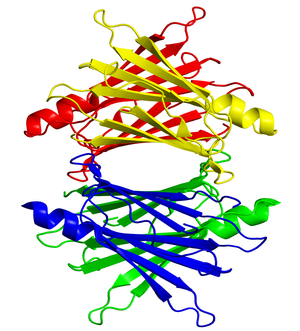
β-amyloid fibrils. (Photo credit: Wikipedia)
Extracellular deposition of insoluble fibrillar proteins in tissues and organs lead to a condition known as amyloidosis which is thought to be caused by misfolding of proteins. There are several types of amyloidosis, but the unifying feature of the amyloidoses is that the deposits share a common ß-pleated sheet structural conformation that confers unique staining properties.
There are several types of amyloidosis and the most common form is the primary amyloidosis (AL) for amyloid of light chain composition. Symptoms can occur in any organ of the body and the organs most often involved include the heart, kidneys, nervous system, and gastrointestinal tract.
Amyloid deposits in these organs can cause
shortness of breath,
fatigue,
edema (swelling of ankles and legs),
dizziness upon standing,
a feeling of fullness in the stomach (especially after eating),
diarrhea,
weight loss,
enlarged tongue,
numbness of the legs and arms,
protein in the urine (proteinurea) and
enlarged liver (hepatomegaly).
Primary amyloidosis (AL) is an acquired plasma cell disorder in which a monoclonal immunoglobulin light chain is produced in the bone marrow and usually found in the blood or urine. AL amyloidosis occasionally occurs with multiple myeloma. The amyloid fibrils in this type of amyloidosis are made up of immunoglobulin light chain proteins (kappa or lambda).
Amyloidosis caused by infection or inflammation is known as Secondary Amyloidosis (also known as AA amyloidosis) in which elevation of an acute phase protein, SAA, a portion of which (AA protein) deposits as amyloid fibrils. AA amyloidosis usually begins as disease in the kidneys, but other organs can be affected, and may cause protein in the urine, edema, and fatigue.
Medical or surgical treatment of the underlying chronic infection or inflammatory disease can slow down or stop the progression of this type of amyloid where as in case of AL chemotherapy is the standard practice.
Other forms of amyloidosis are familial amyloidosis (ATTR) a most common form of inherited amyloidoses caused by a mutation in the transthyretin (TTR) gene that produces abnormal transthyretin protein which deposits as amyloid fibrils. Symptoms of disease are usually neuropathy (numbness and tingling in the arms and legs, dizziness upon standing, and diarrhea) and cardiomyopathy and occur in mid to late life. The standard treatment is liver transplantation since the transthyretin protein which causes familial amyloidosis is made in the liver, replacing this organ removes the source of mutant protein production. A new liver will make only normal transthyretin. Each family has its own pattern of organ involvement and associated symptoms and the mode of transmission is autosomal dominant.
Other rare forms of inherited amyloidosis include apolipoprotein A-I (AApoAI), apolipoprotein A-II (AApoAII) gelsolin (AGel), fibrinogen (AFib), and lysozyme (ALys).
Beta-2 microglobulin amyloidosis is caused by chronic renal failure and often occurs in patients who are on dialysis for many years. Amyloid deposits are made of the beta-2 microglobulin protein that accumulated in tissues, particularly around joints, when it cannot be excreted by the kidney because of renal failure.
There are many types of localized amyloidoses. The most common and best known is Alzheimer’s disease.
Localized amyloid deposits in the airway (trachea or bronchus), eye, or urinary bladder are made up of light chain proteins, similar to those in AL amyloidosis. However, in localized amyloidosis the abnormal plasma cells producing the amyloid light chains are in the tissues, not in the bone marrow. Other localized types of amyloidosis are associated with hormone proteins, aging, or specific areas of the body, and have not been found to develop into systemic amyloidosis
Diagnosis of this disease is sometimes difficult as many of the sysmptoms are general and can occur in other diseases. Symptoms in each patient depend on the type of amyloidosis and on the type of involved organ systems.
Amyloidosis can only be diagnosed by a positive biopsy (i.e., an identification of the amyloid deposits in a piece of tissue). Initial biopsies are most commonly obtained from the abdominal fat.  If amyloid is suspected in other organs, however, a biopsy may be needed from these specific areas. Tissue biopsies must be stained properly with Congo red, a dye which will color the amyloid if it is present and cause it to have a unique appearance when viewed under a special microscope. If amyloid is present in a tissue biopsy, further tests can be done to determine the type of the amyloid.
If amyloid is suspected in other organs, however, a biopsy may be needed from these specific areas. Tissue biopsies must be stained properly with Congo red, a dye which will color the amyloid if it is present and cause it to have a unique appearance when viewed under a special microscope. If amyloid is present in a tissue biopsy, further tests can be done to determine the type of the amyloid.
The Amyloid Treatment & Research Program (ATRP) at Boston Medical Center (BMC) is an international referral center that treats amyloidosis with stem cell transplantation. The Program offers a multi-disciplinary approach to diagnosis and treatment of this multi-organ disorder. Amyloid doctors specializing in cardiology, pulmonary, nephrology, gastroenterology, neurology, and other systems participate in patient evaluation and care.
The ATRP at BMC studies the systemic types of amyloidoses defined under amyloid types. Other forms of amyloidosis include Alzheimer’s and other neurodegenerative diseases, prion diseases, serpinopathies, some of the cystic fibroses, and others.
They have developed Amyloid Light Chain Database, called ALBase, with the support of an NHLBI P01 award, HL68705. ALBase is a curated database and collection of analytical and graphical tools designed to facilitate the analysis of amyloidogenic immunoglobulin (Ig) light chains (LC) occurring in patients with AL amyloidosis. ALBase is designed to compile and analyze Ig LC sequences from patients with AL amyloidosis, to compare their predicted protein sequence and structure to non-amyloidogenic LC sequences from patients with multiple myeloma or health controls. The hypothesis underlying this is that the primary sequence of the LC is likely to be a major determinant of secondary structure and of propensity to unfold, oligomerize, and form fibrils.
“ALBase is available to the scientific community for research purposes. Please reference the site if you make use of it.”
Two patients of Dr. David Seldin are diagnosed with systemic amyloidosis and they shared their experiences from diagnosis to treatment and recovery (You can listen to an audio of this broadcast by clicking here: Rare Disease Feature (WAER 88.3 FM)).
Both patients credit their physicians for investigating abnormal tests and nonspecific symptoms, and for referring them to amyloid specialists early in the disease course.
http://www.bu.edu/amyloid/david-c-seldin-m-d-ph-d/
http://www.bu.edu/amyloid/2012/03/08/npr-interview/
http://www.bmc.org/amyloid.htm#2012gala
Curated by: Dr. Venkat S. Karra, Ph.D
Like this:
Like Loading...
Read Full Post »