Do Novel Anticoagulants Affect the PT/INR? The Cases of XARELTO (rivaroxaban) or PRADAXA (dabigatran)
Curators: Vivek Lal, MBBS, MD, FCIR, Justin D Pearlman, MD, PhD, FACC
and
Article Curator: Aviva Lev-Ari, PhD, RN

WordCloud by Zach Day; Article Title: Do Novel Anticoagulants Affect the PT/INR? The Cases of XARELTO (rivaroxaban) and PRADAXA (dabigatran)
UPDATED on 7/16/2019
More of Xarelto’s scripts came from Medicare Part D patients in Q2 of this year compared with last, according to J&J’s earnings presentation. And J&J was on the hook for a bigger share of patient costs in Medicare Part D’s donut hole. Congress implemented the donut hole change last year, forcing drugmakers to pay more to move patients out of the coverage gap.
Once J&J gets a few quarters ahead of those changes, Xarelto should start turning in more impressive growth percentages, Duato said. How? J&J plans to grow Xarelto’s market share and volume in existing uses, plus focus on launches in new indications, Duato said, though he didn’t specify exactly how it’ll pump up that volume.
Bristol-Myers Squibb and Pfizer’s rival drug Eliquis is surely facing some of the same issues—the donut hole provision, for instance—but its sales look much healthier. While BMS hasn’t yet released second-quarter results, it did report a 36% boost to U.S. Eliquis sales in the first quarter, to $1.2 billion. For comparison, J&J’s Xarelto posted a 6.3% decrease to $542 million for the same period in the U.S.
SOURCE
UPDATED ON 7/21/2016
Xarelto Lawsuits
The blood-thinner Xarelto can cause uncontrolled bleeding — a dangerous and possibly fatal side effect for which there is no antidote. Plaintiffs who say they were harmed by the drug and family members who lost loved ones to severe bleeding filed lawsuits against Bayer, the drug’s maker. They claim Bayer failed to warn them and manufactured a faulty drug.
SOURCE
https://www.drugwatch.com/xarelto/lawsuit/
UPDATED on 8/4/2014
A cost-analysis model for anticoagulant treatment in the hospital setting
Journal of Medical Economics
July 2014, Vol. 17, No. 7 , Pages 492-498 (doi:10.3111/13696998.2014.914032)
Samir H. Modya, Lynn Huynhb, Daisy Y. Zhuob, Kevin N. Tranb, Patrick Lefebvrec, Brahim Bookhartd
aJanssen Scientific Affairs, LLC,
, USA
bAnalysis Group, Inc.,
, USA
cGroupe d’analyse, Ltée,
, Canada
dJanssen Scientific Affairs, LLC,
, USA
Abstract
| Background: |
|---|
Rivaroxaban is the first oral factor Xa inhibitor approved in the US to reduce the risk of stroke and blood clots among people with non-valvular atrial fibrillation, treat deep vein thrombosis (DVT), treat pulmonary embolism (PE), reduce the risk of recurrence of DVT and PE, and prevent DVT and PE after knee or hip replacement surgery. The objective of this study was to evaluate the costs from a hospital perspective of treating patients with rivaroxaban vs other anticoagulant agents across these five populations.
| Methods: |
|---|
An economic model was developed using treatment regimens from the ROCKET-AF, EINSTEIN-DVT and PE, and RECORD1-3 randomized clinical trials. The distribution of hospital admissions used in the model across the different populations was derived from the 2010 Healthcare Cost and Utilization Project database. The model compared total costs of anticoagulant treatment, monitoring, inpatient stay, and administration for patients receiving rivaroxaban vs other anticoagulant agents. The length of inpatient stay (LOS) was determined from the literature.
| Results: |
|---|
Across all populations, rivaroxaban was associated with an overall mean cost savings of $1520 per patient. The largest cost savings associated with rivaroxaban was observed in patients with DVT or PE ($6205 and $2742 per patient, respectively). The main driver of the cost savings resulted from the reduction in LOS associated with rivaroxaban, contributing to ∼90% of the total savings. Furthermore, the overall mean anticoagulant treatment cost was lower for rivaroxaban vs the reference groups.
| Limitations: |
|---|
The distribution of patients across indications used in the model may not be generalizable to all hospitals, where practice patterns may vary, and average LOS cost may not reflect the actual reimbursements that hospitals received.
Keywords
SOURCE
http://informahealthcare.com/doi/abs/10.3111/13696998.2014.914032
Introduction
Justin D Pearlman, MD, PhD, FACC
The classic medication for chronic anti-coagulation is coumadin, but it is problematic. Coumadin impedes the production of coagulation proteins that depend on vitamin K (factors 7, 9, 10, and 2, in order of half-lifes, which range 2-72 hours). Consequently, a change in dose today does not have full impact for 2-3 days. Physicians and pharmacists have difficulties adjusting the dose to its target effect on the biomarker test International Normalized Ratio (INR). The therapeutic range is very narrow. A change in intake of leafy green vegetables can have profound impact (by changing intake of vitamin K). A change in virtually any medication or vitamin that can bind to albumin can also profoundly change the INR to a life-threatening level, because 80% of coumadin is inactivated by binding to albumin, and displacement of coumadin by other agents can boost the effective circulating amount. Those limitations, and the need for testing each month and each medication change have stimulated the development of alternatives. For example, rivaroxaban is a new anticogulant that focuses on factor 10 (factor X), deemed as good as coumadin without the need for the blood tests. In fact, INR test for rivaroxaban is misleading, as values may range as high at 7 (“DANGER”) at normal therapeutic dosing. The following reviews some of the data on that unexpected issue. Physicians not aware of this “false positive” have demanded stoppage of therapy due to the inapplicable spuriously high INR values.
UPDATED on 9/25
Dabigatran versus Warfarin in Patients with Mechanical Heart Valves
Dabigatran is an oral direct thrombin inhibitor that has been shown to be an effective alternative to warfarin in patients with atrial fibrillation. We evaluated the use of dabigatran in patients with mechanical heart valves.
RESULTS
The trial was terminated prematurely after the enrollment of 252 patients because of an excess of thromboembolic and bleeding events among patients in the dabigatran group. In the as-treated analysis, dose adjustment or discontinuation of dabigatran was required in 52 of 162 patients (32%). Ischemic or unspecified stroke occurred in 9 patients (5%) in the dabigatran group and in no patients in the warfarin group; major bleeding occurred in 7 patients (4%) and 2 patients (2%), respectively. All patients with major bleeding had pericardial bleeding.
CONCLUSIONS
The use of dabigatran in patients with mechanical heart valves was associated with increased rates of thromboembolic and bleeding complications, as compared with warfarin, thus showing no benefit and an excess risk. (Funded by Boehringer Ingelheim; ClinicalTrials.gov numbers, NCT01452347 and NCT01505881.)
SOURCE
N Engl J Med 2013; 369:1206-1214 September 26, 2013 DOI: 10.1056/NEJMoa1300615
UPDATED on 9/23
ESC: Edoxaban Bests Warfarin on Safety in VTE
AMSTERDAM — Edoxaban, a novel factor Xa inhibitor, met its primary endpoints in a trial that pitted it against warfarin for treatment of symptomatic venous thromboembolism (VTE).
Among more than 8,000 patients with deep-vein thrombosis (DVT) or pulmonary embolism (PE), 130 (3.2%) of the patients treated with edoxaban had a recurrent, symptomatic VTE versus 146 (3.5%) warfarin-treated patients, a hazard ratio of 0.89 (95% CI 0.70-1.13, P<0.004 for non-inferiority), Harry R. Büller, MD, of the Academic Medical Center, Amsterdam, reported in a Hot Line session at theEuropean Society of Cardiology meeting here.
The safety endpoint was bleeding (major or clinically relevant non-major bleeding), and in that analysis edoxaban was superior to warfarin, as 8.5% of the edoxaban patients had bleeding events versus 10.3% of the patients in the warfarin group (P=0.004 for superiority).
Moreover, edoxaban appeared to work best in the highest-risk patients — 938 patients with pulmonary embolism and right ventricular dysfunction assessed by N-terminal pro-brain natriuretic peptide levels. In those patients, the recurrent VTE rate was 3.3% in the edoxaban group versus 6.2% in the warfarin group, Büller said.
Based on the results in that very high risk population, Büller predicted that clinicians treating those patients will consider that efficacy profile when selecting an oral Factor Xa inhibitor.
The study, from the Hokusai VTE Investigators, was simultaneously published online by the New England Journal of Medicine.
In the highly competitive oral anticoagulant group, those numbers look good, but at first blush the two already approved Factor Xa inhibitors, rivaroxaban (Xarelto) and apixaban (Eliquis) looked better when they were studied in VTE.
In EINSTEIN-VTE, rivaroxaban had a recurrent symptomatic VTE rate of 2.1%, and 8.1% of patients met the safety endpoint.
Likewise, in another VTE trial — AMPLIFY-EXT — apixaban (2.5 mg or 5 mg twice a day) had a recurrent or VTE-related death rate of 1.7%, and 3.2% of the patients who received low-dose apixaban reached the safety endpoint, as did 4.3% of patients treated with 5 mg of apixaban.
Patrick T. O’Gara, MD, American College of Cardiology president-elect, praised the design of the trial, but he agreed that “for mortality benefit, apixaban does appear to have the edge.”
That apixaban benefit, O’Gara said, is militated by the fact that patients need to take the drug twice daily, while “edoxaban is once a day, as is rivaroxaban.”
Asked if there was a specific population that might benefit from edoxaban versus rivaroxaban or apixaban, O’Gara, who is director of clinical cardiology at Brigham and Women’s Hospital and a professor at Harvard Medical School, said the findings from the Hokusai researchers did not provide that answer.
The attempt at a cross-trial comparison drew harsh criticism from Elliott Antman, MD, principal investigator in a trial of edoxaban for prevention of stroke in patients with atrial fibrillation (ENGAGE-AF).
Antman, who like O’Gara is a Harvard professor, said that comparing the edoxaban VTE results to EINSTEIN-VTE or AMPLIFY-EXT would only lead to false conclusions. “You could repeat the rivaroxaban trial 100 times and still not achieve data that can be compared.”
Stavros V. Konstantinides MD, PhD, of the Medical University in Mainz, Germany, who was the ESC discussant for the paper, said that, despite the advantage of once-daily dosing of edoxaban, “apixaban has the best safety profile so far.”
Moreover, unlike the VTE studies of apixaban and rivaroxaban, all patients in the Hokusai trial received heparin for 5 days. After that heparin run-in, patients were randomized to edoxaban or to warfarin. The median duration of heparin after randomization was 7 days.
Antman said that design best replicated real-world clinical practice, in which heparin is usually started before warfarin.
Buller noted that he was an investigator for the EINSTEIN-VTE study, “and after that the thinking was maybe we don’t need low molecular weight heparin, but now I think we need to reconsider that assumption.”
The Hokusai-VTE trial recruited 4,921 patients with DVT and 3,319 patients with PE. Patients initially were treated with heparin, and then were randomized to edoxaban (60 mg or 30 mg) or warfarin. There was an overlap of the heparin therapy when warfarin was started.
During a press conference, Keith Fox, MBChB, chair of the ESC scientific program, asked Buller if that overlap could have increased bleeding risk in the warfarin arm, thus introducing bias, but Buller said the overlap merely allowed warfarin to reach therapeutic range.
The edoxaban regimen “may be less handy, especially for early-discharge patients… [though] some doctors may feel more comfortable starting with low molecular weight heparin and then switching to edoxaban for the one-third of patients with severe PE,” Konstantinides said.
He added, “The NOACs [new oral anticoagulants] have shown efficacy and safety. Now, the test under real life conditions begins. They have to prove efficacy and safety there. I expect that. And they now must justify the high cost by showing … an improvement in patient treatment satisfaction and quality of life and, hopefully, a reduction in healthcare costs … with lower hospitalizations.”
The average age of patients in the Hokusai study was 56-57, and just over half were men.
Patients were enrolled from January 2011 through October 2012 at 439 centers in 37 countries.
About 40% of patients were treated for a year, and 80% of the edoxaban group was adherent to study treatment. Among the warfarin patients, average time in therapeutic range was 63.5%.
The study was supported by Daiichi-Sankyo, which is developing edoxaban.
Buller reported personal fees from Daichi Sankyo during the study, as well as grant support and personal fees from Bayer Health Care and Pfizer. He also received personnal fees from Boehringer Ingelheim, Bristol-Myers Squibb, Isis Pharmaceuticals, and ThromboGenics outside the submitted work.
Antman has a research grant from Daiichi-Sankyo through Brigham and Women’s Hospital. O’Gara said he had no financial disclosures.
SOURCE
http://www.medpagetoday.com/MeetingCoverage/ESC/41301?isalert=1#!
END of UPDATE
Introduction
Author: Vivek Lal, MBBS, MD, FCIR
Pathological thromboembolism, as seen in Myocardial Infarction or stroke, led to the use of low dose aspirin as an-antiplatelet drug, as a prophylaxis for subsequent intravascular thrombotic episodes. Aspirin, an irreversible Cyclo-oxygenase inhibitor, resulted in a reduction of the production of Thromboxane A2, which in itself is a powerful vaso-constrictor and a platelet aggregator. Certain limitation with the use of aspirin necessitated the search for newer anti-platelet drugs, with a quicker onset of action, quick termination of action on cessation of treatment, and minimal side effects like bleeding. ADP inhibitors like Clopidogrel, which inhibits the ADP dependent activation of Glycoprotein IIb/IIIa receptors, was the next in the armamentarium of these drugs. Later, oral anti-coagulants like coumadin (warfarin sodium) were added to anti-platelet approach, to tackle the overactive coagulation cascade in pathological intravascular thrombosis. Warfarin is a drug which counters the effects of Vit-K on the synthesis of coagulation factors in the liver. Thus, all green leafy vegetables, which contain high amounts of Vit-K, will interfere with the action of Warfarin. Moreover, warfarin is extremely prone to drug interations, owing to its biotransformation by hepatic microsomal enzymes, which are also metabolizing many other drugs. Thus, a therapeutic drug monitoring of warfarin action is mandatory, which, is a big limitation to its use. The quest for pharmacologically superior oral anticoagulants, as compared to Warfarin, reached an important milestone with the discovery of two major drugs, Dabigatran and Rivaroxaban. Both these drugs are Direct Thrombin Inhibitors, though the indications and adverse events are somewhat different. This post will discuss Rivaroxaban pharmacology in brief, and address certain clinical issues.
Question: Does rivaroxaban or dabigatran affect the PT or INR? Can either be monitored using the PT or INR?
Response from Jenny A. Van Amburgh, PharmD, CDE
Assistant Dean of Academic Affairs and Associate Clinical Professor, School of Pharmacy, Northeastern University; Director of the Clinical Pharmacy Team and Residency Program Director, Harbor Health Services, Inc., Boston, Massachusetts
Warfarin is the most commonly used anticoagulant for the prevention of thrombosis or stroke. Because of a narrow therapeutic window, it requires regular coagulation monitoring of the prothrombin time (PT)/international normalized ratio (INR).[1] As such, the inconvenience of frequent blood draws remains a major burden. For the first time in over 50 years, 2 new oral anticoagulants, dabigatran, a direct thrombin inhibitor, and rivaroxaban, a factor Xa inhibitor, were approved by the US Food and Drug Administration. While these anticoagulants carry similar side effects to warfarin, such as risk for gastrointestinal bleeding and intracranial hemorrhage, INR and PT monitoring are not required. How then are providers to gauge the safety and efficacy of the medication in a patient? Can clinicians monitor these medications with the conventional coagulation assays, or are they rendered useless?[1]
The effect of both dabigatran and rivaroxaban on commonly used coagulation assays has been evaluated in the literature, both in vitro and in vivo. The usefulness of these tests relates directly to the medications’ mechanisms of action. For both agents, the use of an INR to determine the effectiveness and safety is meaningless because INR is calibrated for use with vitamin K antagonists (such as warfarin) only.[1] Although use may be associated with an increase in INR, this increase does not relate to the effectiveness of therapy or provide a linear correlation of concentration and effect that is seen when measuring warfarin levels.[2,3] In some instances, point-of-care INR measurements have been drawn on patients using dabigatran; however, the results have failed to correlate to appropriateness in therapy and have varied greatly case by case.[4]
As dabigatran directly inhibits thrombin, PT measures lack the sensitivity to detect therapeutic levels.[1,5] Often, if this assay is measured in patients taking dabigatran, a subtherapeutic level is noted, regardless of concentration of dabigatran.[6] More appropriate assays for dabigatran may be activated partial thromboplastin time (aPTT), diluted thrombin time (TT), or ecarin clotting time (ECT). These tests are better able to capture changes throughout the clotting cascade. Using aPTT may underestimate high levels and could be used more as a qualitative assessment of activity instead of a quantitative assessment.[7] Where available and if desired, monitoring via the diluted TT or ECT has proved a more useful measure for dabigatran.[1]
Unlike dabigatran, studies have demonstrated a correlation between the levels of rivaroxaban and PT through inhibition of factor Xa, but not to the same extent as warfarin.[8] In some instances, the use of PT monitoring for this medication may be useful. A linear response between PT and rivaroxaban can be seen; however, the accuracy of the test improves when concentrations of rivaroxaban are higher. Additionally, the use of PT for monitoring rivaroxaban can be difficult because the measurement differs greatly depending on the reagent used to determine PT. Calibrating PT assays to assess rivaroxaban appropriately is an option currently being evaluated.[8]
In conclusion, the INR is not a viable option when assessing the use of dabigatran or rivaroxaban. Additionally, PT is not a viable option when monitoring a patient on dabigatran. However, PT may be an option for monitoring select patients on rivaroxaban until more reliable standardized tests are developed. Methods of measuring the effectiveness of these agents are currently being developed and tested; however, until they are made available, the existing tests may be adapted to be used in a more effective manner.
The author wishes to acknowledge the assistance of Jacqueline M. Kraft, PharmD, Ngoc Diem Nguyen, PharmD, and Phillipa Scheele, PharmD, PGY1 Residents, and Michael P. Conley, PharmD, and Nga T. Pham, PharmD, CDE, AE-C, Assistant Clinical Professors at Northeastern University — School of Pharmacy and Harbor Health Services, Inc., Boston, Massachusetts.
References
- Favaloro EJ, Lippi G. The new oral anticoagulants and the future of haemostasis laboratory testing. Biochem Med (Zagreb). 2012;22:329-341.
- Dager WE, Gosselin RC, Kitchen S, Dwyre D. Dabigatran effects on the international normalized ratio, activated partial thromboplastin time, thrombin time, and fibrinogen: a multicenter, in vitro study. Ann Pharmacother. 2012;46:1627-1636. Abstract
- Samama MM, Martinoli JL, LeFlem L, et al. Assessment of laboratory assays to measure rivaroxaban — an oral, direct factor Xa inhibitor. Thromb Haemost. 2010;103:815-825. Abstract
- O’Riordan M. Falsely elevated point-of-care INR values in dabigatran-treated patients. Heartwire. July 7, 2011.http://www.theheart.org/article/1251461.do. Accessed January 11, 2013.
- Halbmayer WM, Weigel G, Quehenberger P, et al. Interference of the new oral anticoagulant dabigatran with frequently used coagulation tests. Clin Chem Lab Med. 2012;50:1601-1605. Abstract
- Lindahl TL, Baghaei F, Blixter IF, et al. Effects of the oral, direct thrombin inhibitor dabigatran on five common coagulation assays. Thromb Haemost. 2011;105:371-378. Abstract
- Freyburger G, Macouillard G, Labrouche S, Sztark F. Coagulation parameters in patients receiving dabigatran etexilate or rivaroxaban: two observational studies in patients undergoing total hip or total knee replacement. Thromb Res. 2011;127:457-465. Abstract
- Hillarp A, Baghaei F, Fagerberg Blixter I, et al. Effects of the oral, direct factor Xa inhibitor rivaroxaban on commonly used coagulation assays. J Thromb Haemost. 2011;9:133-139. Abstract
SOURCE
http://www.medscape.com/viewarticle/778063
PRADAXA (dabigatran)
COMPARE TO WARFARIN FOR AFIB NOT CAUSED BY A HEART VALVE PROBLEM
PRADAXA represents progress in helping to reduce the risk of stroke due to atrial fibrillation (AFib) not caused by a heart valve problem.
Review the chart below to compare PRADAXA and warfarin (also known as Coumadin® or Jantoven®). And find out why your doctor may choose PRADAXA. Remember, only your doctor can decide which treatment may be right for you.
| Medication type: Both PRADAXA and warfarin are anticoagulants. These blood-thinning medicines help to stop clots by targeting factors your blood needs to form clots.PRADAXA and warfarin work differently to help reduce the risk of stroke due to AFib not caused by a heart valve problem. |
PRADAXA is a direct thrombin inhibitor that helps to stop clots from forming by working directly on thrombin.PRADAXA is not for use in people with artificial (prosthetic) heart valves | Warfarin is a vitamin K antagonist that helps to stop clots from forming by interfering with vitamin K—a vitamin your body needs to form clots. |
| Stroke risk reduction: PRADAXA and warfarin help to stop clots by targeting factors your blood needs to form clots. |
In a clinical trial of more than 18,000 people, PRADAXA 150 mg capsules was proven superior to warfarin at reducing the risk of stroke. | Warfarin has been extensively studied and prescribed by doctors to help reduce the risk of stroke in people with AFib since 1954. |
| How you take the medication: | PRADAXA is taken by mouth 2 times each day. | Warfarin is taken by mouth once every day. |
| Dosing options: | PRADAXA comes in 75 mg and 150 mg strengths.Your doctor will decide which dose is right for you based on a simple kidney function test. | Warfarin comes in 1 mg, 2 mg, 2-1/2 mg, 3 mg, 4 mg, 5 mg, 6 mg, 7-1/2 mg, and 10 mg strengths.Your doctor will decide which dose is right for you. He or she will adjust your dose based on the results ofregular blood tests.Based on these tests, your doctor will determine your dose and adjust it, if necessary. |
| Monitoring: | No need for regular blood tests.PRADAXA has been clinically proven to help reduce the risk of stroke in people with AFib not caused by a heart valve problem. And, unlike warfarin, there is no need for regular blood tests to see if your blood-thinning level is in the right range. Learn more |
Requires regular blood test.Warfarin has also been proven to be an effective blood thinner. When you take warfarin, you need to have a regular blood test to measure International Normalized Ratio (INR) to determine the time it takes for your blood to clot. |
| Dietary restrictions: | No dietary restrictionsPRADAXA requires no changes to your diet. | Dietary restrictions requiredWhen you take warfarin, you need to limit foods high in vitamin K, such as large amounts of leafy green vegetables and some vegetable oils. This is because Vitamin K can affect the way warfarin works in your body.You may also need to limit alcohol, cranberry juice, and products containing cranberries. |
SOURCE
https://www.pradaxa.com/compare-warfarin.jsp
XARELTO (rivaroxaban)
WHAT IS XARELTO®?
XARELTO® is a prescription medicine used to reduce the risk of stroke and blood clots in people with atrial fibrillation, not caused by a heart valve problem. For patients currently well managed on warfarin, there is limited information on how XARELTO® and warfarin compare in reducing the risk of stroke.
XARELTO® is also a prescription medicine used to treat deep vein thrombosis and pulmonary embolism, and to help reduce the risk of these conditions occurring again.
XARELTO® is also a prescription medicine used to reduce the risk of forming a blood clot in the legs and lungs of people who have just had knee or hip replacement surgery.
IMPORTANT SAFETY INFORMATION
WHAT IS THE MOST IMPORTANT INFORMATION I SHOULD KNOW ABOUT XARELTO®?
- For people taking XARELTO® for atrial fibrillation:
- People with atrial fibrillation (an irregular heart beat) are at an increased risk of forming a blood clot in the heart, which can travel to the brain, causing a stroke, or to other parts of the body. XARELTO® lowers your chance of having a stroke by helping to prevent clots from forming. If you stop taking XARELTO®, you may have increased risk of forming a clot in your blood.
- Do not stop taking XARELTO® without talking to the doctor who prescribes it for you. Stopping XARELTO® increases your risk of having a stroke.
- If you have to stop taking XARELTO®, your doctor may prescribe another blood thinner medicine to prevent a blood clot from forming.
- XARELTO® can cause bleeding, which can be serious, and rarely may lead to death. This is because XARELTO® is a blood thinner medicine that reduces blood clotting. While you take XARELTO® you are likely to bruise more easily and it may take longer for bleeding to stop.
You may have a higher risk of bleeding if you take XARELTO® and take other medicines that increase your risk of bleeding, including:
- Aspirin or aspirin-containing products
- Non-steroidal anti-inflammatory drugs (NSAIDs)
- Warfarin sodium (Coumadin®, Jantoven®)
- Any medicine that contains heparin
- Clopidogrel (Plavix®)
- Other medicines to prevent or treat blood clots
Tell your doctor if you take any of these medicines. Ask your doctor or pharmacist if you are not sure if your medicine is one listed above.
Call your doctor or get medical help right away if you develop any of these signs or symptoms of bleeding:
- Unexpected bleeding or bleeding that lasts a long time, such as:
- Nosebleeds that happen often
- Unusual bleeding from gums
- Menstrual bleeding that is heavier than normal, or vaginal bleeding
- Bleeding that is severe or that you cannot control
- Red, pink, or brown urine
- Bright red or black stools (looks like tar)
- Cough up blood or blood clots
- Vomit blood or your vomit looks like “coffee grounds”
- Headaches, feeling dizzy or weak
- Pain, swelling, or new drainage at wound sites
Spinal or epidural blood clots (hematoma): People who take a blood thinner medicine (anticoagulant) like XARELTO®, and have medicine injected into their spinal and epidural area, or have a spinal puncture, have a risk of forming a blood clot that can cause long-term or permanent loss of the ability to move (paralysis). Your risk of developing a spinal or epidural blood clot is higher if:
- A thin tube called an epidural catheter is placed in your back to give you certain medicine
- You take NSAIDs or a medicine to prevent blood from clotting
- You have a history of difficult or repeated epidural or spinal punctures
- You have a history of problems with your spine or have had surgery on your spine
If you take XARELTO® and receive spinal anesthesia or have a spinal puncture, your doctor should watch you closely for symptoms of spinal or epidural blood clots. Tell your doctor right away if you have tingling, numbness, or muscle weakness, especially in your legs and feet.
XARELTO® is not for patients with artificial heart valves.
WHO SHOULD NOT TAKE XARELTO®?
Do not take XARELTO® if you:
- Currently have certain types of abnormal bleeding. Talk to your doctor before taking XARELTO® if you currently have unusual bleeding.
- Are allergic to rivaroxaban or any of the ingredients of XARELTO®.
WHAT SHOULD I TELL MY DOCTOR BEFORE OR WHILE TAKING XARELTO®?
Before taking XARELTO®, tell your doctor if you:
- Have ever had bleeding problems
- Have liver or kidney problems
- Have any other medical condition
- Are pregnant or plan to become pregnant. It is not known if XARELTO® will harm your unborn baby. Tell your doctor right away if you become pregnant while taking XARELTO®. If you take XARELTO® during pregnancy, tell your doctor right away if you have bleeding or symptoms of blood loss.
- Are breastfeeding or plan to breastfeed. It is not known if XARELTO® passes into your breast milk. You and your doctor should decide if you will take XARELTO® or breastfeed.
Tell all of your doctors and dentists that you are taking XARELTO®. They should talk to the doctor who prescribed XARELTO® for you before you have any surgery, medical or dental procedure.
Tell your doctor about all the medicines you take, including prescription and nonprescription medicines, vitamins, and herbal supplements. Some of your other medicines may affect the way XARELTO® works. Certain medicines may increase your risk of bleeding. See “What is the most important information I should know about XARELTO®?”
Especially tell your doctor if you take:
- Ketoconazole (Nizoral®)
- Itraconazole (Onmel™, Sporanox®)
- Ritonavir (Norvir®)
- Lopinavir/ritonavir (Kaletra®)
- Indinavir (Crixivan®)
- Carbamazepine (Carbatrol®, Equetro®, Tegretol®, Tegretol®-XR, Teril™, Epitol®)
- Phenytoin (Dilantin-125®, Dilantin®)
- Phenobarbital (Solfoton™)
- Rifampin (Rifater®, Rifamate®, Rimactane®, Rifadin®)
- St. John’s wort (Hypericum perforatum)
Ask your doctor if you are not sure if your medicine is one listed above. Know the medicines you take. Keep a list of them to show your doctor and pharmacist when you get a new medicine.
HOW SHOULD I TAKE XARELTO®?
Take XARELTO® exactly as prescribed by your doctor.
Do not change your dose or stop taking XARELTO® unless your doctor tells you to.
-
- Your doctor will tell you how much XARELTO® to take and when to take it.
- Your doctor may change your dose if needed.
If you take XARELTO® for:
-
- Atrial Fibrillation: Take XARELTO® 1 time a day with your evening meal. If you miss a dose of XARELTO®, take it as soon as you remember on the same day. Take your next dose at your regularly scheduled time.
- Blood clots in the veins of your legs or lungs:
- Take XARELTO® once or twice a day as prescribed by your doctor.
- Take XARELTO® with food at the same time each day.
- If you miss a dose of XARELTO®:
- and take XARELTO® 2 times a day: Take XARELTO® as soon as you remember on the same day. You may take 2 doses at the same time to make up for the missed dose. Take your next dose at your regularly scheduled time.
- and take XARELTO® 1 time a day: Take XARELTO® as soon as you remember on the same day. Take your next dose at your regularly scheduled time.
- Hip or knee replacement surgery: Take XARELTO® 1 time a day with or without food. If you miss a dose of XARELTO®, take it as soon as you remember on the same day. Take your next dose at your regularly scheduled time.
- If you have difficulty swallowing the tablet whole, talk to your doctor about other ways to take XARELTO®.
- Your doctor will decide how long you should take XARELTO®. Do not stop taking XARELTO® without talking to your doctor first.
- Your doctor may stop XARELTO® for a short time before any surgery, medical or dental procedure. Your doctor will tell you when to start taking XARELTO®again after your surgery or procedure.
- Do not run out of XARELTO®. Refill your prescription for XARELTO® before you run out. When leaving the hospital following a hip or knee replacement, be sure that you have XARELTO® available to avoid missing any doses.
- If you take too much XARELTO®, go to the nearest hospital emergency room or call your doctor right away.
WHAT ARE THE POSSIBLE SIDE EFFECTS OF XARELTO®?
Please see “What is the most important information I should know about XARELTO®?”
Tell your doctor if you have any side effect that bothers you or that does not go away.
Call your doctor for medical advice about side effects. You are also encouraged to report side effects to the FDA: visit http://www.fda.gov/medwatch or call 1-800-FDA-1088. You may also report side effects to Janssen Pharmaceuticals, Inc., at 1-800-JANSSEN (1-800-526-7736).
Please see full Prescribing Information, including Boxed Warnings, and Medication Guide.
SOURCE
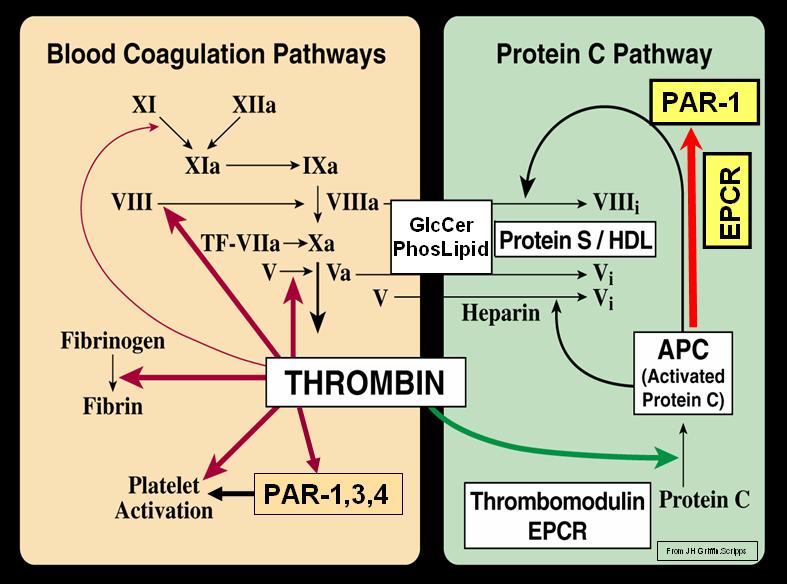
Figure-1 : Targets for anti-coagulant drugs in the coagulation cascade
Pharmacology of Rivaroxaban
Rivaroxaban, chemically an oxazolidinone derivative, is a directly acting Coagulation factor Xa inhibitor, acting on both free Factor Xa as well as that bound to the Prothrombinase complex. It has a good oral bioavailability (~ 80-100%) and a rapid onset of action, with peak plasma concentrations being achieved in about 2-4 hours of oral intake. It is about 95% plasma protein bound, with an aVd of about 50L. It is partly metabolized in liver and excreted both unchanged as well as inactive metabolites in the urine, so also in the feces. Strong CYP3A4 inhibitors like Ketoconazole, Ritonavir, Clarithromycin, Conivaptan etc can increase the pharmacodynamic effects of Rivaroxaban by a gross reduction in its metabolism. Weaker CYP3A4 inhibitors like Amiodarone, Azithromycin, Diltiazem, Dronaderone, Erythromycin, Felodipine, Quinidine, Ranolazine, Verapamil maybe used with Rivaroxaban except in renal impairment. Similarly, enzyme inducers like Rifampicin can decrease the plasma concentrations of Rivaroxaban.
Indications : Prophylaxis of stroke and systemic embolism in patients of atrial fibrillation, treatment and prevention of Deep Vein Thrombosis (DVT) and Pulmonary Embolism (PE).
Dosage : 10-20 mg with or without food, depending on the indication.
Adverse Effects : As with any other anticoagulant, an increased risk of bleeding. An increased risk of stroke after discontinuation of the drug in atrial fibrillation, and spinal and epidural hematomas.
Therapeutic monitoring : Both Dabigatran and Rivaroxaban do not mandate a therapeutic monitoring clinically, as in the case of Warfarin. Moreover, both Prothrombin Time (PT) as well as the International Normalized Ratio (INR) are not suitable to measure the pharmacodynamic profile of Rivaroxaban for various reasons1. Development of novel methods of assays, for instance Anti Factor Xa assay which utilizes rivaroxaban containing plasma calibrators, may provide optimal therapeutic monitoring modalities for Rivaroxaban in the future.
Figure – 2 : PT and aPTT dependent on plasma concentration of anticoagulant drugs.
(A) rivaroxaban (experimental data from internal studies);
(B) DX-9065a (experimental data from the literature, and
(C) ximelagatran (experimental data for PT and aPTT from the literature. aPTT, activated partial thromboplastin time; INR, international normalized ratio; PT, prothrombin time.
There is some concern regarding a spurious rise in the INR values if a patient stabilized on warfarin is switched over to Rivaroxaban. This concern is ill-founded since it is already mentioned above that INR is not a suitable investigation to give an indication of Rivaroxaban pharmacodynamics. Moreover, no suitable litrerature is available which can explain the rise in INR values on Rivaroxaban administration. It may require some additional clinical studies to throw some light on this clinical anomaly.
Figure-3 : Annualized Incidence of Complications of Rivaroxaban
REFERENCE
- Lindhoff-Last et al. Assays for measuring Rivaroxaban : Their suitability and Limitations. Ther Drug Monitoring Dec 2010 (32, Issue 6): 673-79.
RESOURCES
Burghaus R, Coboeken K, Gaub T, Kuepfer L, et al. (2011) Evaluation of the Efficacy and Safety of Rivaroxaban Using a Computer Model for Blood Coagulation. PLoS ONE 6(4): e17626. doi:10.1371/journal.pone.0017626
http://www.plosone.org/article/info:doi/10.1371/journal.pone.0017626
Coumadin
Copyright © McGraw-Hill Education, LLC. All rights reserved.
Hurst’s The Heart > Part 6. Rhythm and Conduction Disorders > Chapter 40. Atrial Fibrillation, Atrial Flutter, and Atrial Tachycardia > Atrial Fibrillation > Treatment > Anticoagulation > Antithrombotic Agents >
Rivaroxaban
Burghaus R, Coboeken K, Gaub T, Kuepfer L, et al. (2011) Evaluation of the Efficacy and Safety of Rivaroxaban Using a Computer Model for Blood Coagulation. PLoS ONE 6(4): e17626. doi:10.1371/journal.pone.0017626
http://www.plosone.org/article/info:doi/10.1371/journal.pone.0017626
Other articles published on this Open Access Online Scientific Journal include the following:
Xarelto (Rivaroxaban): Anticoagulant Therapy gains FDA New Indications and Risk Reduction for: (DVT) and (PE), while in use for Atrial fibrillation increase in Gastrointestinal (GI) Bleeding Reported