In the early 1980s, the Oxford Instrument Company started to produce superconducting magnets with increasing bores and extremely uniform and intense magnetic fields allowing the whole human body to be studied. The major advantages of MRI are that contrary to ultrasound, the images are not degraded by overlying bony structures, that there is a high natural contrast between flowing blood and soft tissue, the wide field of view, and that cross-sections of the heart can be obtained in any arbitrary orientation. The ideal cardiovascular imaging technique would provide the cardiologist with integrated information on structure function, myocardial characteristics, perfusion and metabolism. Potentially, magnetic resonance imaging offers all this and will probably become the one-stop non-invasive diagnostic test of cardiology.
Real-time dynamic display of registered 4D cardiac MR and ultrasound images using a GQ Zhanga,
X Huanga, R Eagleson,G. Guiraudona, and TM Peters
University of Western Ontario, London, ON, Canada
In minimally invasive image-guided surgical interventions, different imaging modalities, such as magnetic resonance imaging (MRI) or computed tomography (CT), and real-time three-dimensional (3D) ultrasound (US), can provide complementary, multi-spectral image information. Multimodality dynamic image registration is a well-established approach that permits real-time diagnostic information to be enhanced by placing lower-quality real-time images within a high quality anatomical context. For the guidance of cardiac procedures, it would be valuable to register dynamic MRI or CT with intraoperative US. However, in practice, either the high computational cost prohibits such real-time visualization of volumetric multimodal images in a real-world medical environment, or else the resulting image quality is not satisfactory for accurate guidance during the intervention. Modern graphics processing units (GPUs) provide the programmability, parallelism and increased computational precision to begin to address this problem.
The Use of Rapid Prototyping in Clinical Applications
G Biglino, S Schievano and AM Taylor
UCL Institute of Cardiovascular Sciences, London
http://www.intechopen.com
Rapid prototyping broadly indicates the fabrication of a three-dimensional (3D) model from a computer-aided design (CAD), traditionally built layer by layer according to the 3D input (Laoui & Shaik, 2003). Rapid prototyping has also been indicated as solid free-form, computer-automated or layer manufacturing (Rengier et al., 2008). The development of this technique in the clinical world has been rendered possible by the concomitant advances in all its three fundamental steps:
1. Medical imaging (data acquisition),
2. Image processing (image segmentation and reconstruction by means of appropriate software) and
3. Rapid prototyping itself (3D printing).
Particular advantages in this discussion are:
1. Customised implants: Instead of using a standard implant and adapting it to the implantation site during the surgical procedure, rapid prototyping enables the fabrication of patient-specific implants, ensuring better fitting and reduced operation time.
2. Microelectromechanical systems (MEMS): These are micro-sized objects that are fabricated by the same technique as integrated circuits. MEMS can have different. applications, including diagnostics (used in catheters, ultrasound intravascular diagnostics, angioplasty, ECG), pumping systems, drug delivery systems, monitoring, artificial organs, minimally invasive surgery.
Example: Stages of rapid prototyping in a clinical setting. From left to right: data acquisition (in this case with magnetic resonance (MR) imaging), image processing, 3D volume reconstruction with appropriate software (in this case, Mimics®, Materialise, Leuven, Belgium) and final 3D model printed in a transparent resin.
Despite its clinical use to the present day is still somewhat limited, considering the potential and flexibility of this technique, it is likely that applications of rapid prototyping such as individual patient care and academic research will be increasingly utilised (Rengier et al., 2010).
Nuclear Cardiology — In the Era of the Interventional Cardiology
B Baskot, I Ivanov, D Kovacevic, S Obradovic, N Ratkovic and M Zivkovic
Chap 10, InTech. http://dx.doi.org/10.5772/55484
The strength and breadth of nuclear cardiology lie in its great potential for future creative growth. This growth involves the development of new biologically derived radiopharmaceuticals, advanced imaging techologies, and a broad/based set of research and clinical applications involving diagnosis, functional categorization, prognosis, evaluation of therapeutic interventions, and the ability to deal with many of the major investigative issues in contemporary cardiology such as myocardial hibernation, stunning, and viability. The past decade has been characterized by major advances in nuclear cardiology that have greatly enhanced the clinical utility of the various radionuclide techniques used for the assessment of regional myocardial perfusion and regional and global left ventricular function under resting and stress conditions. Despite the emergence of alternative noninvasive techniques for the diagnosis of coronary aretry disease (CAD) and the assessment of prognosis of viability, such as ergo- stress tests, stress echocardiography, the use and application of nuclear cardiology techniques have continued to increase.
For many years, planar imaging and SPECT with 201Tl (201 Thalium) constituted the only scintigraphic techniques available for detecting CAD and assessing prognosis in patients undergoing stress perfusion imaging. The major limitation of 201Tl scintigraphy is the high false/positive rate observed in many laboratories, which is attributed predominantly to image attenuation artefact and variants of normal that are interpreted as defects consequent to a significant coronary artery stenoses.
In recent years, new 99mTc (technetium) labeled perfusion agents have been introduced into clinical practice to enhance the specificity of Single Photon Emission Cumputed Tomography (SPECT) and to provide additional information regarding and global left ventricular systolic function via ECG gating of images [3, 4, 8]. It was immediately apparent that the quality of images obtained with these 99mTc-labeled radionuclides was superior to that images obtained with 201Tl because of the more favorable psysical characteristic of 99mTc imaging with gamma camera. Perhaps most importantly, 99mTc imaging allows easy gated acquisition, permitting simultaneous evaluation of regional systolic thickening, global left ventricular function (LVEF), and myocardial perfusion. One the most significant avdances in myocardial perfusion imaging in the past decade is the development of quantitative SPECT perfusion imaging.
Indications for nuclear cardiology procedures
CAD is still the single greatest cause of death of men and women in the world, despite a declining total death rate. The reduction of the morbidity and mortality due to CAD is thus primary importance. The first step in evaluating patients for CAD involves the assessment of the presence of traditional risk factors. Symptoms suggestive of CAD, in addition to other risk factors, drive decisions for further testing.
In patients able to exercise, the diagnostic accuracy of stress myocardial perfusion imaging (MPI) is significantly higher than the ETT alone and provides greater risk stratification for predicting the future cardiac events.
Nuclear cardiology –practical applications
- ETT exercise treadmill test
- DIP-ECHO dipyridamole echocardiography
- DOB-ECHO dobutamine echocardiography
- DIP- MIBI dipyridamole myocardial perfusion imaging with Tc-99m MIBI
- DOB-MIBI dobutamine myocardial perfusion imaging with Tc-99m MIBI
Evaluating and determination CULPRIT lesion, an indication for interventional cardiology
One of the most powerfull uses of MPI is the evaluation of the risk for future events in patients with suspected or known CAD. Over the years, MPI has evolved as an essential tool in the evaluation and assessment of patient prior to coronary revascularization. It has a dual role. Prior to coronary angiography, MPI is extremely useful in documenting ischemia and determining the functional impact of single or multiple lesions subsequently identified. Despite some limitations in the setting of multivessel disease, MPI remains the test of choice for identifying the lesion responsible for the ischemic symptoms. The primary objective of those study is to determine and localize the culprit lesion. The authors introduce parameters SRS (summary reversible score) and ISRS (index of summary reversible score), under the angiographically detected coronary narrowing ≥75% for the least one coronary artery. Coronary angiography, considered the “gold standard” for the diagnosis of CAD, often does not provide information about the physiologic significance of atherosclerotic lesions, especially in borderline lesions. More importantly, it does not provide a clear marker of risk of adverse events, especially in patients with moderate disease severity. The presence of normal scintigraphic MPI study at a high level of stress ( ≥ 85 % of maximum predicted heart rate) or proper pharmacologic stress carries a very benign prognosis, with mortality rate less than 0.5% per year. This finding has been reproduced in many studies. Iskander and Iskandiran, pooling the results of SPECT imaging from more than 12000 patients in 14 studies, demonstrated that the events rate (death/MI) for patients with normal MPI finding is 0.6%, whereas abnormal study carries 7.4% per year event rate, a 12-fold increase.
The size and severity of the perfusion abnormality provide powerful prognostic information and has been shown to directly relate to outcome. MPI perfusion imaging and determination of culprit lesion is more predicitble of cardiac events than coronary angiography. As MPI imaging may identify those patients at high risk for subsequent cardiac events, perfusion imaging may be used to help guide further testing and revascularization procedures. Myocardial perfusion imaging provides information on the extent and location of myocardial ischemia. The assessment of jeopardized myocardium may be performed and provides a measure of the relative value of PTCA in terms of the amount of jeopardized myocardium. The location of the stenosis may dictate the area at risk: extent and severity of perfusion defects were significantly smaller in patients with proximal compared with distal coronary artery occlusions.
The aim of the study Baskot at al.(*) was to determine and localize culprit lesion by MPI in cases of angiographically detected coronary narrowing ≥ 75% of at least one coronary artery. In the study four hundred and thirty-seven [437] patients were studied. Angiographically detected significant coronary narrowing (≥ 75% luminal stenosis) was found in all before PCI. All the patients were submitted to MPI 99mTc-MIBI, with pharmacologic dipyridamole stress protocol with concomitant low level bicycle exercise 50 W (DipyEX). We measured relative uptake 99mTc-MIBI for each myocardial segment using short-axis tomogram study. A 5-point scoring system was used to assess the difference between uptake degree in stress and rest studies for the same segment, and we created two indices: Sum reversible score (SRS), Index of sum reversibility score (ISRS). In the results a total 1311 vascular territories (7429 segments) were analyzed before elective percutaneous coronary intervention (ePCI). Overall sensitivity, specificity and accuracy using SRS were 89.7%, 86, 7%, and 88, 2%, with a positive predictive value of 92, 7%. Overall sensitivity, specificity and accuracy using ISRS were 92.8%, 89.1%, and 92.3%, and the positive predictive value was 93.7%.
Pathophysiology and investigation of coronary artery disease
Ever D Grech
University of Manitoba, Winnipeg
BMJ 2003;326:1027–30
In affluent societies, coronary artery disease causes severe disability and more death than any other disease, including cancer. It manifests as angina, silent ischemia, unstable angina, myocardial infarction, arrhythmias, heart failure, and sudden death. Coronary artery disease is almost always due to atheromatous narrowing and subsequent occlusion of the vessel. A mature plaque is composed of two constituents, each associated with a particular cell population. The lipid core is mainly released from necrotic “foam cells”—monocyte derived macrophages, which migrate into the intima and ingest lipids. The connective tissue matrix is derived from smooth muscle cells, which migrate from the media into the intima, where they proliferate and change their phenotype to form a fibrous capsule around the lipid core.
Stress echocardiography
Stress induced impairment of myocardial contraction is a sensitive marker of ischemia and precedes electrocardiographic changes and angina. Cross sectional echocardiography can be used to evaluate regional and global left ventricular impairment during ischaemia, which can be induced by exercise or an intravenous infusion of drugs that increase myocardial contraction and heart rate (such as dobutamine) or dilate coronary arterioles (such as dipyridamole or adenosine).
Radionuclide myocardial perfusion imaging
Thallium-201 or technetium-99m (99mTc-sestamibi, 99mTc-tetrofosmin) is injected intravenously at peak stress, and its myocardial distribution relates to coronary flow. Images are acquired with a gamma camera. This test can distinguish between reversible and irreversible ischemia (the latter signifying infarcted tissue). Although it is expensive and requires specialised equipment, it is useful in patients whose exercise test is non-diagnostic or whose exercise ability is limited.
A multigated acquisition (MUGA) scan assesses left ventricular function and can reveal salvageable myocardium in patients with chronic coronary artery disease. It can be performed with either thallium scintigraphy at rest or metabolic imaging with fluorodeoxyglucose by means of either positron emission tomography (PET) or single photon emission computed tomography (SPECT).
Intravascular ultrasound (IVUS)
In contrast to angiography, which gives a two dimensional luminal silhouette with little information about the vessel wall, intravascular ultrasound provides a cross sectional, three dimensional image of the full circumference of the artery. It allows precise measurement of plaque length and thickness and minimum lumen diameter, and it may also characterise the plaque’s composition. It is often used to clarify ambiguous angiographic findings and to identify wall dissections or thrombus. It is most useful during percutaneous coronary intervention, when target lesions can be assessed before, during, and after the procedure and at follow up. The procedure can also show that stents which seem to be well deployed on angiography are, in fact, suboptimally expanded.
Interventional Cardiology for Structural Heart Disease
Georgios Parcharidis
Hellenic J Cardiol 2012; 53: 403-404
Many questions arise from this “explosion” of new technologies. Is all this enthusiasm justified and supported by robust scientific evidence? Which is the best way to implement these new treatment options? What is the role of “traditional” surgical treatment? How can we decide which patient should be treated percutaneously and which surgically? What level of training and experience should an interventional cardiologist (or a centre) have in order to perform structural and/or congenital heart disease interventions?
With regard to the scientific evidence, it should be noted that, currently, the number of randomized clinical trials and the duration of follow up is quite limited. Thus, great caution should be exercised in patient selection and planning for these complex procedures. In addition, careful data collection and, ideally, inclusion in a patient registry would increase surveillance and, therefore, patient safety.
Notably, for the majority of structural and congenital heart diseases, surgery is still considered the “gold standard”. It is now globally accepted that decision making for patients with cardiovascular disease should be done in the context of a “Heart Team”, with close collaboration between cardiologists, cardiothoracic surgeons, anesthesiologists, imaging specialists and, occasionally, other specialists. Some patients will benefit more from transcatheter interventions whereas others will do better with surgery. Based on specific criteria, the role of the Heart Team is to identify (and treat) those patients.
PET vs. SPECT: Will PET Dominate Over the Next Decade?
DAIC July/August 2013 pp28-31. www. DIcardiology.com
The future success of PET may be grounded in its inherently better image resolution. In cardiac scanning, it has generally been reported that PET offers a resolution of 5 to 7 mm, compared with a cardiac SPECT resolution of 12 to 15 mm. Better performance has allowed data to emerge suggesting that as many as one in 10 scans interpreted as normal on SPECT would have been abnormal if done on PET due to the presence of unseen microvascular, triple-vessel disease. PET’s superior diagnostic capability is achieved partly through advances in hardware, particularly quantification, which leverages numerical precision to identify global perfusion defects in the heart that otherwise might be hidden from qualitative SPECT scans.
A big difference between the two technologies is the half-life of the isotope that each radiopharmaceutical tracer uses. SPECT tracers have a relatively long half-life (technetium-99m has a half-life of six hours), whereas rubidium-82 is only 75 seconds. This short half-life is a limitation of the current front-line cardiac PET radiotracer, which does not leave much room for error when imaging and presents the inability to do exercise stress testing. New iterative reconstruction (IR) software such as UltaSPECT is improving SPECT image quality by boosting the signal-to-noise ratio. Just as in CT scans, IR can also help reduce dose by enhancing lower-quality scans.
Part III
Heart Failure Patients
Heart Failure Complicating Non–ST-Segment Elevation Acute Coronary Syndrome -Timing, Predictors, and Clinical Outcomes
J Am Coll Cardiol HF 2013;1(3): 223–9This study sought to describe the occurrence and timing of heart failure (HF), associated clinical factors, and 30-day outcomes in patients with non–ST-segment elevation acute coronary syndromes (NSTE-ACS). Using pooled patient-level data from 7 clinical trials from 1994 to 2008, we describe the occurrence and timing of HF,associated clinical factors, and 30-day outcomes in NSTE-ACS patients. HF at presentation was defined as Killip classes II to III; patients with Killip class IV or cardiogenic shock were excluded. New in-hospital cases of HF included new pulmonary edema. After adjusting for baseline variables, we created logistic regression models to identify clinical factors associated with HF at presentation and to determine the association between HF and 30-day mortality.Of 46,519 NSTE-ACS patients, 4,910 (10.6%) had HF at presentation. Of the 41,609 with no HF at presentation, 1,194 (2.9%) developed HF during hospitalization. A total of 40,415 (86.9%) had no HF at any time. Patients presenting with or developing HF during hospitalization were older, more often female, and had a higher risk of death at 30 days than patients without HF (adjusted odds ratio [OR]: 1.74; 95% confidence interval: 1.35 to 2.26). Older age, higher presenting heart rate, diabetes, prior myocardial infarction (MI), and enrolling MI were significantly associated with HF during hospitalization. In this large cohort of NSTE-ACS patients, presenting with or developing HF during hospitalization was associated with an increased risk of 30-day mortality.
Outcomes Following Heart Transplantation among Those Bridged with VAD
Jeffrey Shuhaiber MD
University of Cincinnati and Cincinnati Children’s Hospital
www.intechopen.com
Clinical assessment of outcome for post heart transplant recipients who were bridged with ventricular assist device is essential for service evaluation, device evaluation and audit. We will review the clinical outcomes measured so far in the field of heart transplant recipients who were bridged with VAD. In this chapter we will review the ongoing methods of assessment of outcomes for transplant recipients bridged by VAD and discuss the potential challenges facing the clinicians. We will finalize with brief conclusions and future directions.
Survival following heart transplantation: Does VAD Type matter?
There have been many clinical studies comparing outcomes following heart transplantation. Only one has been done in a multicenter fashion with clinically relevant as well as a robust risk-adjustment. In 2006 we asked the question- does survival differ between those who did and did not receive the left ventricular assist device (LVAD) following heart transplantation? And in summary we found that survival following heart transplantation for patients who received an LVAD prior to transplantation was comparable to those who did not receive an LVAD. The results of this study were published as lead research article in the British Medical Journal earlier this year (Shuhaiber).
We reviewed all patients above 18 years of age who received heart transplants registered in the United Network for Organ Sharing (UNOS) Registry from 1996 to 2004. The study included 2786 status 1/1A/1B heart transplant patients. We used the entry data for all patients who received LVAD pulsatile device. Our study design included a prospective cohort study in which post-transplant survival between patients who received an LVAD and those who did not receive an LVAD was compared.
1:1 propensity score matching analysis was also performed. Comparisons of survival distributions were made using the Kaplan-Meier method and the risk ratios were estimated using Cox proportional model. Our primary outcomes as well as risks and exposures included survival following heart transplantation in heart transplant recipients who did or did not receive ventricular assist device. The strength of the study was in adopting a robust statistical methodology that can adequately control for confounding variables. A stratified propensity score analysis of data revealed that the risk of death following heart transplantation in an LVAD patient was not significantly different from those who did not have an LVAD within each stratum (see table for estimated hazard ratios and their 95% confidence intervals). A 1:1 propensity score matching analysis also revealed no significant difference in post heart transplant survival between the two groups (hazard ratio = 1.18, 95% CIs=0.75 to1.86). The propensity score matching was performed in order to control potential selection biases that can lead to a false association (or false lack of association) between LVAD and survival.
Part IV
Mechanical Heart Devices
The treatment of heart failure at end stage myocardial function has depended on having patients on waiting lists until the time that a donor heart becomes available. Waiting times are within 1.5 to 4.5 years. This required the development for mechanical support until a suitable donor is found. The expectation for future devices will be that suitable mechanical heart assist devices for selected patients will possibly alleviate the need for a donor heart.
There are two main types of mechanical assist devices. One type ios actually a total artificial heart, and the other is an assist that in complementary to the still functioning weak left ventricle. The VAD was just discussed in the preceding discussion. It has a pump that is attached to the atria and the pump controls the flow of blood through the pulmonary circulation. This device is extremely important for patients who have sufficient LV function to not require a TAH.
The total artificial heart (TAH) has been dominated by use of either of two models – the Syncardia temporary artificial heart, and the AbiCor. The difference between them is that one has an externalization outside the thorax to an electrical source. The Syncardia model is a modern day improvement of Jarvik-7.
The controlled flow is a miniature motor that has a rotor that moves the blood forward. Of course, it presents a problem with respect to blood cell damage and anemia. One of the innovations to the blood flow control has been that it flows without a heart beat. The most significant innovation is the entry into the market of a new model, the Carmat, from France. The Carmat would reduce the hemolysis that is associated with the flow of RBCs along a synthetic lining. How? It has the blood in contact with a cow skin lining.
Part V
Heart Transplant
The heart transplant is a technique that has been mastered at a number of excellent cardiothoracic surgical sites, and the facilities are being replaced by Hybrid Units that accommodate cardiology and surgical interventions. This brings to fruition the concept of a “Heart Team”. The procedure has risks of complication, either in the patient condition, or in environmental, or other factors the surgeon has no control over.
These factors include, associated comorbidities, such as
- diabetes mellitus
- Late NYHF Stage 4
- Late stage renal disease
- mismatch of Graft vs Host
- infection
Other related articles published on this Open Access Online Scientific Journal, include the following:
Pearlman, JD and A. Lev-Ari, Cardiovascular Complications: Death from Reoperative Sternotomy after prior CABG, MVR, AVR, or Radiation; Complications of PCI; Sepsis from Cardiovascular Interventions
Larry H Bernstein, Advanced Topics in Sepsis and the Cardiovascular System at its End Stage
Pearlman, JD and A. Lev-Ari Cardiac Resynchronization Therapy (CRT) to Arrhythmias: Pacemaker/Implantable Cardioverter Defibrillator (ICD) Insertion
Lev-Ari, A. 3D Cardiovascular Theater – Hybrid Cath Lab/OR Suite, Hybrid Surgery, Complications Post PCI and Repeat Sternotomy