On Devices and On Algorithms: Arrhythmia after Cardiac Surgery Prediction and ECG Prediction of Paroxysmal Atrial Fibrillation Onset
Author, and Content Consultant to e-SERIES A: Cardiovascular Diseases: Justin Pearlman, MD, PhD, FACC
and
Article Curator: Aviva Lev-Ari, PhD, RN
Cleveland Clinic research spurs a device that could predict arrhythmia after cardiac surgery
April 30, 2013 9:03 am by Deanna Pogorelc |

Heart doctors at the Cleveland Clinic hope to give doctors a way to tell which patients might develop arrhythmia after cardiac surgery.
Atrial fibrillation (AFIB) is one of the most common complications of heart surgeries, and also occurs as a complication of elevated alcohol use, high blood pressure, valve disease or thyroid disease. Atrial fibrillation consists of the round parts of the Valentine heart (the atria) shivering chaotically instead of beating rhythmically. Atrial fibrillation is a common arrhythmia, eventually affecting 20% of adults. There are 3 varieties: paroxysmal (intermittent), persistent (continual) and permanent (unremitting). When AFIB lasts longer than 24-48 hours the risk of forming a blood clot in the atria rises, which in turn can cause a stroke or a heart attack. AFIB often results in fast heart rates which may cause low blood pressure and its possible consequences (organ injury, heart attack). Also, prolonged fast rates weaken the heart (reversible rate-related cardiomyopathy), which can persist for months after regaining target ranges for the heart rates (target for rate control is 60-80/minute instead of the fast rates of 100-180/min that are common with untreated AFIB).
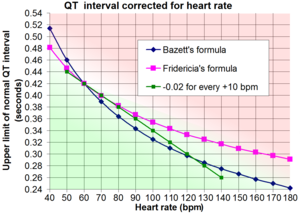
A scoring system (CHADS2) can predict who may suffer from a stroke due to AFIB that lasts >24-48 hours, and in particular, who may benefit from longterm anticoagulation (blood thinners to interfere with clot formation). A pill-in-the-pocket can stop AFIB within hours. Amiodarone, a highly toxic medication (10% long-term uses face side effects of serious damage to liver, lung, thyroid or eyes), is often prescribed “off-label” (without FDA endorsement) because it is 70% effective in preventing AFIB recurrence, and it has less anticontractility (weakening of the strength of heart beats) than most other rhythm medications. Then next most effective medication for suppression of AFIB long-term is sotalol, which reduces the strength of heart contraction (may not be tolerated by patients with severe heart failure) and it prolongs QT interval of repolarization after each heartbeat, a risk factor for a deadly rhythm called torsades de pointes. Interventional cures (“AFIB ablation”) have been developed to prevent recurrences.
Predicting AFIB may have several benefits: (1) potentially, earlier use of pill-in-the-pocket could prevent episodes rather that wait for them to occur, get noticed, and then treated, as only ~50% of AFIB episodes are noticed by the patient, according to electrographic monitor reports; (2) surrogate endpoint (prediction of onset) may offer useful guidance as to sufficiency of a suppressive therapy to enable lower dosing of toxic treatments; (3) surrogate endpoint (prediction of onset) may offer useful guidance as to sufficient lowering of alohol intake, sufficient control of blood pressure, sufficient control of thyroid abnormalities, and other prevention opportunities; (4) surrogate endpoints may facilitate AFIB ablation.
Work done in the lab of Dr. C. Allen Bashour indicated that most patients who experience atrial fibrillation after heart surgery show clues beforehand in the form of subtle changes in their ECG readings that aren’t detected with the way they’re monitored now.
Rindex Medical is commercializing a tool that would enable physicians to predict which patients will experience AF so they can receive prophylactic treatment before it occurs.
“Right now they basically guess, or treat everyone prophylactically,” said co-founder Alex Arrow. “Some clinicians say they have an intuition about who will get it, but it’s mostly guesswork.”
Rindex’s A-50 AF Prediction System uses algorithms developed at the Clinic to analyze a patient’s ECG signals through 17 steps and produce a score, from 1 to 100, of how likely that patient is to experience AF. Arrow said the final product will be a touch-screen monitor that displays a score and tracks the score over a nine-hour period.
The Redwood City, California, company has been issued the first of its patents for the device and the exclusive license from Cleveland Clinic to develop the technology. Self-funded by Arrow and co-founders Denis Hickey and Lucas Fairfield, Rindex has a working prototype and is making progress on preparations for its 510(k) application. Arrow said the company shouldn’t need to raise a series A until it’s ready for a clinical trial.
Many other research groups have explored ways to predict AF in its various forms from natriuretic peptides to ECG changes, but no method has been established as reliably for this purpose.
Dec 13, 2012
ECG predicts atrial fibrillation onset
Atrial fibrillation (AF), the most common cardiac arrhythmia, is categorized by different forms. One sub-type is paroxysmal AF (PAF), which refers to episodes of arrhythmia that generally terminate spontaneously after no more than a few days. Although the underlying causes of PAF are still unknown, it’s clear that predicting the onset of PAF would be hugely beneficial, not least because it would enable the application of treatments to prevent the loss of sinus rhythm.
Many research groups are tackling the issue of predicting the onset of PAF. Now, however, researchers in Spain have developed a method that assesses the risk of PAF at least one hour before its onset. To date, the approach has not only successfully discriminated healthy individuals and PAF patients, but also distinguished patients far from and close to PAF onset (Physiol. Meas. 33 1959).
“The ability to assess the risk of arrhythmia at least one hour before its onset is clinically relevant,” Arturo Martinez from the University of Castilla-La Mancha told medicalphysicsweb. “Our method assesses the P-wave feature time course from single-lead long-term ECG recordings. Using a single ECG lead reduces the computational burden, paving the way for a real-time system in future.”
Analysing sinus rhythm
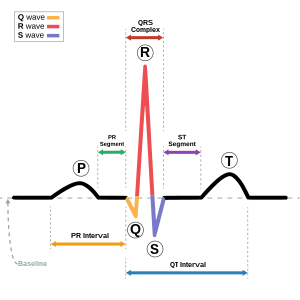
If the heart is beating normally, the sinus rhythm observed on an ECG will contain certain generic features, such as a P-wave that reflects the atrial depolarization and a large characteristic R peak flanked by two minima representing the depolarization of the heart’s right and left ventricles. If an irregular heart beat is suspected, an ECG will be used and typical findings include the absence of a P-wave.
“We hypothesized that different stages of AF could be identified when analysing long-term recordings extracted from patients prone to AF,” commented Martinez. “Our method differs to others in that we also use just one single lead to detect small differences in features from the P-wave time course.”
P for paroxysmal
Martinez and his collaborators, Raul Alcaraz and Jose Rieta, studied 24-hour Holter ECG recordings from 24 patients in whom PAF had been detected for the first time. For each patient, the longest sinus rhythm interval in the recording was selected, and the two hours preceding the onset of PAF were analysed. These readings were compared with those from 28 healthy individuals. In all cases, only the trace from the V1 ECG lead was considered.
A major challenge for the researchers was to extract the P-wave from the baseline noise. To overcome this, they used an automatic delineator algorithm based on a phasor transform that determines the precise time point relating to the onset, peak and offset of the P-wave. The authors described this algorithm in a previous research paper (Physiol. Meas. 31 1467).
“All of the recordings in our study were visually supervised by expert cardiologists who corrected the P-wave fiducial points when needed,” said Martinez. “Even in the presence of noise, which generated an incredible amount of P-wave distortion, our delineator provided location errors lower than 8 ms.”
In order to assess which time course features might be useful to predict the onset of PAF, the researchers analysed a number of variables. First, they examined factors representing the duration of the P-wave (Pdur), such as the distance between the P-wave onset and peak (Pini) and the distance between the P-wave peak and its offset (Pter). They then studied factors relating P- to R-waves, such as the distance between the two waves’ peaks (PRk) and, finally, beat-to-beat P-wave factors, such as the distance between two consecutive P-wave onset points (PPon).
“The most remarkable trends were provided by the features measuring P-wave duration,” report the authors in their paper. “Pduridentified appropriately 84.21% of all the analysed patients, obtaining a discriminant accuracy of 90.79% and 83.33% between healthy subjects and PAF patients far from PAF and close to PAF, respectively. The metrics related to the PR interval showed the most limited ability to identify patient groups.”
About the author
Jacqueline Hewett is a freelance science and technology journalist based in Bristol, UK.
http://medicalphysicsweb.org/cws/article/research/51820
Original Article
Application of the phasor transform for automatic delineation of single-lead ECG fiducial points.
Martínez A, Alcaraz R, Rieta JJ.
Source
Innovation in Bioengineering Research Group, University of Castilla La Mancha, Spain. arturo.martinez@uclm.es
Abstract
This work introduces a new single-lead ECG delineator based on phasor transform. The method is characterized by its robustness, low computational cost and mathematical simplicity. It converts each instantaneous ECG sample into a phasor, and can precisely manage P and T waves, which are of notably lower amplitude than the QRS complex. The method has been validated making use of synthesized and real ECG sets, including the MIT-BIH arrhythmia, QT, European ST-T and TWA Challenge 2008 databases. Experiments with the synthesized recordings reported precise detection and delineation performances in a wide variety of ECGs, with signal-to-noise ratios of 10 dB and above. For real ECGs, the QRS detection was characterized by an average sensitivity of 99.81% and positive predictivity of 99.89%, for all the analyzed databases (more than one million beats). Regarding delineation, the maximum localization error between automatic and manual annotations was lower than 6 ms and its standard deviation was in agreement with the accepted tolerances for expert physicians in the onset and offset identification for QRS, P and T waves. Furthermore, after revising and reannotating some ECG recordings by expert cardiologists, the delineation error decreased notably, becoming lower than 3.5 ms, on average, and reducing by a half its standard deviation. This new proposed strategy outperforms the results provided by other well-known delineation algorithms and, moreover, presents a notably lower computational cost.
SOURCES:
MIT-BIH Polysomnographic Database
This database is described in
Ichimaru Y, Moody GB. Development of the polysomnographic database on CD-ROM. Psychiatry and Clinical Neurosciences 53:175-177 (April 1999).
Please cite this publication when referencing this material, and also include the standard citation for PhysioNet:
Goldberger AL, Amaral LAN, Glass L, Hausdorff JM, Ivanov PCh, Mark RG, Mietus JE, Moody GB, Peng C-K, Stanley HE. PhysioBank, PhysioToolkit, and PhysioNet: Components of a New Research Resource for Complex Physiologic Signals. Circulation 101(23):e215-e220 [Circulation Electronic Pages; http://circ.ahajournals.org/cgi/content/full/101/23/e215]; 2000 (June 13).
 The MIT-BIH Polysomnographic Database is a collection of recordings of multiple physiologic signals during sleep. Subjects were monitored in Boston’s Beth Israel Hospital Sleep Laboratory for evaluation of chronic obstructive sleep apnea syndrome, and to test the effects of constant positive airway pressure (CPAP), a standard therapeutic intervention that usually prevents or substantially reduces airway obstruction in these subjects. The database contains over 80 hours’ worth of four-, six-, and seven-channel polysomnographic recordings, each with an ECG signal annotated beat-by-beat, and EEG and respiration signals annotated with respect to sleep stages and apnea. For further information, see Signals and Annotations.
The MIT-BIH Polysomnographic Database is a collection of recordings of multiple physiologic signals during sleep. Subjects were monitored in Boston’s Beth Israel Hospital Sleep Laboratory for evaluation of chronic obstructive sleep apnea syndrome, and to test the effects of constant positive airway pressure (CPAP), a standard therapeutic intervention that usually prevents or substantially reduces airway obstruction in these subjects. The database contains over 80 hours’ worth of four-, six-, and seven-channel polysomnographic recordings, each with an ECG signal annotated beat-by-beat, and EEG and respiration signals annotated with respect to sleep stages and apnea. For further information, see Signals and Annotations.
The database consists of 18 records, each of which includes 4 files:
(*) You may follow these links to view the signals and st annotations using either WAVE (under Linux, SunOS, or Solaris) or WVIEW (under MS-Windows). To do so successfully, you must have configured your browser to use wavescript (for WAVE) or wvscript (for WVIEW) as a helper application, as described in the WAVE User’s Guide(see the section titled WAVE and the Web) and in Setting up WVSCRIPT.
Andrew Walsh observed that the calibration originally provided for the BP signal of record slp37 is incorrect (since it yielded negative BPs). slp37.hea now contains an estimated BP calibration that yields more plausible BPs; these should not be regarded as accurate, however, since there is no independent calibration standard available for this recording.
Finding events of electrocardiogram and arterial blood pressure signals via discrete wavelet transform with modified scales.
Ghaffari A, Homaeinezhad MR, Akraminia M, Davaeeha M.
Source
Cardiovascular Research Group, Department of Mechanical Engineering, K. N. Toosi University of Technology, Tehran, Iran.
Abstract
A robust electrocardiogram (ECG) wave detection-delineation algorithm that can be applied to all ECG leads is developed in this study on the basis of discrete wavelet transform (DWT). By applying a new simple approach to a selected scale obtained from DWT, this method is capable of detecting the QRS complex, P-wave, and T-wave as well as determining parameters such as start time, end time, and wave sign (upward or downward). In the proposed method, the selected scale is processed by a sliding rectangular window of length n and the curve length in each window is multiplied by the area under the absolute value of the curve. In the next step, an adaptive thresholding criterion is conducted on the resulted signal. The presented algorithm is applied to various databases including the MIT-BIH arrhythmia database, European ST-T database, QT database, CinC Challenge 2008 database as well as high-resolution Holter data gathered in the DAY Hospital. As a result, the average values of sensitivity and positive prediction Se = 99.84 per cent and P+ = 99.80 per cent were obtained for the detection of QRS complexes with an average maximum delineation error of 13.7, 11.3, and 14.0 ms for the P-wave, QRS complex, and T-wave respectively. The presented algorithm has considerable capability in cases of a low signal-to-noise ratio, high baseline wander, and in cases where QRS complexes and T-waves appear with abnormal morphologies. Especially, the high capability of the algorithm in the detection of the critical points of the ECG signal, i.e. the beginning and end of the T-wave and the end of the QRS complex was validated by the cardiologist and the maximum values of 16.4 and 15.9 ms were recognized as absolute offset error of localization respectively. Finally, in order to illustrate an alternative capability of the algorithm, it is applied to all 18 subjects of the MIT-BIH polysomnographic database and the end-systolic and end-diastolic points of the blood pressure waveform were extracted and values of sensitivity and positive prediction Se = 99.80 per cent and P+ = 99.86 per cent were obtained for the detection of end-systolic, end-diastolic pulses.
http://www.ncbi.nlm.nih.gov/pubmed/20225455
Original Article
A robust wavelet-based multi-lead electrocardiogram delineation algorithm
- A. Ghaffaria, b,
- M.R. Homaeinezhada, b,
 ,
,  ,
, - M. Akraminiaa, b,
- M. Ataroda, b,
- M. Daevaeihac
- a Department of Mechanical Engineering, K.N. Toosi University of Technology, Tehran, Iran
- b CardioVascular Research Group (CVRG), Iran
- c Non-invasive Cardiac Electrophysiology Laboratory, DAY Hospital, Tehran, Iran
Abstract
A robust multi-lead ECG wave detection-delineation algorithm is developed in this study on the basis of discrete wavelet transform (DWT). By applying a new simple approach to a selected scale obtained from DWT, this method is capable of detecting QRS complex, P-wave and T-wave as well as determining parameters such as start time, end time, and wave sign (upward or downward). First, a window with a specific length is slid sample to sample on the selected scale and the curve length in each window is multiplied by the area under the absolute value of the curve. In the next step, a variable thresholding criterion is designed for the resulted signal. The presented algorithm is applied to various databases including MIT-BIH arrhythmia database, European ST-T Database, QT Database, CinC Challenge 2008 Database as well as high resolution Holter data of DAY Hospital. As a result, the average values of sensitivity and positive predictivity Se = 99.84% and P+ = 99.80% were obtained for the detection of QRS complexes, with the average maximum delineation error of 13.7 ms, 11.3 ms and 14.0 ms for P-wave, QRS complex and T-wave, respectively. The presented algorithm has considerable capability in cases of low signal-to-noise ratio, high baseline wander, and abnormal morphologies. Especially, the high capability of the algorithm in the detection of the critical points of the ECG signal, i.e. the beginning and end of T-wave and the end of the QRS complex was validated by cardiologists in DAY hospital and the maximum values of 16.4 ms and 15.9 ms were achieved as absolute offset error of localization, respectively.
Abbreviations
- ACL, area-curve length;
- ECG, electrocardiogram;
- DWT, discrete wavelet transform;
- QTDB, QT database;
- MITDB, MIT-BIH arrhythmia database;
- TWADB, T-wave alternans database;
- CSEDB, common standards for electrocardiography database;
- EDB, European ST-T database;
- P+, positive predictivity (%);
- Se,sensitivity (%);
- FIR, finite-duration impulse response;
- LE, location error;
- CHECK#0, procedure of evaluating obtained results using MIT annotation files;
- CHECK#1, procedure of evaluating obtained results consulting with a control cardiologist;
- CHECK#2, procedure of evaluating obtained results consulting with a control cardiologist and also at least with 3 residents
Keywords
- ECG delineation;
- Discrete wavelet transform;
- Variable threshold;
- Validation
Figures and tables from this article:
- Fig. 5. Procedure of detecting and delineating of P and T-waves using ACL signal between two successive QRS complexes. (a) Simultaneously depiction of ACL, original ECG and the corresponding selected DWT scale, (b) QRS delineation, and (c) P and T-waves delineation.

Volume 31, Issue 10, December 2009, Pages 1219–1227
http://www.sciencedirect.com/science/article/pii/S1350453309001647
Other related articles published on this Open Access Online Scientific Journal include the following:
Sustained Cardiac Atrial Fibrillation: Management Strategies by Director of the Arrhythmia Service and Electrophysiology Lab at The Johns Hopkins Hospital http://pharmaceuticalintelligence.com/2012/10/16/sustained-cardiac-atrial-fibrillation-management-strategies-by-director-of-the-arrhythmia-service-and-electrophysiology-lab-at-the-johns-hopkins-hospital/
Acute Chest Pain/ER Admission: Three Emerging Alternatives to Angiography and PCI http://pharmaceuticalintelligence.com/2013/03/10/acute-chest-painer-admission-three-emerging-alternatives-to-angiography-and-pci/
Dilated Cardiomyopathy: Decisions on implantable cardioverter-defibrillators (ICDs) using left ventricular ejection fraction (LVEF) and Midwall Fibrosis: Decisions on Replacement using late gadolinium enhancement cardiovascular MR (LGE-CMR)
http://pharmaceuticalintelligence.com/2013/03/10/dilated-cardiomyopathy-decisions-on-implantable-cardioverter-defibrillators-icds-using-left-ventricular-ejection-fraction-lvef-and-midwall-fibrosis-decisions-on-replacement-using-late-gadolinium/
Ablation Devices Market to 2016 – Global Market Forecast and Trends Analysis by Technology, Devices & Applications
http://pharmaceuticalintelligence.com/2012/12/23/ablation-devices-market-to-2016-global-market-forecast-and-trends-analysis-by-technology-devices-applications/
http://pharmaceuticalintelligence.com/2012/08/17/expected-new-trends-in-cardiology-and-cardiovascular-medical-devices/