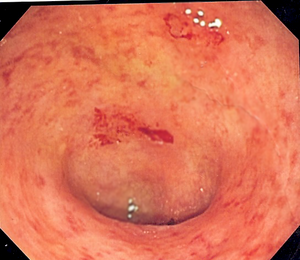
Diarrheas – Bacterial and Nonbacterial
Writer and Curator: Larry H. Bernstein, MD, FCAP
Introduction
Diarrheas are one of the common problems of societies worldwide. However, the prevalence of cause of the diarrhea may be different depending on location, water quality, food source, age, and psychological stress factors.
Microbial and Parasitic Diseases
A Systematic Review on Neglected Important Protozoan Zoonoses
Yibeltal Muhie Mekonen and Simenew Keskes Melaku
Int. J. Adv. Res. Biol.Sci. 2(1): (2015): 53–65
Infectious protozoan parasites are transmitted to humans through several routes, including contaminated food and water, inadequately treated sewage/sewage products, and livestock and domestic pet handling. Several enteric protozoa cause severe morbidity and mortality in both humans and animals worldwide. In developed settings, enteric protozoa are often ignored as a cause of diarrheal illness due to better hygiene conditions, and as such, very little effort is used toward laboratory diagnosis. Although these protozoa contribute to the high burden of infectious diseases, estimates of their true prevalence are sometimes affected by the lack of sensitive diagnostic techniques to detect them in clinical and environmental specimens. Despite recent advances in the epidemiology, molecular biology, and treatment of protozoan illnesses, gaps in knowledge still exist, requiring further research. There is evidence that climate-related changes will contribute to their burden due to displacement of ecosystems and human and animal populations, increases in atmospheric temperature, flooding and other environmental conditions suitable for transmission, and the need for the reuse of alternative water sources to meet growing population needs. This review discusses the common enteric protozoa from a public health perspective, highlighting their epidemiology, modes of transmission, prevention and control and epidemiological pictures in Ethiopia. It also discusses the potential impact of climate changes on their epidemiology and the issues surrounding waterborne transmission and suggests a multidisciplinary approach to their prevention and control.
Approximately 60 percent of all human pathogens are zoonoses of microbes that are naturally transmitted between animals and humans. Neglect of their control persists because of a lack of information and awareness about their distribution, a lack of suitable tools and managerial capacity for their diagnosis, and a lack of appropriate and sustainable strategies for their prevention and control. Furthermore, many of the most affected countries have poor or non-existent veterinary public health infrastructures. This situation has marginalized control of zoonoses to the gap between veterinary responsibilities and medical needs, generating a false perception that their burden and impact on society are low. As a result, neither the human and animal health resources nor the research needed for their control are available spawning a category of non zoonotic diseases (Choffnes and Relman, 2011).
The neglected tropical diseases (NTDs) are the most common conditions affecting the poorest 500 million people living in sub-Saharan Africa (SSA), and together produce a burden of disease that may be equivalent to up to one-half of SSA’s malaria disease burden and more than double that caused by tuberculosis (Hotez and Kamath, 2009).Starting with an initial set of 13-15 diseases, there are now over 40 helminth, protozoal, bacterial, viral, fungal and ectoparasitic infections covered under the brand-name of the neglected tropical diseases. Gaps in our understanding of the epidemiology and control of many of the neglected tropical diseases remain, which calls for additional funding for innovative research (Jürg et al, 2012).
The health and socioeconomic impacts of zoonotic parasitic and related food-borne diseases are growing continuously and increasingly being felt most particularly by developing countries. Apart from causing human morbidity and mortality, they hamper agricultural production, decrease availability of food, and create barriers to international trade (Solaymani-Mohammadi and Petri, 2006). The problem of zoonoses has spread from predominantly restricted rural areas into regional and, in some cases, worldwide epidemics. This is due to the great changes of the previous decades, especially the increasing urbanization, most of which is inadequate planned. In addition, large movements of populations, opening up of badly needed new areas for food production, the increasing trade in meat, milk and other products of animal origin, the increasing number and speed of vehicles, and even tourism have contributed to expanding the impact of zoonotic diseases. The challenges of food-borne, waterborne, and zoonotic protozoan diseases associated with climate change are expected to increase, with a need for active surveillance systems, some of which have already been initiated by several developed countries. However, very little effects are attempting in the developing world which actually are the main victims.
The prevalence rates are generally higher in immunodeficient compared to immune-competent patients. However, most studies on prevalence have been carried out in developed countries where the laboratory and clinical infrastructure are more easily available. Protozoan pathogens and HIV interact in their host, modifying the immunopathology of disease and complicating therapeutic intervention. Disease prevalence and distribution and population movements impact greatly on HIV/protozoan parasite co-infections (Andeani et al, 2012).
In Ethiopia there are little reports regarding protozoan zoonoses. However, there are still reports from clinics and hospitals where these diseases are becoming major issues of concern. This review will examine published data on the neglected protozoan pathogens in Ethiopia and analyses their current importance to public health.
Important but Neglected Protozoan Zoonoses Dealt in this Critical Review
This disease is caused by a single cell protozoan parasite called Entamoeba spp. (E. histolytica, E. polecki). Invasive amebiasis is one of the world most prevalent and fatal infectious diseases. Around 500 million people are infected worldwide while 75,000 die of the disease annually. Behind malaria and schistosomiasis, amebiasis ranks third on the list of parasitic causes of death worldwide. The infection is common in developing countries and predominantly affects individuals with poor socioeconomic conditions, non hygienic practices, and malnutrition (Stanley, 2003).
A number of survey and routine diagnosis in Ethiopia indicate that amebiasis is one of the most widely distributed diseases. In a countrywide survey of amebiasis in 97 communities, the overall prevalence of Entamoeba histolytica infections, as measured by rate of cyst-passers, in schoolchildren and non-school communities were 15.0% and 3.5%, respectively (Erko et al, 1995). A study conducted on the prevalence of Entamoeba histolytica/dispar among children in Legedini, Adada and Legebira, Dire-Dawa administrative region was 33.7% (Dawit, 2006 Unpublished MSc Thesis).
Giardiasis is caused by Giardia lamblia (also known as Giardia duodenalis or G. intestinalis) is a unicellular, flagellated intestinal protozoan parasite of humans isolated worldwide and is ranked among the top 10 parasites of man (Farthing and Kelly, 2005). Its occurrence is worldwide (Figure 1) and prevalence very high in areas with poor sanitation and in institutions. Human infections usually originate from other humans but may result from contact with dogs, cats, rodents, beavers, or nonhuman primates. The prevalence of the disease varies from 2% to 5% in developed to 20% to 30% in developing countries. The variation in prevalence might be attributed to factors such as the geographical area, the urban or rural setting of the society, the age group composition and the socio-economical conditions of the study subject.

Risk of disease caused by Giarda species
Risk of disease caused by Giarda species with different degrees Source: Esch and Petersen (2013)
According to Birrie and Erko (1995) based on a countrywide survey of giardiasis, the overall prevalence among school children and residents were 8.9% and 3.1%, respectively and that of the non-school children were 4.4%. Recent report indicates that the prevalence of Giardia lamblia among diarrhea patients referred to EHNRI (Ethiopian Health and Nutrition Research Institute) was 8.6%. In a study conducted in South Western Ethiopia, the prevalence of Giardiasis was 13.7%. A study conducted for the determination of Prevalence of Giardiasis and Cryptosporidiosis among children in relation to water sources in selected Village of Pawi Special District in Benishangul-Gumuz Region, Northwestern Ethiopia showed that out of the 384 children examined, 102 for giardiasis.
Leishmaniasis is an ancient disease caused by protozoans from the Leishmania genus and transmitted by the bite of a sand fly. It has four subtypes of varying severity, which include cutaneous and visceral infections. Cutaneous infection results in the formation of disfiguring lesions which frequently occur on the face, arms and legs. Lesions may last anywhere from a few weeks to over a year; secondary lesions may also occur years after the initial lesion has healed. Visceral cases can result in anemia, fever, debility and death if left untreated.
About 20 species of Leishmania infect mammals and many of them can cause human leishmaniasis. Motile infective forms of the parasite (metacyclic promastigotes with a long free flagellum) develop in the guts of competent sand fly vectors, which inoculate them into mammalian skin. Infections can spread, often via the lymphatic system, to cause secondary dermal lesions with forms and tissue tropisms in humans that show some parasite species specificity. Leishmaniasis can visceralize (for example Leishmania (Leishmania) tropica, which normally causes Oriental sore), but only two species of the subgenus Leishmania routinely do so, and these are the causative agents of most human visceral leishmaniasis (VL) worldwide.

Global burden of Leishmania
Global burden of Leishmania as adapted from the “Leshimaniases and Leishmania HIV co-infection” WHO fact sheet No. 116, May 2000
The New World visceral leishmaniasis is in Latin America and southern United States. Of course the visceral form also is common in Asia, Africa, Europe and Latin America. Both VL and CL are important endemic vector‐borne diseases in Ethiopia. The Federal Ministry of Health (FMoH) estimates the annual burden of VL to be between 4,500 and 5,000 cases (FMoH Ethiopia, 2006 unpublished). Known VL endemic foci are in the arid southwest, and the Humera and Metema lowlands in the north‐west. About 2-12% of all visceral leishmaniasis cases involve HIV coinfections underlines the synergic aspect of both diseases; such proportions may reach 40%, as in Humera, northwest Ethiopia (WHO, 2007), where coinfections have increased two-fold in the last decade (Andreani et al, 2012).
The causes of this disease are Cryptosporidium spp. (C. parvum, possibly others). In humans, abdominal pain, nausea, watery diarrhea lasting 3-4 days. In immune-deficient or immune-suppressed people, the disease is severe, with persistent diarrhea (6-25 evacuations per day) and malabsorption of nutrients. In normal persons the disease is self-limiting. In immune-compromised individuals, disease is severe and case fatality rate may be high. In animals normally a clinical disease can be seen only among young neonates. In ruminants, gastroenteritis and diarrhea are common.
Toxoplasmosis is among the global major zoonotic diseases and the third leading cause of food-related deaths in the USA. It is caused by Toxoplasma gondii, an Apicomplexa protozoan parasite, with cats as the definitive host. Cats are considered the key in the transmission of Toxoplasma gondii to humans because they are the only hosts that can excrete the environmentally resistant oocysts in their feces.

Human seroprevalece of Toxoplasma gondii
Human seroprevalece of Toxoplasma gondii. Esch and Petersen (2013)
The clinical impact of zoonotic enteric protozoan infections is greatest in the developing world where inadequate sanitation, poor hygiene and proximity to zoonotic reservoirs, particularly companion animals and livestock are greatest. In such circumstances, it is not surprising that infections with more than one species of enteric protozoan are common, and in fact single infections are rare.

Impact of animal disease on human health
Impact of animal disease on human health
The protozoan zoonoses circulating in Ethiopia are major burden on public health and wellbeing. The magnitude and scope of this burden varies for each of the protozoan parasites discussed in this manuscript. Apart from causing human morbidity and mortality, they hamper agricultural production, decrease availability of food, and create barriers to international trade. It is generally believed that although these parasitic infections are distributed worldwide, their prevalence is higher in developing compared to developed countries. However, the relative importance of zoonotic infections especially in developing countries has not been studied in detail including. These protozoan zoonoses are the most neglected but very important in terms of human health and veterinary concerns. The main share belongs to cryptosporidiosis; giardiasis, toxoplasmosis, leishmaniasis and amebiasis are some of the major protozoan zoonoses.
Clinical Microbiology: Past, Present, and Future
Henry D. Isenberg
J Clin Microbiol, Mar. 2003; 41(3):917–918
http://dx.doi.org:/10.1128/JCM.41.3.917–918.2003
During the last two decades of the 19th century, a plethora of bacteria were isolated and designated etiological agents of human infectious diseases. As with many instances at the interface between cause and effective therapy, the further characterization of these alleged pathogens remained in the hands of a few devoted investigators until drugs with therapeutic potential became available. This vague period before the advent of proper cures for infections explains the shadowy origin of clinical or diagnostic microbiology. But, as R. Porter has stated, “history should be rooted in detail and as messy as life itself”; this is an undeniable description of the history of clinical microbiology, long the stepchild, frequently denied legitimacy, among the many siblings that constitute the science of microbiology. Yet the practice of clinical microbiology is the application of knowledge gained to the betterment of the human condition, the goal of clinical microbiologists.
The advances in the grouping and typing of streptococci, salmonellae, and shigellae, the separation of Staphylococcus aureus on the basis of the coagulase reaction, and the growing awareness of the need for safe water and uncontaminated food items established the need for laboratories to assume these responsibilities. It was only logical that microbiology should join endeavors such as chemistry, hematology, and serology under the rubric of clinical pathology. Differential media especially designed to sequester species increased dramatically during Word War II; military hospitals developed clinical microbiology sections devoted not only to recognizing agents endangering the health of troops in camps, in battle, and in foreign environments but also to assessing the responses of certain of the microorganisms isolated to several sulfonamides and that hitherto unknown agent, penicillin. The subsequent explosion of antimicrobial agents—streptomycin, chloramphenicol, tetracyclines, and erythromycin—suggested to the reigning powers of medical facilities that clinical microbiologists could be phased out, since infectious disease would disappear before the onslaught of agents discovered through human ingenuity.
In the interim, cotton plugs gave way to Bakelite, polypropylene, glass, metal, and plastic closures; in-house medium preparation was relieved in part by the beginnings of commercially manufactured ready-to-use media especially for mycobacteria and antimicrobial susceptibility testing. Alcohol, Bunsen, and Tyril burners were replaced by microincinerators, eventually followed by disposable loops and transfer needles. The prescient wisdom of hospital boards soon was shattered by the genetic versatility of the microbial world, dramatically demonstrated by the pandemic of S. aureus 80/81 in the late 1950s and early 1960s and the emergence of gram-negative rods that demonstrated the superiority of the bacterial physiology over the commercially prepared secondary microbial metabolites that initially appeared so promising. To be sure, the tug of war between antimicrobial agents—natural and synthetic—and the microorganisms continues unabated, with signs that the evolutionary potential of the microbial world will succeed in the long run.
Since the 1960s, numerous ingenious innovations have been introduced. Molecular biology techniques promise to revolutionize the diagnosis of infectious disease—to date a promise still in its infancy. Systems approaches began to replace the single test tube with but one substrate. Perhaps the first was double sugar iron agar for the recognition of so-called enteric pathogens, followed by triple sugar iron agar and the next tentative shortcut, the r/b tube. Rollender and Beckford, the inventors of the r/b tube, must be credited with initiating manufacturers’ efforts to teach laboratory staffs the vagaries and problems of new system approaches. Shortly thereafter, the API system was introduced in the United States, bringing a novel numerical approach first to the identification of Enterobacteriaceae (enteric – gut bacteria) and then to that of several other categories of microorganisms. Similarly, the Roche Enterotube used fewer reaction substrates to decrease the time needed to identify isolates to the species level; initially it was used for members of the Enterobacteriaceae and eventually for other microbial representatives. All systems eventually addressed yeasts and nutritionally demanding bacteria, obviating the multiple-tube approaches in use.
Clinical microbiologists are acutely aware of the constantly emerging intruders into the intimate human biosphere. These agents appear as the traditional scourges of humanity are brought under control. But the application of antimicrobial agents to the food chain, cosmetics, and over-the-counter medications, and the advances in medical science, sparing individuals afflicted with a variety of diseases but accompanied by impaired immunity—all these factors have combined to increase nosocomial infections, placing the medical facility at the very apex of the selective-pressure pyramid. The selection results in colonization by microbiota with a minority of antimicrobial-tolerant or -resistant constituents; administration of antimicrobial therapy converts these organisms to a majority. These selected prokaryotes and eukaryotes,
along with the emerging viruses, coccidia, yeasts, and molds, pose a dynamic challenge to the clinical microbiologist and promise a continued need for her or his services. But these challenges must be met by the expansion of technical skills brought to bear on the changing nature of the challenging microbiota and the willingness of clinical microbiologists
to adopt and practice evolving technologies, to gain knowledge in addition to information, and to remain in the forefront of innovation and invention.
Gut microbiota: next frontier in understanding human health and development of biotherapeutics
Satya Prakash, L Rodes, M Coussa-Charley, C Tomaro-Duchesneau
Biologics: Targets and Therapy 2011:5 71–86
http://dx.doi.org/10.2147/BTT.S19099
The human gastrointestinal tract houses a huge microbial ecosystem, the gut microbiota. This intestinal ecosystem is partially responsible for maintaining human health. However, particular changes in the ecosystem might contribute to the development of certain diseases. With this in mind, there is a need for an exhaustive review on the functions of the gut microbiota, occurrence of gut dysbiosis (alteration of the microbiota), mechanisms by which intestinal bacteria can trigger development of disease, how this ecosystem can be exploited for understanding human health, development of biotherapeutics, expert opinion on current biotherapeutics, and future perspectives. This review presents a descriptive and comprehensive analysis on “the good, the bad, and the ugly” of the gut microbiota, and methods to study these and their modulation of human health.
The gut microbiota is a remarkable asset for human health. As a key element in the development and prevention of specific diseases, its study has yielded a new field of promising biotherapeutics. This review provides comprehensive and updated knowledge of the human gut microbiota, its implications in health and disease, and the potentials and limitations of its modification by currently available biotherapeutics to treat, prevent and/ or restore human health, and future directions. Homeostasis of the gut microbiota maintains various functions which are vital to the maintenance of human health. Disruption of the intestinal ecosystem equilibrium (gut dysbiosis) is associated with a plethora of human diseases, including autoimmune and allergic diseases, colorectal cancer, metabolic diseases,
and bacterial infections. Relevant underlying mechanisms by which specific intestinal bacteria populations might trigger the development of disease in susceptible hosts are being explored across the globe. Beneficial modulation of the gut microbiota using biotherapeutics, such as prebiotics, probiotics, and antibiotics, may favor health-promoting populations of bacteria and can be exploited in development of biotherapeutics. Other technologies, such as development of human gut models, bacterial screening, and delivery formulations e.g., microencapsulated probiotics, may contribute significantly in the near future. Therefore, the human gut microbiota is a legitimate therapeutic target to treat and/or prevent various diseases. Development of a clear understanding of the technologies needed to exploit the gut microbiota is urgently required.
Seven bacterial divisions constitute the gut microbiota, i.e., Firmicutes, Bacteroides, Proteobacteria, Fusobacteria, Verrucomicrobia, Cyanobacteria, and Actinobacteria, with Firmicutes and Bacteroides being the most abundant species. Bacterial communities exhibit quantitative and qualitative variations along the length of the gastrointestinal tract due to host factors (e.g., pH, transit time, bile acids, digestive enzymes, and mucus), nonhost factors (eg, nutrients, medication, and environmental factors), and bacterial factors (e.g., adhesion capacity, enzymes, and metabolic capacity).
Until recently, the analysis of bacterial ecosystems was performed by growth on defined media, which has some limitations because this method is labor-intensive and, more importantly, only 80% of stool bacteria can be cultivated. As a consequence, new molecular techniques have been developed. In terms of qualitative measurements of the microbiota, techniques such as fingerprinting (denaturing gradient gel electrophoresis), terminal restriction fragment length polymorphism, ribosomal intergenic spacer analysis, and 16S ribosomal RNA sequencing are widely used. Specifically, genome sequencing has provided tremendous information in the microbial world, spearheading technologies such as microarrays. New automated parallel sequencing technologies, based on the 16S ribosomal RNA gene present in all prokaryotes, can offer a cost-effective solution for rapid sequencing and identification of bacterial species of the gut.
Essential metabolic functions
Metabolic functions of the gut microbiota include production of vitamin, amino acid synthesis, and bile acid biotransformation. Bile acid biotransformations, performed by microbial enzymes, have implications for cholesterol and glucose metabolism. Importantly, the microbiome provides biochemical pathways required for the fermentation of nondigestible substrates and endogenous mucus. Through fermentation, bacterial growth is stimulated, producing short-chain fatty acids and gases. The major short-chain fatty acids produced are acetate, butyrate, and propionate. Other bacterial end products include lactate, ethanol, succinate, formate, valerate, caproate, isobutyrate, 2-methyl-butyrate,
and isovalerate. Bacterial fermentation is present in the cecum and colon, where the short-chain fatty acids are absorbed, stimulating the absorption of salts and water.
Ensures protection
Pathogen displacement or “colonization resistance” is an accepted function of the gut microbiota. Commensal organisms prevent pathogenic colonization by competing for attachment sites and nutrients, and also through the production and secretion of antimicrobials. Those mechanisms are relevant for reducing the level of lipopolysaccharides, peptidoglycans, bacterial CpG-DNA motifs, and superantigens, which can all be detrimental to the host. The indigenous microbiota is also essential for development of the immune system. Short-chain fatty acids, such as butyrate, may exert potent immunomodulatory effects by suppressing nuclear factor-kB activation and/or by acting on G-coupled receptors, as demonstrated with acetate. These concepts illustrate a dynamic relationship between the immune system and the microbiota. The intestinal mucosa averts threats by signaling to the innate immune system through pattern recognition receptors, such as toll-like receptors. Pattern recognition receptors recognize and bind to specific microbial macromolecules, referred to as microbial-associated molecular patterns. These include lipopolysaccharide, flagellin, peptidoglycan, and N-formylated peptides.
Structural and histological function
The microbiota ensures intestinal structure and function. Firstly, the mucus layer, which reflects the balance between mucus secretion and bacterial degradation, constitutes an obstacle to the uptake of antigens and proinflammatory molecules. Secondly, some bacterial communities may strengthen the barrier at the level of the tight junctions, ie, protein clusters that form a barrier between the lumen and the lamina propria. Moreover, the gut microbiota is involved in cell and tissue development. Butyrate regulates cell growth and differentiation, inhibiting transformed cell growth while encouraging reversion of cells from a neoplastic to a non-neoplastic phenotype. Most of the structural and morphological development of the gut contributes to and manages the gut bacterial system.
Dysbiosis is a state in which the microbiota becomes altered as a consequence of an alteration in the composition of the microbiota, a change in bacterial metabolic activity, and/or a shift in local distribution of communities. Many factors can alter the gastrointestinal ecosystem, including antibiotics, psychological and physical stresses, radiation, altered peristalsis, and dietary changes. At present, the focus is on the description of dysbiosis in a plethora of human disorders.
Autoimmune diseases occur when the body’s immune system attacks and destroys healthy cells and tissues, as is the case in type 1 diabetes mellitus, celiac disease, inflammatory bowel diseases, and allergic asthma. Most often, the immune response is initiated by unknown factors. Alteration of the gut microbiota as a result of modern lifestyles is an attractive hypothesis to explain the rise in prevalence of celiac disease, type 1 diabetes mellitus, and inflammatory bowel diseases.
Celiac disease is an inflammatory disease of the small intestine that is triggered and maintained by the storage proteins of wheat, barley, and rye. Studies have investigated the composition of the microbiota in patients with celiac disease. Fecal samples from patients with celiac disease had reduced the proportions of Bifidobacterium, Clostridium histolyticum, Clostridium lituseburense, Faecalibacterium prausnitzii, and increased proportions of Bacteroides/Prevotella.
Type 1 diabetes mellitus, characterized by insulin deficiency resulting from immune-mediated destruction of pancreatic β cells, is thought to be triggered by environmental factors in genetically susceptible individuals. Given that antibiotics prevented type 1 diabetes mellitus in biobreeding diabetes-prone rats and in nonobese diabetic mice, alteration of the microbiota has been associated with progression of type 1 diabetes mellitus. Evidence shows that bacterial communities from biobreeding diabetes-prone and diabetes-resistant rats differ, marked by a higher abundance of Lactobacillus and Bifidobacterium in diabetes-resistant rats.
Inflammatory bowel diseases include ulcerative colitis and Crohn’s disease. Crohn’s disease is characterized by patchy and transmural inflammation that may affect any part of the gastrointestinal tract, while ulcerative colitis is a chronic episodic inflammatory condition that involves only the large bowel. There is evidence that species belonging to the normal gut microbiota are involved in the etiology and/or maintenance of inflammatory processes. Reduced microbial diversity, increased Bacteroidetes and Enterobacteriaceae, and decreased Firmicutes were all observed in patients with inflammatory bowel diseases.
Irritable bowel syndrome is characterized by abdominal pain, bloating, and changes in bowel habit, in the absence of any overt mucosal abnormality. Observations have directed attention towards the gut microbiota, identifying a postinfectious variant of the syndrome, ie, evidence that antibiotics induced a reduction in the microbiota which may be a risk factor, and the proposal that some patients may have bacterial overgrowth in the small bowel.49 Studies have demonstrated that patients with irritable bowel syndrome have fewer intestinal Bifidobacteria, Collinsella aerofaciens, Coprococcus eutactus, and Clostridium cocleatum, and an increase in Veillonella and Enterobacteriaeae.
It is well established that a disruption in the commensal microbiota increases susceptibility to enteric infections. Antibiotic-treated mice are particularly useful for studying colitis induced by Salmonella spp, Shigella spp, and E. coli infections. In addition, in murine Citrobacter rodentium infections, pathogen colonization is associated with a reduced total density and a relative increase in γ-Proteobacteria. Furthermore, elderly patients with C. difficile-associated diarrhea demonstrate reduced numbers of Bacteroides, Prevotella, and Bifidobacteria, and a greater diversity of facultative species, ie, Lactobacilli and Clostridia. The evidence suggests an association between disruption of the gut microbiota and bacterial infections, further accentuating the dysbiosis.
Altered composition of the human gastrointestinal ecosystem can lead to physiological changes in the intestinal environment, disrupting the functions of the microbiota and having serious consequences for human health.
- Altered gut microbiota may trigger serious immune deregulation
- Specific gut dysbiosis can engender metabolic endotoxemia
- Bacterial infection might be promoted by gut dysbiosis
- Abnormal bacterial metabolite levels may trigger cancer
An altered microbial balance in the gut can lead to A) an increase in immune mediated disorders and B) chronic low-grade inflammation.
A mechanism based on the triggering of the host’s immune defenses was elucidated using models of C. rodentium (mimicking diarrheal pathogen associated inflammation), Campylobacter jejuni infection, and chemically and genetically induced models of intestinal inflammation are used for altered microbiota investigations. An overgrowth of Enterobacteriaceae was observed in all models, indicating that inflammation induced microbiota changes support colonization by aerotolerant bacteria.
Many etiological bacterial mechanisms have been hypothesized to promote carcinogenesis. Amongst those, hydrogen sulfide, a product of bacterial sulfate reduction, appears to be linked to the incidence of chronic disorders, such as ulcerative colitis and colorectal cancer. Because DNA strand breaks are associated with mutation and promotion of carcinogenesis, bacterial hydrogen sulfide may be responsible for the induction of mutations in the development of sporadic colorectal cancer.
- Gut microbiota alters energy and lipid metabolism
Reared mice have more body and gonadal fat than germ-free mice, despite reduced chow consumption. The increase in fat was accompanied with increased fasting glucose and insulin levels and an insulin-resistant state.
– Prebiotics
Prebiotics are “nondigestible food ingredients that beneficially affect the host by selectively stimulating the growth and/or the activity of one or a limited number of bacteria in the colon, and thus improves host health”. A prebiotic should not be hydrolyzed by human intestinal enzymes, but selectively fermented by bacteria, benefiting the host.
The relationship between health and the gastrointestinal system is established. Due to the inherent plasticity of microbiota, one can consider exploiting it to develop biotherapeutics.
Gut Microbiota Regulates Bile Acid Metabolism by Reducing the Levels of Tauro-beta-muricholic Acid, a Naturally Occurring FXR Antagonist
Sama I. Sayin, Annika Wahlstrom, Jenny Felin, Sirkku Jantti, et al.
Cell Metabolism Feb 5, 2013; 17, 225–235
http://dx.doi.org/10.1016/j.cmet.2013.01.003
Bile acids are synthesized from cholesterol in the liver and further metabolized by the gut microbiota into secondary bile acids. Bile acid synthesis is under negative feedback control through activation of the nuclear receptor farnesoid X receptor (FXR) in the ileum and liver. Here we profiled the bile acid composition throughout the enterohepatic system in germfree (GF) and conventionally raised (CONV-R) mice.
We confirmed a dramatic reduction in muricholic acid, but not cholic acid, levels in CONV-R mice. Rederivation of Fxr-deficient mice as GF demonstrated that the gut microbiota regulated expression of fibroblast growth factor 15 in the ileum and cholesterol 7α-hydroxylase (CYP7A1) in the liver by FXR-dependent mechanisms. Importantly, we identified tauroconjugated β- and α-muricholic acids as FXR antagonists. These studies suggest that the gut microbiota not only regulates secondary bile acid metabolism but also inhibits bile acid synthesis in the liver by alleviating FXR inhibition in the ileum.
Diet rapidly and reproducibly alters the human gut microbiome.
Lawrence A David, Corinne F Maurice, Rachel N Carmody, et al.
Nature 12/2013; http://dx.doi.org:/10.1038/nature12820
Long-term dietary intake influences the structure and activity of the trillions of microorganisms residing in the human gut, but it remains unclear how rapidly and reproducibly the human gut microbiome responds to short-term macronutrient change. Here we show that the short-term consumption of diets composed entirely of animal or plant products alters microbial community structure and overwhelms inter-individual differences in microbial gene expression. The animal-based diet increased the abundance of bile-tolerant microorganisms (Alistipes, Bilophila and Bacteroides) and decreased the levels of Firmicutes that metabolize dietary plant polysaccharides (Roseburia, Eubacterium rectale and Ruminococcus bromii). Microbial activity mirrored differences between herbivorous and carnivorous mammals, reflecting trade-offs between carbohydrate and protein fermentation. Foodborne microbes from both diets transiently colonized the gut, including bacteria, fungi and even viruses. Finally, increases in the abundance and activity of Bilophila wadsworthia on the animal-based diet support a link between dietary fat, bile acids and the outgrowth of microorganisms capable of triggering inflammatory bowel disease. In concert, these results demonstrate that the gut microbiome can rapidly respond to altered diet, potentially facilitating the diversity of human dietary lifestyles
Honing in on enteric fever
Lyle R Mckinnon And Quarraisha Abdool Karim
eLife 2014;3:e03545. http://dx.doi.org:/10.7554/eLife.03545
Enteric fever, also known as typhoid, is a disease that affects about 22 million people and causes about 200,000 deaths every year, according to conservative estimates. Enteric fever is spread by bacteria belonging to the Salmonella genus, with two sub-species—Salmonella Typhi and Salmonella Paratyphi A—being responsible for most cases of the disease. And although the number of cases of enteric fever has fallen significantly over recent decades, there is a clear need for a diagnostic test for Salmonella that is rapid, affordable and accurate. Moreover, it is important to be able to distinguish between enteric fever caused by Salmonella Typhi and enteric fever caused by Salmonella Paratyphi A in order to ensure that the correct drugs are prescribed and to combat the development of antibiotic resistance.
The application of metabolomics is relatively new in infectious diseases research compared to the application of genomics and proteomics. Despite this, screening the metabolome in blood plasma has identified useful prognostic profiles of several diseases, including sepsis. Using a combination of gas chromatography and mass spectrometry, Näsström et al. identified 695 distinct peaks that were associated with different metabolites: from these they selected six peaks that had significantly different heights in the three groups of patients. This meant that they were able to tell if the patient had S. Typhi, S. Paratyphi A, or neither. That this mass spectrometric analysis was able to distinguish two Salmonella groups that share many similarities is remarkable. Moreover, in addition to its diagnostic potential, this new approach might also provide insights into the antigenic and physiological differences between the two strains.
http://emedicine.medscape.com/article/186458-overview
Clostridium difficile colitis results from a disturbance of the normal bacterial flora of the colon, colonization by C difficile, and the release of toxins that cause mucosal inflammation and damage. Antibiotic therapy is the key factor that alters the colonic flora. C difficile infection (CDI) occurs primarily in hospitalized patients.
Essential update: CDC promotes improving inpatient antibiotic prescribing to reduce drug resistance and increase patient safety In a CDC analysis of data regarding antibiotic prescribing in hospitalized patients, Fridkin and colleagues estimated that a 30% reduction in use of broad-spectrum antibiotics would result in a 26% reduction in C difficile infections (CDIs).[1, 2] In addition, improvement in physician antibiotic prescribing habits from overuse and incorrect use would also help to reduce antibiotic resistance.
The authors recommend the following[2] :
Promptly initiate antibiotics for a presumed infection, but first obtain any recommended cultures.
Document and specify the drug’s indication, dose, and expected duration of use in the patient’s medical chart.
Reassess the patient within 48 hours based on test results and patient examination; adjust the antibiotic regimen (dose, duration) and/or the agent, or end the antibiotic treatment, as needed.
Signs and symptoms
Symptoms of C difficile colitis often include the following:
Mild to moderate watery diarrhea that is rarely bloody
Cramping abdominal pain
Anorexia
Malaise
Physical examination may reveal the following in patients with the disorder:
Fever: Especially in more severe cases
Dehydration
Lower abdominal tenderness
Rebound tenderness: Raises the possibility of colonic perforation and peritonitis
Regulatory T-cells in autoimmune diseases: Challenges, controversies and—yet—unanswered questions
Charlotte R. Grant, Rodrigo Liberal, Giorgina Mieli-Vergani, et al.
Autoimmunity Reviews 14 (2015) 105–116
http://dx.doi.org/10.1016/j.autrev.2014.10.012
Regulatory T cells (Tregs) are central to the maintenance of self-tolerance and tissue homeostasis. Markers commonly used to define human Tregs in the research setting include high expression of CD25, FOXP3 positivity and low expression/negativity for CD127. Many other markers have been proposed, but none unequivocally identifies bona fide Tregs. Tregs are equipped with an array of mechanisms of suppression, including the modulation of antigen presenting cell maturation and function, the killing of target cells, the disruption of metabolic pathways and the production of anti-inflammatory cytokines. Treg impairment has been reported in a number of human autoimmune conditions and includes Treg numerical and functional defects and conversion into effector cells in response to inflammation. In addition to intrinsic Treg impairment, resistance of effector T cells to Treg control has been described. Discrepancies in the literature are common, reflecting differences in the choice of study participants and the technical challenges associated with investigating this cell population. Studies differ in terms of the methodology used to define and isolate putative regulatory cells and to assess their suppressive function. In this review we outline studies describing Treg frequency and suppressive function in systemic and organ specific autoimmune diseases, with a specific focus on the challenges faced when investigating Tregs in these conditions.
Role of dendritic cells in the initiation, progress and modulation of systemic autoimmune diseases
Juan Pablo Mackern-Oberti, Carolina Llanos, Fabián Vega, et al.
Autoimmunity Reviews 14 (2015) 127–139
http://dx.doi.org/10.1016/j.autrev.2014.10.010
Dendritic cells (DCs) play a key role in the activation of the immune response against pathogens, as well as in the modulation of peripheral tolerance to self-antigens (Ags). Furthermore, an imbalance in the activating/inhibitory receptors expressed on the surface of DCs has been linked to increased susceptibility to develop autoimmune diseases underscoring their immunogenicity potential. It has been described that modulation of activating or inhibitory molecules expressed by DCs, such as CD86, TLRs, PDL-1 and FcγRs, can define the immunogenic phenotype. On the other hand, T cell tolerance can be achieved by tolerogenic DCs, which have the capacity of blocking undesired autoimmune responses in several experimental models, mainly by inducing T cell anergy, expansion of regulatory T cells and limiting B cell responses. Due to the lack of specific therapies to treat autoimmune disorders and the tolerogenic capacity of DCs shown in experimental autoimmune disease models, autologous tol-DCs are a potential therapeutic strategy for fine-tuning the immune system and reestablishing tolerance in human autoimmune diseases. New advances in the role of DCs in systemic lupus erythematosus (SLE) pathogenesis and the identification of pathogenic self-Ags may favor the development of novel tol-DC based therapies with amajor clinical impact. In this review, we discuss recent data relative to the role of DCs in systemic autoimmune pathogenesis and their use as a therapy to restore tolerance.
T cell subsets and their signature cytokines in autoimmune and inflammatory diseases
Itay Raphael, Saisha Nalawade, Todd N. Eagar, Thomas G. Forsthuber
Cytokine xxx (2014) xxx–xxx
http://dx.doi.org/10.1016/j.cyto.2014.09.011
CD4+ T helper (Th) cells are critical for proper immune cell homeostasis and host defense, but are also major contributors to pathology of autoimmune and inflammatory diseases. Since the discovery of the Th1/Th2 dichotomy, many additional Th subsets were discovered, each with a unique cytokine profile, functional properties, and presumed role in autoimmune tissue pathology. This includes Th1, Th2, Th17, Th22, Th9, and Treg cells which are characterized by specific cytokine profiles. Cytokines produced by these Th subsets play a critical role in immune cell differentiation, effector subset commitment, and in directing the effector response. Cytokines are often categorized into proinflammatory and anti-inflammatory cytokines and linked to Th subsets expressing them. This article reviews the different Th subsets in terms of cytokine profiles, how these cytokines influence and shape the immune response, and their relative roles in promoting pathology in autoimmune and inflammatory diseases. Furthermore, we will discuss whether Th cell pathogenicity can be defined solely based on their cytokine profiles and whether rigid definition of a Th cell subset by its cytokine profile is helpful.
Irritable Bowel Syndrome and Gluten Sensitivity Without Celiac Disease: Separating the Wheat from the Chaff
Biesiekierski JR, Newnham ED, Irving PM, et al. Gluten causes gastrointestinal symptoms in subjects without celiac disease: a double-blind randomized placebo controlled trial. Am J Gastroenterol 2011;106:508–514.
Courtney C. Ferch, William D. Chey
Gastroenterology 2012; 142:664–673
Over the past several years, there has been increasing discussion concerning the topic of gluten sensitivity as a cause of irritable bowel syndrome (IBS) symptoms in patients for whom celiac disease has been excluded. Biesiekierski et al performed a double-blind, placebo-controlled, dietary rechallenge trial to better understand the role of gluten ingestion in the development of gastrointestinal (GI) and non-GI symptoms in patients diagnosed with IBS. This study included a sample of 34 patients diagnosed with IBS by the Rome III criteria who had experienced symptom improvement with a gluten-free diet for 6 weeks before study enrollment. Celiac disease had been excluded in all study participants by either a negative HLADQ2/HLA-DQ8 haplotype or a normal duodenal biopsy. Patients with potentially important confounders such as cirrhosis, inflammatory bowel disease, nonsteroidal anti-inflammatory drug ingestion, or excessive alcohol use were excluded from the study.
Upon completion of the study period, it was found that a significantly greater proportion of patients in the gluten group compared with the gluten-free group answered “no” to the primary outcome question (68% vs 40%; P < .001). Compared with the gluten group, those who remained gluten free also reported significant improvements in pain (P < .016), bloating (P < .031), satisfaction with stool consistency (P <.024), and tiredness (P < .001), but showed no significant differences in wind (P < .053) or nausea (P < .69). The results of celiac antibodies at baseline and after the dietary intervention were similar. Intestinal permeability as measured by urine lactulose-to-rhamnose ratio was also unchanged by the dietary intervention. Fecal lactoferrin levels were persistently undetectable in all but 1 patient during the treatment period. High-sensitivity C-reactive protein levels remained normal before and after the dietary intervention. There were no differences in the likelihood of symptomatic response in those with and without HLA-DQ2 and HLA-DQ8 alleles, arguing against undiagnosed celiac disease as a cause for symptom response to a gluten-free diet.
The authors felt that these data support the existence of non–celiac-associated gluten sensitivity. They concluded that gluten is indeed associated with overall IBS symptoms, bloating, dissatisfaction with stool consistency, abdominal pain, and fatigue in a subset of patients.
A recent meta-analyses of studies from around the world found that patients with IBS symptoms were significantly more likely to have celiac disease than controls. (Arch Intern Med 2009;169:65165– 65168). As such, the American College of Gastroenterology Task Force has recommended that routine serologic screening for celiac sprue be pursued in patients with diarrhea-predominant IBS and IBS with a mixed bowel pattern (grade 1B recommendation; Am J Gastroenterol 2009;104[Suppl 1]:S1–S35). Although much of the recent discussion around the potential role of food in IBS symptoms has focused on celiac disease, it is important to note that data from the available US studies have not shown a significantly greater risk for celiac disease among patients with IBS symptoms and no warning signs (Am J Gastroenterol 2008;103[Suppl 1]:S472; Gastroenterology 2011;141:1187–1193). A recent prospective study from the United States reported a 0.4% prevalence of biopsy-proven celiac disease in 492 patients with IBS symptoms and 458 asymptomatic persons undergoing colonoscopy for colorectal cancer screening or surveillance (Gastroenterology 2011;141:1187–1193). Although not significantly different, it is interesting that 7.3% of the IBS group and 4.8% of controls had 1 abnormal celiac serology test result (adjusted odds ratio, 1.49; 95% confidence interval, 0.76 – 0.90; P =.25). Thus, this study suggests that the likelihood of an abnormal immunologic response to gluten is orders of magnitude more common than biopsy-proven celiac disease in IBS patients and controls from the United States. It has been suggested that ~20% of the general population reports symptoms in association with the ingestion of gluten. Such patients have been said to suffer from “gluten sensitivity.”
It is also interesting to consider the potential effects of food on gut immune function beyond celiac disease. There is emerging evidence to suggest that immune activation and/or low-grade inflammation may play a role in the pathogenesis of IBS (GI Clin North Am 2011;40:65–85). The data are currently conflicting, but alternations in the number of mast cells in close proximity to afferent neurons, mucosal lymphocytes, and certain pro-inflammatory or anti-inflammatory cytokines have been identified in a subset of patients with IBS. It is not difficult to envision that alterations in the gut immune system could occur as a consequence of an acute GI infection in a genetically susceptible individual. However, it is interesting to speculate that other environmental factors, such as an altered gut microbiota, physical or emotional abuse, stress, or food, might result in abnormal gut immune function translating clinically into IBS symptoms.
A better understanding of how differences in gut immune function, the microbiome, and fermentation might influence the development of IBS symptoms in association with the ingestion of gluten are all deserving of further investigation. The study by Biesiekierski et al is the first randomized, controlled trial to suggest that nonceliac IBS patients might benefit from a gluten-free diet. Although these results are certainly intriguing and hypothesis generating, they require validation in larger, randomized, controlled trials in other parts of the world. What is clear and important for providers to understand is that gluten sensitivity is here to stay and significantly more likely for them to encounter in day-to-day practice than celiac disease.
No Effects of Gluten in Patients With Self-Reported Non-Celiac Gluten Sensitivity After Dietary Reduction of Fermentable, Poorly Absorbed, Short-Chain Carbohydrates
Jessica R. Biesiekierski, Simone L. Peters, Evan D. Newnham, et al.
Gastroenterology 2013;145:320–328
http://dx.doi.org/10.1053/j.gastro.2013.04.051
Background & Aims: Patients with non-celiac gluten sensitivity (NCGS) do not have celiac disease but their symptoms improve when they are placed on gluten-free diets. We investigated the specific effects of gluten after dietary reduction of fermentable, poorly absorbed, short-chain carbohydrates (fermentable, oligo-, di-, monosaccharides, and polyols [FODMAPs]) in subjects believed to have NCGS. Methods: We performed a double-blind crossover trial of 37 subjects (aged 2461 y, 6 men) with NCGS and irritable bowel syndrome (based on Rome III criteria), but not celiac disease. Participants were randomly assigned to groups given a 2-week diet of reduced FODMAPs, and were then placed on high-gluten (16 g gluten/d), low-gluten (2 g gluten/d and 14 g whey protein/d), or control (16 g whey protein/d) diets for 1 week, followed by a washout period of at least 2 weeks. We assessed serum and fecal markers of intestinal inflammation/injury and immune activation, and indices of fatigue. Twenty-two participants then crossed over to groups given gluten (16 g/d), whey (16 g/d), or control (no additional protein) diets for 3 days. Symptoms were evaluated by visual analogue scales. Results: In all participants, gastrointestinal symptoms consistently and significantly improved during reduced FODMAP intake, but significantly worsened to a similar degree when their diets included gluten or whey protein. Gluten-specific effects were observed in only 8% of participants. There were no diet-specific changes in any biomarker. During the 3-day rechallenge, participants’ symptoms increased by similar levels among groups. Gluten-specific gastrointestinal effects were not reproduced. An order effect was observed. Conclusions: In a placebo controlled, cross-over rechallenge study, we found no evidence of specific or dose-dependent effects of gluten in patients with NCGS placed diets low in FODMAPs. www.anzctr.org.au.ACTRN12610000524099
Infection, inflammation, and the irritable bowel syndrome
Spiller, K. Garsed
Digestive and Liver Disease 41 (2009) 844–849
http://dx.doi.org:/10.1016/j.dld.2009.07.007
Infectious diarrhea is one of the commonest afflictions of mankind. Worldwide most of the burden, about 1 billion cases a year, is seen in children <5 years old, the vast majority in the developing world in communities where access to clean water and adequate sanitation is restricted. Here a child can expect to have 6–7 episodes per year compared to 1–2 in the developed world. Following recovery from an episode of gastroenteritis (GE) the vast majority of healthy adults and children develop some degree of immunity to the organism responsible and return to normal functioning. However 7–31% develop post-infectious irritable bowel syndrome (PI-IBS). The proportion of unselected IBS that is post-infectious varies from 6 to 17% in the USA and Europe but whether this differs in the developing world is unknown, though previous enteric infection is a known risk factor for IBS in Southern China.
This review will compare the epidemiology of infectious diarrhea in the developing and developed world and the link between mucosal inflammation and the development of IBS symptoms. The available evidence suggests that the acquisition of immunity in early childhood reduces the severity of subsequent gastroenteritis in adulthood. Since these are known risk factor for developing PI-IBS we hypothesize that this may underlie some of the regional differences in the incidence of both infection and IBS.
Gastrointestinal infection is ubiquitous worldwide though the pattern of infection varies widely. Poor hygiene and lack of piped water is associated with a high incidence of childhood infection, both viral and bacterial. However in developed countries bacterial infection is commoner in young adults. Studies of bacterial infections in developed countries suggest 75% of adults fully recover, however around 25% have long lasting changes in bowel habit and a smaller number develop the irritable bowel syndrome (IBS). Whether the incidence is similar in developing countries is unknown. Post-infective IBS (PI-IBS) shares many features with unselected IBS but by having a defined onset allows better definition of risk factors. These are in order of importance: severity of initial illness, smoking, female gender and adverse psychological factors. Symptoms may last many years for reasons which are unclear. They are likely to include genetic factors controlling the immune response, alterations in serotonin signaling, low grade mucosal inflammation maintained by psychological stressors and alterations in gut microbiota. As yet there are no proven specific treatments, though 5HT3 receptor antagonists, anti-inflammatory agents and probiotics are all logical treatments which should be examined in large well-designed randomized placebo controlled trials.
There are three key questions. Firstly is the incidence of IBS less in the developing world, secondly is the incidence increasing with the adoption of a western urban life style and finally is the disease itself different? The answer to all three is probably yes though interpretation of cross-cultural surveys is fraught with problems relating to the imprecise translation of questions into different cultures. Initial reports from small uncontrolled studies suggested that IBS was very uncommon and predominantly affected a subpopulation who pursued a “western life style”. More recent and robust work gives a range of values for prevalence from very low in Iran and India with just 5.8 and 4.2% respectively, to values in developed Asian countries that are generally lower but not dissimilar to those seen in the west. The key factors associated with rapid westernization that underlie this increase in numbers is unclear but could include the effect of improved hygiene, increased overcrowding, stress and changes in diet. The best evidence comes from studies in which the same populations have been studied over a number of years as has been done in Singapore where after a decade of steady industrial growth the prevalence of IBS has risen from 2.3% to 8.6%.
This raises is a most important question – why should these differences occur? It is clear that major differences in the epidemiology of gut infection exist between the west and the developing world. This is illustrated by Campylobacter jejuni enteritis, which causes a shorter, less severe illness in childhood than in adulthood, which is when most Europeans and North Americans are infected. The greater degree of inflammation which adults experience may increase the risk of developing subsequent PI-IBS which might partly account for the higher prevalence of IBS in the westernized nations.
Worldwide the average number of episodes of infection annually per person is 3. A poorly nourished child living in cramped conditions without access to sewerage and running water will have 8 or more infections in the first year of life, most frequently with enteric bacteria and parasites whereas a child in better sanitary conditions would have less infections and these would be more likely to be viral in origin. Even in England an estimated 1 in 5 people per year have an episode of diarrhea in the community adding up to 9.4 million cases in total a year, largely unreported since only 1 in 30 present to their doctor. It seems here that viral infections predominate in the very young, with bacterial infection particularly Campylobacter spp. being most common in adolescence and early adulthood. PCR analysis of stool in the same study showed that Norovirus and Rotavirus were the commonest pathogens detected across all age groups. Campylobacter spp. were most commonly found in age group 30–39 (16% compared to 6.7% of those aged 1–4).
Infectious diarrhea results from either an increase in fluid and electrolyte secretion, predominantly in the small intestine, or a decrease in absorption which can involve both the small and large bowel. During a diarrheal illness these two mechanisms frequently co-exist. Enterotoxins from Vibrio cholerae or enterotoxigenic E. coli induce profuse secretion while decreased intestinal absorption can be induced by mucosal injury caused by enteroinvasive organisms (e.g., Salmonella, Shigella, and Yersinia spp.). These invasive infections injure cells and excite an immune response and activate enteric nerves and mast cells resulting in an acute inflammatory infiltrate with the release of pro-inflammatory mediators and stimulation of secretion. Clinically the patient will have an acutely inflamed mucosa with ulceration and bleeding.
Campylobacter jejuni produces a range of toxins including cytolethal distending toxin, that first produces a secretory diarrhea in the small intestine in the early part of the illness after which there is invasion of the distal ileum and colon to produce an inflammatory ileocolitis, which can extend all the way to the rectum. The disease is less severe in developing countries than in developed countries, with watery stool, fever, abdominal pain, vomiting and dehydration predominating as opposed to the severe abdominal pain, weight loss, fever and bloody stool that is seen more frequently in infections in the west. Infants usually have milder disease with less fever and pain, which in some cases is due to immunity acquired during previous infection. The reasons for these differences between the developed and developing world are unclear.
The composition of the resident intestinal microbiota is highly variable between individuals but relatively stable for each individual, though IBS patients showamore unstable microbiota. This instability may be due to antibiotic therapy or alterations in diet, both of which are commoner in IBS. Patients given antibiotics are 4 times more likely than untreated controls to report bowel symptoms 4 months later, and antibiotic use is a risk factor for developing IBS with an adjusted OR of 3.70 (1.80–7.60). Antibiotic use increases the incidence of post-infective functional diseases following both Salmonella enteritidis and travellers’ diarrhea, in whom antibiotic treatment gave a relative risk of developing PI-IBS of 4.1 (1.1–15.3) compared with those not receiving treatment.
During acute infectious diarrhea there is a decrease in anaerobes. Mice infected with Citrobacter rodentium or C. jejuni or subjected to a chemically induced colitis show significant reduction in the total numbers of microbiota, which is mainly due to activation of the host immune response and only to a much lesser degree by bacterial factors. This loss of anaerobes is associated with a depletion in short chain fatty acids and an increase in the pH of the stool allowing overgrowth of other organisms which may contribute to disturbed bowel function.
The study of patients with PI-IBS has yielded many new insights for several reasons. Firstly the patients are a more homogenous group than unselected IBS, most having diarrhea with fewer psychological problems than unselected IBS. Secondly the direction of causation is easier to ascertain as they represent a “natural experiment”, with subjects “randomized” to receive an infection, thus producing an unbiased study group. Finally onset of symptoms on a clearly defined date in a previously well patient provides an opportunity to examine the prior host and bacterial factors that predispose to developing IBS.
The severity of injury is mediated not only by factors related to the infecting organism but also by the host’s own immune response which develops in early life and declines in old age. However little is known about the incidence of PI-IBS in the pediatric population and whether it is different to the condition seen in adults. Functional bowel disorders are common in children, with IBS affecting 14% of high school and 6% of middle school patients in a US community study and are classified according to the main complaints made by parents or children rather than in an organ-specific way. This makes comparisons with the adult population difficult however a single recent study reports a very high incidence of postinfectious symptoms in 88 children with positive bacterial stool culture results presenting to a single institution. These had a 36% prevalence of functional gastrointestinal disorders compared to 11% in age- and sex-matched healthy controls. This is much higher than most adult studies with the exception of the Walkerton outbreak. Unlike adults, female gender is not a risk factor for PI-IBS in children suggesting the gender effect depends on hormonal and/or psychosocial factors rather than being genetic.
Despite uncertainty about PI-IBS in childhood we do know that age in adulthood does have an effect on the likelihood of developing PI-IBS. A meta-analysis indicates that patients who develop PI-IBS are slightly younger and one study showed increasing age was protective with age >60 years giving a relative risk of PI-IBS of 0.36 (0.1–0.09) though not all studies have shown this.
Why should this inflammation persist in some and not others? As we have already discussed adverse life events, anxiety and epression may play a part however less psychological morbidity is seen in PI-IBS than IBS indicating the presence of other factors which predispose to an exaggerated or prolonged inflammatory response. These factors might be genetic since a larger proportion of IBS patients have the high producing heterozygous TNF-α G/A polymorphism at position-308 than controls. Some PI-IBS patients were contained in this study but too few to examine as a subgroup. This study did not confirm an earlier finding of a decrease in the presumed immunoregulatory high IL-10 producing phenotype in IBS.
Although it is likely from animal work that infection does alter the gut microbiota there is no data on this in PI-IBS. There is some indirect evidence that altered microbiota may be important in IBS since fecal serine protease activity, which may be of bacterial origin, is increased in D-IBS. This is of great interest because these proteases can increase visceral sensitivity in rats, acting via the protease activated receptor-2 (PAR-2) group of receptors found in the mucosa and enteric nerves.
A recent small randomized placebo controlled trial of Mesalazine suggested this could reduce mast cell numbers and improve symptoms, a finding which needs repeating with larger numbers. Given the increase in 5HT availability and the effectiveness of 5HT3 receptor antagonists in animal studies and in unselected IBS-D patients a trial of a 5HT3 receptor antagonist would also be logical.
Gut motility and enteroendocrine secretion
Tongzhi Wu, Christopher K Rayner, Richard L Young and Michael Horowitz
Current Opinion in Pharmacology 2013, 13:928–934
http://dx.doi.org/10.1016/j.coph.2013.09.002
The motility of the gastrointestinal (GI) tract is modulated by complex neural and hormonal networks; the latter include gut peptides released from enteroendocrine cells during both the interdigestive and postprandial periods. Conversely, it is increasingly recognised that GI motility is an important determinant of gut hormone secretion, in that the transit of luminal contents influences the degree of nutrient stimulation of enteroendocrine cells in different gut regions, as well as the overall length of gut exposed to nutrient. Of particular interest is the relationship between gallbladder emptying and enteroendocrine secretion. The inter-relationships between GI motility and enteroendocrine secretion are central to blood glucose homeostasis, where an understanding is fundamental to the development of novel strategies for the management of diabetes mellitus.
Enteroendocrine cells account for release of more than 30 known peptides, including motilin and ghrelin during the interdigestive period, and cholecystokinin (CCK), glucose-dependent insulinotropic polypeptide (GIP), glucagon-like peptide-1 (GLP-1) and peptide YY (PYY) after meals. The latter are key mediators of the shift from an interdigestive to a postprandial GI motor pattern. Conversely, the delivery of luminal contents to be sensed by enteroendocrine cells in various gut regions is dependent on GI motor activity.
During the interdigestive period, both the stomach and small intestine undergo a cyclical motor pattern — the ‘migrating motor complex (MMC)’ — consisting of a quiescent phase (~40 min, phase I), a phase of irregular contraction (~50 min, phase II), and a period of maximum contraction (5–10 min, phase III). The MMC migrates from the stomach (or proximal small intestine) to the terminal ileum, and acts to sweep small intestinal contents (including bile, digestive juice and indigestible debris) towards the large intestine. Phase III of the MMC is also associated with spontaneous gallbladder emptying.
The cyclical occurrence of MMC activity during the interdigestive state closely parallels the secretion of motilin, and to a lesser degree, ghrelin. Increases in plasma motilin concentrations follow immediately each episode of spontaneous gallbladder emptying, while after phase III there is a decrease in motilin. The latter might be associated with the relative absence of luminal content due to the ‘house-keeping’ effect of phase III. Patients with gallstones have defective gallbladder emptying and lack the cyclical profile of motilin concentrations and exhibit a reduced frequency of phase III activity.
GI motility has a major impact on enteroendocrine secretion; conversely, enteroendocrine hormones play a pivotal role in the regulation of interdigestive and postprandial GI motility. The significance of these interrelationships is increasingly recognized as being central to the regulation of postprandial glycemia. Slowing gastric emptying and intestinal transit, accelerating gallbladder emptying and intestinal exposure to bile acids, and stimulating postprandial enteroendocrine hormones, all represent novel therapeutic approaches for the management of type 2 diabetes.
Enteroendocrine cell types revisited
Maja S Engelstoft, Kristoffer L Egerod, Mari L Lund and Thue W Schwartz
Current Opinion in Pharmacology 2013, 13:912–921
http://dx.doi.org/10.1016/j.coph.2013.09.018
The GI-tract is profoundly involved in the control of metabolism through peptide hormones secreted from enteroendocrine cells scattered throughout the gut mucosa. A large number of recently generated transgenic reporter mice have allowed for direct characterization of biochemical and cell biological properties of these previously highly elusive enteroendocrine cells. In particular the surprisingly broad co-expression of six functionally related hormones in the intestinal enteroendocrine cells indicates that it should be possible to control not only the hormone secretion but also the type and number of enteroendocrine cells. However, this will require a more deep understanding of the factors controlling differentiation, gene expression and specification of the enteroendocrine cells during their weekly renewal from progenitor cells in the crypts of the mucosa.
Go with the flow — membrane transport in the gut
Editorial overview, David T Thwaites
Current Opinion in Pharmacology 2013, 13:843–846
http://dx.doi.org/10.1016/j.coph.2013.09.019
The primary function of the gastrointestinal tract is the assimilation of nutrients from diet. The final stages of digestion and almost all absorption take place in the small intestine and, to a lesser extent, the large intestine. The intestinal epithelium is the single layer of polarized, differentiated cells that lines the wall of the intestine. It sits at the interface between the outside world and the internal environment of the human body. It is across this epithelial barrier that all essential nutrients, vitamins, electrolytes and fluid are absorbed. Many toxins and waste products can be secreted directly across the intestinal epithelium or excreted through the biliary route. The gastrointestinal tract is of great interest to the pharmacologist, and the pharmaceutical industry beyond, because most patients, if given the opportunity, would choose to take medication orally rather than have it delivered by any other route. In addition, many drugs and metabolites are lost from the body by active secretion from the intestine and liver. Thus, the intestinal epithelium is a major target for clinical intervention to improve bioavailability and modulate gut function.
To allow net transport in either the absorptive or secretory direction, the polarised cells in the small intestine (enterocytes), large intestine (colono-cytes) and liver (hepatocytes) express a distinct set of membrane transport proteins in their apical and basolateral membrane domains. Each epithelial cell type mediates net solute and ion movement through the coordinated activity of an array of membrane transport proteins (primary active transporters or pumps, secondary active cotransporters or antiporters, and channels).
Chloride channel-targeted therapy for secretory diarrheas
Jay R Thiagarajah and AS Verkman
Current Opinion in Pharmacology 2013, 13:888–894
http://dx.doi.org/10.1016/j.coph.2013.08.005
Secretory diarrheas caused by bacterial and viral enterotoxins remain a significant cause of morbidity and mortality. Enterocyte Cl– channels represent an attractive class of targets for diarrhea therapy, as they are the final, rate-limiting step in enterotoxin-induced fluid secretion in the intestine. Activation of cyclic nucleotide and/or Ca2+ signaling pathways in secretory diarrheas increases the conductance of Cl– channels at the enterocyte luminal membrane, which include the cystic fibrosis transmembrane conductance regulator (CFTR) and Ca2+-activated Cl– channels (CaCCs). High-throughput screens have yielded several chemical classes of small molecule CFTR and CaCC inhibitors that show efficacy in animal models of diarrheas. Natural-product diarrhea remedies with Cl– channel inhibition activity have also been identified, with one product recently receiving FDA approval for HIV-associated diarrhea.
The intestinal epithelium consists of villi and crypts, with absorption occurring mainly in villi and secretion in crypts. Fluid absorption in the small intestine is driven by the luminal Na+/H+ exchanger (NHE3), Na+-glucose cotransporter (SGLT1), and Cl–/HCO3– exchanger (DRA)(Figure 1, not shown). As in all epithelia the electrochemical driving force is established by a basolateral Na+K+-ATPase pump. The pro-absorptive solute transporters are constitutively active, though they can be modulated by second-messengers including cAMP and Ca2+. NHE3, SGLT1 and DRA are thus potential membrane transporter targets to increase intestinal fluid absorption. In the colon, fluid absorption is also facilitated by the epithelial Na+ channel (ENaC) and short-chain fatty acid (scfa) transporters (SMCT1).
Intestinal signal pathways controlling fluid secretion. Not shown. (a) Signaling pathways in CFTR activation by bacterial enterotoxins. Cholera toxin and heat stable enterotoxin (STa) bind to membrane receptors (GM1 —ganglioside receptor, guanylin receptor) causing increases in cyclic nucleotides (cAMP, cGMP) and neurotransmitters, resulting in CFTR activation. EC — enterochromaffin cells, 5-HT — 5-hydroxytryptamine, VIP — vasoactive intestinal peptide, ENS — enteric nervous system. (b) Signaling pathways in CaCC activation by rotavirus. Rotavirus releases NSP4 (non-structural protein 4), which causes elevation of cytoplasmic Ca2+ either: directly via binding to a membrane receptor (integrin α1β2); via neuropeptide galanin; or through activation of enteric nerves. Gal1-R — galanin 1 receptor. (c) Cross-talk between Ca2+ and cAMP pathways in intestinal epithelial cells. Epac — exchange protein directly activated by cAMP, PDE — phosphodiesterase, AC —adenylate cyclase, CaSR — calcium sensing receptor.
Natural-product ClS channel inhibitors Natural products have been identified with antidiarrheal efficacy in humans and a putative mechanism of action involving Cl– channel inhibition. Crofelemer, a heterogeneous proanthocyanidin oligomer extracted from the bark latex of South American tree Croton lechleri, was approved recently for HIV-associated diarrhea following clinical trials showing efficacy in reducing the number and severity of diarrhea episodes. Whether CaCC inhibition by crofelemer can explain its efficacy in HIV-associated diarrhea is unclear.
Following a natural product screen that identified tannic acid as a general CaCC inhibitor, we found that red wines containing polyphenolic gallotannins fully inhibited intestinal CaCC without effect on CFTR. In recent follow-up work, we generated an alcohol-free red wine extract with potent CaCC inhibition activity, and showed its efficacy in a neonatal mouse model of rotaviral diarrhea (unpublished data). The wine extract inhibited intestinal Ca2+-activated Cl– current and fluid secretion without affecting rotaviral infection of intestinal epithelial cells. CaCC inhibition may account for anecdotal reports of antidiarrheal action of red wines. Motivated by the possibility that known herbal antidiarrheal remedies might act by Cl– channel inhibition, we recently screened a selection of diarrhea remedies from sources worldwide and identified a commonly used Thai herbal remedy that fully inhibited both CFTR and CaCC (unpublished observations). The herbal remedy showed efficacy in mouse models of cholera and rotaviral diarrhea.
Clinical relevance of drug efflux pumps in the gut
Shingen Misaka, Fabian Muller and Martin F Fromm
Current Opinion in Pharmacology 2013, 13:847–852
http://dx.doi.org/10.1016/j.coph.2013.08.010
Important export pumps expressed in the apical membrane of enterocytes are P-glycoprotein (P-gp), breast cancer resistance protein (BCRP) and multidrug resistance protein 2 (MRP2). They are believed to be a crucial part of the bodies’ defense mechanisms against potentially toxic, orally administered xenobiotics. In particular P-gp and BCRP also limit the bioavailability of drugs. Inhibition of these intestinal export pumps by concomitantly administered drugs leads to increased plasma concentrations, whereas induction can reduce absorption of the substrate drugs and decrease plasma concentrations. The role of polymorphisms in genes encoding for these transporters will also be discussed. Taken together this review will focus on the role of intestinal export pumps using selected examples from clinical studies in humans.
P-gp (gene: ABCB1) is a protein consisting of two homologous halves, each containing six transmembrane helices and one nuclear-binding domain. The protein expression of P-gp has been shown to increase from proximal to distal parts of the intestine. P-gp generally tends to transport hydrophobic, amphipathic or cationic compounds. Clinically important P-gp substrates include anticancer agents, cardiovascular drugs and immunosuppressants. It is of note that most of the listed drugs are also substrates of CYP3A4, and thus intestinal P-gp and intestinal CYP3A4 efficiently collaborate to enhance the removal of their substrates. ABCB1 mRNA expression is regulated by several nuclear receptors such as pregnane X receptor (PXR), constitutive androstane receptor (CAR), thyroid hormone receptor and vitamin D receptor (VDR).
Human intestinal P-gp limits bioavailability of drugs and induction and inhibition of intestinal P-gp are important mechanisms underlying drug–drug interactions in humans. Direct evidence for these processes in humans was largely generated using studies in healthy volunteers, who received P-gp drug substrates with negligible drug metabolism such as digoxin and talinolol. Further work is required regarding the importance of intestinal P-gp for drug disposition and drug–drug interactions for the majority of P-gp substrates, which are also metabolized, for example, by intestinal and hepatic CYP3A4, since inducers or inhibitors of P-gp frequently also affect CYP3A4 expression or function. For intestinal BCRP and intestinal MRP2, so far only a limited number of examples with specific drugs exist, which indicate their clinical importance in humans.
Gastrointestinal HCO3– S transport and epithelial protection in the gut: new techniques, transport pathways and regulatory pathways
Ursula E Seidler
Current Opinion in Pharmacology 2013, 13:900–908
http://dx.doi.org/10.1016/j.coph.2013.10.001
The concept of a protective alkaline gastric and duodenal mucus layer is a century old, yet it is amazing how much new information on HCO3– transport pathways has emerged recently, made possible by the extensive utilization of gene deleted and transgenic mice and novel techniques to study HCO3– transport. This review highlights recent findings regarding the importance of HCO3– for mucosal protection of duodenum and other gastrointestinal epithelia against luminal acid and other damaging factors. Recently, methods have been developed to visualize HCO3– transport in vivo by assessing the surface pH in the mucus layer, as well as the epithelial pH. New information about HCO3– transport pathways, and emerging concepts about the intricate regulatory network that governs duodenal HCO3– secretion are described, and new perspectives for drug therapy discussed.
The lack of HCO3– ions in the pancreatic secretions of children with cystic fibrosis was recognized in the 1960s and the significance for impaired mucus release discussed. It is now evident that CFTR expression is essential for HCO3– secretion in most gastrointestinal epithelia, such as the esophagus, the small intestine, the biliary tract, and the pancreatic ducts, as well as the reproductive tract and the airways. The low pH in the acinar-ductal unit after release of the zymogen granules needs to be quickly neutralized to prevent acinar damage. Similarly, the bile ducts need a ‘biliary HCO3– umbrella’ to keep toxic bile acids ionized and thereby membrane-impermeable, and the esophagus needs HCO3– secretion to protect the epithelial surface from acid reflux, and this is possibly mediated also by CFTR-dependent mechanisms. HCO3– is essential for the release and proper expansion of mucin molecules. CF patients and CFTR-deficient mice have impaired lipid absorption, which in mice has been experimentally linked with the duodenal HCO3– deficit. Thus the HCO3– secretory defect of cystic fibrosis patients is closely linked to many of the pathophysiological GI manifestations of CF.
Fluid and electrolyte secretion in the inflamed gut: novel targets for treatment of inflammation-induced diarrhea
Melanie G Gareau and Kim E Barrett
Current Opinion in Pharmacology 2013, 13:895–899
http://dx.doi.org/10.1016/j.coph.2013.08.014
Diarrheal disease can occur in the context of both inflammatory and infectious challenges. Inflammation can result in changes in ion transporter expression or simply mislocalization of the protein. In addition to development of diarrhea, an altered secretory state can lead to changes in mucus secretion and luminal pH. Bacterial infection can lead to subversion of host cell signaling, leading to transporter mislocalization and hyposecretion, promoting bacterial colonization. Novel therapeutic strategies are currently being developed to ameliorate transporter defects in the setting of inflammation or bacterial infection including, for example, administration of probiotics and fecal microbiota transplantation. This review will highlight recent findings in the literature detailing these aspects of ion transport in the inflamed gut.
Inflammatory diarrhea can occur in many different pathological conditions including IBD, comprising Crohn’s disease (CD) and ulcerative colitis (UC). The resulting inflammation triggers production of cytokines, including TNFα and IFNϒ, that can modulate ion transporters directly, including Na+K+ATPase and Na+H+ exchanger (NHE)-1 (SLC9A1), and decrease barrier function. Inflammation can activate several potential mechanisms that can underlie diarrheal symptoms via distinct pathways.
The presence of immune cells, such as T cells, results in the production of cytokines that can inhibit Na+ absorption, activate Cl– secretion, and cause mucosal barrier dysfunction, resulting in diarrhea. In the IL-10 deficient mouse model of colitis, inflammation is characterized by T cells and macrophages, and high levels of pro-inflammatory cytokines, including TNFα. This was accompanied by dysfunctional NHE3 (SLC9A3) transport activity in the absence of overall changes in gene expression and protein localization. A decrease in expression of PDZ adaptor proteins (NHERF2 and PDZK1 scaffolding proteins), which modulate NHE3 activity by regulating transporter interactions and signal transduction, was also observed.
Ion transporters and their regulatory mechanisms represent potential therapeutic targets for the treatment of inflammatory diarrhea. Probiotics, live microorganisms provided in adequate amounts to confer a benefit on the host beyond their inherent nutrition, have been demonstrated to provide a beneficial effect in various GI diseases, including diarrhea. Acute administration of Lactobacillus acidophilus to Caco-2 cells in vitro and to mice in vivo increased DRA expression. Administration of Bifidobacterium breve, but not Lactobacillus rhamnosus or Eubacterium rectale, to HT29 cells down-regulated both Ca2+ (carbachol [CCh]) and cAMP (FSK) mediated Cl– secretion. This effect by B. breve was not seen at the expense of monolayer integrity or tight junction dysfunction, occurred downstream of Ca2+ mobilization and was hypothesized to occur via CFTR based on the observation that a CFTR inhibitor could block the effects of CCh. In contrast, administration of the probiotic strain Enterococcus faecium was able to improve intestinal barrier function in piglets, as measured by mannitol flux rates, whereas prostaglandin E2-induced short circuit current was increased, suggesting an increased secretory state.
Differing degrees of susceptibility to infection with C. rodentium within different strains of mice have been well established and characterized; however the precise mechanisms involved are not well defined. A decrease in DRA was found in C3H and FVB mice, which succumb to C. rodentium infection, compared to resistant C57BL/6 mice. It was recently demonstrated that gavaging C3H mice with the colonic microbiota of C57BL/6 mice, following antibiotic administration, could transfer the protection against death following infection with C. rodentium in C3H mice. Survival was accompanied with restoration of DRA gene expression and other transporters that are known to be involved in protection from diarrhea. While this is extremely preliminary, fecal microbiota transplant may serve as an alternative in a subset of cases of infectious diarrhea, separate from the well-established data on C. difficile.
Phospholipids are increasingly being recognized for their signaling roles in addition to their traditional roles in cell structure. Lysophosphatidic acid (LPA) is a naturally occurring glycerophospholipid that can serve as a signaling molecule via binding to its G-protein coupled receptors LPA1, LPA2, and LPA3. In colonic Caco-2 cells, administration of LPA for 24 hours induced DRA expression via LPA2, increasing its Cl–/HCO3– exchange activity via a PI3 kinase pathway. The ability of LPA to increase ion transporter activity in the setting of inflammation or infection needs to be tested directly, but the findings at least potentially suggest that LPA may serve as a useful anti-diarrheal agent. Studies in bronchial epithelial cells suggest that LPA can also ameliorate lipopoly-saccharide-induced barrier dysfunction, suggesting a similar effect may be present in the intestinal tract. The ability of LPA to increase migration and proliferation of intestinal epithelial cells, however, would warrant some concerns with long-term administration and would need to be carefully assessed.
Intestinal ion transporters represent a valid physiological target for limiting inflammatory and infectious diarrhea. Their ability to regulate both water secretion and absorption allows bidirectional mechanisms to be exploited, creating a wide range of possible therapeutic targets.
Discovery and Development of Antisecretory Drugs for Treating Diarrheal Diseases
Jay R. Thiagarajah, Eun–A Ko, L Tradtrantip, M Donowitz, and A. S. Verkman
Clinical Gastroenterology and Hepatology 2014;12:204–209
http://dx.doi.org/10.1016/j.cgh.2013.12.001
Diarrheal diseases constitute a significant global health burden and are a major cause of childhood mortality and morbidity. Treatment of diarrheal disease has centered on the replacement of fluid and electrolyte losses using oral rehydration solutions. Although oral rehydration solutions have been highly successful, significant mortality and morbidity due to diarrheal disease remains. Secretory diarrheas, such as those caused by bacterial and viral enterotoxins, result from activation of cyclic nucleotide and/or Ca2+ signaling pathways in intestinal epithelial cells, enterocytes, which increase the permeability of Cl– channels at the lumen-facing membrane. Additionally, there is often a parallel reduction in intestinal Na+ absorption. Inhibition of enterocyte Cl– channels, including the cystic fibrosis transmembrane conductance regulator and Ca2-activated Cl– channels, represents an attractive strategy for antisecretory drug therapy. High-throughput screening of synthetic small-molecule collections has identified several classes of Cl– channel inhibitors that show efficacy in animal models of diarrhea but remain to be tested clinically. In addition, several natural product extracts with Cl– channel inhibition activity have shown efficacy in diarrhea models. However, a number of challenges remain to translate the promising bench science into clinically useful therapeutics, including efficiently targeting orally administered drugs to enterocytes during diarrhea, funding development costs, and carrying out informative clinical trials. Nonetheless, Cl– channel inhibitors may prove to be effective adjunctive therapy in a broad spectrum of clinical diarrheas, including acute infectious and drug-related diarrheas, short bowel syndrome, and congenital enteropathies.

Cl- channels as targets for therapy of secretory diarrheas
Cl– channels as targets for therapy of secretory diarrheas. This diagram of fluid secretory mechanism in enterocytes lining intestinal crypts and villi illustrates active Cl– transport from the blood or submucosa to the intestinal lumen facilitated by luminal membrane CFTR and CaCC channels.
Natural products represent a potentially attractive source of antidiarrheal therapeutics, because they are generally inexpensive and have the potential for rapid translation to the clinic. In addition, there is a long history of anecdotal evidence of efficacy of various antidiarrheal remedies in many parts of the world.
A number of hurdles remain in the translation of antidiarrheal drug candidates to widely used therapy. Although a number of compounds have been advanced through preclinical testing in murine models, new high throughput model systems of enterocyte fluid secretion, such as human intestinal enteroids, or genetically tractable systems, such as zebrafish, warrant development to identify novel compounds and antidiarrheal drug targets. A major translational roadblock, however, is the difficulty in designing and funding informative clinical trials.
Barriers to diarrheal drug development in developing countries include the need for very low manufacture cost, high stability in hot and humid environments, and obtaining funding to support commercial development of new chemical entities with relatively low profit potential.
For drugs targeting the enterocyte extracellular surface, an additional challenge is convective washout in which secreted fluid in intestinal crypts washes away inhibitor drugs. A mathematical model of intestinal convection-diffusion concluded that in severe secretory diarrheas, such as cholera, the antisecretory efficacy of an orally administered, surface-targeted inhibitor requires high inhibitor affinity to its target (low nanomolar Kd) to obtain sufficiently high luminal inhibitor concentration (>100-fold Kd), and sustained high luminal inhibitor concentration or slow inhibitor dissociation. Washout is a significant concern for small-molecule CFTR glycine hydrazides, such as iOWH032, and potentially for several of the natural product agents.
Current and emerging therapies in irritable bowel syndrome: from pathophysiology to treatment
Joseph Y. Chang and Nicholas J. Talley
Trends in Pharmacological Sciences 31 (2010) 326–334
http://dx.doi.org:/10.1016/j.tips.2010.04.008
Irritable bowel syndrome is a common functional gastrointestinal disorder with characteristic symptoms of abdominal pain/discomfort with a concurrent disturbance in defecation. It accounts for a significant healthcare burden, and symptoms may be debilitating for some patients. Traditional symptom-based therapies have been found to be ineffective in the treatment of the entire syndrome complex, and do not modify the natural history of the disorder. Although the exact etiopathogenesis of IBS is incompletely understood, recent advances in the elucidation of the pathophysiology and molecular mechanisms of IBS have resulted in the development of novel therapies, as well as potential future therapeutic targets. This article reviews current and emerging therapies in IBS based upon: IBS as a serotonergic disorder; stimulating intestinal chloride channels; modulation of visceral hypersensitivity; altering low-grade intestinal inflammation; and modulation of the gut microbiota.
Irritable bowel syndrome (IBS) is a functional gastrointestinal (GI) disorder characterized by abdominal pain or discomfort that is associated with disturbances in defecation; bloating is common, and the symptoms are not estimates for North America being 10–15%. Only a minority seek care for their symptoms, but IBS has a dramatic impact on patients and utilization of healthcare resources. It is estimated that IBS accounts for 3.5 million physician visits annually in the USA, and is associated with annual direct costs of $1.6 billion and indirect costs of $19.2 billion; patients with IBS consistently report lower health-related quality of life (HRQOL).
Serotonin, or 5-hydroxytryptamine (5-HT), is a neurotransmitter which is largely stored in the enterochromaffin cells of the gut and plays a critical part in the motility, sensation, and secretion of the GI tract. There is growing evidence that a serotonergic mechanism may be involved in the pathophysiology of IBS. Some of the notable findings include: increased postprandial levels of circulating 5-HT in subjects with diarrhea-predominant IBS (D-IBS); D-IBS subjects were observed to have elevated platelet-depleted plasma 5-HT levels in fasting and fed states; the mucosal 5-Hydroxyindoleacetic acid (5-HIAA)/5-HT ratio was decreased in subjects with constipation-predominant IBS (C-IBS); and a lack of increase in plasma 5-HT levels after meal ingestion in those with C-IBS. These findings suggested that a subset of IBS may be a disorder centered on the serotonin disequilibrium, with 5-HT excess responsible for symptoms of D-IBS and insufficient release of 5-HT in the circulation being responsible for the features of C-IBS. However, not all studies support this disease model.
Given the possible role of serotonin in IBS, several 5-HT receptor-modulating agents have been developed as disease-specific therapeutic agents. The 5-HT3 antagonist alosetron has been shown in multiple randomized clinical trials as well as meta-analyses to be an effective agent in the treatment of D-IBS with improvements in global IBS symptoms, relief of abdominal pain, improvement of the consistency and frequency of bowel movements, and reduced fecal urgency. Furthermore, alosetron has been reported to inhibit intestinal secretion, delay colonic transit time, increase colonic compliance in response to distention, and have central effects that result in its beneficial effects on sensation in IBS.
Current and emerging therapies in irritable bowel syndrome
| Serotonergic mechanisms· Alosetron
· Tegaserod
· Prucalopride |
| Chloride channelsActivators
· Lubiprostone
· Linaclotide
Inhibitors
· Crofelemer |
| Visceral hypersensitivityTricyclic antidepressants (TCAs)
· Selective serotonin reuptake inhibitors (SSRIs)
· ϒ-Aminobutyric acid analog (pregabalin)
K-opioid receptor agonists
· Asimadoline
Corticotropin-releasing factor (CRF) receptor antag |
| Modulation of immune activation and inflammation· 5-aminosalicylic acid
· Corticosteroids ? |
| Modulating intestinal floraProbiotics
· Bifidobacteria
Prebiotics
Antibiotics
· Rifaximin |
| Fiber supplementation· Psyllium |
| Antispasmodics· Hyoscine
· Cimetropium
· Pinaverium
· Peppermint oil |
| Alternative therapiesDietary factors and modification
· Food elimination diet (based on IgG antibodies)
· Low fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAPs) diet
· Gluten-free diet |
Agonists to 5-HT4 receptors have been found to be effective in the treatment of C-IBS. 5-HT4 receptor agonists accelerate intestinal transit in the small intestine and colon. Tegaserod is an aminoguanidine indole and selective partial agonist of the 5-HT4 receptor that has been shown to provide improvements in global IBS symptoms and improve constipation in female C-IBS patients. Reports have supported the efficacy of tegaserod in CIBS in terms of global symptom improvement as well as improvement of constipation.
The GI tract contains numerous chloride channels that have an integral role in the transport and secretion of fluids. Type-2 chloride channels (ClC-2) have been investigated with respect to their role in C-IBS and constipation. The ClC-2 channel is an a-helical transmembrane protein located on the apical cell membrane of the intestines, is highly selective for chloride ions, and is involved in the transport and secretion of fluids as well as maintaining cellular membrane potential. Activation of ClC-2 channels through second messenger induced phosphorylation causes an efflux of chloride ions into the lumen of the GI tract, which results in a subsequent efflux of sodium ions due to isoelectric balance. It is the efflux of sodium that results in the efflux of water into the lumen due to the maintenance of isotonic neutrality through the paracellular pathway. This resulting increase in intestinal secretion and fluid volume has been of interest in the development of chloride channel-directed therapies for C-IBS and constipation.
TCAs and SSRIs have been of interest in the treatment of IBS for their modulation of hyperalgesia and not for their psychotropic effects. TCAs have been demonstrated to be effective in the treatment of neuropathic pain, whereas SSRIs have been suggested to enhance the effectiveness of endogenous pain inhibition systems, and both have been effective the in treatment of various chronic pain disorders. Despite the analgesic effects of these agents, some authors have cited the lack of evidence based on well designed large clinical trials of these agents in IBS as reason for caution.
Gammaa Aminobutyric acid (GABA) analog: pregabalin
Pregabalin is a novel second-generation α2δ ligand that is structurally related to ϒ-aminobutyric acid (GABA). It has been shown to be effective in the treatment of inflammatory and neuropathic pain. Its precise mechanism of action is incompletely understood because it does not appear to have GABA-related functional activity or metabolites; it is believed to decrease depolarization-induced calcium influx at nerve terminals, and thereby inhibit release of excitatory neurotransmitters by acting on the α2δ auxiliary proteins associated with voltage-gated calcium channels. Its potential role in IBS is based upon a recent study demonstrating normalization of rectal distension sensory thresholds in IBS patients with rectal hypersensitivity. Placebo-controlled trials of pregabalin for IBS are currently ongoing.
Potential advances in the visceral modulation of IBS have been seen through studies of the role of opiate receptors in visceral pain. Specifically, peripheral K-opioid receptor agonists are of great interest because they are involved in the inhibition of noxious stimuli from the gut and are devoid of many of the adverse side effects (e.g. constipation, opioid dependence) seen in other opioid agonists that bind to µ receptors; K receptors are found most abundantly in the stomach and colon and in the brain. Asimadoline, a novel selective K-opioid receptor agonist, may be promising in the treatment of IBS. Its low blood–brain barrier permeability and low distribution in the central nervous system (CNS) suggest that its analgesic effects are mediated by reduction of excitability of nociceptors on peripheral nerve endings. Human pharmacodynamics studies of asimadoline demonstrated attenuation of visceral sensation without affecting gut motor function, a decrease in satiation and postprandial fullness independent of effects on gastric volume, and attenuation of pain intensity to colonic distension in IBS subjects. These findings led to the investigation of the possible role of asimadoline in IBS.
Like this:
Like Loading...
Read Full Post »