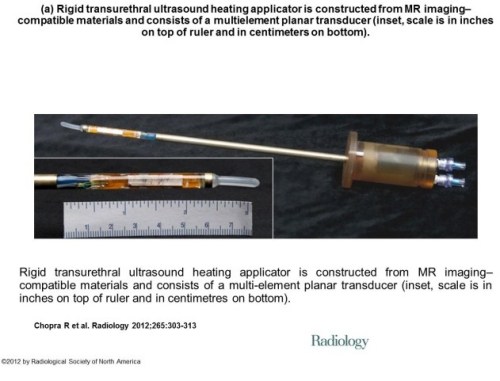
New development in measuring mechanical properties of tissue
Author – Writer: Dror Nir, PhD
Measuring the effects induced onto imaging by the mechanical properties of tissue is a common approach to differentiate tissue abnormalities. In previous posts I discussed the applicability of imaging applications that visualize variations in tissue stiffness; e.g. ultrasound-elastography and MRI-elastography as aid in the diagnosis workflow of cancer. Today, I would like to report on a recent publication made in SPIE Newsroom describing an optical-imaging system to measure tissue stiffness at high resolution. I think that such emerging technologies should be followed up as they bear promise to bridge deficiencies of the traditional modalities currently in use.
Reporting on: Optical elastography probes mechanical properties of tissue at high resolution
By: David Sampson, Kelsey Kennedy, Robert McLaughlin and Brendan Kennedy
Information published at: SPIE Newsroom – Biomedical Optics & Medical Imaging
11 January 2013, SPIE Newsroom. DOI: 10.1117/2.1201212.004605

Elastography is an emerging branch of medical imaging that uses mechanical contrast to better characterize tissue pathology than can be achieved with structural imaging alone. It achieves this by imaging a tissue’s response to mechanical loading. Although commercial products based on ultrasonography and magnetic resonance imaging (MRI) have been available for several years, these new modalities offer superior tissue differentiation deep in the human body. However, elastography is limited by its low resolution compared with the length scales relevant to many diseases. Increasing the resolution with optical techniques might offer new opportunities for elastography in medical imaging and surgical guidance.
An elastography system requires a means of loading the tissue to cause deformation and an imaging system with sufficient sensitivity and range to capture this deformation. Implicit in these requirements is access to the tissue of interest. Optical elastography has previously been largely based on schemes that suit small tissue samples rather than intact tissue in living humans. Additionally, such schemes have not had the sensitivity or range to produce high-fidelity images of mechanical properties. We have addressed both these issues in our recent work, developing the means to access tissues in vivo and improve the sensitivity and range of optical elastography using phase-sensitive optical coherence tomography as the underlying modality. The use of optical coherence tomography to perform elastography has come to be referred to as optical coherence elastography.1
To make optical coherence elastography on human subjects feasible, we designed an annular piezoelectric loading transducer (see Figure 1), through which we could simultaneously image, enabling the first in vivo dynamic optical coherence elastography on human subjects.2 We were subsequently able to extend this to three dimensions (see Figure 2), in collaboration with Stephen Boppart’s group at the University of Illinois at Urbana-Champaign.3 This extension took advantage of the high speed of spectral-domain optical coherence tomography, and the maturity of phase-sensitive detection techniques originally developed for Doppler flowmetry and microangiography.
For general access to tissues in the body, optical coherence elastography faces two basic limitations. The free-space probe requires miniaturization for versatile access to tissue in confined or convoluted geometries. We addressed this in studies of the elastic properties of human airways using catheter-based anatomical optical coherence tomography.4
More fundamentally, optical coherence tomography can only penetrate, at best, 1–2mm into most tissues, limiting it to superficial applications. To address this issue, we combined optical coherence elastography with needle probes, an active research area in our group (see Figure 3).5 We conveniently use the needle probe itself to deform the tissue during insertion.6 The deformation ahead of the needle tip depends on the mechanical properties of the tissue encountered, as well as on the nearby tissue environment, particularly on any interfaces ahead of it. We measure the local sub-micrometer displacement of the tissue between two positions of the moving needle probe. We plot this displacement versus distance ahead of the probe: see Figure 3(c). The slope of the displacement at location z is a measure of the local strain. A change in slope signifies a change in tissue stiffness; the steeper the slope, the softer the tissue (other things being equal). Figure 3 highlights this effect in a layered sample of pig trachea. The positions of the changes in slope correlate well with the tissue interfaces shown in the accompanying histology: see Figure 3(d).
The other key area of improvement we have focused on is lowering the optical coherence elastography noise floor by increasing the detection sensitivity, which is vital to make clinical imaging practical. We firstly showed that Gaussian-smoothed, weighted-least squares strain estimation improved the sensitivity of estimates by up to 12dB over conventional finite-difference methods.7 Next, we showed that performance could be further improved at low optical coherence tomo- graphy signal-to-noise ratios (and, therefore, at greater depths in tissue) by employing a 2D Fourier transform technique.8Combined with other system refinements, these improvements have enabled us to reach a displacement sensitivity of 300pm for typical optical coherence tomography signal-to-noise ratios in tissue, with room for improvement.
The Young’s modulus of soft tissue varies from kPa to tens of MPa, whereas the scattering coefficient of such tissues—which is largely responsible for determining the contrast of optical coherence tomography—is typically in the range 2–20mm−1. This apparent native advantage in mechanical over optical contrast (see the example in Figure 4), combined with the maturation of optical coherence elastography methods, bodes well for the future. In our group, we are pursuing tumor-margin identification using elastography; others have begun to consider corneal elastography,9, 10 and still others are examining shear wave schemes with the aim of probing Young’s modulus much deeper in tissues.11,12
Optical elastography currently sits at a similar stage of development as ultrasound elastography did in 1999. Based on a similar trajectory, this field will rapidly expand over the next decade. Our recent results point to the first convincing applications of optical elastography being just around the corner.
We acknowledge funding for this work from Perpetual Trustees, the Raine Medical Research Foundation, the Cancer Council of Western Australia, the Australian Research Council, the National Health and Medical Research Council (Australia), and the National Breast Cancer Foundation (Australia).
Optical+Biomedical Engineering Laboratory
School of Electrical, Electronic and Computer Engineering
Centre for Microscopy, Characterisation and Analysis
The University of Western Australia
Optical+Biomedical Engineering Laboratory
School of Electrical, Electronic and Computer Engineering
The University of Western Australia