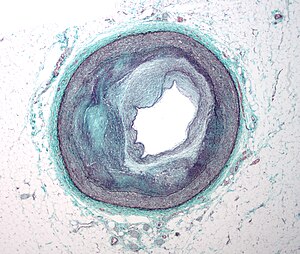
microglia and brain maintenance
Larry H. Bernstein, MD, FCAP, Curator
LPBI
Mapping mosaicism: Tracing subtle mutations in our brains
Posted on January 14, 2015 by Nancy Fliesler
Posted in All Posts, Information technology
More On: brain development, DNA sequencing, genetics, mosaicism, neuroscience, somatic mutations
DNA sequences were once thought to be the same in every cell, but the story is now known to be more complicated than that. The brain is a case in point: Mutations can arise at different times in brain development and affect only a percentage of neurons, forming a mosaic pattern.
Now, thanks to new technology described last week in Neuron, these subtle “somatic” brain mutations can be mapped spatially across the brain and even have their ancestry traced.
Like my family, who lived in Eastern Europe, migrated to lower Manhattan and branched off to Boston, California and elsewhere, brain mutations can be followed from the original mutant cells as they divide and migrate to their various brain destinations, carrying their altered DNA with them.
“Some mutations may occur on one side of the brain and not the other,” says Christopher Walsh, MD, PhD, chief of Genetics and Genomics at Boston Children’s Hospital and co-senior author on the paper. “Some may be ‘clumped,’ affecting just one gyrus [fold] of the brain, disrupting just a little part of the cortex at a time.”
This tracking capability represents a significant advance for genetics research. And for neuroscientists, it provides a new way to study both the normal brain and brain disorders like epilepsy, autism and intellectual disability.
Walsh and colleagues studied normal brain tissue from a teenage boy who had passed away from other causes. Sampling in more than 30 brain locations, they used deep, highly sensitive, whole-genome sequencing of one neuron at a time—unlike usual methods, which sequence thousands or millions of cells mixed together and simply read out an average.
http://vectorblog.org/wp-content/uploads/2015/01/Walsh-figure3B-v2-1024×735.jpg
The blue and green boxes indicate different degrees of mosaicism (based on proportion of cells affected) in the left half of this teen’s normal brain. The blue shaded area indicates that retrotransposon mutation #1 (blue boxes) is limited to a focal area in the middle frontal gyrus. The empty boxes indicate areas where mutation #1 was not detected. (Courtesy Gilad Evrony, PhD, Boston Children’s Hospital)
Next, using technology developed by Alice (Eunjung) Lee in the lab of Peter Park, PhD, at Harvard Medical School’s Center for Biomedical Informatics, they zeroed in on inserted bits of DNA caused by retrotransposons, one type of mutation that can arise as the brain develops. These essentially served as markers that allowed cell lineages to be traced.
“Our findings are intriguing because they suggest that every normal brain may in fact be a mosaic patchwork of focal somatic mutations, though in normal individuals most are likely silent or harmless,” says Gilad Evrony, PhD, in the Walsh Lab.
http://vectorblog.org/wp-content/uploads/2015/01/Walsh-figure5-1024×509.jpg
This model illustrates the origins of two somatic retrotransposon mutations during prenatal development and their subsequent dissemination in the brain. Insertion #2 (in green) occurred soon after conception; #1 (in blue) happened sometime later during brain development. The ‘pie slices’ show a closeup of the layers of the cerebral cortex. Later in development, additional somatic mutations occurred inside insertions #1 and #2, creating new, smaller sublineages of cells. (Courtesy Gilad Evrony, PhD)
A parallel study from Walsh’s lab in 2014 used single-neuron sequencing to find copy number variants— a different type of mutation affecting the number of copies of chromosomes or chromosome fragments. It, too, found the mutations to be present in normal brains as well as neurologically diseased brains.
Walsh and others speculate that some somatic brain mutations might play a role in autism, epilepsy, schizophrenia and other unsolved neuropsychiatric diseases whose causes are mostly still a mystery.
“It is possible that a whole new class of brain disorders may exist that has not been previously recognized,” says Evrony. “In such disorders, a somatic mutation may subtly affect only one small part of the brain involved in a specific ability, for example language, while sparing the rest of the brain.”
Read more:
Tracking subtle brain mutations, systematicallyTool can trace and spatially map “mosaic” mutations in the brain
http://www.prnewswire.com/news-releases/tracking-subtle-brain-mutations-systematically-300017369.html
BOSTON, Jan. 7, 2015 /PRNewswire-USNewswire/ — DNA sequences were once thought to be identical from cell to cell, but it’s increasingly understood that mutations can arise during brain development that affect only certain groups of brain cells. A technique developed at Boston Children’s Hospital allows these subtle mutation patterns to be traced and mapped spatially for the first time. This capability is a significant advance for genetics research and provides a new way to study both the normal brain and brain disorders such as epilepsy and autism.
Described in the January 7th issue of Neuron, the technique uses “deep,” highly sensitive whole-genome sequencing of single neurons and a new technology that identifies inserted bits of DNA caused by retrotransposons, one of several kinds of so-called somatic mutations that can arise as the brain develops.
The technique picks up somatic mutations that affect just a fraction of the brain’s cells, in a “mosaic” pattern. It also allows “lineage tracing,” showing when during brain development the mutations arise and how they spread through brain tissue as the mutated cells grow, replicate and migrate, carrying the mutation with them.
“There is a lot of genetic diversity from one neuron to the other, and this work gets at how somatic mutations are distributed in the brain,” says Christopher Walsh, MD, PhD, chief of Genetics and Genomics at Boston Children’s and co-senior author on the paper. “Some mutations may occur on one side of the brain and not the other. Some may be ‘clumped,’ affecting just one gyrus [fold] of the brain, disrupting just a little part of the cortex at a time.”
The study examined brain tissue from a deceased 17-year-old who had been neurologically normal, sampling in more than 30 brain locations. It builds on work published by the Walsh lab in 2012, which developed methods to sequence the genomes of single neurons, and represents the first time single neurons have been sequenced in their entirety. The single-cell technique is better at detecting subtle mosaicism than usual DNA sequencing methods, which sequence many thousands or millions of cells mixed together and read out an average for the sample.
Somatic brain mutations, affecting just pockets of cells, can be harmful, and have been suggested as a possible cause of neurodevelopmental disorders such as autism, epilepsy or intellectual disability (see this review article for further background). But they also can be completely benign or have just a subtle effect.
“Our findings are intriguing because they suggest that every normal brain may in fact be a mosaic patchwork of focal somatic mutations, though in normal individuals most are likely silent or harmless,” says Gilad Evrony, PhD, in the Walsh Lab, co-first author on the Neuron paper. “These same technologies can now be used to study the brains of people who died from unexplained neuropsychiatric diseases to determine whether somatic mutations may be the cause.”
Finally, says Evrony, the findings provide a proof-of-principle for a systematic way of studying how brain cells disperse and migrate during development, “something that has not been possible to do before in humans,” he says.
Co-first author Alice Eunjung Lee, PhD, from the lab of Peter Park, PhD, at the Center for Biomedical Informatics at Harvard Medical School, developed the study’s retrotransposon analysis tool, which detects somatic retrotransposon mutations in single-cell sequencing data.
Mirroring these findings, study published by Walsh’s lab in 2014 used single-neuron sequencing to detect copy number variants—another type of mutation affecting the number of copies of chromosomes or chromosome fragments. The study found that these mutations can occur in both normal and neurologically diseased brains.
Evrony and Lee are first authors on the Neuron paper; Walsh and Park are senior authors. The research was supported by the National Institutes of Health (MSTP grant T32GM007753), the National Institute of Neurological Disorders and Stroke (R01 NS079277 and R01 NS032457), the Louis Lange III Scholarship in Translational Research, the Eleanor and Miles Shore Fellowship, the Research Connection and the Manton Center for Orphan Disease Research at Boston Children’s Hospital, the Paul G. Allen Family Foundation and the Howard Hughes Medical Institute.
SOURCE Boston Children’s Hospital
Beth Stevens: A transformative thinker in neuroscience
Posted on September 29, 2015 by Nancy Fliesler
Posted in All Posts, Drug discovery, Profiles
More On: Alzheimer’s disease, autism, FM Kirby Neurobiology Center, glial cells, neuroscience, synapse development
http://vector.childrenshospital.org/2015/09/beth-stevens-a-transformative-thinker-in-neuroscience/
https://youtu.be/6DOYTpXkLOY
When 2015 MacArthur “genius” grant winner Beth Stevens, PhD, began studying the role of glia in the brain in the 1990s, these cells—“glue” from the Greek—weren’t given much thought. Traditionally, glia were thought to merely protect and support neurons, the brain’s real players.
But Stevens, from the Department of Neurology and the F.M. Kirby Neurobiology Center at Boston Children’s Hospital, has made the case that glia are key actors in the brain, not just caretakers. Her work—at the interface between the nervous and immune systems—is helping transform how neurologic disorders like autism, amyotrophic lateral sclerosis (ALS), Alzheimer’s disease and schizophrenia are viewed.
Soon after college graduation in 1993, without prior experience in neuroscience, she helped discoveran interplay between neurons and glial cells known as Schwann cells that controlled production of the nerve insulation known as myelin It was one of the early pieces of evidence that glia and neurons talk to each other.
In 2007, while still a postdoctoral fellow, Stevens showed how star-shaped glial cells called astrocytes influence the development of synapses, or brain connections. Studying neurons, her lab showed that a gene called C1q was markedly more active when astrocytes were present. C1q is an immune gene, one nobody had expected to see in a normal brain. In the context of disease, it initiates the complement cascade, an immunologic pathway for tagging unwanted cells and debris for clearance by other immune cells.
But in healthy developing brains, Stevens showed, C1q was concentrated at developing synapses, or brain connections, apparently marking certain synapses for pruning.
Then in 2012, the Stevens lab showed that microglia—another type of glia usually thought of as immune cells themselves—actively sculpt the brain’s wiring. They literally trim away unwanted, inappropriate synapses by eating them—in the same way they’d engulf and destroy invading bacteria.
http://19g6dy4by8jx1b5cx74fh0f2.wpengine.netdna-cdn.com/wp-content/uploads/2012/06/Microglial-cell.jpg
That paper was cited by the journal Neuron as the year’s most influential paper.
The same year, she received a Presidential Early Career Award for Scientists and Engineers, honoring her innovative research and scientific leadership.
Stevens’s current investigations are looking at synapse loss—a hallmark of neurodegenerative conditions such as Alzheimer’s—and trying to understand why it occurs. Her lab’s recent work suggests that normal pruning mechanisms that are active during early brain development get re-activated later in life. Intervening with this activation could lead to a new treatment approach, she believes.
Stevens isn’t the only brain researcher at Boston Children’s to become a MacArthur fellow. Neurosurgeon Benjamin Warf, MD, received the honor in 2012.
For more:
Immune cells “sculpt” brain circuits — by eating excess connections
Posted on June 5, 2012 by Nancy Fliesler
Posted in All Posts, Drug discovery, Pediatrics
More On: ALS, Alzheimer’s disease, autism, brain development, epilepsy, glaucoma, Huntington’s disease, Lou Gehrig’s disease,Parkinson’s disease, synapse development
https://youtu.be/wb8UAyf8Nhw
The above movie shows an immune cell caught in the act of tending the brain—it’s just eaten away unnecessary connections, or synapses, between neurons.
That’s not something these cells, known as microglia, were previously thought to do. As immune cells, it was thought that their job was to rid the body of unwanted pathogens and debris, by engulfing and digesting them.
The involvement of microglia in the brain’s development has started to be recognized only recently. The latest research finds that microglia tune into the brain’s cues, akin to the way they survey their environment for invading microbes, and get rid of excess synapses the same way they’d dispatch these invaders—by eating them.
It’s a whole other way of understanding how the healthy brain develops—at the hands of cells that were once thought to be merely nerve “glue” (the literal meaning of “glia” from the Greek), playing a protective role to neurons, say investigators Beth Stevens, PhD, and Dori Schafer, PhD, of the F.M. Kirby Neurobiology Center at Boston Children’s Hospital.
“In the field of neuroscience, glia have often been ignored,” says Stevens. “But glia aren’t the nerve glue, they’re actively communicating with neurons. People have gotten a new respect for glia and are hungry to know more about them.”
Such knowledge could eventually shed light on brain disorders ranging from autism to Alzheimer’s.
The “eat me” sign
We’re all born with more brain connections than we need. As we begin to encounter our world, they’re trimmed back to fine-tune our circuitry. It’s a bit of an oversimplification, but Stevens and Schafer demonstrated last week in the journal Neuron that when two neurons start talking to each other less – because their connection is no longer important to our lives– the microglia notice that and prune the synapse away.
To study microglia’s pruning activity, Stevens and Schafer used a time-honored model: the visual system. When you cover one eye soon after birth, you force the brain to rewire: Brain connections with the covered eye weaken and those synapses eventually get eliminated.
Using this model, Stevens and Schafer showed that microglia take their cues from a set of signals also used by the immune system, known as the complement cascade. Specifically, microglia carry receptors that recognize the complement protein C3—the same protein found on synapses that are destined for elimination.
“We think that weaker synapses are being tagged with C3, and that microglia are eliminating them just as macrophages would eliminate bacteria,” says Schafer. “C3 is like an ‘eat me’ signal.”
As a postdoctoral fellow in 2007, Stevens showed that neurons are loaded with complement proteins soon after birth, just when pruning is at its peak. In the new study, she and Schafer deliberately disrupted complement signaling in mice—stripping the microglia of C3 receptors, or blocking those receptors with a drug. When they did so, pruning of irrelevant synapses didn’t occur.
Stevens thinks their findings might have relevance for brain disorders. Developmental brain disorders such as autism, epilepsy or schizophrenia are increasingly seen as disorders of synapse development, and some data suggest that microglia and/or the complement cascade are involved.
At the other end of the spectrum, scientists have noted that microglia—normally in a resting state in adults—are activated in neurodegenerative diseases like glaucoma, Alzheimer’s disease, Lou Gehrig’s disease, Huntington’s disease and Parkinson’s disease. Subtle changes have been found in synapses that might cause them to be targeted for elimination.
So could targeting microglia or the complement cascade prevent synapse loss or alter pruning in these diseases? “All this is still very speculative,” Stevens cautions. “We first need to understand normal brain development.”
Beth Stevens
Neuroscientist
Assistant Professor of Neurology, F. M. Kirby Neurobiology Center, Boston Children’s Hospital
Department of Neurology, Harvard Medical School
Boston, Massachusetts
Age: 45
Published September 28, 2015
https://www.macfound.org/fellows/946/#sthash.GpHuiEC6.dpuf
Beth Stevens is a neuroscientist whose research on microglial cells is prompting a significant shift in thinking about neuron communication in the healthy brain and the origins of adult neurological diseases. Until recently, it was believed that the primary function of microglia was immunological; they protected the brain by reducing inflammation and removing foreign bodies.
Stevens identified an additional, yet critical, role: the microglia are responsible for the “pruning” or removal of synaptic cells during brain development. Synapses form the connections, or means of communication, between nerve cells, and these pathways are the basis for all functions or jobs the brain performs. Using a novel model system that allows direct visualization of synapse pruning at various stages of brain development, Stevens demonstrated that the microglia’s pruning depends on the level of activity of neural pathways. She identified immune proteins called complement that “tag” (or bind) excess synapses with an “eat me” signal in the healthy developing brain. Through a process of phagocytosis, the microglia engulf or “eat” the synapses identified for elimination. This pruning optimizes the brain’s synaptic arrangements, ensuring that it has the most efficient “wiring.”
Stevens’s discoveries indicate that our adult neural circuitry is determined not only by the nerve cells but also by the brain’s immune cells. Her work suggests that adult diseases caused by deficient neural architecture (such as autism and schizophrenia) or states of neurodegeneration (such as Alzheimer’s or Huntington’s disease) may be the result of impaired microglial function and abnormal activation of this pruning pathway. Stevens is redefining our understanding of how the wiring in the brain occurs and changes in early life and shedding new light on how the nervous and immune systems interact in the brain, both in health and disease.
Beth Stevens received B.S. (1993) from Northeastern University and a Ph.D. (2003) from the University of Maryland. She was a postdoctoral fellow (2005–2008) at Stanford University and is currently an assistant professor in the Department of Neurology at Harvard Medical School and the F. M. Kirby Neurobiology Center at Boston Children’s Hospital. She is also an Institute Member of the Broad Institute of MIT and Harvard. Her scientific papers have appeared in such journals as Neuron, Science, Proceedings of the National Academy of Sciences, and Nature Neuroscience, among others.
– See more at: https://www.macfound.org/fellows/946/#sthash.GpHuiEC6.dpuf
Portraits of scientists who are making a mark on autism research.
http://spectrumnews.org/news/profiles/beth-stevens-casting-immune-cells-as-brain-sculptors/
Beth Stevens: Casting immune cells as brain sculptors
BY NICHOLETTE ZELIADT / 24 SEPTEMBER 2015
Shortly after Beth Stevens launched her lab at Boston Children’s Hospital in 2008, she invited students from the Newton Montessori School, in a nearby suburb, to come for a visit. The children peered at mouse and rat brains bobbing in fluid-filled jars. They also learned how to position delicate slices of brain tissue on glass slides and inspect them with a microscope.
This visit sparked a running relationship with the school, with a steady stream of students visiting the growing lab each year. Soon it became too complicated to bring so many children to the lab, so Stevens decided to take her neuroscience lessons on the road, visiting a number of local elementary schools each year. Last year, she dropped in on the classrooms of her 5- and 8-year-old daughters, Zoe and Riley.
“The kids got really excited,” Stevens says. “It’s become such a thing that the principal wants me to come back for the whole school.”
Stevens’ enthusiasm for science has left a lasting impression on researchers, too. Her pioneering work points to a surprise role in brain development formicroglia, a type of cell once considered to simply be the brain’s immune defense system, cleaning up cellular debris, damaged tissue and pathogens. But thanks to Stevens, researchers now appreciate that these non-neuronal cells also play a critical role in shaping brain circuits.
In a 2012 discovery that created a buzz among autism researchers, Stevens and her colleagues discovered that microglia prune neuronal connections, calledsynapses, in the developing mouse brain. The trimming of synapses is thought to go awry in autism. And indeed, emerging work from Stevens’ lab hints at a role for microglia in the disorder.
Stevens has already earned praise and several prizes for her work. In 2012, shereceived the Presidential Early Career Award for Scientists and Engineers, the most prestigious award that the U.S. government bestows on young scientists. And in October, she’ll deliver one of four presidential lectures at the world’s largest gathering of neuroscientists — the annual meeting of the Society for Neuroscience — an honor she shares with three neuroscience heavyweights, including two Nobel laureates.
“The field is probably expecting a lot from Beth,” says Jonathan Kipnis, professor of neuroscience at the University of Virginia. Stevens has put microglia at the forefront, Kipnis says. “What used to be a stepchild of neuroscience research is now getting a lot of attention, and I think in part it’s due to her research.”
Curious mind:
Stevens was born in 1970 in Brockton, Massachusetts, where her mother taught elementary school and her father was the school’s principal. As a child, she was deeply inquisitive, eager to understand how things work. She enjoyed collecting bugs and worms, and would analyze these precious specimens in makeshift labs in her backyard.
But a career in science wasn’t on her radar until high school, when she took a biology class with an inspiring teacher named Anthony Cabral. “He totally made me realize that this could be a career, that I could be a scientist,” Stevens says. “It was that one class that changed it, and I’m like, ‘Okay, I’m going to do this.’”
In 1988, she began studying biology at Northeastern University in Boston, which offered an unusual opportunity. It had a unique cooperative education program that allowed Stevens to spend several semesters working full time in medical labs after finishing her coursework.
After that experience, Stevens knew she wanted to find a job in a research lab. After graduating in 1993, she joined her then-boyfriend Rob Graham, now her husband, in Washington, D.C., where he had landed a job in the U.S. Senate. Stevens headed to the National Institutes of Health (NIH) in Rockville, Maryland, to apply for a job as a research assistant.
At around the same time, neuroscientist R. Douglas Fields was launching his lab at the NIH. He studied how neural impulses influence glia — a class of non-neuronal cells that includes microglia — and shape the structure of the developing brain. Fields readily hired Stevens despite her lack of expertise in neuroscience. “I was impressed with her work ethic, energy and drive,” he says.
Stimulating research:
In Fields’ lab, Stevens used a multi-compartment cell culture system to investigate whether stimulating neurons influences the activity of Schwann cells, glial cells that produce a fatty substance called myelin, which insulates nerves1. She discovered that patterns of neural impulses similar to those that occur during early development influence the maturation of Schwann cells and the production of myelin.
The findings added to mounting evidence that glia and neurons communicate with each other, a newly emerging concept at the time.
“What I loved about the glia research was that there were so few neuroscientists studying it; it was such a mysterious part of neuroscience,” Stevens says. “Those years in Doug’s lab were really exciting because it was a new field.”
Stevens spent five years in Fields’ lab. “She was doing extraordinary work,” Fields says. “She had the potential and the interest to do neuroscience research, and I recommended that she should consider going to graduate school.”
But Stevens didn’t want to give up her position in the lab, and at that time, the NIH did not allow its researchers to have graduate students. So she and Fields convinced the University of Maryland, College Park, just 10 miles away, to allow her to take graduate courses in neuroscience while completing the necessary research for her Ph.D. in Fields’ lab.
In 2000, less than two years after starting graduate school, Stevens published a paper in Science showing that nerves in the peripheral nervous system (located outside the brain and spinal cord) use chemical signals to communicate with Schwann cells2. Two years later, she reported in Neuron that a similar form of communication occurs in the brain, between neurons and oligodendrocytes, the myelin-producing cells in the brain3.
As she was closing in on her Ph.D., Stevens sought career advice from Story Landis, then-director of the National Institute of Neurological Disorders and Stroke. Landis turned Stevens on to the possibility of starting her own lab one day. “I convinced her that she really had the abilities and energy and intelligence to run an independent research program,” Landis says.
In 2004, Stevens sought a postdoctoral fellowship with neurobiologist Ben Barres at Stanford University. “She was already seen as a leading researcher in the glial field,” recalls Barres, who promptly hired her. “She had done all sorts of beautiful work on glia.”
In Barres’ lab, Stevens continued to explore the dialogue between neurons and glia, turning her attention to star-shaped glia called astrocytes. Barres and his team had discovered that astrocytes help neurons form synapses4. To get a better handle on this process, Stevens examined how astrocytes influence gene expression in neurons in the developing mouse brain.
To her surprise, she found that astrocytes trigger neurons to produce a ‘complement’ protein that is best known for its role in the immune system. There, the protein serves as an ‘eat me’ signal, flagging pathogens and debris for removal. She found that neurons deposit this tag around immature synapses, but not mature ones, in mouse brain tissue, and mice that lack this protein have too many immature synapses. The findings suggested that astrocytes might help eliminate synapses by triggering the complement cascade5.
http://spectrumnews.org/wp-content/uploads/2015/09/20150929ProfileBethStevensChild350.jpg
Young recruit: Beth Stevens’ daughter Riley inspects brain tissue during a visit to her mother’s lab. | Courtesy of Beth Stevens
But it was still unclear exactly how the tagged synapses are cleared. The prime suspects were microglia, the only cells in the brain known to have the receptor for the ‘eat me’ signal.
Stevens set out to test this hypothesis in her own lab: After four years as a postdoc, she had decided to branch out on her own. In 2008, neuroscientist Michael Greenberg — chair of the neurobiology department at Harvard — recruited her to the Harvard-affiliated Boston Children’s Hospital. Even when her lab was in its infancy, she had little trouble convincing new staff to join her.
“A lot of people might be a little hesitant to join a new lab,” says Dorothy Schafer, a former postdoctoral fellow in Stevens’ lab who is now assistant professor of neurobiology at the University of Massachusetts-Worcester. “But I was so excited by the research, and she was so energetic and extremely positive, and just seemed like a very nice person.”
One decision Stevens made early on was to continue to studying microglia in mice rather than experiment with new model systems. “You’ll never see her working on songbirds, because she has this aversion to birds,” Schafer says. “I think they think her curly blond hair is a nest or something, and she’s had really bad experiences with many types of birds dive-bombing her head.”
Just four years into her foray as an independent researcher, Stevens found the proof she had been looking for. In 2012, her team published evidence that microglia eat synapses, especially those that are weak and unused6.
The findings pinned down a new role for microglia in wiring the brain. They also helped to explain how the brain, which starts out with a surplus of neurons, trims some of the excess away. Neuron named the paper its most influential publication of 2012.
Stevens continues to study the function of microglia in the healthy brain, most recently uncovering preliminary evidence that a certain protein serves as a ‘don’t eat me’ tag that protects synapses from being engulfed by microglia. She is also exploring the role of microglia in disorders such as autism.
Several studies suggest that microglia are more active and more numerous in the brains of people with autism than in controls. Stevens and her team are looking at whether the activity of microglia is altered during brain development in mouse models of autism.
Immunodulatory Thalidomides in ~ conjugants unleash proteasome degradation on ~ oncoproteins with distinct mechanisms- BRD4,MYC & PIM1 & little collteral damage to 7429 other proteins!
Imagine being able to specifically target a cancer protein for immediate destruction, slipping Robert Louis Stevenson’s notorious black spot into a crevice in the secondary structure and spelling imminent death. Well, this is what Winter et al. (2015) describe in a recent drug discovery report for Science.1 Using phthalimide conjugation, the researchers not only specifically marked BRD4, a transcriptional coactivator important in MYC oncogene upregulation, for proteasomal degradation, but also achieved reduced tumor burdens in vivo.
The research team combined two drugs, thalidomide and JQ1, exploiting the properties of each to create a bifunctional compound, dBET1, that drives the proteasomal degradation of BRD4. JQ1, which in itself is anti-oncogenic, selectively binds BET bromodomains on the transcription factor, thus competitively inhibiting BRD4 activity on chromatin. Thalidomide, a phthalimide-based drug with immunomodulatory properties, binds cereblon (CRBN) in the cullin-RING ubiquitin ligase (CRL) complex, which is important in proteasomal protein degradation.
After confirming that the new phthalimide conjugate, dBET1, retained affinity for BRD4 and that this binding was specific, the team used a human acute myelocytic leukemia (AML) cell line, MV4;11, to show that treatment with the conjugate over 18 hours reduced BRD4 abundance. The researchers also found this with dBET1 treatment of other human cancer cell lines (SUM159, MOLM13). Following this, Winter et al. investigated the mechanisms by which dBET1 inhibits BRD4. By focusing primarily on proteasome function, the researchers determined that the reduction in BRD4 abundance in MV4;11 cells is proteasomal and dependent on CRBN binding activity.
Having established targeted proteasomal degradation using the dBET1 conjugate, Winter et al. then investigated the proteomic consequences of treatment in MV4;11 cells. Scientists at the Thermo Fisher Scientific Center for Multiplexed Proteomics (Harvard Medical School) used quantitative proteomics analysis with an isobaric tagging approach to compare the immediate effects of dBET1 treatment following two hours of incubation with the responses to JQ1 and vehicle control. Spectral data analysis identified 7,429 proteins with few differences in response to either treatment. JQ1 treatment reduced levels of MYC and oncoprotein PIM1 similarly to the response following dBET1 incubation. However, treatment with the latter also reduced BRD2, BRD3 and BRD4 abundance, findings that the research team confirmed with specific immunoblotting. Measuring expression of mRNA showed that both treatments reduced levels of MYC and PIM1 abundance. However, Winter et al. found no difference in BRD3 and BRD4, suggesting that dBET1 reduces the protein levels by post-transcriptional regulation.
Investigating the antiproliferative potential of the phthalimide conjugate, dBET1, Winter and coauthors examined apoptotic response in both MV4;11 and DHL4 lymphoma cells, and in primary human AML blast cultures. Compared to JQ1 treatment, dBET1 stimulated a profound and prolonged apoptotic response in both cell lines, suggesting that targeted degradation could be a more effective treatment than target inhibition.

shapes of proteins as they shift from one stable shape to a different, folded one Protein-structural-changes
Orchestrating the unfolded protein response in health and disease
Randal J. Kaufman Department of Biological Chemistry,
Howard Hughes Medical Institute, University of Michigan Medical Center, Ann Arbor, Michigan, USA J. Clin. Invest. 110:1389–1398 (2002). http://dx.doi.org:/10.1172/JCI200216886
The endoplasmic reticulum (ER), the entrance site for proteins destined to reside in the secretory pathway or the extracellular environment, is also the site of biosynthesis for steroids and for cholesterol and many lipids. Given the considerable number of resident structural proteins and biosynthetic enzymes and the high expression of many secreted proteins, the total concentration of proteins in the this organelle can reach 100 mg/ml. The ER relies on an efficient system of protein chaperones that prevent the accumulation of unfolded or aggregated proteins and correct misfolded proteins that are caught in low-energy kinetic traps (see Horwich, this Perspective series, ref. 1).
These chaperone-mediated processes expend metabolic energy to ensure high-fidelity protein folding in the lumen of the ER. For example, the most abundant ER chaperone, BiP/GRP78, uses the energy from ATP hydrolysis to promote folding and prevent aggregation of proteins within the ER. In addition, the oxidizing environment of the ER creates a constant demand for cellular protein disulfide isomerases to catalyze and monitor disulfide bond formation in a regulated and ordered manner. Operating in parallel with chaperone dependent protein folding are several “quality control” mechanisms, which ensure that, of all proteins translocated into the ER lumen, only those that are properly folded transit to the Golgi compartment. Proteins that are misfolded in the ER are retained until they reach their native conformation or are retrotranslocated back into the cytosol for degradation by the 26S proteasome. The ER has evolved highly specific signaling pathways to ensure that its protein-folding capacity is not overwhelmed. These pathways, collectively termed the unfolded protein response (UPR), are required if the cell is to survive the ER stress (see Ron, this Perspective series, ref. 2) that can result from perturbation in calcium homeostasis or redox status, elevated secretory protein synthesis, expression of misfolded proteins, sugar/glucose deprivation, or altered glycosylation. Upon accumulation of unfolded proteins in the ER lumen, the UPR is activated, reducing the amount of new protein translocated into the ER lumen, increasing retrotranslocation and degradation of ER-localized proteins, and bolstering the protein-folding capacity of the ER. The UPR is orchestrated by the coordinate transcriptional activation of multiple genes, a general decrease in translation initiation, and a concomitant shift in the mRNAs that are translated.
The recent discovery of the mechanisms of ER stress signaling, coupled with the ability to genetically engineer model organisms, has led to major new insights into the diverse cellular and physiological processes that are regulated by the UPR. Here, I summarize current discoveries that have offered insights into the complex regulation of the UPR and its relevance to human physiology and disease.
Glucose and protein folding Early studies demonstrated that both viral transformation and glucose depletion induce transcription of a set of related genes that were termed glucose-regulated proteins (GRPs) (3). Since viral transformation increases both the cellular metabolic rate and ATP utilization, it became evident that, in both cases, this signal emanates from the ER as a consequence of energy deprivation. Because proteins have different ATP requirements for protein folding prior to export, it has been proposed that the threshold for UPR activation might differ among various cell types, depending on their energy stores and the amount and nature of the secretory proteins they produce (4). Glucose not only provides the metabolic energy needed by cells but also participates directly in glycoprotein folding as a component of oligosaccharide structures.
The recognition and modification of oligosaccharide structures in the lumen of the ER is intimately coupled to polypeptide folding (5). As the growing nascent chain is translocated into the lumen of the ER, a 14-oligosaccharide core (GlcNAc2Man9Glc3) is added to consensus asparagine residues. Immediately after the addition of this core, the three terminal glucose residues are cleaved by the sequential action of glucosidases I and II to yield a GlcNAc2Man9 structure. If the polypeptide is not folded properly, a UDP-glucose:glycoprotein glucosyltransferase (UGGT) recognizes the unfolded nature of the glycoprotein and reglucosylates the core structure to re-establish the glucose-α(1, 3)–mannose glycosidic linkage. Monoglucosylated oligosaccharides containing this bond bind to the ER-resident protein chaperones calnexin and calreticulin.
This quality control process ensures that unfolded glycoproteins do not exit the ER. Treatment of cells with castanospermine, a transition-state analogue inhibitor of glucosidases I and II, inhibits this monoglucosylation cycle, prevents interaction of unfolded glycoproteins with calnexin and calreticulin, and activates the UPR. Genetic alterations that reduce the nucleotide sugar precursor pool or glycosyltransferase reactions likewise activate the UPR (6). Therefore, the recognition of altered carbohydrate structures is in some manner linked to UPR activation.
The UPR in yeast and higher eukaryotes On a cellular level, the accumulation of unfolded proteins in the ER lumen induces the transcription of a large set of genes whose products increase the ER’s volume or its capacity for protein folding or promote the degradation of misfolded proteins through the process of ER-associated protein degradation (ERAD) (7). For example, transcription of the ER protein chaperone BiP is a classical marker for UPR activation in yeast and mammalian cells (8). BiP binds hydrophobic exposed patches on the surfaces of unfolded proteins and interactive sites on unassembled protein subunits, and it releases its polypeptide substrates upon ATP binding.
In parallel, as Ron (this Perspective series, ref. 2) details in his accompanying article, translation is attenuated to decrease the protein-folding load. The complex network of physiological responses to ER stress is regulated by only a few ER transmembrane proteins: IRE1, PERK, and ATF6 (9). IRE1, PERK, and ATF6 are proximal sensors that regulate the production and/or quality of basic leucine zipper–containing (bZIP-containing) transcription factors that may form homo- and heterodimers. Combinatorial interactions of these factors generate diversity in responses for different subsets of UPRresponsive genes. In multicellular organisms, if these adaptive responses are not sufficient to relieve ER stress, the cell dies through apoptosis or necrosis.
IRE1-dependent splicing The UPR-signaling pathway was first described less than ten years ago in the budding yeast Saccharomyces cerevisiae. Elegant studies identified IRE1 as the sensor of unfolded proteins in the ER lumen. IRE1 is a type 1 transmembrane Ser/Thr protein kinase that also has a site-specific endoribonuclease (RNase) activity. The presence of unfolded proteins in the ER lumen promotes dimerization and trans-autophosphorylation, rendering IRE1 active as an RNase, and allowing it to cleave a 252-base intron from the mRNA encoding the transcription factor HAC1 (10). The 5′ and 3′ ends of HAC1 mRNA are spliced together by tRNA ligase in a process that is independent of the spliceosome and the usual intranuclear machinery for mRNA splicing. Splicing of HAC1 mRNA increases its translational efficiency and alters sequence of the encoded HAC1 protein, yielding a potent transcriptional activator (11) that can bind and activate the UPR elements (UPREs) upstream of many UPR-inducible genes. In S. cerevisiae, the UPR activates transcription of approximately 381 genes (7).
All eukaryotic cells appear to have maintained the essential and unique properties of the UPR present in S. cerevisiae, but higher eukaryotes possess additional sensors that generate diverse, coordinately regulated responses that promote stress adaptation or cell death. The mammalian genome contains two homologues of yeast IRE1 — IRE1α and IRE1β. Whereas IRE1α is expressed in most cells and tissues, with high-level expression in the pancreas and placenta (12), IRE1β expression is prominent only in intestinal epithelial cells (13). Both IRE1 molecules respond to the accumulation of unfolded proteins in the ER, which activate their kinase and, thereby, their RNase activities. The cleavage specificities of IRE1α and IRE1β are similar, if not identical, suggesting that they do not recognize different sets of substrates but rather generate temporally specific and tissue-specific expression (14, 15).
Searching for transcription factors that mediate the UPR, Yoshida et al. defined a mammalian ER stress response element [ERSEI; CCAAT(N9)CCACG] that is necessary and sufficient for UPR gene activation. Using a yeast one-hybrid screen, these authors isolated XBP1, a bZIP transcription factor X-box DNA binding protein (16). Subsequently, several groups demonstrated that XBP1 mRNA is a substrate for mammalian IRE1, much as the HAC1 mRNA in S. cerevisiae is processed by the yeast IRE1; this pathway is also conserved in Caenorhabditis elegans (17–20). On activation of the UPR, XBP1 mRNA is cleaved by IRE1 to remove a 26-nucleotide intron and generate a translational frameshift. As expected given the precedent of HAC1 regulation in yeast, the resulting processed mRNA encodes a protein with a novel carboxy-terminus that acts as a potent transcriptional activator.
Overexpression of either IRE1α or IRE1β is sufficient to activate transcription from a BiP promoter reporter construct (15). Analysis of a minimal UPRE motif (TGACGTGC/A) (21) uncovered a transcriptional defect in IRE1α-null mouse embryo fibroblasts that could be complemented by expression of spliced XBP1 mRNA (20), and Yoshida et al. (unpublished data) recently identified a UPR-inducible gene that uniquely requires IRE1α-mediated splicing of XBP1 mRNA. However, neither IRE1α nor IRE1β is necessary for transcriptional activation of the BiP gene, as judged by the phenotype of IRE1α/β–deleted murine cells (20, 22, 23). These results indicate that a subset of UPR targets require IRE1 but that at least one IRE1-independent pathway exists for UPR-mediated transcriptional induction. Deletion of IRE1α causes embryonic lethality at embryonic day 10.5 (E10.5) (20, 22, 23). Therefore, although IRE1α is not required for the UPR, it is clearly required for mammalian embryogenesis. XBP1 deletion also causes embryonic lethality, but the mutant embryos can survive up to day E14.5, consistent with the notion that XBP1 acts downstream of IRE1α. XBP1 deletion causes cardiomyopathy and liver hypoplasia (24, 25). In contrast, IRE1β-null mice develop normally but exhibit increased susceptibility to experimentally induced colitis, a phenotype that is consistent with the specific expression of this kinase in the intestinal epithelium (26).
Activation of ATF6 and PERK by ER stress The activating transcription factor ATF6 (16) has been identified as another regulatory protein that, like XBP1, can bind ERSEI elements in the promoters of UPRresponsive genes. There are two forms of ATF6, both synthesized as ER transmembrane proteins. ATF6α (90 kDa) and ATF6β (110 kDa, also known as CREB-RP) both require the presence of the transcription factor CBF (also called NF-Y) to bind ERSEI (27–30).
On activation of the UPR, both forms of ATF6 are processed to generate 50- to 60-kDa cytosolic, bZIP containing transcription factors that migrate to the nucleus (27). Processing of ATF6 by site-1 protease (S1P) and site-2 protease (S2P) occurs within the transmembrane segment and at an adjacent site exposed to the ER lumen. S1P and S2P are the processing enzymes that cleave the ER-associated transmembrane sterolresponse element–binding protein (SREBP) upon cholesterol deprivation (31). The cytosolic fragment of cleaved SREBP migrates to the nucleus to activate transcription of genes required for sterol biosynthesis. Interestingly, although the mechanism regulating ATF6 processing is similar to that regulating SREBP processing (32), the UPR only elicits ATF6 processing, whereas sterol deprivation alone induces SREBP processing. The SREBP cleavage–activating protein (SCAP) confers specificity for SREBP transport to the Golgi compartment, and consequently cleavage in response to sterol deprivation (33). It is unknown whether another cleavage-activating protein, analogous to SCAP but active only following induction of the UPR, promotes the specific cleavage and activation of ATF6 by S1P and S2P.
Transcription of UPR-responsive genes is induced when the cleaved form of ATF6 activates the XBP1 promoter. Therefore, signaling through ATF6 and IRE1 merges to induce XBP1 transcription and mRNA splicing, respectively (Figure 1, a and b). ATF6 increases XBP1 transcription to produce more substrate for IRE1- mediated splicing that generates more active XBP1, providing a positive feedback for UPR activation. However, cells that lack either IRE1α or ATF6 cleavage can induce XBP1 mRNA (20). These two pathways may thus provide parallel signaling pathways for XBP1 transcriptional induction. Alternatively, another pathway — possibly mediated by the ER-localized protein kinase PERK (see Ron, this Perspective series, ref. 2) — may also contribute to induction of XBP1 mRNA. The binding specificities of XBP1 and ATF6 are similar, although ATF6 binding requires CBF binding to an adjacent site, whereas XBP1 binds independently (17, 20, 21, 34). These binding specificities provide another avenue for complementary interaction between the IRE1-XBP1 and ATF6 pathways at the level of transcriptional activation. In addition, these transcription factors might regulate transcription from a second ERSE (ERSEII), which also contains a CCACG motif (35).
In parallel with the activation of ATF6 processing and the consequent changes in gene transcription, the accumulation of unfolded proteins in the ER also alters cellular patterns of translation. The protein kinase PERK has been implicated in this aspect of the ER stress response (see Ron, this Perspective series, ref. 2). Activated PERK phosphorylates the α subunit of eukaryotic translation initiation factor 2 (eIF2α) and attenuates general protein synthesis. Inactivation of the PERK-eIF2α phosphorylation pathway decreases cells’ ability to survive ER stress (36, 37). The PERK pathway promotes cell survival not only by limiting the protein-folding load on the ER, but also by inducing transcription of UPR- activated genes, one-third of which require phosphorylation of eIF2α for their induction (36). Preferential translation of the transcription factor ATF4 allows for continued activation of these genes under conditions of stress, when general protein synthesis is inhibited (36, 37).
A coordinated mechanism for activation One puzzling question about the UPR is how three independent sensors are activated by a common stimulus, the accumulation of unfolded proteins in the ER lumen. BiP, which negatively regulates the UPR, interacts with all three sensors, IRE1, PERK, and ATF6, under nonstressed conditions and may indeed be the master regulator of UPR activation.
Upon accumulation of unfolded proteins in the ER, BiP is released from IRE1, PERK, and ATF6. It is believed that the unfolded proteins bind BiP and sequester it from interacting with IRE1, PERK, and ATF6 to elicit their activation. In this manner, BiP senses both the level of unfolded proteins and the energy (ATP) level in the cell in regulating the UPR. Following release from BiP, IRE1 and PERK are each free to undergo spontaneous homodimerization mediated by their lumenal domains and to become phosphorylated by their endogenous kinase activities (38, 39). BiP interaction with ATF6 prevents trafficking of ATF6 to the Golgi compartment. For this reason, BiP release permits ATF6 transport to the Golgi compartment, where it gains access to S1P and S2P proteases (32). The regulation of signaling through the free level of BiP is an attractive hypothesis providing a direct mechanism by which all three ER stress sensors could be activated by the same stimulus. In addition, the increase in BiP during the UPR would provide a negative feedback to turn off UPR signaling. However, in certain cells, different stress conditions can selectively activate only one or two of the ER stress sensors. For example, in pancreatic β cells, glucose limitation appears to activate PERK prior to activation of IRE1 (D. Scheuner and R.J. Kaufman, unpublished results). It will be important to elucidate how general BiP repression permits the selective activation of individual components of the UPR that mediate various downstream effects.

Signaling the UPR in eukaryotes
Figure 1 Signaling the UPR in eukaryotes.
http://dm5migu4zj3pb.cloudfront.net/manuscripts/16000/16886/small/JCI0216886.f1.gif
Three proximal sensors, IRE1, PERK, and ATF6, coordinately regulate the UPR through their various signaling pathways. Whereas IRE1 and PERK are dispensable for many aspects of the response, ATF6 cleavage is required for UPR transcriptional induction and appears to be the most significant of these effectors in mammalian cells. BiP negatively regulates these pathways. BiP interacts with ATF6 to prevent its transport to the Golgi compartment (a). BiP binds to the lumenal domains of IRE1 (b) and PERK (c) to prevent their dimerization. As unfolded proteins accumulate, they bind BiP and reduce the amount of BiP available to bind and inhibit activation of IRE1, PERK, and ATF6. (a) BiP release from ATF6 permits transport to the Golgi compartment. In the Golgi, ATF6 is cleaved by S1P and S2P proteases to yield a cytosolic fragment that migrates to the nucleus to activate transcription of responsive genes, including XBP1. (b) BiP release from IRE1 permits dimerization to activate its kinase and RNase activities to initiate XBP1 mRNA splicing. XBP1 splicing removes a 26-base intron, creating a translational frameshift to yield a more potent transcriptional activator. (c) BiP release permits PERK dimerization and activation to phosphorylate Ser51 on eIF2α to reduce the frequency of AUG initiation codon recognition. As eIF2α phosphorylation reduces the functional level of eIF2, the general rate of translation initiation is reduced. However, selective mRNAs, such as ATF4 mRNA, are preferentially translated under these conditions, possibly by the presence of open reading frames within the 5′ untranslated region of the mRNA. Upon recovery from the UPR, GADD34 targets PP1 to dephosphorylate eIF2α and increase protein translation.
The UPR as a mediator of programmed cell death In contrast to UPR-signaling adaptation in response to ER stress, prolonged UPR activation leads to apoptotic cell death (Figure 2). The roles of several death-promoting signaling pathways have been shown by analysis of specific gene-deleted cells. Activated IRE1 recruits c-Jun-N-terminal inhibitory kinase (JIK) and the cytosolic adaptor TRAF2 to the ER membrane (22, 40). TRAF2 activates the apoptosis-signaling kinase 1 (ASK1), a mitogen-activated protein kinase kinase kinase (MAPKKK) (41). Activated ASK1 leads to activation of the JNK protein kinase and mitochondriadependent caspase activation (40–42).
ER insults lead to caspase activation by mitochondria/APAF-1–dependent and –independent pathways. ER stress promotes cytochrome c release from mitochondria, possibly by c-ABL kinase (43) or calcium (44). However, APAF1–/– cells are susceptible to ER stress–induced apoptosis, indicating that the mitochondrial pathway is not essential (45). Caspase-12 is an ER-associated proximal effector in the caspase activation cascade, and cells lacking this enzyme are partially resistant to inducers of ER stress (46). ER stress induces TRAF2 release from procaspase 12, allowing it to bind activated IRE1. As shown in Figure 2, release of TRAF2 permits clustering of procaspase-12 at the ER membrane, leading to its activation (40). Caspase-12 can activate caspase-9, which in turn activates caspase- 3 (47). Procaspase-12 can also be activated by m-calpain in response to calcium release from the ER, although the physiological significance of this pathway is not known (48). In addition, upon ER stress, procaspase-7 is activated and recruited to the ER membrane (49). These findings support the notion that ER stress leads to several redundant pathways for caspase activation.
A second death-signaling pathway activated by ER stress is mediated by transcriptional activation of genes encoding proapoptotic functions. Activation of UPR sensor IRE1, PERK, or ATF6 leads to transcriptional activation of CHOP/GADD153, a bZIP transcription factor that potentiates apoptosis (see Ron, this Perspective series, ref. 2).
The UPR in health and disease Primary amino acid sequence contains all the information for a protein to attain its final folded conformation. However, many folding intermediates exist along the folding pathway (see Horwich, this Perspective series, ref. 1), and some of these intermediates can become irreversibly trapped in low-energy states and activate the UPR. Clearance of such misfolded species requires a functional ER-associated degradation (ERAD) pathway, which is regulated by the UPR. Proteasomal degradation of ER-associated misfolded proteins is required to protect from UPR activation. Proteasomal inhibition is sufficient to activate the UPR, and, in turn, genes encoding several components of ERAD are transcriptionally induced by the UPR (7). Therefore, it is to be expected that UPR activation and impaired ERAD function might contribute to a variety of diseases and that polymorphisms affecting the UPR and ERAD responses could modify disease progression. The following examples provide the best available evidence linking the UPR pathway to the natural history of human diseases and animal models of these diseases.
The UPR and ERAD in genetic disease Many recessive inherited genetic diseases are due to loss of-function mutations that disturb productive folding and that produce proteins that are either not secreted or not functional. In other cases, protein-folding mutations can interfere with cellular processes, resulting in a gain of function and a dominant pattern of inheritance. In several instances, UPR activation by the accumulation of unfolded proteins in the ER is known to contribute to disease progression. The distinction between these two classes of genetic disease is important, because gain-of-function protein-misfolding mutations will be less amenable to treatment by gene therapy to deliver a wild-type copy of the mutant gene.
One well-characterized protein-folding defect results from a mutation that leads to type 1 diabetes. The Akita mouse has a gain-of-function Cys96Tyr mutation in the proinsulin 2 (Ins2) gene; this mutation disrupts proinsulin folding. The mutant protein is retained in the ER of the pancreatic β cell and activates the UPR. Crucially, the progressive development of diabetes in this model is not solely due to the lack of insulin but is rather a consequence of the misfolded protein accumulation, UPR activation, and β cell death. When bred into a Chop–/–background, the Akita mutation causes a lesser degree of β cell death and delayed onset of diabetes (50), indicating that the loss of at least one downstream signaling component of the UPR can ameliorate pathogenesis in this setting.

Signaling UPR-mediated cell death
Figure 2 Signaling UPR-mediated cell death.
http://dm5migu4zj3pb.cloudfront.net/manuscripts/16000/16886/medium/JCI0216886.f2.jpg
The activation of procaspase-12 is likely the major pathway that induces apoptosis in response to ER stress. Upon activation of the UPR, c-Jun-N-terminal inhibitory kinase (JIK) release from procaspase-12 permits clustering and activation of procaspase-12. Caspase-12 activates procaspase-9 to activate procaspase-3, the executioner of cell death. In addition, activated IRE1 binds JIK and recruits TRAF2, which signals through apoptosis-signaling kinase 1 (ASK1) and JNK to promote mitochondria-dependent apoptosis. In addition, in vitro studies suggest that localized calcium release from the ER activates m-calpain to cleave and activate procaspase-12. Upon UPR activation, procaspase-7 is activated and recruited to the ER membrane. Finally, IRE1, PERK, and ATF6 induce transcription of several genes encoding apoptotic functions, including CHOP/GADD153. CSP, caspase; pCSP, procaspase.
Deficiency in α1-proteinase inhibitor (α1-PI, also known as α1-antitrypsin) results in emphysema and destructive lung disease in one out of 1,800 births. However, a subgroup of affected individuals develop chronic liver disease and hepatocellular carcinoma as a consequence of a secretion defect in the misfolded protein at the site of synthesis, the hepatocyte. This is the most common genetic cause of liver disease in children. The Z allele of the α1 gene PI (Glu342Lys mutation) produces a protein that polymerizes and is retained in the ER for degradation by the proteasome (see Lomas and Mahadeva, this Perspective series, ref. 51; and Perlmutter, this series, ref. 52). While α1-PI Z neither binds BiP nor activates the UPR, analysis of fibroblasts obtained from these patients demonstrates that individuals susceptible to liver disease have inherited a second trait that slows degradation of the misfolded protein in the ER (53), consistent with the idea that polymorphisms that reduce ERAD function can exacerbate pathogenesis of certain diseases.
There are numerous additional genetic misfolding diseases that are also likely influenced by UPR signaling. Because BiP release from IRE1, PERK, or ATF6 can activate the UPR, the expression of any wild-type or mutant protein that binds BiP can have a similar effect. In contrast, misfolded proteins that do not bind BiP are unlikely to activate the UPR. For example, cystic fibrosis is due to mutations in the cystic fibrosis transmembrane conductance regulator (CFTR) protein. Approximately 70% of patients with this disease carry a common mutation, deletion of Phe508, that results in a molecule that is retained in the ER and eventually degraded by the proteosome (see Gelman and Kopito, this Perspective series, ref. 54). Although expression of ∆508 CFTR does not activate the UPR in cultured cells, the protein does interact with calnexin, as well as HSP70, and requires ERAD function for cell survival.
Osteogenesis imperfecta (OI) results from misfolding mutations in procollagen that produce molecules that bind BiP and activate the UPR (55). Interestingly, Wolcott-Rallison syndrome is due to inactivating mutations in the PERK gene. Affected individuals, as well as mice with deletions in Perk, display osteoporosis and deficient mineralization throughout the skeletal system (56, 57), the same defects that are observed in OI. Procollagen type I accumulates to high levels and mature collagen is not detected in bone and osteoblasts from PERKnull mice. Osteoblasts from PERK-null humans and mice display fragmented and distended ER that is filled with electron-dense material (56, 57). These observations suggest that procollagen type 1 uniquely requires PERK function to maintain its transport out of the ER, processing, and secretion In this case, PERK may be required to limit procollagen synthesis so that it does not saturate the ER protein-folding capacity.
The UPR and ERAD in conformational diseases Diseases caused by expansion of polyglutamine repeats and neurodegenerative diseases, such as Alzheimer disease and Parkinson disease, represent a large class of conformational diseases associated with accumulation of abnormal protein aggregates in and around affected neurons. Recent evidence indicates that the pathogenesis of these diseases is due to a defect in proteasomal function that results in UPR activation, leading to cell death. The protein aggregates in these diseases are localized to the nucleus or the cytoplasm and would not be predicted to disturb ER function directly. Nevertheless, they have been found in some cases to activate the UPR and to promote cell death. Analysis of the polyglutamine repeat associated with the spinocerebrocellular atrophy protein (SCA3) in Machado-Joseph disease suggests that cytoplasmic accumulation of the SCA3 aggregate can inhibit proteasome function, thereby interfering with ERAD to induce the UPR and elicit caspase-12 activation (41, 58). These findings support the idea that the UPR can signal the accumulation of unfolded proteins in the cytosol via proteasomal inhibition and disruption of ERAD function.
Parkinson disease is the most common movement disorder, affecting about 1% of individuals 65 years of age or older. Autosomal recessive juvenile parkinsonism (AR-JP) results from defects in the Parkin gene (59), which encodes a ubiquitin protein ligase (E3) that functions with ubiquitin-conjugating enzyme UbcH7 or UbcH8 to tag proteins for degradation. Overexpression of Parkin suppresses cell death associated with ER stress (60). Inherited Parkinson disease is associated with the accumulation in the ER of dopaminergic neurons of PAEL-R, a putative transmembrane receptor protein that is detected in an insoluble form in the brains of AR-JP patients (61). The accumulation of PAEL-R results from defective Parkin that does not maintain the proteasome-degrading activity necessary to maintain ER function (62). Other, still-unidentified substrates of the Parkin E3 ligase may also be relevant to the pathogenesis of AR-JP.
The UPR in diabetes The metabolism of glucose is tightly controlled at the levels of synthesis and utilization through hormonal regulation. The most dramatic phenotype in Wolcott-Rallison syndrome is pancreatic β cell death with infancy onset diabetes (56). A similar defect is observed in PERK-null mice; this defect also correlated with increased apoptosis of β cells (57, 63). In addition, mice with a homozygous Ser51Ala mutation at the PERK phosphorylation site in eIF2α display an even greater β cell loss that appears in utero (36). Therefore, translational control through PERK-mediated phosphorylation of eIF2α is required to maintain β cell survival (see Ron, this Perspective series, ref. 2). The more severe β cell loss in mice harboring the Ser51Ala eIF2α mutation suggests that additional eIF2α kinases partially complement the requirement for PERK in β cell function (36)
Glucose not only promotes the secretion of insulin but also stimulates insulin transcription and translation (64–66). Our group has proposed that glucose stimulated proinsulin mRNA translation is regulated by PERK-mediated phosphorylation of eIF2α in response to UPR activation 36). As blood glucose declines, energy may become limiting for protein folding in the ER and therefore activate the UPR to promote PERK-mediated phosphorylation of eIF2α. Conversely, a rise in blood glucose would turn off the UPR so that translation would accelerate, allowing entry of new preproinsulin into the ER. In this manner, PERK mediated phosphorylation of eIF2α provides a brake on protein synthesis, including proinsulin translation. Continual elevation of blood glucose may also prolong elevated proinsulin translation, eventually activating the UPR as the secretion capacity of the ER is overwhelmed. Therefore, a delicate balance between glucose levels and eIF2α phosphorylation needs to be maintained: Disturbances in either direction may lead to excessive UPR activation, with eventual β cell death.
The insulin resistance and hyperglycemia associated with type 2 diabetes is accommodated by an increase in proinsulin translation. Under these conditions the UPR is activated to compensate for the increased protein-folding requirement in the ER. Prolonged activation of the UPR could contribute to the β cell death associated with insulin resistance. Thus, the signaling mechanisms that β cells use for sensing glucose levels, triggering insulin secretion, and rapidly controlling insulin biosynthesis may have coevolved with ER signaling pathways to support these specialized functions. Pancreatic β cells are exquisitely sensitive to physiological fluctuations in blood glucose, because, in contrast to other cell types, they lack hexokinase, an enzyme with a low affinity but a high capacity for binding glucose. Therefore, in β cells, the production of glucose 6-phosphate and the production of ATP through glycolysis are controlled by glucokinase (67), and the ratio of ATP to ADP correlates directly with the blood glucose level. Periodic decreases in blood glucose level (as occurs between meals) would decrease the ATP/ADP ratio and compromise protein folding in the ER so that the UPR may be frequently activated in these cells. Hence, when glucose levels vary within the normal physiological range, the ER compartment of the β cell may be exposed to greater energy fluctuations than is the ER of other cell types, making the β cell uniquely dependent on the UPR for survival during intermittent decreases in blood glucose levels, as happens between meals. Additionally, the high-level expression of PERK and IRE1α in the pancreas may predispose these kinases to dimerization and activation in response to intermittent stress.
The UPR in organelle expansion The UPR is required for ER expansion that occurs upon differentiation of highly specialized secretory cells, but ER membrane expansion can also proceed independently of UPR activation. Overexpression of membrane proteins, such as HMG CoA reductase or the peroxisomal protein Pex15, promotes the expansion of smooth membranes without UPR activation (68, 69), as does overexpression of the p180 ribosome acceptor in the rough ER membrane (70). Conversely, protein overexpression, even under circumstances in which secretory capacity is unchanged (as occurs following the induction of high levels of cytochrome p450), can activate the UPR to induce ER chaperone levels to match the expanded membrane area (71, 72).
During the terminal differentiation of certain secretory cells, such as those in the pancreas or liver, membrane expansion is accompanied by a dramatic increase in protein secretion. Likewise, upon B cell maturation into high-level antibody-secreting plasma cells, the ER compartment expands approximately fivefold to accommodate the large increase in Ig synthesis. The requirement for the UPR in this latter process has been demonstrated in XBP1–/– cells. Since deletion of XBP1 produces an embryonic-lethal phenotype at day E14.5, the role of XBP1 in B and T cell development had to be studied in immunoincompetent RAG1–/– mice reconstituted with XBP1–/– embryonic stem cells (73). Work in these chimeric mice demonstrated that XBP1 is required for high-level Ig production. Interestingly, the induction of Ig heavy-chain and light-chain gene rearrangement and the assembly and transport of Igµ to the surface of the B cells occurred normally. However, plasma cells were not detected, suggesting a role for XBP1 in plasma cell differentiation or survival.
These findings support the hypothesis that induction of Ig synthesis activates the UPR to induce ER expansion to accommodate the high-level antibody expression. Alternatively, activation of the UPR may be part of the differentiation program that occurs prior to induction of high-level antibody synthesis. Plasma cell differentiation is stimulated in vivo by treatment with LPS or by ligation of CD40 receptors, treatments that activate the innate immune response and have been shown to induce XBP1 mRNA splicing (19). Thus, the UPR may contribute to a programmed response to signals that increase a cell’s protein-secretory demand.
The UPR in hyperhomocysteinemia. The association between high levels of serum homocysteine and the development of ischemic heart disease and stroke is supported by substantial epidemiological data. Unfortunately, it is not known whether homocysteine is the underlying cause of atherosclerosis and thrombosis. Severe hyperhomocysteinemia is caused by mutation in the cystathionine β-synthase (CBS) gene, whose product is a vitamin B6–dependent enzyme required for the conversion of homocysteine to cysteine. Elevated homocysteine is also associated with vitamin B deficiency. In cultured vascular endothelial cells, homocysteine induces protein misfolding in the ER by interfering with disulfide bond formation, and it activates the UPR to induce expression of several ER stress response proteins, such as BiP, GRP94, CHOP, and HERP (74–76). Homocysteine also activates apoptosis in a manner that requires an intact IRE1-signaling pathway (76).
These findings suggest that homocysteine acts intracellularly to disrupt ER homoeostasis. Indeed, recent studies confirm that induction of hyperhomocysteinemia elicits UPR activation in the livers of normal or Cbs+/– mice (77). In addition, hyperhomocysteinemia activates SREBP cleavage, leading to intracellular accumulation of cholesterol (77). Increased cholesterol biosynthesis may explain the hepatic steatosis and possibly the atherosclerotic lesions associated with hyperhomocysteinemia. Finally, hyperhomocysteinemia accelerates atherosclerosis in ApoE–/– mice (78, 79), although the molecular mechanisms remain to be elucidated.
Hyperhomocysteinemia is also associated with increased amyloid production and increased amyloid-mediated neuronal death in animal models of Alzheimer disease (80). These observations suggest that the UPR may link the disease etiologies of hyperhomocysteinemia and Alzheimer disease. HERP, a homocysteine-induced ER stress–responsive gene, appears to be involved in amyloid β-protein (Aβ) accumulation, including the formation of senile plaques and vascular Aβ deposits (81), and that it interacts with both presenilin-1 (PS1) and presenilin-2 (PS2), thus regulating presenilin-mediated Aβ generation. Immunohistochemical analysis of brains from patients with Alzheimer disease reveals intense HERP staining in activated microglia in senile plaques.
The UPR in cancer Hypoxia is a common feature of solid tumors that display increased malignancy, resistance to therapy, and poor prognosis. Hypoxia in the tumor results from increased demand due to dysregulated cell growth and from vascular abnormalities associated with cancerous tissue. The importance of hypoxia has been seen in the clinic, since it predicts for poor outcome of treatments, independent of treatment modality. Hypoxia activates the UPR, whose downstream signaling events can undermine the efficacy of treatment. Tumor cells need to adapt to the increasingly hypoxic environment that surrounds them as they grow, and the induction of the UPR is key to this response. Induction of the ER stress response genes, for example BiP and GRP94, in cancerous tissue correlates with malignancy, consistent with their antiapoptotic function (82). In addition, the UPR confers resistance to topoisomerase inhibitors, such as etoposide, and some UPR-induced genes directly mediate drug resistance via the multi-drug-resistance gene MDR. Therefore, approaches to prevent UPR activation in cancerous cells may significantly improve treatment outcome.
The proteasome inhibitor PS-341 is now in earlyphase clinical evaluation for the treatment of multiple myeloma, a clonal B cell tumor of differentiated plasma cells (83). The mechanism of PS-341 function is thought to be inhibition of IκB degradation, which prevents activation of the antiapoptotic transcription factor NF-κB. However, proteasomal inhibition would also prevent ERAD. As high-level heavy- or light-chain Ig production is likely associated with a certain degree of protein misfolding, it is possible that inhibition of ERAD function may be selectively toxic to B cell myelomas through activation of the UPR and apoptosis.
The UPR and viral pathogenesis The two major mediators of the IFN-induced arm of the innate immune response are evolutionarily related to IRE1 and PERK. The kinase/endoribonuclease domain of IRE1 is homologous to RNaseL, and the protein kinase domain of PERK is related to the double-stranded RNA–activated (dsRNA-activated) eIF2α protein kinase PKR. RNase L and PKR mediate the IFN induced antiviral response of the host, which is required to limit viral protein synthesis and pathogenesis. As part of the innate immune response to viral infection, RNase L and PKR are activated by dsRNAs produced as intermediates in viral replication. In contrast to activation by dsRNA, IRE1 and PERK are activated by ER stress, which can be induced by high-level viral glycoprotein expression. All enveloped viruses produce excess glycoproteins that could elicit PERK and IRE1 activation to meet the need for increased folding and secretory capacity. More studies will be required to elucidate the role of the UPR in various viral diseases.
Hepatitis C virus (HCV) is a positive-stranded RNA virus encoding a single polyprotein. Polyprotein cleavage generates at least ten polypeptides, including two glycoproteins, E1 and E2. A large amount of E1 forms disulfide–cross-linked aggregates with E2 in the ER (84). Since the accumulation of misfolded α1-PI elicits UPR activation, with subsequent hepatocyte death and hepatocellular carcinoma, it is possible that the aggregated E1/E2 complexes in the HCV-infected hepatocyte also contribute to hepatitis and hepatocellular carcinoma. Future studies should identify whether these glycoprotein aggregates activate the UPR to mediate the hepatocyte cell death and transformation associated with the pathogenesis of HCV infection.
The UPR in tissue ischemia Finally, neuronal death due to reperfusion after ischemic injury is associated with activation of the UPR (85, 86). Immediately after reperfusion, protein synthesis is inhibited, due at least in part to phosphorylation of eIF2α; this inhibition may represent a protective mechanism to prevent further neuron damage. Recent studies support the idea that eIF2α phosphorylation in response to reperfusion injury is mediated by PERK and hence that it depends on the UPR (87). If so, UPR activation prior to ischemic injury might protect the brain and other tissues from cell death during periods of reperfusion.
Summary A variety of approaches have been employed to identify the UPR signaling components, their function, and their physiological role. Yeast genetics allowed the definition of the basic ER stress–signaling pathway. The identification of homologous and parallel signaling pathways in higher eukaryotes has produced a mechanistic framework the cell uses to sense and compensate for ER over-load and stress. The high-level tissue-specific expression patterns of several ER stress–signaling molecules indicated the pancreas and intestine as organs that require UPR for physiological function. Analysis of UPR-induced gene expression established that protein degradation is required to reduce the stress of unfolded protein accumulation in the ER. Major advances in identifying UPR function and rele vance to disease were derived from mutation of UPR signaling components in model organisms and the identification of mutations in humans.
Despite tremendous progress, our knowledge of the UPR pathway remains incomplete. Further studies promise to expand our understanding of how ER stress impacts the other cellular signaling pathways. It will be very exciting and informative to understand how the UPR varies when critical components are genetically manipulated by deletion or other types of mutations. In addition, although the accumulation of unfolded protein in the ER is now known to contribute to pathogenesis in a variety of diseases, there are still few therapeutic approaches that target these events. With a greater understanding of protein-folding processes, pharmacological intervention with chemical chaperones to promote proper folding becomes feasible, as observed with sodium phenylbutyrate for ∆508 CFTR (see Gelman and Kopito, this Perspective series, ref. 53). Future intervention should consider activation of different subpathways of the UPR or overexpression of appropriate protein chaperones, as in the case of overexpression of the J domain of cytosolic HSP70, which suppresses polyglutamine toxicity in flies (88). Treatments that activate the ERAD response may also ameliorate pathogenesis in a number of the conformational diseases.
Over the past ten years, tremendous progress has been made in understanding the mechanisms and physiological significance of the UPR. The processes of protein folding and secretion, transcriptional and translational activation, and protein degradation are intimately interconnected to maintain homeostasis in the ER. A variety of environmental insults, genetic disease, and underlying genetic modifiers of UPR function contribute to the pathogenesis of different disease states. As we gain a greater understanding of the mechanisms that control UPR activation, it should be possible to discover methods to activate or inhibit the UPR as desired for therapeutic benefit.
- Horwich, A. 2002. Protein aggregation in disease: a role for folding intermediates forming specific multimeric interactions. J. Clin. Invest. 110:1221–1232. doi:10.1172/JCI200216781.
- Ron, D. 2002. Translational control in the endoplasmic reticulum stress response. J. Clin. Invest. 110:1383–1388. doi:10.1172/JCI200216784.
- Lee, A.S. 1992. Mammalian stress response: induction of the glucose-regulated protein family. Curr. Opin. Cell Biol. 4:267–273.
- Kaufman, R.J., et al. 2002. The unfolded protein response in nutrient sensing and differentiation. Nat. Rev. Mol. Cell Biol. 3:411–421.
- Ellgaard, L., and Helenius, A. 2001. ER quality control: towards an understanding at the molecular level. Curr. Opin. Cell Biol. 13:431–437.
- Jakob, C.A., Burda, P., Te Heesen, S., Aebi, M., and Roth, J. 1998. Genetic tailoring of N-linked oligosaccharides: the role of glucose residues in glycoprotein processing of Saccharomyces cerevisiae in vivo. Glycobiology. 8:155–164.
- Travers, K.J., et al. 2000. Functional and genomic analyses reveal an essential coordination between the unfolded protein response and ER-associated degradation. Cell. 101:249–258.
……
Citation: Cell Death and Disease (2014) 5, e1578; doi:10.1038/cddis.2014.539
Published online 18 December 2014
An activated unfolded protein response promotes retinal degeneration and triggers an inflammatory response in the mouse retina
http://www.nature.com/cddis/journal/v5/n12/full/cddis2014539a.html
T Rana1, V M Shinde1, C R Starr1, A A Kruglov1, E R Boitet1, P Kotla1, S Zolotukhin2, A K Gross1 and M S Gorbatyuk1
- 1Department of Vision Sciences, University of Alabama at Birmingham, AL, USA
- 2Department of Pediatrics, University of Florida, FL, USA
Correspondence: M Gorbatyuk, Department of Vision Sciences, University of Alabama at Birmingham, 1670 University Boulevard, Birmingham, 35233 AL, USA. Tel: +1 205 934 6762; Fax: +1 205 934 3425; E-mail:mgortk@uab.edu
Received 20 July 2014; Revised 23 October 2014; Accepted 27 November 2014
Edited by P Ekert
Recent studies on the endoplasmic reticulum stress have shown that the unfolded protein response (UPR) is involved in the pathogenesis of inherited retinal degeneration caused by mutant rhodopsin. However, the main question of whether UPR activation actually triggers retinal degeneration remains to be addressed. Thus, in this study, we created a mouse model for retinal degeneration caused by a persistently activated UPR to assess the physiological and morphological parameters associated with this disease state and to highlight a potential mechanism by which the UPR can promote retinal degeneration. We performed an intraocular injection in C57BL6 mice with a known unfolded protein response (UPR) inducer, tunicamycin (Tn) and examined animals by electroretinography (ERG), spectral domain optical coherence tomography (SD-OCT) and histological analyses. We detected a significant loss of photoreceptor function (over 60%) and retinal structure (35%) 30 days post treatment. Analysis of retinal protein extracts demonstrated a significant upregulation of inflammatory markers including interleukin-1β (IL-1β), IL-6, tumor necrosis factor-α (TNF-α), monocyte chemoattractant protein-1 (MCP-1) and IBA1. Similarly, we detected a strong inflammatory response in mice expressing either Ter349Glu or T17M rhodopsin (RHO). These mutant rhodopsin species induce severe retinal degeneration and T17M rhodopsin elicits UPR activation when expressed in mice. RNA and protein analysis revealed a significant upregulation of pro- and anti-inflammatory markers such as IL-1β, IL-6, p65 nuclear factor kappa B (NF-kB) and MCP-1, as well as activation of F4/80 and IBA1 microglial markers in both the retinas expressing mutant rhodopsins. We then assessed if the Tn-induced inflammatory marker IL-1β was capable of inducing retinal degeneration by injecting C57BL6 mice with a recombinant IL-1β. We observed ~19%reduction in ERG a-wave amplitudes and a 29% loss of photoreceptor cells compared with control retinas, suggesting a potential link between pro-inflammatory cytokines and retinal pathophysiological effects. Our work demonstrates that in the context of an established animal model for ocular disease, the persistent activation of the UPR could be responsible for promoting retinal degeneration via the UPR-induced pro-inflammatory cytokine IL-1β.
Abbreviations:
ERG, electroretinography; SD-OCT, spectral domain optical coherence tomography; UPR, unfolded protein response; IL-1β, Interleukin-1β; TNF-α, tumor necrosis factor-α; MCP-1, monocyte chemoattractant protein-1; NF-kB, ; nuclear factor kappa B, ; ER, endoplasmic reticulum; ADRP, autosomal dominant retinitis pigmentosa; RHO, rhodopsin; ERAI, ER stress activated indicator; Tn, tunicamycin; ONL, outer nuclear layer; H&E, hematoxylin and eosin; ONH, optic nerve head
ER stress and neuroinflammation: connecting the unfolded protein response to JAK/STAT signaling (P5196)
Gordon Meares,1 and Etty Benveniste1
1Department of Cell, Developmental and Integrative Biology, University of Alabama at Birmingham, Birmingham, AL
J Immunol May 2013 190 (Meeting Abstract Supplement) 198.5
http://www.jimmunol.org/cgi/content/meeting_abstract/190/1_MeetingAbstracts/198.5
Neuroinflammation and endoplasmic reticulum (ER) stress are associated with many neurological diseases. ER stress is brought on by misfolded proteins. In turn, cells respond with activation of the unfolded protein response (UPR). The UPR is a highly conserved pathway that transmits both adaptive and apoptotic signals to restore homeostasis or eliminate the irreparably damaged cell. Recent evidence indicates that ER stress and inflammation are linked. In this study, we have examined the interaction between ER stress and JAK/STAT-dependent inflammation in astrocytes. The JAK/STAT pathway mediates the biological actions of many cytokines and growth factors. We have found that ER stress leads to the activation of STAT3 in a JAK1-dependent fashion. ER stress-induced activation of the JAK1/STAT3 axis leads to expression of IL-6 and several chemokines. The activation of STAT3 signaling is dependent on the protein kinase PERK, a central component of the UPR. Knockdown of PERK abrogates ER stress-induced activation of STAT3 and overexpression of PERK is sufficient to activate STAT3. Additionally, ER stressed astrocytes, via paracrine signaling, can stimulate activation of microglia leading to production of oncostatin M (OSM). OSM can then synergize with ER stress in astrocytes to drive inflammation. Together, this work describes a new PERK-JAK1-STAT3 signaling pathway that may elicit a feed-forward inflammatory loop involving astrocytes and microglia to drive neuroinflammation.
Neural Plasticity
Volume 2014 (2014), Article ID 610343, 15 pages
http://dx.doi.org/10.1155/2014/610343
Review Article
Surveillance, Phagocytosis, and Inflammation: How Never-Resting Microglia Influence Adult Hippocampal Neurogenesis
Amanda Sierra,1,2,3 Sol Beccari,2,3 Irune Diaz-Aparicio,2,3 Juan M. Encinas,1,2,3 Samuel Comeau,4,5 and Marie-Ève Tremblay4,5
1Ikerbasque Foundation, 48011 Bilbao, Spain
2Achucarro Basque Center for Neuroscience, Bizkaia Science and Technology Park, 48170 Zamudio, Spain
3Department of Neurosciences, University of the Basque Country, 48940 Leioa, Spain
4Centre de Recherche du CHU de Québec, Axe Neurosciences, Canada G1P 4C7
5Département de Médecine Moléculaire, Université Laval, Canada G1V 4G2
Received 10 December 2013; Accepted 11 February 2014; Published 19 March 2014
Academic Editor: Carlos Fitzsimons
http://www.hindawi.com/journals/np/2014/610343/
Microglia cells are the major orchestrator of the brain inflammatory response. As such, they are traditionally studied in various contexts of trauma, injury, and disease, where they are well-known for regulating a wide range of physiological processes by their release of proinflammatory cytokines, reactive oxygen species, and trophic factors, among other crucial mediators. In the last few years, however, this classical view of microglia was challenged by a series of discoveries showing their active and positive contribution to normal brain functions. In light of these discoveries, surveillant microglia are now emerging as an important effector of cellular plasticity in the healthy brain, alongside astrocytes and other types of inflammatory cells. Here, we will review the roles of microglia in adult hippocampal neurogenesis and their regulation by inflammation during chronic stress, aging, and neurodegenerative diseases, with a particular emphasis on their underlying molecular mechanisms and their functional consequences for learning and memory.
- Microglia: The Resident Immune Cells of the Brain
Microglia were first described in 1919 by the Spanish neuroanatomist Pío del Río Hortega, a disciple of the renowned Santiago Ramón y Cajal, almost half a century later than neurons and astrocytes and just before oligodendrocytes [1]. This delayed appearance into the neuroscience arena is still apparent today, as microglia remain one of the least understood cell types of the brain. Traditionally, microglia were simply considered as “brain macrophages” controlling the inflammatory response during acute insults and neurodegenerative conditions, and only recently was their unique origin revealed. Indeed, microglia were shown to derive from primitive myeloid progenitors of the yolk sac that invade the central nervous system (CNS) during early embryonic development (reviewed in [2]). In contrast, circulating monocytes and lymphocytes, as well as most tissue macrophages, derive from hematopoietic stem cells located initially in the foetal liver and later in the bone marrow [3]. In the adult brain, the microglial population is maintained exclusively by self-renewal during normal physiological conditions [2]. As a consequence, microglia are the only immune cells which permanently reside in the CNS parenchyma, alongside neural tube-derived neurons, astrocytes, and oligodendrocytes.
These past few years, unprecedented insights were also provided into their extreme dynamism and functional behaviour, in health as much as in disease. Indeed, microglia were revealed to be exceptional sensors of their environment, responding on a time scale of minutes to even subtle variations of their milieu, by undergoing concerted changes in morphology and gene expression [4, 5]. During pathological insults, “activated” microglia were particularly shown to thicken and retract their processes, extend filopodia, proliferate and migrate, release factors and compounds influencing neuronal survival (such as proinflammatory cytokines, trophic factors, reactive oxygen species (ROS), etc.), and phagocytose pathogens, degenerating cells and debris, thus providing better understanding of their roles in orchestrating the inflammatory response [6]. These abilities as immune cells are also recruited during normal physiological conditions, where “surveillant” microglia further participate in the remodeling of neuronal circuits by their phagocytic elimination of synapses and their regulation of glutamatergic receptors maturation and synaptic transmission, among other previously unexpected roles [7–9], in addition to their crucial involvement in the phagocytic elimination of newborn cells in the context of adult neurogenesis [10].
Our review will discuss the emerging roles of microglia in adult hippocampal neurogenesis and their regulation by inflammation during chronic stress, aging, and neurodegenerative diseases, with a particular emphasis on their underlying molecular mechanisms and their functional consequences for learning and memory (Figure 1).
http://www.hindawi.com/journals/np/2014/floats/610343/thumbnails/610343.fig.001_th.jpg
Figure 1: The effects of surveillant and inflammatory microglia on the adult hippocampal neurogenic cascade. During physiological conditions, surveillant microglia effectively phagocytose the excess of apoptotic newborn cells and may release antineurogenic factors such as TGF. This anti-inflammatory state is maintained by neuronal (tethered or released) fractalkine. Enriched environment drives microglia towards a phenotype supportive of neurogenesis, via the production of IGF-1. In contrast, inflammatory challenge triggered by LPS, irradiation, aging, or AD induces the production of proinflammatory cytokines such as IL-1, TNF, and IL-6 by microglia as well as resident astrocytes and infiltrating monocytes, neutrophils, and lymphocytes. These cytokines have profound detrimental effects on adult neurogenesis by reducing the proliferation, survival, integration, and differentiation of the newborn neurons and decreasing their recall during learning and memory paradigms.
- A Brief Overview of Adult Hippocampal Neurogenesis
Adult hippocampal neurogenesis is continuously maintained by the proliferation of neural stem cells located in the subgranular zone (SGZ) [11–13]. These neuroprogenitors have been named “radial glia-like cells” (rNSCs), or type 1 cells, since they morphologically and functionally resemble the embryonic radial glia. They have also been defined as “quiescent neuroprogenitors” because only a small percentage of the population is actively dividing during normal physiological conditions. The lineage of these cells is frequently traced by using analogs of the nucleotide thymidine, such as bromodeoxyuridine (BrdU) which gets incorporated into the DNA of dividing cells during the S phase and can be detected by immunofluorescence. Alternatively, their lineage can be traced by labeling with fluorescent reporters which are delivered to dividing cells by retroviral vectors or expressed by specific cell type promoters via inducible transgenic mice (for a review of the methods commonly used to study adult neurogenesis, see [14]). The daughter cells of rNSCs, also called type 2 cells or amplifying neuroprogenitors (ANPs), rapidly expand their pool by proliferating before becoming postmitotic neuroblasts. Within a month, these neuroblasts differentiate and integrate as mature neurons into the hippocampal circuitry [15]. They however display unique electrophysiological characteristics during several months, being more excitable than mature neurons [16], and constitute a special cell population that is particularly inclined to undergo synaptic remodeling and activity-dependent plasticity [17].
These unique properties of the newborn neurons and the neurogenic cascade in general suggested that adult hippocampal neurogenesis could play an important role in hippocampal-dependent functions that require extensive neuroplasticity such as learning and memory. Indeed, activity-dependent plasticity and learning are long known for modulating adult neurogenesis in a complex, yet specific manner, with adult hippocampal neurogenesis being influenced by learning tasks which depend on the hippocampus [44, 45]. For instance, hippocampal-dependent learning paradigms were found to regulate the survival of newborn neurons, in a positive manner that depends on the timing between their birth and the phases of learning [46, 47]. Young (1.5–2 months old) newborn neurons were also shown to be preferentially activated during memory recall in a water maze task, compared to mature neurons, as determined by colabeling of BrdU with immediate early genes such as c-Fos and Arc, in which expression correlates with neuronal firing [48]. Nonetheless, it has only been in the last few years that loss-of-function and gain-of-function approaches with inducible transgenic mice were able to confirm that adult hippocampal neurogenesis is necessary for synaptic transmission and plasticity, including the induction of long-term potentiation (LTP) and long-term depression [49], as well as trace learning in conditioned protocols [50], memory retention in spatial learning tasks [51, 52], and encoding of overlapping input patterns, that is, pattern separation [53].
Adult hippocampal neurogenesis and its functional implications for learning and memory are however influenced negatively by a variety of conditions that are commonly associated with microglial activation and inflammation in the brain, such as chronic stress, aging, and neurodegenerative diseases, as we will review herein. Indeed, inflammation caused by irradiation produces a sustained inhibition of neurogenesis, notably by decreasing the proliferation and neuronal differentiation of the progenitors, and therefore, exposure to therapeutic doses of cranial irradiation has been widely used for modulating neurogenesis experimentally before the development of more specific approaches [54].
- Regulation of Adult Hippocampal Neurogenesis by Inflammation
Inflammation is a natural bodily response to damage or infection that is generally mediated by proinflammatory cytokines such as interleukin 1 beta (IL-1), interleukin 6 (IL-6), and tumour necrosis factor alpha (TNF), in addition to lipidic mediators such as prostaglandins and leukotrienes. Oftentimes, it is associated with an increased production of ROS, as well as nitric oxide (NO). Together, these proinflammatory mediators lead to an increase in local blood flow, adhesion, and extravasation of circulating monocytes, neutrophils, and lymphocytes [55]. In the brain, microglia are the main orchestrator of the neuroinflammatory response, but other resident cell types, including astrocytes, endothelial cells, mast cells, perivascular and meningeal macrophages, and even neurons, can produce proinflammatory mediators, though perhaps not to the same extent as microglia [56]. In addition, peripheral immune cells invading the CNS during inflammation can further produce proinflammatory mediators, but the respective contribution of microglia versus other cell types in the inflammatory response of the brain is poorly understood.
The harmful effects of inflammation are also widely determined by the actual levels of proinflammatory mediators released, rather than the occurrence or absence of an inflammatory response in itself. For instance, TNF regulates synaptic plasticity by potentiating the cell surface expression of AMPA glutamatergic receptors, thus resulting in a homeostatic scaling following prolonged blockage of neuronal activity during visual system development [57]. However, TNF also produces differential effects at higher concentrations,ranging from an inhibition of long-term potentiation to an enhancement of glutamate-mediated excitotoxicityin vitro [58]. Inflammation induced by chronic ventricular infusion of bacterial lipopolysaccharides (LPS; a main component of the outer membrane of Gram-negative bacteria), that is, the most widely used method for inducing an inflammatory challenge, also increases ex vivo the hippocampal levels of TNF and IL-1, thereby impairing novel place recognition, spatial learning, and memory formation, but all these cognitive deficits can be restored by pharmacological treatment with a TNF protein synthesis inhibitor, a novel analog of thalidomide, 3,6′-dithiothalidomide [59].
The impact of inflammation on adult hippocampal neurogenesis was originally discovered by Olle Lindvall and Theo Palmer’s groups in 2003, showing that systemic or intrahippocampal administration of LPS reduces the formation of newborn neurons in the adult hippocampus, an effect that is prevented by indomethacin, a nonsteroidal anti-inflammatory drug (NSAID) which inhibits the synthesis of proinflammatory prostaglandins [60, 61]. Similarly, inflammation can determine the increase in neurogenesis that is driven by seizures, a context in which neurogenesis can be prevented by LPS and increased by the anti-inflammatory antibiotic minocycline [60]. In these studies, hippocampal proliferation remained unaffected by LPS or minocycline and thus it is likely that inflammation targeted the survival of newborn cells [60, 61], as LPS is known to increase SGZ apoptosis [62]. Inflammation also has further downstream effects on the neurogenic cascade. For instance, LPS increases the number of thin dendritic spines and the expression of the excitatory synapses marker “postsynaptic density protein of 95kDa” (PSD95) in newborn neurons. LPS in addition increases the expression of GABAA receptors at early stages of synapse formation, leading to suggesting a possible imbalance of excitatory and inhibitory neurotransmission in these young neurons [63]. Finally, LPS also prevents the integration of newborn neurons into behaviourally relevant networks, including most notably their activation during spatial exploration, as determined by the percentage of BrdU cells colabeled with the immediate early gene Arc [64].
Importantly, none of these manipulations is specific to microglia and may directly or indirectly affect other brain cells involved in the inflammatory response of the brain. For instance, both LPS and minocycline affect astrocytic function in vitro and in vivo [65–69]. Furthermore, LPS is known to drive infiltration of monocytes and neutrophils into the brain parenchyma [70]. Monocytes and neutrophils produce major proinflammatory mediators and could therefore act on the neurogenic cascade as well. The implication of microglia in LPS-induced decrease in neurogenesis is nonetheless supported in vivo by the negative correlation between the number of newborn neurons (BrdU+, NeuN+ cells) and the number of “activated” microglia (i.e., expressing ED1) [60]. ED1, also called CD68 or macrosialin, is a lysosomal protein which is overexpressed during inflammatory challenge. While the location of ED1 previously suggested its involvement in phagocytosis, its loss of function did not result in phagocytosis deficits and thus, its function still remains unknown (reviewed in [10]). The number of ED1-positive microglia also negatively correlates with neurogenesis during inflammation provoked by cranial irradiation [61]. While correlation does not involve causation, nor can pinpoint to the underlying mechanism, these experiments were the first to reveal a potential role for “activated” microglia in the regulation of adult hippocampal neurogenesis. More direct evidence of microglial mediation in LPS deleterious effects was obtained from in vitro experiments, as it was shown that conditioned media from LPS-challenged microglia contained IL-6, which in turn caused apoptosis of neuroblasts [61]. Nonetheless, astrocytes can also release IL-6 when stimulated with TNF or IL-1 [71] and chronic astrocytic release of IL-6 in transgenic mice reduced proliferation, survival, and differentiation of newborn cells, thus resulting in a net decrease in neurogenesis [72]. In summary, while the detrimental impact of inflammation on neurogenesis is well established, more work is needed to define the specific roles played by the various inflammatory cells populating the brain.
- Inflammation Associated with Chronic Stress
Across health and disease, the most prevalent condition that is associated with neuroinflammation is “chronic stress,” which commonly refers to the repeated or sustained inability to cope with stressful environmental, social, and psychological constraints. Chronic stress is characterized by an imbalanced secretion of glucocorticoids by the hypothalamic-pituitary-adrenal (HPA) axis (most notably cortisol in humans and corticosterone in rodents), which leads to an altered brain remodeling, massive loss of synapses, and compromised cognitive function [73]. In particular, an impairment of spatial learning, working memory, novelty seeking, and decision making has been associated with chronic stress [74]. Glucocorticoids are well known for their anti-inflammatory properties, as they interfere with NF-B-mediated cytokine transcription, ultimately delaying wound healing [75]. They are also potent anti-inflammatory mediators in vivo [76] and in purified microglia cultures [77]. Recently, repeated administration of high doses of glucocorticoids by intraperitoneal injection, to mimic their release by chronic stress, was also shown to induce a loss of dendritic spines in the motor cortex, while impairing learning of a motor task. A transcription-dependent pathway acting downstream of the glucocorticoid receptor GR was proposed [78, 79] but the particular cell types involved were not identified.
Microglia are considered to be a direct target of the glucocorticoids, as they were shown to express GR during normal physiological conditions in vivo [77]. In fact, transgenic mice lacking GR in microglia and macrophages show an increased production of proinflammatory mediators (including TNF and IL-1) and greater neuronal damage in response to an intraparenchymal injection of LPS, compared to wild-type mice [80]. In contrast, glucocorticoids are considered to be proinflammatory in the chronically stressed brain [81], where among other changes they can promote inflammation, oxidative stress, neurodegeneration, and microglial activation [82]. For example, repeated restraint stress induces microglial proliferation and morphological changes, including a hyperramification of their processes in the adult hippocampus following restraint stress [83], but a nearly complete loss of processes in the context of social defeat [84]. Prenatal restraint stress also causes an increase in the basal levels of TNF and IL-1, while increasing the proportion of microglia showing a reactive morphology in the adult hippocampus [85]. Similarly, social defeat leads to an enhanced response to the inflammatory challenge induced by intraperitoneal injection of LPS, including an increased production of TNF and IL-1, and expression of inducible NO synthase (iNOS) by microglia, accompanied by an increased infiltration of circulating monocytes [84, 86]. Therefore, microglia are a strong candidate for mediating some of the effects of stress on adult neurogenesis, as will be discussed below, in synergy with other types of inflammatory cells.
Chronic stress is well known for its negative effects on hippocampal neurogenesis (reviewed in [87, 88]), although not all stress paradigms are equally effective [89]. Several stress paradigms can decrease neuroprogenitors proliferation in the tree shrew [90] and in mice [91, 92], although this effect seems to be compensated by an increased survival of newborn neurons [92] and whether stress results in a net increase or decrease in neurogenesis remains controversial (reviewed in [87, 88]). The effects of stress on adult neurogenesis seem to be mediated at least partially by glucocorticoids, because mice lacking a single copy of the GR gene show behavioural symptoms of depression including learned helplessness, neuroendocrine alterations of the HPA axis, and impaired neurogenesis [93]. In parallel, chronic stress is associated with an increased inflammatory response, which may inhibit neurogenesis as well. For instance, serum levels of IL-1and IL-6 are significantly increased in depressed patients [94]. In mice, restraint stress leads to a widespread activation of NF-B in the hippocampus, including at the level of neuroprogenitors [95] and increased protein levels of IL-1 [96]. In addition to the direct role of glucocorticoids, IL-1 also seems to mediate some of the effects of mild chronic stress, because in vivo manipulations that block IL-1 (either pharmacologically or in null transgenic mice) prevent the anhedonic stress response and the antineurogenic effect of stress [91, 96]. Moreover, the corticoids and IL-1 pathways may regulate each other in a bidirectional manner because the administration of a GR antagonist can blunt the LPS-induced production of hippocampal IL-1 in stressed mice [97], whereas mice knockout for the IL-1 receptor (IL-1R1) fail to display the characteristic elevation of corticosterone induced by mild chronic stress [96]. Another stress-related cytokine, IL-6, induces depressive phenotypes and prevents the antidepressant actions of fluoxetine when administered to mice in vivo [98]. So far the effects of stress on neurogenesis via corticosteroids and inflammation have been assumed to be cell autonomous, as neuroprogenitors express both GR [99] and IL-1R1 [95]. The potential participation of microglia is yet to be determined, but there are some reports of a direct effect of stress on microglial activation. For instance, microglia acutely isolated from mice subjected to acute stress (by inescapable tail shock) showed a primed response to LPS challenge by producing higher levels of IL-1 mRNA ex vivo [100], and the specific loss of expression of GR in microglia leads to a blunted inflammatory response in vitro and to a decreased neuronal damage in vivo in response to LPS [80]. In stress paradigms, these enhanced responses of microglia to inflammatory challenges are similar to their age-related “priming” which has been associated with and is possibly due to an increased basal production of proinflammatory mediators. However, whether microglia express increased levels of IL-1 and other proinflammatory cytokines in response to stressful events is presently unclear [101]. It is thus possible that some of the antineurogenic effects of stress are exerted by means of microglial-dependent inflammation, but this hypothesis remains to be experimentally tested.
- Inflammation Associated with Aging and Neurodegenerative Diseases
Inflammation is also commonly associated with normal aging and neurodegenerative diseases and, therefore, could represent a putative underlying mechanism that explains their decrease in hippocampal neurogenesis. Nonetheless, inflammation is also associated with neurological diseases, such as epilepsy or stroke, where neurogenesis is thought to be increased, although the data from rodents and humans is somewhat conflictive [102]. Neurogenesis is well known to decline throughout adulthood and normal aging in rodents and humans [103, 104], but the decay is more pronounced and occurs later in life in mice than in humans [105]. The aging-associated decrease in neurogenesis has been shown to occur mainly as a consequence of exhaustion of the rNSC population which, after being recruited and activated, undergo three rounds of mitosis in average and then terminally differentiate into astrocytes [12, 106]. In addition, a reduced mitotic capacity of the neuroprogenitors could further contribute to decreasing neurogenesis [106], and moreover, an age-related increase in the levels of proinflammatory cytokines could also hinder neurogenesis in the aging brain. Serum levels of IL-1, IL-6, and TNF are elevated in elderly patients [107, 108]. Aged microglia express higher levels of these proinflammatory cytokines and show a greater response to LPS inflammatory challenge, that is, a “primed” response, than their younger counterparts [109]. The origin of this low-grade age-related inflammation (“inflamm-aging” [110]) remains unknown and may be related to both aging and damage to the surrounding neurons, as well as aging of the immune system per se.
At the cellular level, stress to the endoplasmic reticulum (ER) caused by various perturbations, such as nutrient depletion, disturbances in calcium or redox status, or increased levels of misfolded proteins, can induce a cell-autonomous inflammatory response to neurons. Stress to the ER, a multifunctional organelle which is involved in protein folding, lipid biosynthesis, and calcium storage triggers a homeostatic response mechanism named the unfolding protein response (UPR), aiming to clear the unfolded proteins in order to restore normal ER homeostasis [111]. However, if the ER stress cannot be resolved, the UPR also initiates inflammatory and apoptotic pathways via activation of the transcription factor NF-B which controls the expression of most proinflammatory cytokines [112]. In the brain, ER stress is often initiated by the formation of abnormal protein aggregates in several neurodegenerative diseases such as Alzheimer’s disease (AD), Parkinson’s disease (PD), amyotrophic lateral sclerosis (ALS), Huntington’s disease (HD), and prion-related disorders [113]. This neurodegeneration-associated ER stress is assumed to occur mostly in neurons, but there are some examples of microglial protein misfolding as well. For instance, both microglia and neurons overexpress CHOP (C/EBP homologous protein), a transcription factor which is activated during ER stress in human patients and mouse models of ALS [114]. Inflammation has been speculated to be a main negative contributor to the pathology of ALS [115], but a direct microglial involvement in mediating the inflammatory response to abnormal protein aggregation in ALS and other neurodegenerative conditions remains to be tested. Finally, ER stress has been linked to a variety of inflammatory conditions [116, 117], including chronic stress, diet-induced obesity, and drug abuse, as well as atherosclerosis and arthritis [118–120]. During normal aging, a progressive decline in expression and activity of key ER molecular chaperones and folding enzymes could also compromise the adaptive response of the UPR, thereby contributing to the age-associated decline in cellular functions [118]. Therefore, aging is strongly associated with a chronic ER stress which leads to increased activation of NF-B [112]; however, the contribution of the different brain cell types to “inflamm-aging” is still poorly understood. The detrimental effects on neurogenesis of increased proinflammatory cytokines in the aging brain are not necessarily related to microglia, but also to stressed neurons. Furthermore, ER stress may also cause a cell-autonomous response in neural stem cells [121], although its impact on neurogenesis remains to be experimentally determined.
In addition, aging is accompanied by an increased level of mitochondrial oxidative stress, which in turn activates the “Inflammasome” [122], a group of multimeric proteins comprising the interleukin 1 converting enzyme (ICE, caspase 1) which serves to release the active form of the cytokine [123]. IL-1 may act directly on rNSCs (visualised by labeling with the Sox2 marker), as they express IL-1R1 in the adult hippocampus [91]. Treatment with IL-1 decreases hippocampal proliferation in young mice [91] and pharmacological inhibition of ICE partially restores the number of newborn neurons in aged mice without significantly affecting their differentiation rate [124]. Transgenic IL-1 overexpression results in chronic inflammation and depletion of doublecortin-labeled neuroblasts, thus mimicking the aging-associated depletion of neurogenesis [125]. The actual mechanism of action of IL-1 on neurogenesis in aged mice, including decreased proliferation of rNSCs/ANPs and survival of newborn neurons, remains undetermined. Microglia are a main source of IL-1in the aging brain, but the hypothesis that microglia-derived IL-1 is responsible for depleting neurogenesis in the aging brain remains to be directly tested.
The regulation of neurogenesis by IL-1 in the aging brain has been further linked to the activity of another cytokine, the chemokine fractalkine, or CX3CL1. Fractalkine has soluble and membrane-tethered forms and is exclusively expressed by neurons, while the fractalkine receptor (CX3CR1) is expressed in the brain by microglia alone [126]. This module forms a unique neuron-microglia signalling unit that controls the extent of microglial inflammation in several neurodegenerative conditions including PD, ALS [127], or AD [128]. In fact, CX3CR1 blocking antibodies increase the production of hippocampal IL-1 when administered to young adult rats [129]. Importantly, chronic treatment with fractalkine increases hippocampal proliferation and the number of neuroblasts in aged (22 months old) but not young (3 months old) or middle-aged rats (12 months old), whereas an antagonists of CX3CR1 has the opposite effects in young, but not in middle-aged nor old rats [129]. Since fractalkine expression is decreased during aging [129], a reduced neuron-microglia signalling might be releasing the brake on microglial contribution to inflammatory responses, although increased levels of fractalkine were instead reported in aged rat hippocampus by other studies [68]. Additional insights into the role of fractalkine signalling come from knock-in mice in which the endogenous CX3CR1 locus is replaced by the fluorescent reporter GFP [126]. The initial studies suggested that (i.e., ) mice have no significant differences in brain development and functions [130], but more systematic investigations recently revealed a long list of hippocampal-dependent changes in young (3 months old) and mice compared to wild-type mice. These changes notably included decreased neuroprogenitors proliferation and neuroblasts number, impaired LTP, performance in contextual fear conditioning and water maze spatial learning and memory, and, importantly, increased IL-1 protein levels [131]. The signalling pathway of fractalkine-IL-1 is functionally relevant, because IL-1R1 antagonists rescued LTP and cognitive function in mice [131]. In sum, even though neuronal fractalkine seems to be sufficient for restraining the inflammatory activity of microglia in young rats, its downregulation during aging could activate the microglial inflammatory response and thereby subsequently reduce the proliferation of remaining neuroprogenitors.
In AD, inflammatory cytokines such as IL-1 are overexpressed in the microglia associated with the amyloid beta (A) plaques of postmortem samples [132] and in transgenic mice modeling the disease [133]. The loss of synapses (from hippocampus to frontal cortex) is one of the main pathological substrates in this disease, but adult neurogenesis is also severely reduced in most mouse models of AD, possibly due to a decreased proliferation of neuroprogenitors and a decreased survival of newborn cells, even though the putative changes in the neurogenic cascade in postmortem samples remain controversial (reviewed in [102]). This lack of agreement is possibly explained by the fact that the vast majority of AD cases have a late onset over 65 years of age, when little neurogenesis remains. In contrast, in most transgenic AD mouse models, the Aaccumulation, cognitive deficits, and changes in neurogenesis are already detectable in young animals (2-3 months old). The study of AD is further hindered by the difficulty in comparing the time course and pathology across different mouse models. For instance, early treatment with minocycline can improve cognition and reduce A burden in mice expressing the human amyloid precursor protein (APP) [134]. In contrast, in mice expressing APP and a mutated form of presenilin 1 (PS1), which is part of the secretase pathway that cleaves A, inflammation is reduced without any detectable changes in A plaques deposition [135]. Concomitantly with a decrease in tissue inflammatory cytokines and number of microglial cells, minocycline restores neurogenesis and hippocampus-dependent memory deficits in these APP/PS1 mice [135], indirectly suggesting that cognitive decay in AD may be at least in part related to a detrimental effect of inflammation on hippocampal neurogenesis. Direct evidence that neurogenesis is associated with the cognitive performance in AD is still lacking. Further research is also necessary to determine the neurogenic targets of AD-related inflammation. One central open question for future therapies aiming at increasing neurogenesis and cognition in AD is whether neuroprogenitors are spared or whether their age-induced loss becomes accelerated. Rather than increasing the proliferation and neurogenic output of the few rNSCs remaining in an old AD brain, it may be more relevant to develop strategies that prevent the age-related loss of neuroprogenitors in presymptomatic patients.
In summary, inflammation associated with a wide variety of experimental models of disease produces strong detrimental effects on hippocampal neurogenesis. These effects on human neurogenesis are however not so well described and, in vitro, IL-1 increases the proliferation of hippocampal embryonic neuroprogenitors but decreases their differentiation into neurons [136]. Novel methods to assess hippocampal neurogenesis in the living human brain, from metabolomics of neuroprogenitors to hippocampal blood brain volume (reviewed in [102]), will help to determine the contribution of inflammation to adult neurogenesis in the healthy and diseased human brain during aging.
- Normal Physiological Conditions
In the healthy mature brain, microglia are an essential component of the neurogenic SGZ niche, where they physically intermingle with neuroprogenitors, neuroblasts, and newborn neurons [62]. Here, surveillant microglia effectively and rapidly phagocytose the excess of newborn cells undergoing apoptosis [62]. Importantly, microglial phagocytosis in the adult SGZ is not disturbed by inflammation associated with aging or by LPS challenge, as the phagocytic index (i.e., the proportion of apoptotic cells completely engulfed by microglia) is maintained over 90% in these conditions [62]. Nonetheless, the consequences of microglial phagocytosis on adult hippocampal neurogenesis remain elusive. Treatment of mice with annexin V, which binds to the phosphatidylserine (PS) receptor and prevents the recognition of PS on the surface of apoptotic cells, presumably blocking phagocytosis, increases the number of apoptotic cells in the SGZ [40]. Concomitantly, annexin V reduces neurogenesis by decreasing the survival of neuroblasts without affecting neuroprogenitors proliferation [40]. Similar results were obtained in transgenic mice knock-out for ELMO1, a cytoplasm protein which promotes the internalization of apoptotic cells, although the effects on neurogenesis were ascribed to a decreased phagocytic activity of neuroblasts [40]. The actual phagocytic target of the neuroblasts remains undetermined, but the newborn apoptotic cells in the adult SGZ are exclusively phagocytosed by microglia, at least in physiological conditions [62]. Nevertheless, none of the above manipulations has specifically tested the role of microglial phagocytosis in hippocampal-dependent learning and memory and thus, the functional impact of microglial phagocytosis in adult neurogenic niches during normal physiological conditions remains to be elucidated.
Microglial phagocytosis of apoptotic cells is actively anti-inflammatory, at least in vitro, and thus it has been hypothesized that anti-inflammatory cytokines produced by phagocytic microglia may further regulate neurogenesis [10]. For instance, transforming growth factor beta (TGF), which is produced by phagocytic microglia in vitro [137], inhibits the proliferation of SGZ neuroprogenitors [138]. Microglia are further able to produce proneurogenic factors in vitro [139]. When primed with cytokines associated with T helper cells such as interleukin 4 (IL-4) or low doses of interferon gamma (IFN), cultured microglia support neurogenesis and oligodendrogenesis through decreased production of TNF and increased production of insulin-like growth factor 1 (IGF-1) [139], an inducer of neuroprogenitor proliferation [26]. A list of potential factors produced by microglia and known to act on neuroprogenitor proliferation can be found in Table 1. In addition, recent observations suggest that neuroprogenitor cells may not only regulate their own environment, but also influence microglial functions. For instance, vascular endothelial growth factor (VEGF) produced by cultured neuroprecursor cells directly affects microglial proliferation, migration, and phagocytosis [20]. More potential factors produced by neuroprogenitors shown to be influencing microglial activity and function can be found in Table 2. However, it has to be taken into account that most of these observations were obtained in culture and that further research is needed in order to elucidate whether those factors are also secreted and have the same regulatory responses in vivo.
| Table 1: Summary of factors secreted by microglia and the potential effect they have on neuroprogenitors in vitro. |
|
Microglia secreted
factors |
Reference |
Modulation of neural progenitor cells |
Reference |
|
| BDNF |
[18] |
Differentiation |
[19] |
| EGF |
[20] |
Survival, expansion, proliferation, differentiation |
[21] |
| FGF |
[22] |
Survival and expansion |
[23] |
| GDNF |
[24] |
Survival, migration, and differentiation |
[25] |
| IGF-1 |
[21] |
Proliferation |
[26] |
| IL-1 |
[27] |
Reduction in migration |
[27] |
| IL-6 |
[28] |
Inhibition of neurogenesis |
[29] |
| IL-7 |
[20] |
Differentiation |
[30] |
| IL-11 |
[20] |
Differentiation |
[30] |
| NT-4 |
[24] |
Differentiation |
[31] |
| PDGF |
[32] |
Expansion and differentiation |
[33] |
| TGF |
[34] |
Inhibition of proliferation |
[19] |
|
Table 1: Summary of factors secreted by microglia and the potential effect they have on neuroprogenitors in vitro.
http://www.hindawi.com/journals/np/2014/610343/tab1/
Table 2: Summary of factors secreted by neuroprogenitors and the potential effect they have on microglia in vitro.
|
| NPC secreted factors |
Reference |
Modulation of microglia |
Reference |
|
| BDNF |
[18] |
Proliferation and induction of phagocytic activity |
[35] |
| Haptoglobin |
[24] |
Neuroprotection |
[36] |
| IL-1 |
[37] |
Intracellular Ca+2 elevation and proliferation |
[22] |
| IL-6 |
[37] |
Increase in proliferation |
[38] |
| M-CSF |
[20] |
Mitogen |
[39] |
| NGF |
[40] |
Decrease in LPS-induced NO |
[41] |
| TGF |
[37] |
Inhibition of TNF secretion |
[42] |
| TNF |
[37] |
Upregulation of IL-10 secretion |
[43] |
| VEGF |
[20] |
Induction of chemotaxis and proliferation |
[20] |
|
http://www.hindawi.com/journals/np/2014/floats/610343/thumbnails/610343.tab2_th.jpg
Table 2: Summary of factors secreted by neuroprogenitors and the potential effect they have on microglia in vitro.
In addition, microglial capacity to remodel and eliminate synaptic structures during normal physiological conditions has suggested that microglia could also control the synaptic integration of the newborn neurons generated during adult hippocampal neurogenesis [140]. Three main mechanisms were proposed: (1) the phagocytic elimination of nonapoptotic axon terminals and dendritic spines, (2) the proteolytic remodeling of the perisynaptic environment, and (3) the concomitant structural remodeling of dendritic spines [7, 140]. Indeed, microglial contacts with synaptic elements are frequently observed in the cortex during normal physiological conditions, sometimes accompanied by their engulfment and phagocytic elimination [141–143], as in the developing retinogeniculate system [144]. Microglial cells are distinctively surrounded by pockets of extracellular space, contrarily to all the other cellular elements [142], suggesting that microglia could remodel the volume and geometry of the extracellular space, and thus the concentration of various ions, neurotransmitters, and signalling molecules in the synaptic environment. Whether microglia create the pockets of extracellular space themselves or not remains unknown, but these pockets could result from microglial release of extracellular proteases such as metalloproteinases and cathepsins [145], which are well known for influencing the formation, structural remodeling, and elimination of dendritic spines in situ and also experience-dependent plasticity in vivo [7, 146]. More recently, microglial phagocytosis of synaptic components was also observed in the developing hippocampus, in the unique time window of synaptogenesis, a process which is notably regulated by fractalkine-CX3CR1 signalling [147]. Therefore, the attractive hypothesis that microglial sculpts the circuitry of newborn cells in the adult hippocampus deserves further attention.
Lastly, microglia were also involved in increasing adult hippocampal neurogenesis in the enriched environment (EE) experimental paradigm. EE is a paradigm mimicking some features of the normal living circumstances of wild animals, as it gives them access to social interactions, toys, running wheels, and edible treats. EE has long been known to enhance neurogenesis by acting on newborn cells survival, resulting ultimately in an enlargement of the dentate gyrus [148]. Functionally, these changes are accompanied by enhanced spatial learning and memory formation with the water maze paradigm [149]. Similar increases in neurogenesis are obtained by subjecting mice to voluntary running paradigms, although in this case the effect is mediated by increased neuroprogenitor proliferation [150]. During inflammatory conditions, EE is antiapoptotic and neuroprotective [151] and it limits the hippocampal response to LPS challenge by decreasing the expression of several cytokines and chemokines, including IL1- and TNF [152]. In fact, EE is believed to counteract the inflammatory environment and rescue the decreased number of neuroblasts in mice compared to wild-type mice [153]. The effects of EE are independent of the IL-1 signalling pathway, as it increases neurogenesis in mice that are null for IL-1R1 [154]. EE also induces microglial proliferation and expression of the proneurogenic IGF-1 [155], but the full phenotype of microglia in EE compared to standard housing and its impact on the neurogenic cascade remains to be determined.
The mechanisms behind the anti-inflammatory actions of EE are unknown, but they were suggested to involve microglial interactions with T lymphocytes through an increased expression of the major histocompatibility complex of class II (MHC-II) during EE [155]. MHC-II is responsible for presenting the phagocytosed and degraded antigens to the antibodies expressed on the surface of a subtype of T lymphocytes (T helper or CD4+ cells), thus initiating their activation and production of antigen-specific antibodies. Severe combined immunodeficient (SCID) mice lacking either T and B lymphocytes or nude mice lacking only T cells have impaired proliferation and neurogenesis in normal and EE housing compared to wild-type mice [155], as well as impaired performance in the water maze [156]. Similarly, antibody-based depletion of T helper lymphocytes impairs basal and exercise-induced proliferation and neurogenesis [157]. Furthermore, a genetic study in heterogeneous stock mice, which descend from eight inbred progenitor strains, has found a significant positive correlation between genetic loci associated to hippocampal proliferation and to the proportion of CD4+ cells among blood CD3+ lymphocytes [158]. Additional experiments are needed to fully determine the possible interactions between microglia and T cells in neurogenesis, because, at least in normal physiological conditions, (1) T cell surveillance of the brain parenchyma is minimal, (2) microglia are poor antigen presenting cells, and (3) antigen presentation by means of MHC-II family of molecules is thought to occur outside the brain, that is, in the meninges and choroid plexus [159]. In fact, during voluntary exercise, there are no significant changes in T cell surveillance of the hippocampus, nor a direct interaction between T cells and microglia, nor any changes in the gene expression profile of microglia, including that of IGF-1, IL-1, and TNF [160]. The number of microglia is also inversely correlated with the number of hippocampal proliferating cells, rNSCs, and neuroblasts in aged (8 months) mice subjected to voluntary running, as well asin vitro cocultures of microglia and neuroprogenitors, which has been interpreted as resulting from an overall inhibitory effect of microglia on adult neurogenesis [161]. Even though EE is clearly a more complex environmental factor than voluntary running, further research is necessary to disregard nonspecific or indirect effects of genetic or antibody-based T cells depletion on microglia and other brain cell populations, including rNSCs. For instance, adoptive transfer of T helper cells treated with glatiramer acetate, a synthetic analog of myelin basic protein (MBP) approved for the treatment of multiple sclerosis, produces a bystander effect on resident astrocytes and microglia by increasing their expression of anti-inflammatory cytokines such as TGF[162]. Alternatively, it has been suggested that T cells may mediate an indirect effect on adult hippocampal neurogenesis by increasing the production of brain-derived neurotrophic factor (BDNF) [157], which is involved in the proneurogenic actions of EE [163]. Whether BDNF can counteract the detrimental effects of T cell depletion on neurogenesis remains unknown. Overall, the roles of microglia in EE and running-induced neurogenesis are unclear and have to be addressed with more precise experimental designs. In summary, surveillant microglia are part of the physical niche surrounding the neural stem cells and newborn neurons of the mature hippocampus, where they continuously phagocytose the excess of newborn cells. Microglia were also linked to the proneurogenic and anti-inflammatory effects of voluntary running and EE, but direct evidence is missing. The overall contribution of microglia to neurogenesis and learning and memory in normal physiological conditions remains largely unexplored at this early stage in the field.
- Conclusion
In light of these observations, microglia are now emerging as important effector cells during normal brain development and functions, including adult hippocampal neurogenesis. Microglia can exert a positive or negative influence on the proliferation, survival, or differentiation of newborn cells, depending on the inflammatory context. For instance, microglia can compromise the neurogenic cascade during chronic stress, aging, and neurodegenerative diseases, by their release of proinflammatory cytokines such as IL-1, IL-6, and TNF. A reduced fractalkine signalling between neurons and microglia could also be involved during normal aging. However, microglia are not necessarily the only cell type implicated because astrocytes, endothelial cells, mast cells, perivascular and meningeal macrophages, and to a lesser extent neurons and invading peripheral immune cells could further contribute by releasing proinflammatory mediators.
Additionally, microglia were shown to phagocytose the excess of newborn neurons undergoing apoptosis in the hippocampal neurogenic niche during normal physiological conditions, while a similar role in the synaptic integration of newborn cells was also proposed in light of their capacity to phagocytose synaptic elements. Lastly, microglial interactions with T cells, leading to the release of anti-inflammatory cytokines, neurotrophic factors, and other proneurogenic mediators (notably during EE and voluntary running), could counteract the detrimental effects of inflammation on adult hippocampal neurogenesis and their functional implications for learning and memory.
However, further research is necessary to assess the relative contribution of microglia versus other types of resident and infiltrating inflammatory cells and to determine the nature of the effector cytokines and other inflammatory mediators involved, as well as their cellular and molecular targets in the neurogenic cascade. Such research will undoubtedly help to develop novel strategies aiming at protecting the neurogenic potential and ultimately its essential contribution to learning and memory.
Abbreviations
| AD: |
Alzheimer’s disease |
| ANPs: |
Amplifying neuroprogenitors |
| APP: |
Amyloid precursor protein |
| A: |
Amyloid beta |
| BDNF: |
Brain-derived neurotrophic factor |
| BrdU: |
5-Bromo-2′-Deoxyuridine |
| CX3CL1: |
Fractalkine |
| CX3CR1: |
Fractalkine receptor |
| EAE: |
Experimental acute encephalomyelitis |
| EE: |
Enriched environment |
| EGF: |
Epidermal growth factor |
| FGFb: |
Basic fibroblast growth factor |
| GDNF: |
Glial cell line-derived neurotrophic factor |
| GFAP: |
Glial fibrillary acidic protein |
| GR: |
Glucocorticoid receptor |
| HPA: |
Hypothalamic-pituitary-adrenal axis |
| ICE: |
Interleukin 1 converting enzyme |
| IL-1: |
Interleukin 1 beta |
| IL-1R1: |
Interleukin 1 beta receptor |
| IL-4: |
Interleukin 4 |
| IL-6: |
Interleukin 6 |
| IL-7: |
Interleukin 7 |
| IL-11: |
Interleukin 11 |
| IFN: |
Interferon gamma |
| IGF-1: |
Insulin-like growth factor 1 |
| iNOS: |
Inducible nitric oxide synthase |
| LPS: |
Bacterial lipopolysaccharides |
| LTP: |
Long term potentiation |
| M-CSF: |
Macrophage colony-stimulating factor |
| MBP: |
Myelin basic protein |
| MHC-II: |
Major histocompatibility complex class II |
| MOG: |
Myelin oligodendrocyte glycoprotein |
| NF-B: |
Nuclear factor kappa-light-chain-enhancer of activated B cells |
| NGF: |
Nerve growth factor |
| NO: |
Nitric oxide |
| NSAID: |
Nonsteroidal anti-inflammatory drug |
| NT-4: |
Neurotrophin-4 |
| PDGF: |
Platelet-derived growth factor |
| PS: |
Phosphatidylserine |
| PS1: |
Presenilin 1 |
| ROS: |
Radical oxygen species |
| SCID: |
Severe combined immunodeficiency |
| SGZ: |
Subgranular zone |
| TGF: |
Transforming growth factor beta |
| TNF: |
Tumor necrosis factor alpha |
| VEGF: |
Vascular endothelial growth factor. |
Conflict of Interests
The authors declare that there is no conflict of interests regarding the publication of this paper.
Acknowledgments
This work was supported by grants from the Spanish Ministry of Economy and Competitiveness to Amanda Sierra (BFU2012-32089) and Juan M. Encinas (SAF2012-40085), from Basque Government (Saiotek S-PC 12UN014) and Ikerbasque start-up funds to Juan M. Encinas and Amanda Sierra, and from The Banting Research Foundation, the Scottish Rite Charitable Foundation of Canada, and start-up funds from Université Laval and Centre de recherche du CHU de Québec to Marie-Ève Tremblay.
References
- P. Rezaie and D. Male, “Mesoglia and microglia—a historical review of the concept of mononuclear phagocytes within the central nervous system,” Journal of the History of the Neurosciences, vol. 11, no. 4, pp. 325–374, 2002. View at Publisher · View at Google Scholar · View at Scopus
- F. Ginhoux, S. Lim, G. Hoeffel, D. Low, and T. Huber, “Origin and differentiation of microglia,”Frontiers in Cellular Neuroscience, vol. 7, article 45, 2013. View at Publisher · View at Google Scholar
- E. Gomez Perdiguero, C. Schulz, and F. Geissmann, “Development and homeostasis of “resident” myeloid cells: the case of the microglia,” GLIA, vol. 61, no. 1, pp. 112–120, 2013. View at Publisher ·View at Google Scholar
- H. Kettenmann, F. Kirchhoff, and A. Verkhratsky, “Microglia: new roles for the synaptic stripper,”Neuron, vol. 77, no. 1, pp. 10–18, 2013. View at Publisher · View at Google Scholar
- A. Aguzzi, B. A. Barres, and M. L. Bennett, “Microglia: scapegoat, saboteur, or something else?” Science, vol. 339, no. 6116, pp. 156–161, 2013. View at Publisher · View at Google Scholar
- K. Helmut, U. K. Hanisch, M. Noda, and A. Verkhratsky, “Physiology of microglia,” Physiological Reviews, vol. 91, no. 2, pp. 461–553, 2011. View at Publisher · View at Google Scholar · View at Scopus
- M. È. Tremblay, B. Stevens, A. Sierra, H. Wake, A. Bessis, and A. Nimmerjahn, “The role of microglia in the healthy brain,” Journal of Neuroscience, vol. 31, no. 45, pp. 16064–16069, 2011. View at Publisher ·View at Google Scholar · View at Scopus
- A. Miyamoto, H. Wake, A. J. Moorhouse, and J. Nabekura, “Microglia and synapse interactions: fine tuaning neural circuits and candidate molecules,” Frontiers in Cellular Neuroscience, vol. 7, article 70, 2013. View at Publisher · View at Google Scholar
- C. Bechade, Y. Cantaut-Belarif, and A. Bessis, “Microglial control of neuronal activity,” Frontiers in Cellular Neuroscience, vol. 7, article 32, 2013. View at Publisher · View at Google Scholar
- A. Sierra, O. Abiega, A. Shahraz, and H. Neumann, “Janus-faced microglia: beneficial and detrimental consequences of microglial phagocytosis,” Frontiers in Cellular Neuroscience, vol. 7, article 6, 2013. View at Publisher · View at Google Scholar
- G. Kempermann, S. Jessberger, B. Steiner, and G. Kronenberg, “Milestones of neuronal development in the adult hippocampus,” Trends in Neurosciences, vol. 27, no. 8, pp. 447–452, 2004. View at Publisher ·View at Google Scholar · View at Scopus
- J. M. Encinas, T. V. Michurina, N. Peunova et al., “Division-coupled astrocytic differentiation and age-related depletion of neural stem cells in the adult hippocampus,” Cell Stem Cell, vol. 8, no. 5, pp. 566–579, 2011. View at Publisher · View at Google Scholar · View at Scopus
- M. A. Bonaguidi, M. A. Wheeler, J. S. Shapiro et al., “In vivo clonal analysis reveals self-renewing and multipotent adult neural stem cell characteristics,” Cell, vol. 145, no. 7, pp. 1142–1155, 2011. View at Publisher · View at Google Scholar · View at Scopus
- J. J. Breunig, J. I. Arellano, J. D. Macklis, and P. Rakic, “Everything that glitters isn’t gold: a critical review of postnatal neural precursor analyses,” Cell Stem Cell, vol. 1, no. 6, pp. 612–627, 2007. View at Publisher · View at Google Scholar · View at Scopus
- L. S. Overstreet-Wadiche and G. L. Westbrook, “Functional maturation of adult-generated granule cells,” Hippocampus, vol. 16, no. 3, pp. 208–215, 2006. View at Publisher · View at Google Scholar · View at Scopus
……………….
Review
Nature Reviews Molecular Cell Biology 8, 519-529 (July 2007) | doi:10.1038/nrm2199
Signal integration in the endoplasmic reticulum unfolded protein response
David Ron & Peter Walter
http://www.nature.com/nrm/journal/v8/n7/full/nrm2199.html
The endoplasmic reticulum (ER) responds to the accumulation of unfolded proteins in its lumen (ER stress) by activating intracellular signal transduction pathways — cumulatively called the unfolded protein response (UPR). Together, at least three mechanistically distinct arms of the UPR regulate the expression of numerous genes that function within the secretory pathway but also affect broad aspects of cell fate and the metabolism of proteins, amino acids and lipids. The arms of the UPR are integrated to provide a response that remodels the secretory apparatus and aligns cellular physiology to the demands imposed by ER stress.
Figure 1: The unfolded protein response (UPR) signalling pathways.
FromThe impact of the endoplasmic reticulum protein-folding environment on cancer development
Nature Reviews Cancer 14, 581–597 (2014) http://dx.doi.org:/10.1038/nrc3800

(UPR) signalling pathways
http://www.nature.com/nrc/journal/v14/n9/images/nrc3800-f1.jpg
Upon endoplasmic reticulum (ER) stress, unfolded and misfolded proteins bind and sequester immunoglobulin heavy-chain binding protein (BIP), thereby activating the UPR. The UPR comprises three parallel signalling branches: PRKR-like ER kinase (PERK)–eukaryotic translation initiation factor 2α (eIF2α), inositol-requiring protein 1α (IRE1α)–X-box binding protein 1 (XBP1) and activating transcription factor 6α (ATF6α). The outcome of UPR activation increases protein folding, transport and ER-associated protein degradation (ERAD), while attenuating protein synthesis. If protein misfolding is not resolved, cells enter apoptosis. CHOP, C/EBP homologous protein; GADD34, growth arrest and DNA damage-inducible protein 34; JNK, JUN N-terminal kinase; P, phosphorylation; RIDD, regulated IRE1-dependent decay; ROS, reactive oxygen species; XBP1s, transcriptionally active XBP1; XBP1u, unspliced XBP1.
Figure 3: The unfolded protein response (UPR) and inflammation.

(UPR) and inflammation
http://www.nature.com/nrc/journal/v14/n9/images/nrc3800-f3.jpg
The three UPR pathways augment the production of reactive oxygen species (ROS) and activate nuclear factor-κB (NF-κB) and activator protein 1 (AP1) pathways, thereby leading to inflammation. NF-κB, which is a master transcriptional regulator of pro-inflammatory pathways, can be activated through binding to the inositol-requiring protein 1α (IRE1α)–TNF receptor-associated factor 2 (TRAF2) complex in response to endoplasmic reticulum (ER) stress, leading to recruitment of the IκB kinase (IKK), IκB phosphorylation (P) and degradation, and nuclear translocation of NF-κB196. Moreover, the IRE1α–TRAF2 complex can recruit apoptosis signal-regulating kinase 1 (ASK1) and activate JUN N-terminal kinase (JNK), increasing the expression of pro-inflammatory genes through enhanced AP1 activity197. The PRKR-like ER kinase (PERK)–eukaryotic translation initiation factor 2α (eIF2α) and activating transcription factor 6α (ATF6α) branches of the UPR activate NF-κB through different mechanisms. Engaging PERK–eIF2α signalling halts overall protein synthesis and increases the ratio of NF-κB to IκB, owing to the short half-life of IκB, thereby freeing NF-κB for nuclear translocation198, 199. ATF6α activation following exposure to the bacterial subtilase cytotoxin that cleaves immunoglobulin heavy-chain binding protein (BIP) leads to AKT phosphorylation and consequent NF-κB activation109, 200.
Figure 4
The cancer-supporting role of the unfolded protein response (UPR).
http://www.nature.com/nrc/journal/v14/n9/images/nrc3800-f4.jpg

cancer-supporting role of the unfolded protein response
Read Full Post »