UPDATED: PLATO Trial on ACS: BRILINTA (ticagrelor) better than Plavix® (clopidogrel bisulfate): Lowering chances of having another heart attack
Reporter: Aviva Lev-Ari, PhD, RN
UPDATED on 9/1/2019
Extended DAPT with Brilinta: No Benefit for Stable CAD in T2D
Substudy in those with prior PCI might identify group where bleeding tradeoff is worthwhile
PARIS — Ticagrelor (Brilinta) as part of a dual antiplatelet therapy (DAPT) regimen didn’t improve net outcomes for stable coronary artery disease (CAD) among type 2 diabetes patients, except perhaps in the setting of percutaneous coronary intervention (PCI), the THEMIS trial showed.
Adding the potent antiplatelet agent to aspirin reduced cardiovascular (CV) death, myocardial infarction (MI), or stroke (7.7% vs 8.5%, HR 0.90, 95% CI 0.81-0.99), reported Deepak Bhatt, MD, MPH, of Brigham and Women’s Hospital and Harvard Medical School in Boston, at the European Society of Cardiology (ESC) congress and online in the New England Journal of Medicine.
But it also increased
- TIMI major bleeding (2.2% vs 1.0%, HR 2.32, 95% CI 1.82-2.94) and
- intracranial hemorrhage (0.7% vs 0.5%, HR 1.71, 95% CI 1.18- 2.48) over aspirin alone, albeit
- without more fatal bleeding (0.2% vs 0.1%, P=0.11).
The combined effect was neutral for the exploratory composite outcome of “irreversible harm” (death from any cause, MI, stroke, fatal bleeding, or intracranial hemorrhage 10.1% vs 10.8%, HR 0.93, 95% CI 0.86-1.02).
ESC session study discussant Colin Baigent, MD, of Oxford University in England, actually calculated 12 major bleeds for every eight events prevented.
“This is a consistent story: when we add an antiplatelet agent for risk reduction, we increase the risk of bleeding,” noted Richard Kovacs, MD, of Indiana University in Indianapolis and president of the American College of Cardiology.
THEMIS is the final part of a largely-disappointing PARTHENON development program for ticagrelor, he noted. “It hasn’t changed practice. …Will the main THEMIS trial change clinical practice? In my opinion, no.”
-
Primary Source
New England Journal of Medicine
-
Secondary Source
New England Journal of Medicine
-
Additional Source
The Lancet
SOURCE
UPDATED on 10/4/2016
Soriot’s $3.5B Brilinta dream is dashed by yet another big trial flop for AstraZeneca
by john carroll
October 4, 2016 09:00 AM EDT
Updated: 09:33 AM
Brilinta, the drug failed to demonstrate a benefit over generic Plavix (clopidogrel) for peripheral artery disease. Back in March, the heart drug flopped in a large stroke study, unable to prove that it could beat aspirin. And Soriot can chalk up those expensive studies to proving Brilinta’s serious deficiencies.
“We don’t believe the goal of $3.5 billion is attainable. I think it would be unrealistic to believe that,” Ludovic Helfgott, head of AstraZeneca’s Brilinta business, told Reuters.
Brilinta brought in a total of $619 million last year after disappointing analysts repeatedly with lower-than-expected quarterly revenue.
Heart studies aren’t cheap. AstraZeneca recruited 13,500 patients for the EUCLID study, and it had enrolled close to that number for the earlier SOCRATES trial.
SOURCE
UPDATED on 9/4/2014
Prehospital Ticagrelor in ST-Segment Elevation Myocardial Infarction
September 1, 2014DOI: 10.1056/NEJMoa1407024
-
BACKGROUND
The direct-acting platelet P2Y12 receptor antagonist ticagrelor can reduce the incidence of major adverse cardiovascular events when administered at hospital admission to patients with ST-segment elevation myocardial infarction (STEMI). Whether prehospital administration of ticagrelor can improve coronary reperfusion and the clinical outcome is unknown.
METHODS
We conducted an international, multicenter, randomized, double-blind study involving 1862 patients with ongoing STEMI of less than 6 hours’ duration, comparing prehospital (in the ambulance) versus in-hospital (in the catheterization laboratory) treatment with ticagrelor. The coprimary end points were the proportion of patients who did not have a 70% or greater resolution of ST-segment elevation before percutaneous coronary intervention (PCI) and the proportion of patients who did not have Thrombolysis in Myocardial Infarction flow grade 3 in the infarct-related artery at initial angiography. Secondary end points included the rates of major adverse cardiovascular events and definite stent thrombosis at 30 days.
RESULTS
The median time from randomization to angiography was 48 minutes, and the median time difference between the two treatment strategies was 31 minutes. The two coprimary end points did not differ significantly between the prehospital and in-hospital groups. The absence of ST-segment elevation resolution of 70% or greater after PCI (a secondary end point) was reported for 42.5% and 47.5% of the patients, respectively. The rates of major adverse cardiovascular events did not differ significantly between the two study groups. The rates of definite stent thrombosis were lower in the prehospital group than in the in-hospital group (0% vs. 0.8% in the first 24 hours; 0.2% vs. 1.2% at 30 days). Rates of major bleeding events were low and virtually identical in the two groups, regardless of the bleeding definition used.
CONCLUSIONS
Prehospital administration of ticagrelor in patients with acute STEMI appeared to be safe but did not improve pre-PCI coronary reperfusion. (Funded by AstraZeneca; ATLANTIC ClinicalTrials.gov number, NCT01347580.)
SOURCE
http://www.nejm.org/doi/full/10.1056/NEJMoa1407024?query=TOC
UPDATED on 2/7/2014
PLATO Controversy Hits the Wall Street Journal
February 05, 2014
NEW YORK, NY – The controversy surrounding the PLATOtrial of ticagrelor (Brilinta, AstraZeneca) continues unabated, according to a story published in the Wall Street Journal. Specifically, a sealed complaint filed in US district court in the District of Columbia by a researcher contends that the cardiovascular events in the study “may have been manipulated” [1].
Dr Victor Serebruany (HeartDrug Research Laboratories, Johns Hopkins University, Towson, MD), who has long been a thorn in the side of AstraZeneca and the PLATO investigators, filed the complaint under the False Claims Act, reports theWall Street Journal. The Journal notes that the US attorney’s office in Washington, DC, has contacted Serebruany and is currently investigating the clinical trial.As reported by heartwirein October 2013, the US Department of Justice issued a civil investigative demand from its civil division “seeking documents and information regarding PLATO.” AstraZeneca is complying with the request.
First reported by heart wirein 2009 , the PLATO trial was a positive study involving more 18 000 patients from 43 countries. PLATO investigators, led by Dr Lars Wallentin (Uppsala Clinical Research Center, Sweden), showed that treating acute coronary syndrome patients with ticagrelor significantly reduced the rate of MI, stroke, and cardiovascular death compared with patients taking clopidogrel. Results were presented at the European Society of Cardiology 2009 Congress and reported in the New England Journal of Medicine.
PLATO has been dogged by questions, including prior to approval. In the sealed complaint, Serebruany takes issue with a number of things, many of which have been reported previously. He alleges that the
- number of clinical events among those taking clopidogrel was high compared with other studies, pointing out that the rate of all-cause death was 5.9% among clopidogrel-treated patients—nearly twice as high as earlier studies. In addition,
- the sealed complaint documents the geographic discrepancies in the trial, noting there was a trend toward worse outcomes with ticagrelor at North American sites.The complaint also alleges that
- an initial count of clinical events suggested the two drugs were equivalent, but adjudication by the Duke Clinical Research Institute attributed another 45 MIs to the clopidogrel group, which tipped the results in favor of ticagrelor. Other questions raised about the study include
- site monitoring and timing of clinical events. Serebruany also alleges that
- the trial may have unintentionally been unblinded because of the shape of clopidogrel’s “split capsules,” which would have enabled doctors and nurses to know which drug patients received.
AstraZeneca rebutted these issues, telling the Journal that it is cooperating with the government. It said it is confident in the integrity of the trial and noted the overall study showed the superiority of ticagrelor over clopidogrel. There is no evidence the trial was unblinded and researchers used the same standards when qualifying all clinical events, including MIs, they noted. In addition, the company said it is not possible to compare event rates with clopidogrel in PLATO with other studies because the patient populations differ.
The Journal reports that Serebruany became embroiled in the controversy when asked by the FDA‘s Dr Thomas Marciniak to advise the agency about the PLATO data in 2010. Marciniak, who led the FDA’s review of PLATO, called AstraZeneca’s submission on serious adverse events the “worst submission” he ever encountered. According to the submission, he noted, 12 patients reported their own deaths by telephone. Before approving ticagrelor, the FDA requested an additional analysis of PLATO, and it was eventually approved in the US in July 2011. Ticagrelor was approved in Europe in December 2010 and is authorized for use in more than 100 countries.
The Journal called Serebruany an expert in the antiplatelet field but said he is a “controversial figure,” partly because of his financial ties to industry and repeated criticisms of new drug approvals. Through HeartDrug Research, Serebruany has worked on prasugrel (Effient, Lily/Daiichi-Sankyo), a competing antiplatelet agent, but has also done work for AstraZeneca.
REFERENCE
Burton TM. Doctor challenges testing of AstraZeneca’s Brilinta. Wall Street Journal, February 2, 2014. Available here.
SOURCE
http://www.medscape.com/viewarticle/820236?nlid=47583_1984&src=wnl_edit_medn_card&uac=93761AJ&spon=2
UPDATED 3/28/2013
How AstraZeneca Will Use A Diagnostic To Market Its Blood Thinner
Earlier today I wrote about how AstraZeneca is telling investors that its blood-thinner Brilinta, used to prevent second heart attacks, could be a multi-billion dollar drug, at least twice as big as Wall Street analysts expect. So far the drug has been a disappointment.
I wrote:
Another key data point Astra presented was that blood levels of troponin, a muscle protein released by the heart during a heart attack, predict which patients get the most benefit from Brilinta. This data is not in AstraZeneca’s label, but a spokeswoman said that she believed it would be something the company can market to doctors.
via Can Pascal Soriot Turn Around AstraZeneca? It May Come Down To One Drug – Forbes.
But will the Food and Drug Administration allow Astra to tell doctors that? Stratification using troponin is not in Brilinta’s FDA-approved label, and off-label promotion is illegal. But Ferguson says that communications about troponin will be allowed because all patients with high troponin are patients who would be included in the FDA-approved indication. He confirms that use of troponin testing will be part of the new marketing plan for Brilinta.
SOURCE:
Can Pascal Soriot Turn Around AstraZeneca? It May Come Down To One Drug
by Matthew Herper, Forbes Staff on 3/21/2013
This morning in New York, new AstraZeneca chief executive Pascal Soriot is telling investors how he is going to turn around the company that has had the absolute worst track record in research and development among any big pharmaceutical firm. The plan is fairly wide-ranging and involves a lot of the steps one might expect:
- new layoffs (2,300 jobs);
- a re-focusing of research and development on three areas: heart disease and diabetes; oncology; and respiratory and inflammation;
- new R&D initiatives involving Moderna, a biotech company, and the Karolinska Instutet;
- moving the company’s headquarters to its R&D hub in Cambridge, U.K.;
- re-focusing on emerging markets, where AZ already gets $6 billion in sales, especially China.
But the short-term key to delivering on his promises today seems to come down to a single drug: Brilinta, the Plavix competitor thatAstraZeneca introduced in 2011 which has so far disappointed, generating just $324 $89 million in global sales last year. This is a medicine to prevent heart attacks and strokes in patients who suffer acute coronary syndrome, the condition that occurs after a heart attack or serious heart-related chest pain. It works by preventing the formation of blood clots.
Plavix was the second biggest drug in the world, with $6 billion in annual sales, but it is now generic. The conventional wisdom is that it will be difficult to compete with cheap generics. Brilinta is actually trailing Effient, a similar medicine from Eli Lilly, in usage. Wall Street consensus currently sees Brilinta growing to become a moderate-sized drug in 2018, with $1.3 billion in annual sales. But AstraZeneca is saying that it thinks Brilinta can be a multi-billion dollar product. Astra has confirmed that this means Brilinta will have to surpass Effient. The newer drugs also cause more bleeding than Plavix.
What is the company’s argument? In his presentation today, Paul Hudson, Astra’s Executive Vice President, North America, said that the key would be focusing on one key fact: Brilinta reduced cardiovascular deaths by 21% compared to Plavix in a big clinical trial. That would mean that if everyone eligible for Brilinta got it, 100,000 lives would be saved.
But the reality is that doctors have been skeptical of that data because in the part of that trial that was run in North America, the benefit was less clear. AstraZeneca says that this may have been due to an interaction of Brilinta and aspirin and that, according to current cardiovascular guidelines, doctors should be prescribing less aspirin anyway.
Another key data point Astra presented was that blood levels of troponin, a muscle protein released by the heart during a heart attack, predict which patients get the most benefit from Brilinta. This data is not in AstraZeneca’s label, but a spokeswoman said that she believed it would be something the company can market to doctors.
A lot of what Astra will do in the short term on Brilinta will be blocking and tackling. It needs to pay bigger rebates to insurers to make sure that patients can get cheap access to the drug. (This is how discounts happen in the American insurance system: the patient pays a co-payment and the insurer pays full price for the drug, but then the drug maker gives the insurer money back to make the end cost cheaper.) It will also be doing a lot of medical marketing, involving its internal experts or paid, external doctors, to get the word out about the benefits of Brilinta.
Brilinta has other advantages (it stops acting quickly) and disadvantages (it must be given twice a day). But the other big question for expanding results is whether large clinical trials that are now ongoing will show that it works in a broader array of heart patients. Astra is starting a big trial to show Brilinta prevents strokes. These trials are risky and expensive, but there will be a big payoff if they work.
Astra has some other commercial levers to point to. It’s diabetes pill Onglyza, which is sold with Bristol-Myers Squibb, will have results in a big study of its efficacy in preventing heart disease before a similar study of Merck’s top-selling Januvia, which started first. Soriot has smart ideas about which drugs to advance into later testing. But Brilinta is going to be the biggest single indicator of whether Soriot’s new strategies are paying off.
SOURCE:
BRILINTA is an antiplatelet medication
Taking BRILINTA is a first step in the treatment your physician has chosen for you. At BRILINTA.com, you will find helpful information and useful learning tools to help you complete your course of BRILINTA therapy. Make sure you and your loved ones read through all of the sections.
What is BRILINTA?
BRILINTA is a type of prescription antiplatelet medication for people who have had a recent heart attack or severe chest pain that happened because their heart wasn’t getting enough oxygen and who are being treated with medicines or procedures to open blocked arteries in the heart. BRILINTA is used with aspirin to stop platelets from sticking together and forming a blood clot that could block blood flow to the heart and cause another, possibly fatal, heart attack. Platelets are small cells in the blood that help with normal blood clotting.
Take BRILINTA and aspirin exactly as instructed by your doctor: BRILINTA twice a day, plus one 81-mg aspirin tablet once a day. You should not take a dose of aspirin higher than 100 mg each day because it can affect how well BRILINTA works. Tell your doctor about any medicines you are taking that contain aspirin. Do not take any new medicines that contain aspirin.
Why BRILINTA?
BRILINTA used with aspirin lowers your chance of having another serious problem with your heart or blood vessels such as heart attack, stroke, or blood clots in your stent if you received one. These can be fatal. In fact, in a large clinical study BRILINTA was even better than Plavix® (clopidogrel bisulfate) tablets at lowering your chances of having another heart attack.
BRILINTA is used to lower your chance of having another heart attack or dying from a heart attack, but BRILINTA (and similar drugs) can cause bleeding that can be serious and sometimes lead to death.
Course Program
IMPORTANT SAFETY INFORMATION ABOUT BRILINTA
BRILINTA is used to lower your chance of having another heart attack or dying from a heart attack or stroke, but BRILINTA (and similar drugs) can cause bleeding that can be serious and sometimes lead to death. Instances of serious bleeding, such as internal bleeding, may require blood transfusions or surgery. While you take BRILINTA, you may bruise and bleed more easily and be more likely to have nosebleeds. Bleeding will also take longer than usual to stop.
Call your doctor right away if you have any signs or symptoms of bleeding while taking BRILINTA, including: severe, uncontrollable bleeding; pink, red, or brown urine; vomit that is bloody or looks like coffee grounds; red or black stool; or if you cough up blood or blood clots.
Do not stop taking BRILINTA without talking to the doctor who prescribes it for you. People who are treated with a stent, and stop taking BRILINTA too soon, have a higher risk of getting a blood clot in the stent, having a heart attack, or dying. If you stop BRILINTA because of bleeding, or for other reasons, your risk of a heart attack or stroke may increase. Tell all your doctors and dentists that you are taking BRILINTA. To decrease your risk of bleeding, your doctor may instruct you to stop taking BRILINTA 5 days before you have elective surgery. Your doctor should tell you when to start taking BRILINTA again, as soon as possible after surgery.
Take BRILINTA and aspirin exactly as instructed by your doctor. You should not take a dose of aspirin higher than 100 mg daily because it can affect how well BRILINTA works. Tell your doctor if you take other medicines that contain aspirin. Do not take new medicines that contain aspirin.
Do not take BRILINTA if you are bleeding now, especially from your stomach or intestine (ulcer), have a history of bleeding in the brain, or have severe liver problems.
BRILINTA can cause serious side effects, including bleeding and shortness of breath. Call your doctor if you have new or unexpected shortness of breath or any side effect that bothers you or that does not go away. Your doctor can decide what treatment is needed.
Tell your doctor about all the medicines you take, including prescription and nonprescription medicines, vitamins, and herbal supplements. BRILINTA may affect the way other medicines work, and other medicines may affect how BRILINTA works.
Approved uses
BRILINTA is a prescription medicine for people who have had a recent heart attack or severe chest pain that happened because their heart wasn’t getting enough oxygen and who are being treated with medicines or procedures to open blocked arteries in the heart.
BRILINTA is used with aspirin to lower your chance of having another serious problem with your heart or blood vessels such as heart attack, stroke, or blood clots in your stent if you received one. These can be fatal.
Please read Prescribing Information, including Boxed WARNINGS.
Please read Medication Guide.
You are encouraged to report negative side effects of prescription drugs to the FDA. Visit www.fda.gov/medwatch or call 1-800-FDA-1088.
If you are without prescription coverage and cannot afford your medication, AstraZeneca may be able to help. For more information, please visit www.AstraZeneca.com.
This product information is intended for US consumers only.
BRILINTA is a trademark of the AstraZeneca group of companies.
Plavix® is a registered trademark of sanofi-aventis.
©2012 AstraZeneca.706809-1789005 8/12
SOURCE:
http://www.brilinta.com/antiplatelet-prescription-medication.aspx#au
http://www1.astrazeneca-us.com/pi/brilinta.pdf
BRILINTA (ticagrelor)
Ticagrelor (trade name Brilinta in the US, Brilique and Possia in the EU) is a platelet aggregation inhibitor produced by AstraZeneca. The drug was approved for use in the European Union by the European Commission on December 3, 2010.[1][2] The drug was approved by the US Food and Drug Administrationon July 20, 2011.[3]
Indications
Ticagrelor is indicated for the prevention of thrombotic events (for example stroke or heart attack) in patients with acute coronary syndrome or myocardial infarction with ST elevation. The drug is combined with acetylsalicylic acid unless the latter is contraindicated.[4] Treatment of acute coronary syndrome with ticagrelor as compared with clopidogrel significantly reduces the rate of death.[5]
Contraindications
Contraindications for ticagrelor are: active pathological bleeding and a history of intracranial bleeding, as well as reduced liver function and combination with drugs that strongly influence activity of the liver enzymeCYP3A4, because the drug is metabolized via CYP3A4 and excreted via the liver.[4]
Adverse effects
The most common side effects are shortness of breath (dyspnea, 14%)[6] and various types of bleeding, such as hematoma, nosebleed, gastrointestinal, subcutaneous or dermal bleeding. Allergic skin reactions such as rash and itching have been observed in less than 1% of patients.[4]
Physical and chemical properties
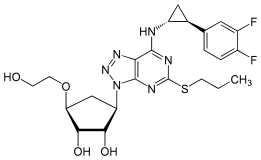
Ticagrelor is a nucleoside analogue: the cyclopentane ring is similar to the sugar ribose, and the nitrogen rich aromatic ring system resembles the nucleobase purine, giving the molecule an overall similarity toadenosine. The substance has low solubility and low permeability under the Biopharmaceutics Classification System.[1]
|
Ticagrelor as a nucleoside analogue |
The nucleoside adenosinefor comparison |
Pharmacokinetics
Ticagrelor is absorbed quickly from the gut, the bioavailability being 36%, and reaches its peak concentration after about 1.5 hours. The main metabolite, AR-C124910XX, is formed quickly via CYP3A4 by de-hydroxyethylation at position 5 of the cyclopentane ring.[7] It peaks after about 2.5 hours. Both ticagrelor and AR-C124910XX are bound to plasma proteins (>99.7%), and both are pharmacologically active. Blood plasma concentrations are linearly dependent on the dose up to 1260 mg (the sevenfold daily dose). The metabolite reaches 30–40% of ticagrelor’s plasma concentrations. Drug and metabolite are mainly excreted via bile and feces.
Plasma concentrations of ticagrelor are slightly increased (12–23%) in elderly patients, women, patients of Asian ethnicity, and patients with mild hepatic impairment. They are decreased in patients that described themselves as ‘coloured’ and such with severe renal impairment. These differences are considered clinically irrelevant. In Japanese people, concentrations are 40% higher than in Caucasians, or 20% after body weight correction. The drug has not been tested in patients with severe hepatic impairment.[4]
Mechanism of action
Like the thienopyridines prasugrel, clopidogrel and ticlopidine, ticagrelor blocks adenosine diphosphate (ADP) receptors of subtype P2Y12. In contrast to the other antiplatelet drugs, ticagrelor has a binding site different from ADP, making it an allosteric antagonist, and the blockage is reversible.[8] Moreover, the drug does not need hepatic activation, which might work better for patients with genetic variants regarding the enzyme CYP2C19 (although it is not certain whether clopidogrel is significantly influenced by such variants).[9][10][11]
Comparison with clopidogrel
The PLATO trial, funded by AstraZeneca, in mid-2009 found that ticagrelor had better mortality rates than clopidogrel (9.8% vs. 11.7%, p<0.001) in treating patients with acute coronary syndrome. Patients given ticagrelor were less likely to die from vascular causes, heart attack, or stroke but had greater chances of non-lethal bleeding (16.1% vs. 14.6%, p=0.0084), higher rate of major bleeding not related to coronary-artery bypass grafting (4.5% vs. 3.8%, P=0.03), including more instances of fatal intracranial bleeding. Rates of major bleeding were not different. Discontinuation of the study drug due to adverse events occurred more frequently with ticagrelor than with clopidogrel (in 7.4% of patients vs. 6.0%, P<0.001)[5] The PLATO trial showed a statistically insignificant trend toward worse outcomes with ticagrelor versus clopidogrel among US patients in the study – who comprised 1800 of the total 18,624 patients. The HR actually reversed for the composite end point cardiovascular (death, MI, or stroke): 12.6% for patients given ticagrelor and 10.1% for patients given clopidogrel (HR = 1.27). Some believe the results could be due to differences in aspirin maintenance doses, which are higher in the United States.[12] Others state that the central adjudicating committees found an extra 45 MIs in the clopidogrel (comparator) arm but none in the ticagrelor arm, which improved the MI outcomes with ticagrelor. Without this adjudication the trials’ primary efficacy outcomes should not be significant[13]
Consistently with its reversible mode of action, ticagrelor is known to act faster and shorter than clopidogrel.[14] This means it has to be taken twice instead of once a day which is a disadvantage in respect of compliance, but its effects are more quickly reversible which can be useful before surgery or if side effects occur.[4][15]
Interactions
Inhibitors of the liver enzyme CYP3A4, such as ketoconazole and possibly grapefruit juice, increase blood plasma levels and consequently can lead to bleeding and other adverse effects. Conversely, drugs that are metabolized by CYP3A4, for example simvastatin, show increased plasma levels and more side effects if combined with ticagrelor. CYP3A4 inductors, for example rifampicin and possibly St. John’s wort, can reduce the effectiveness of ticagrelor. There is no evidence for interactions via CYP2C9.
The drug also inhibits P-glycoprotein (P-gp), leading to increased plasma levels of digoxin, ciclosporin and other P-gp substrates. Ticagrelor and AR-C124910XX levels are not significantly influenced by P-gp inhibitors.[4]
In the US a boxed warning states that use of ticagrelor with aspirin doses exceeding 100 mg/day decreases the effectiveness of the medication.[16]
References
- ^ a b “Assessment Report for Brilique”. European Medicines Agency. January 2011.
- ^ European Public Assessment Report Possia
- ^ “FDA approves blood-thinning drug Brilinta to treat acute coronary syndromes”. FDA. 20 July 2011.
- ^ a b c d e f Haberfeld, H, ed. (2010) (in German). Austria-Codex (2010/2011 ed.). Vienna: Österreichischer Apothekerverlag.
- ^ a b Wallentin, Lars; Becker, RC; Budaj, A; Cannon, CP; Emanuelsson, H; Held, C; Horrow, J; Husted, S et al. (August 30, 2009). “Ticagrelor versus Clopidogrel in Patients with Acute Coronary Syndromes”. NEJM 361 (11): 1045–57. doi:10.1056/NEJMoa0904327. PMID 19717846.
- ^ Brilinta: Highlights of prescribing information
- ^ Teng, R; Oliver, S; Hayes, MA; Butler, K (2010). “Absorption, distribution, metabolism, and excretion of ticagrelor in healthy subjects”. Drug metabolism and disposition: the biological fate of chemicals 38 (9): 1514–21. doi:10.1124/dmd.110.032250. PMID 20551239.
- ^ Birkeland, Kade; Parra, David; Rosenstein, Robert (2010). “Antiplatelet therapy in acute coronary syndromes: focus on ticagrelor”. Journal of Blood Medicine 1: 197–219.
- ^ H. Spreitzer (February 4, 2008). “Neue Wirkstoffe – AZD6140” (in German). Österreichische Apothekerzeitung (3/2008): 135.
- ^ Owen, RT, Serradell, N, Bolos, J (2007). “AZD6140”. Drugs of the Future 32 (10): 845–853. doi:10.1358/dof.2007.032.10.1133832.
- ^ Tantry, Udaya S; Bliden, Kevin P (2010). “First Analysis of the Relation Between CYP2C19 Genotype and Pharmacodynamics in Patients Treated With Ticagrelor Versus Clopidogrel”. Circulation: Cardiovascular Genetics 3: 556–566. doi:10.1161/CIRCGENETICS.110.958561.
- ^ Bernardo Lombo, José G Díez. Ticagrelor: the evidence for its clinical potential as an oral antiplatelet treatment for the reduction of major adverse cardiac events in patients with acute coronary syndromes Core Evid. 2011; 6: 31–42. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3065559/
- ^ Serebruany VL, Atar D. Viewpoint: Central adjudication of myocardial infarction in outcome-driven clinical trials—Common patterns in TRITON, RECORD, and PLATO? Thromb Haemost 2012; DOI: 10.1160/TH12-04-0251. http://www.theheart.org/article/1433145/print.do
- ^ Miller, R (24 February 2010). “Is there too much excitement for ticagrelor?”. TheHeart.org.
- ^ H. Spreitzer (17 January 2011). “Neue Wirkstoffe – Elinogrel” (in German). Österreichische Apothekerzeitung (2/2011): 10.
- ^ July 20, 2011 AstraZeneca: Ticagrelor (Brilinta) Gains FDA Approval Larry Husten cardiobrief.org/2011/07/20/astrazeneca-ticagrelor-brilinta-gains-fda-approval/
SOURCE:
| http://en.wikipedia.org/wiki/Ticagrelor |