- More than 77 percent of patients in the REMfresh® Patient Reported Outcomes DURation (REMDUR) study reported achieving 6 or more hours of sleep after taking REMfresh®, the first continuous release and absorption melatonin™ (CRA-melatonin™)
- More than 91 percent experienced improvements in sleep onset, sleep maintenance and total sleep quality, after taking REMfresh® (CRA-melatonin™)
- Post-marketing, patient-reported outcomes data reinforces clinical trial evidence demonstrating the potential of non-prescription REMfresh®, as a new, non-prescription, drug-free hypnotic (sleep) product designed to achieve 7-hour sleep
- New data confirms previously presented SLEEP 2017 study showing the patented Ion Powered Pump™ (IPP™) technology in REMfresh® helps extend melatonin-targeted sleep maintenance levels in the body from 3.7 hours (with marketed immediate-release melatonin) to 6.7 hours, while mimicking the pattern of the body’s natural melatonin blood levels during the nightly sleep cycle
Real Time Coverage at SLEEP 2018 meeting, Baltimore.
Reporters: Aviva Lev-Ari, PhD, RN, and Gail S. Thornton, MA
BALTIMORE – (June 6, 2018) – A patient-reported outcomes study presented at SLEEP 2018 provides confirmatory real-world evidence of the previously peer-reviewed and presented data showing the 7-hour action of REMfresh®, a new product for sleep. REMfresh® Ion-Powered Melatonin™ is the first and only, continuous release and absorption melatonin™ (CRA-melatonin™) to mimic the body’s own 7-hour Mesa Wave™, the natural pattern of melatonin blood levels during a normal night’s sleep cycle. This induces sleep onset and provides lasting and restorative sleep for up to 7 hours.
This new data shows a correlative relationship between a 7-hour Mesa Wave™ pharmacokinetic (PK) profile and real-world evidence of improvements in sleep duration, onset, maintenance and sleep quality after taking REMfresh® (CRA-melatonin™).
The post-marketing REMfresh® Patient Reported Outcomes DURation (REMDUR) study was presented at SLEEP 2018, the 32nd Annual Meeting of the Associated Professional Sleep Societies (APSS), LLC, a joint partnership of the American Academy of Sleep Medicine (AASM) and the Sleep Research Society (SRS).

Pictured here is David C. Brodner, M.D., and David J. Seiden, M.D., FAASM, after presenting the latest study data which found REMfresh is the first and only continuous release and absorption melatonin™ to mimic the body’s own 7-hour Mesa Wave™.
In a sample of 500 patients on REMfresh® (CRA-melatonin™) responding to an online survey, 77.6 percent achieved 6 or more hours of sleep compared to 23.6 percent who slept that duration prior to taking REMfresh® (p<.0001). A vast majority of respondents also reported a major or moderate improvement in sleep onset (91.6 percent, p<.0001), sleep maintenance (94.8 percent, p<.0001) and total sleep quality (97.2 percent, p<.0001). More than three-quarters (76.6 percent) of patients indicated they take REMfresh® (CRA-melatonin™) nightly. The proportion of patients reporting nightly CRA-melatonin™ use was significantly greater than the proportion of patients with less than nightly use (p<.0001). Most importantly, over 98 percent of patients reported they were very likely or likely to continue taking REMfresh® (CRA-melatonin™) to treat their sleep complaints.
“The real-world evidence reported today in REMDUR provides further confirmation that REMfresh® represents a significant advance in the use of melatonin as a baseline therapy for treating sleep complaints,” said David C. Brodner, M.D., a leading sleep specialist who is Double Board-Certified in Otolaryngology — Head and Neck Surgery and Sleep Medicine, founder and principle Physician at the Center for Sinus, Allergy, and Sleep Wellness, in Palm Beach County, Florida, and Senior Medical Advisor for Physician’s Seal, LLC®.
“REMfresh® Ion-Powered Melatonin™ has been shown to be an effective drug-free solution that is now available to the millions of Americans in need of a good night’s sleep, many of whom seek new therapies that will induce sleep and keep them asleep until the morning, without causing residual effects they’ll feel the next day. With its unique delivery system that imitates the body’s own natural sleep pattern, REMfresh® has revolutionized the role of melatonin, when delivered in the CRA form. It is no longer just a treatment for jet lag, but the CRA-melatonin™ found in REMfresh® has been shown to provide substantial relief to individuals having nightly sleep challenges,” said Dr. Brodner.
The scientifically advanced, patented delivery system in REMfresh® (CRA-melatonin™), called Ion Powered Pump™ (IPP™) technology, replicates the way in which the body naturally releases and absorbs melatonin, unlike conventional melatonin sleep products. Since REMfresh® is not a drug, there is no drug hangover.
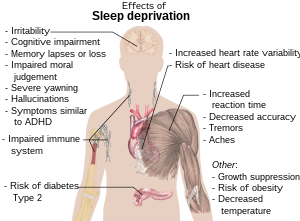
Nearly one-third of U.S. adults sleep less than the recommended seven hours daily.[1],[2] Increasing evidence suggests an association between sub-optimal sleep duration and adverse health outcomes including a higher risk of diabetes, hypertension, heart attack, stroke, obesity and depression.[3] A pooled analysis of 16 studies and over one million patients found short sleep duration corresponded with greater risk of morbidity and mortality.[4]
REMDUR Study Design
The post-marketing REMfresh® Patient Reported Outcomes DURation (REMDUR) study was designed to obtain real-world evidence about patients’ sleep patterns, duration of sleep before and after REMfresh® (CRA-melatonin™), daily REMfresh® (CRA-melatonin™) use, onset of action, sleep maintenance, quality of sleep, and overall satisfaction with REMfresh® (CRA-melatonin™).
Patients with sleep disturbances in the general population who received a sample of CRA-melatonin™ (REMfresh®) from their physicians were invited to complete a 12-question survey. Survey responses were received from 500 patients.
Confirmation of the REMAKT Clinical Study
REMDUR confirmed clinical trial findings from REMAKT (REM Absorption Kinetics Trial), a U.S.-based randomized, crossover pharmacokinetic (PK) evaluation study in healthy, non-smoking adults that compared REMfresh® (CRA-melatonin™) with a market-leading, immediate-release melatonin (IR-melatonin).[5]
The study results, peer-reviewed and presented last year at SLEEP 2017, showed that melatonin levels with REMfresh® (CRA-melatonin™) exceeded the targeted sleep maintenance threshold for a median of 6.7 hours, compared with 3.7 hours with the leading IR-melatonin. Conversely, the levels of the market-leading IR-melatonin formulation dramatically increased 23 times greater than the targeted levels of exogenous melatonin for sleep maintenance and had a rapid decline in serum levels that did not allow melatonin levels to be maintained beyond 4 hours.
The REMfresh® (CRA-melatonin™) studies build upon the body of evidence from prolonged-release melatonin (PR-M), marketed in Europe, which demonstrated in well-conducted, placebo-controlled studies, statistically significant improvement in sleep quality, morning alertness, sleep latency and quality of life in patients aged 55 years and older compared with placebo. REMfresh® (CRA-melatonin™) was designed to overcome the challenges of absorption in the intestines, thereby extending the continual and gradual release pattern of melatonin through the night (known as the Mesa Wave™, a flat-topped hill with steep sides). There was a fast time to Cmax, which is anticipated to result in improved sleep onset, while the extended median plateau time to 6.7 hours and rapid fall-off in plasma levels at the end of the Mesa Wave™, may help to improve sleep maintenance and morning alertness.
Conventional melatonin products have had challenges at mimicking the profile of a Mesa Wave™. The scientific work behind REMfresh® (CRA-melatonin™) sought to overcome these challenges by having the melatonin formulation in a matrix that maintains a patented, solubility-enhancing pH environment to help with the transport to the brush border of the gut and its subsequent absorption.
Designed as a hydrogel matrix tablet, REMfresh® (CRA-melatonin™) provides rapid release of the melatonin from the surface of the tablet, as the hydrogel release-controlling matrix is setting up in the acidic environment (pH of 1 to 3.5) in the stomach. As the tablet moves into the higher pH (5.5 to 6.5) environment of the small-intestine, which is above the pKa of melatonin (~4.0), the acidic moiety in the tablet is designed to maintain the pH within the tablet below 4.0 for 7+ hours. The hydrogel matrix, after proper hydration, allows continuous release of the active melatonin and acidic moiety into the lumen of the intestines.
Melatonin: The Body’s Natural Sleep Ingredient
Melatonin is produced by the pineal gland in the brain and is the body’s natural sleep ingredient. Melatonin levels normally begin to rise in the mid-to late evening and remain high for the majority of the night. Levels begin to decline towards early morning, as the body’s wake cycle is triggered. As people age, melatonin levels can drop by as much as 70 percent[6] and their bodies may no longer produce enough melatonin to ensure adequate sleep.
Other available products, such as immediate-release melatonin, help initiate the onset of sleep but are usually unable to sustain prolonged sleep maintenance due to an immediate burst of melatonin, which is quickly degraded due to its relatively short half-life (60 minutes). Absorption in the lower digestive tract is limited by melatonin’s limited ability to be absorbed in a low acidity or neutral pH environment.
Importance of Sleep
Sleep is an essential part of every person’s life. The body requires a certain amount of sleep in order to properly rest, repair and renew itself. Sleep is customarily divided in four different stages, with each stage having a different effect. These four stages are:
N1, N2, deep sleep and REM sleep. The body moves among these four stages several times while asleep. If sleep is disrupted for any reason, a person’s body may not have a chance to properly restore itself, especially if it is struggling to get to the later stages, called deep sleep and REM sleep. Studies have shown that sound and sufficient sleep is important for learning, memory and a healthy immune system. A regular pattern of deep sleep and REM sleep will help a person begin the next day feeling refreshed and ready to go.
About Non-Prescription REMfresh®
REMfresh® (CRA-melatonin™) is the first and only, continuous release and absorption formulation of UltraMel® melatonin (available as 2 mg and 5 mg and with a 0.5 mg anticipated in the second half of 2018). UltraMel® melatonin is a high-quality, 99 percent ultra-pure melatonin sourced from Western Europe exclusively for Physician’s Seal®.
REMfresh® (CRA-melatonin™) is a dietary supplement and is regulated under the Federal Dietary Supplement Health and Education Act, which does not require pre-approval. Melatonin has been in common use for over two decades and has a well-established profile of safe use by millions of people around the world. As with all supplements, individual results may vary.
REMfresh® (CRA-melatonin™) is non-habit forming and does not contain narcotics, hypnotics, barbiturates, sedatives, antihistamines, alcohol or other harsh or additive chemicals. The usual adult recommended dose is 1-2 tablets 30-60 minutes before bedtime. Follow specific dosing instructions found on the back of the box for proper use of supplements.
REMfresh® (CRA-melatonin™) is available at Walmart, Rite Aid and CVS/pharmacy. In 2017 REMfresh® was ranked as the #1 recommended brand for sleep management by sleep doctors[7].
About Physician’s Seal®
Physician’s Seal® is the innovator of REMfresh®, the first and only continuous release and absorption, 99 percent ultra-pure melatonin™ (CRA-melatonin™) that mimics the way the body naturally releases and maintains melatonin over a 7-hour period. Physician’s Seal®, founded in 2015, is a privately held company based in Boca Raton, Florida. It is committed to bringing cutting-edge life science applications to doctors and their patients. For more information, visit www.remfresh.com and connect with us on Facebook and You Tube.
Its sister subsidiary, IM HealthScience® (IMH) is the innovator of IBgard® and FDgard® for the dietary management of Irritable Bowel Syndrome (IBS) and Functional Dyspepsia (FD), respectively. In 2017, IMH added Fiber Choice®, a line of prebiotic fibers, to its product line via an acquisition. IMH® is a privately held company based in Boca Raton, Florida. It was founded in 2010 by a team of highly experienced pharmaceutical research and development and management executives. The company is dedicated to developing products to address overall health and wellness, including conditions with a high unmet medical need, such as digestive health. The IM HealthScience® advantage comes from developing products based on its patented, targeted-delivery technologies called Site Specific Targeting® (SST®). For more information, visit www.imhealthscience.com to learn about the company, or www.IBgard.com, www.FDgard.com,and www.FiberChoice.com.
This information is for educational purposes only and is not meant to be a substitute for the advice of a physician or other health care professional. You should not use this information for diagnosing a health problem or disease. The company will strive to keep information current and consistent but may not be able to do so at any specific time. Generally, the most current information can be found on www.remfresh.com. Individual results may vary.
Data Presented at SLEEP 2018 Poster Session on Sleep Maintenance/Sleep Quality
Tuesday, June 5, 2018, 5-7pm
- (Abstract 0419, Poster Board #104) Improvement in Sleep Maintenance and Sleep Quality with Ion Powered Pump Continuous Release and Absorption Melatonin: Results from a Self-Reported Patient Outcomes Study
- David J. Seiden, M.D., FAASM, David C. Brodner, M.D., Syed M. Shah, Ph.D.
Visit Physician’s Seal® at booth 220 to learn more about REMfresh®.
The abstract is published in an online supplement of the journal, Sleep, which is available at http://www.sleepmeeting.org/docs/default-source/default-document-library/abstractbook2018.pdf?sfvrsn=2
[1] Ford, E.S., Cunningham, T.J., & Croft, J.B. (2015, May 1). Trends in Self-Reported Sleep Duration among US Adults from 1985 to 2012. Sleep, 38(5):829-832. doi: 10.5665/sleep.4684.
[2] Watson, N.F., Badr, M.S., Belenky, G., Bliwise, D.L., Buxton, G.M., Buysse, D.,…Tasali, E. (2015). Joint Consensus Statement of the American Academy of Sleep Medicine and Sleep Research Society on the Recommended Amount of Sleep for a Healthy Adult: Methodology and Discussion. Journal of Clinical Sleep Medicine, 11(8):931-952. doi:10.1176/appi.ajp.158.11.1856.
[3] Colten, H.R., & Altevogt, B.M. (Eds). (2006). Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. Institute of Medicine (US) Committee on Sleep Medicine and Research. Washington, DC: National Academies Press (US). doi: https://doi.org/10.17226/11617.
[4] Cappuccio, F.P., D’Elia, L., Strazzullo, P.,& Miller, M.A. (2010). Sleep duration and all-cause mortality: a systematic review and meta-analysis of prospective studies. Sleep, 33(5):585-592
[5] For this clinical trial, the head-to-head comparison was with the 5 mg form; a 2 mg form of the comparator was not available.
[6] Zisapel, N. (2010). Melatonin and sleep. The Open Neuroendocrinology Journal, 3: 85-95.
[7] Among primary care physicians with a certification in sleep disorders who recommended a brand of modified-release melatonin. Quintiles IMS ProVoice July-September 2017 survey.
REFERENCE/SOURCE
Physician’s Seal® and REMfresh® (www.remfresh.com)
Other related articles published in this Open Access Online Scientific Journal include the following:
2017
Ultra-Pure Melatonin Product Helps Maintain Sleep for Up to 7 Hours
Ultra-Pure Melatonin Product Helps Maintain Sleep for Up to 7 Hours
2016
Sleep Science
Genetic link to sleep and mood disorders
https://pharmaceuticalintelligence.com/2016/02/27/genetic-link-to-sleep-and-mood-disorders/
2015
Sleep quality, amyloid and cognitive decline
https://pharmaceuticalintelligence.com/2015/10/31/sleep-quality-amyloid-and-cognitive-decline/
2013
Day and Night Variation in Melatonin Level affects Plasma Membrane Redox System in Red Blood Cells
https://pharmaceuticalintelligence.com/2013/02/23/httpwww-ncbi-nlm-nih-govpubmed22561555/
Read Full Post »