English: Amino acid sequence of the molecule of the brain natriuretic peptide (BNP) 32 (functional). Português: Sequência de aminoácidos da molécula de BNP 32 (funcional). (Photo credit: Wikipedia)
Assessing Cardiovascular Disease with Biomarker
Author and Curator: Larry H Bernstein, MD, FCAP
A Changing expectation from cardiac biomarkers.
This article on Assessing Cardiovascular Disease with Biomarkers will demonstrate the unique role in the discipline evolution that each of the following biomarkers has played in our understanding of CVD risk:
The article is introduced with an entire section on the evolution of our knowledge of cardiac biomarkers and how concepts from thermodynamics have transformed
the way we investigate biochemical mechanisms, and how we have gone from a macro- to a micro- landscape of high complexity. The same concepts from physics
have also transformed the mathematical stage upon which we model data. BIG Data is not just about business! We have entered a new domain of knowledge enabling.
(1) Enzymes and Isoenzymes
- AST, ALT, LD, alkaline phosphatase
- Isoenzymes evolution and genomic loci for polypeptides
- Emergence of pathway divergence and regulation from gene-loci peptide changes
- A reflection to implications for biomarkers and therapeutic development based on critical links
(2) Natriuretic Peptides
- Cause of Death: silent cardiac target organ damage (cTOD) (no so sign of cardiac disease)
- B Type natriuretic peptide in evolution of CHF
- 2D and Doppler echocardiography and BNP serum level
- Amino terminal pro B-type Natriuretic Peptide
- Renal Effect on NT-proBNP
- pro-atrial natriuretic peptide
(3) CRP as Biomarker, theory that lowering the C-reactive protein (CRP) level with statin therapy is predictive of cardiovascular outcomes independent of lowering the low-density lipoprotein (LDL) cholesterol level
(4) CRP as an Inflammatory Agent
Acute phase reaction is a systemic response: physiological condition in the beginning of an inflammatory process.
(5) troponins and hs-troponins (I, T)
(6) New Candidate Biomarkers for NSTEMI
(7) Guidelines for Cardiovascular Risk Assessment
(8) Statistical Issues to be Resolved
Historical perspective
The use of cardiac markers emerged in the late 1950s, when the physician was faced with the problem of a patient with recent onset of squeezing, crushing, or heaviness in the chest, with or without a Q-wave or definitive ST elevation (acute injury), and perhaps a non specific elevation of the neutrophil count. A medical student at Albert Einstein Medical school at the time, Arthur Karmen identified the first enzymatic test for acute myocardial infarct (MI), serum glutamic oxaloacetic acid transaminase (SGOT), which is renamed Aspartate Aminotransferase (AST) in a seminal study with Wroblewski and LaDue[1]. The enzyme is ubiquitous, and the authors published another observation that the SGPT, now referred to as Alanine Aminotransferase, has a greater specific activity in liver and myocardial infarct can be distinguished from necrotizing liver disease by using AST and ALT. These two enzymes were among the three enzymes,with lactate dehydrogenase (LD) and alkaline phosphatase that appeared on the original Technicon (later Siemens) SMA-12 profile, prior to the designated panels used today. At that time it was common for the pathologist to stain the heart lesion at autopsy in identifying the “ischemic necrosis” postmortem.
In 1957 Hunter and Markert described the five isoenzymes of lactate dehydrogenase, the most anodal migrating pattern was associated with heart and the most cathodal isoenzymes with liver, the five bands being combinations of two subunits. These were described as different variants of the same enzyme having identical functions, but different tissue specific patterns, such that, enzyme variants have altered gene loci that results in an amino acid change but catalyze the same reaction. When mutation modifies the enzymatic catalysis, or its pattern of gene expression, then any of two (or more) variants may be favoured by natural selection and become specialized to different cell environments. His group suggested that a single gene might somehow encode an array of isozymes differing in “structural variations,” a concept that seems to presage our current understanding of alternative mRNA splicing and post-translational protein modification. A former student of George beadle, he transformed the “concept of one gene one enzyme” to “one gene one polypeptide”. By treating the enzyme with denaturing agents it was learned that LDH is a tetramer of two types of polypeptide chains (Appella and Markert, 1961). Thus the multiple-gene hypothesis was partially correct: Two different LDH subunits, each encoded by a distinct gene, re-sort themselves in various tetrameric combinations to give rise to five different isozymes (Markert, 1963). During the succeeding years Markert and his students and postdocs elucidated how the study of isozymes could contribute to our understanding of the biochemical variation that underlies cell differentiation and evolution, culminating in the new perspective presented in a Science paper (Markert et al., 1975) entitled “Evolution of a Gene.”
In the early 1960’s Nathan Kaplan postulated that the major LD-isoenzyme types were associated with fundamental differences in the metabolism of the tissue of origin, either catabolic (heart) or anabolic (liver), and skeletal muscle would appear to be in the same class as liver (ignore the ratio of fast and slow twitch), which was elaborated on further by studies of the flight wing patterns of birds. These isoenzymes not only had different migration in an electrophoretic field and could be separated chromatographically, but they also had different kinetic properties. They all have the same Km, but the purified heart LD is inhibited by a ternary complex of the enzyme, the NAD, and pyruvate that forms, slowing the reaction in the forward direction (pyruvate to lactate).
At about the same time, Masahiro Chiga discovered that adenylate kinase, the enzyme that converts ATP to ADP, from skeletal muscle can be inhibited by inorganic S (myokinase), which led Bernstein and Russell to publish on the identification of adenylate kinase from heart in myocardial infarction using sulfhydryl inhibition in J Molec Cellular Cardiology. Burton Sobel in the early 1970s showed that CK and the MB isoenzyme of CK, which has a more rapid increase and disappearance than the AST or LD , could be used to estimate the amount of cardiac damage in MI. This meant that a test could be done at any time of day or night with a result in less than an hour. He applied this to determining whether the extent of infarction was an important determinant of prognosis after myocardial infarction and furthermore, whether the extent of infarction could be modified by interventions that reduce myocardial oxygen requirements or increase myocardial oxygen supply. This work has had a major impact on how patients with acute myocardial infarction are treated and led to a reduction of mortality secondary to treatments, such as thrombolysis, that were validated initially with the methods developed. This led to an immunoassay for CK isoenzyme MB that was offered by Roche on the Cobas analyzer, and by Dupont on the ‘aca’. What emerged is a new imperative to reduce infarct size under the rubrick – “Time is Muscle”.
References
- Karmen Arthur, Wróblewski Felix, LaDue John S. TRANSAMINASE ACTIVITY IN HUMAN BLOOD. J Clin Invest. 1955; 34(1):126–133.
- LADUE JS, WROBLEWSKI F, KARMEN A. Serum glutamic oxaloacetic transaminase activity in human acute transmural myocardial infarction. Science 1956; 75(11).
- Hunter, R. L. and C.L. Merkert. (1957) Histochemical demonstration of enzymes separated by zone electrophoresis in starch gels. Science 125: 1294-1295.
- Bernstein L, Kerrigan M, Maisel H. Lactic dehydrogenase isoenzymes in lens and cornea. Exp Eye Res 1965; 5(3):999-1005. ICID: 844979
- Nathan O. Kaplan Papers. MSS 0099. UC San Diego::Mandeville Special Collections Library.
Enzyme-coenzyme-substrate complex. of pyridine nucleotide depend. dehydrogenases 1958. box 39, folder 5.
Enzymatic studies with analogues of diphosphopyridine nucleotide 1959. box 39, folder 12.
Heterogeneity of the lactic dehydrogenases of new-born and adult rat heart as determined with enzyme analogs 1961. box 39, folder 37.
Regulatory effects of enzyme action 1961. box 39, folder 38.
Inhibition of dehydrogenase reactions by a substance formed from reduced dpn 1961. box 39, folder 40.
Lactic dehydrogenases: functions of the two types 1964. box 39, folder 67.
Lactate dehydrogenase – structure and function. 1964. box 40, folder 4.
Role of the two types of lactic dehydrogenases 1964. Box 40, folder 9.
Structural and functional properties of h and m subunits of lactic dehydrogenase 1965. Box 40, folder 12.
- Bernstein LH, Everse J, Shioura N, Russell PJ. Detection of cardiac damage using a steady state assay for lactate dehydrogenase isoenzymes in serum. J Mol Cell Cardiol 1974; 6(4):297-315. ICID: 825597
- Bernstein LH, Everse J. Determination of the isoenzyme levels of lactate dehydrogenase. Methods Enzymol 1975; 41 47-52.
- Bernstein LH. Automated kinetic determination of lactate dehydrogenase isoenzymes in serum. Clin Chem 1977; 23(10):1928-1930. ICID: 825616
- Bernstein LH, Scinto P. Two methods compared for measuring LD-1/total LD activity in serum. Clin Chem 1986; 32(5):792-796. ICID: 825581
- Shell WE, Kjekshus JK, Sobel BE: Quantitative assessment of the extent of myocardial infarction in the conscious dog by means of analysis of serial changes in serum creatine phosphokinase activity. J Clin Invest 50:2614-2626, 1971.
- Bergmann SR, Fox KAA, Ter-Pogossian MM, Sobel BE (Washington University), Collen D (University of Leuven): Clot-selective coronary thrombolysis with tissue-type plasminogen activator. Science 220:1181-1183, 1983.
- Van de Werf F, Ludbrook PA, Bergmann SR, Tiefenbrunn AJ, Fox KAA, de Geest H, Verstraete M, Collen D, Sobel BE: Coronary thrombolysis with tissue-type plasminogen activator in patients with evolving myocardial infarction. N Engl J Med 310:609-613, 1984.
- Adan J, Bernstein LH, Babb J. Can peak CK-MB segregate patients with acute myocardial infarction into different outcome classes? Clin Chem 1985; 31(2):996-997. ICID: 844986
- Bernstein LH, Reynoso G. Creatine kinase B-subunit activity in serum in cases of suspected myocardial infarction: a prediction model based on the slope of MB increase and percentage CK-MB activity. Clin Chem 1983; 29(3):590-592. ICID: 825549
- Bernstein LH, Horenstein JM, Sybers HB, Russell PJ. Adenylate kinase in human tissue. II. Serum adenylate kinase and myocardial infarction. J Mol Cell Cardiol 1973; 5(1):71-85. ICID: 825590
A Metabolic Functional Meaning of Existence of Isoenzymes
There are many examples of isozymes, such as glucokinase, a variant of hexokinase which is not inhibited by glucose 6-phosphate. It has different regulatory features and lower affinity for glucose (compared to other hexokinases). Alkaline and acid phosphatase isoenzymes were used briefly for a time in clinical diagnostics. These isoenzymes are oligomeric proteins that have distinct subunits that affect their binding with substrate. A distinctive type of protein that can form two or more different homo-oligomers, comes apart and changes shape to convert between forms is called a morpheein. The alternate shape may reassemble to a different oligomer, and the shape of the subunit dictates which oligomer is formed. Morpheeins can interconvert between forms under physiological conditions and can exist as an equilibrium of different oligomers. Features of morpheeins can be exploited for drug discovery. A small molecule compound can shift the equilibrium either by blocking or favoring formation of one of the oligomers. The equilibrium can be shifted using a small molecule that has a preferential binding affinity for only one of the alternate morpheein forms. This introduces the concept of allostericity. Most allosteric effects can be explained by a model put forth by Monod, Wyman, and Changeux, and also by a model described by Koshland, Nemethy, and Filmer. Both postulate that enzyme subunits exist in one of two conformations, tensed (T) or relaxed (R), and that relaxed subunits bind substrate more readily than those in the tense state. This concept provides a foundation for another generation of biomarkers than was the focus of the 20th century, and only has been investigated since the 1980’s, and takes another dimension after the completion of the Human Genome Project, opening a “Pandora’s box”. This moved biomedical science forward into an emerging field of ‘OMICs’, which tied small molecules into regulatory processes, transcription, and the possibility of identifying new biomarkers and developing new biomolecules that could modify disease progression.
References
- Bu Z, Callaway DJ. “Proteins MOVE! Protein dynamics and long-range allostery in cell signaling”. Adv in Protein Chemistry and Structural Biology 2011; 83: 163–221. doi:10.1016/B978-0-12-381262-9.00005-7. PMID 21570668.
- Monod J, Wyman J, Changeux JP. On the nature of allosteric transitions:A plausible model. J Mol Biol, May 1965; 12:88-118.
- Koshland DE, Némethy G, Filmer D. Comparison of experimental binding data and theoretical models in proteins containing subunits. Biochemistry. Jan 1966; 5(1):365-8
- Jaffe EK. “Morpheeins – a new structural paradigm for allosteric regulation”. Trends Biochem Sci 2005; 30(9): 490–497. doi:10.1016/j.tibs.2005.07.003. PMID 16023348.
- Huang Z, Zhu L, Cao Y, Wu G, Liu X, et al. ASD: a comprehensive database of allosteric proteins and modulators. Nucleic Acids Res 2011; 39: D663-669
Fundamental Transformative Concepts Carried Over from Physics to Biomolecular Processes.
A colleague once noted that we are learning more and more about less and less. This is the remarkable evolution of our thinking from macrostates to microstates and segmentation of processes, further leading us to exploration of interactions between states. This has required a breakdown and a repeated remodeling or resynthesis of ideas based on new findings in science. It has gradually driven medicial science to a greater dependence on chemistry and physics in underlying principle. We can better envision the mechanism of evolution from the concepts put forth.
In 1824 Sadi Carnot published the concept that heat is lost in the conversion into work, using the term “caloric”, equivalent to entropy in the second law of thermodynamics. Clausius then develops the concepts of interior work in 1854, i.e. that “which the atoms of the body exert upon each other”, and exterior work, i.e. that “which arise from foreign influences [to] which the body may be exposed”, anticipating the concept of entropy. He enunciated the passage of the quantity of heat Q from the temperature T1 to the temperature T2 has the equivalence-value entropy, symbolized by S : dS = Q (1/T2 – 1/T1), which led to his 1865 statement on irreversible heat loss: I propose to name the quantity S the entropy of the system, after the Greek word [τροπη trope], the transformation. I have deliberately chosen the word entropy to be as similar as possible to the word energy.” In 1876, physicist J. Willard Gibbs, building on the work of Clausius, Hermann von Helmholtz and others, proposed that the measurement of “available energy” ΔG in a thermodynamic system could be mathematically accounted for by subtracting the “energy loss” TΔS from total energy change of the system ΔH, and in 1877, Ludwig Boltzmann formulated the alternative definition of entropy S defined as:
S = kBlnΩ
where
kB is Boltzmann’s constant and
Ω is the number of microstates consistent with the given macrostate.
An analog to thermodynamic entropy is information entropy. Claude Shannon set out to mathematically quantify the statistical nature of “lost information” in phone-line signals and developed a concept of information entropy, a fundamental cornerstone of information theory. The close similarity between his new quantity and earlier work in thermodynamics is attributed to a visit and discussion with Jon von Neumann in 1949. Shannon then called the “measure of uncertainty” or attenuation in phone-line signals with reference to his new information theory. This led to the elucidation of a signal (as opposed to noise, by Solomon Kullback, which became the basis for the measure of an optimum diagnostic decision point of a laboratory test by Bernstein and Rudolph, related to Eugene Rypka’s “Syndromic Clustering”. The loop was closed by the Japanese mathematician Akaike, who brought Fisher’s statistical formulations and Kullback-Liebler distance into alignment. This is not a digression because it has been central to underlying principles in resolution in spectroscopy, and to classification of biochemical molecular features.
Although Boltzmann first linked entropy and probability in 1877, it seems the relation was never expressed with a specific constant until Max Planck first introduced k, and gave an accurate value for it (1.346×10−23 J/K, about 2.5% lower than today’s figure), in his derivation of the law of black body radiation in 1900–1901. Before 1900, equations involving Boltzmann factors were not written using the energies per molecule and the Boltzmann constant, but rather using a form of the gas constant R, and macroscopic energies for macroscopic quantities of the substance. The iconic terse form of the equation S = k log W on Boltzmann’s tombstone is in fact due to Planck, not Boltzmann. Planck actually introduced it in the same work as his h. Planck noted in his 1920 Nobel Prize acceptance : “:This constant is often referred to as Boltzmann’s constant, although, to my knowledge, Boltzmann himself never introduced it — a peculiar state of affairs.” The Kullback–Leibler divergence (also information divergence, information gain, relative entropy, or KLIC) is a non-symmetric measure of the difference between two probability distributions P and Q, was introduced by Solomon Kullback and Richard Leibler in 1951. KL-divergence of a model from reality may be estimated, to within a constant additive term, by a function (like the squares summed) of the deviations observed between data and the model’s predictions. When trying to fit parametrized models to data there are various estimators which attempt to minimize Kullback–Leibler divergence, such as, the familiar maximum likelihood estimator.
References
- Planck, Max (2 June 1920), The Genesis and Present State of Development of the Quantum Theory (Nobel Lecture)
- Kalinin M, Kononogov S. “Boltzmann’s Constant, the Energy Meaning of Temperature, and Thermodynamic Irreversibility”, Measurement Techniques 2005; 48 (7): 632–36, doi:10.1007/s11018-005-0195-9
- Kullback S, Leibler RA “On Information and Sufficiency”. Annals of Mathematical Statistics 1951; 22 (1): 79–86. doi:10.1214/aoms/1177729694. MR 39968.
- Kullback S (1959) Information theory and statistics (John Wiley and Sons, NY).
- Jaynes ET(1957) Information theory and statistical mechanics, Physical Review 106:620
- Jaynes ET(1957) Information theory and statistical mechanics II, Physical Review 108:171
- Burnham KP and Anderson DR. (2002) Model Selection and Multimodel Inference: A Practical Information-Theoretic Approach, Second Edition (Springer Science, New York) ISBN 978-0-387-95364-9.
- Rudolph RA, Bernstein LH, Babb J. Information induction for predicting acute myocardial infarction. Clin Chem 1988; 34(10):2031-2038. ICID: 825568
A New Imperative
Cardiovascular Biomarkers
I. BNP:
[A] Aids in the Prevention of Cardiac Events by Detecting Silent Ischemic Lesions and Selecting Patients for Imaging
12/17/12 · Emily Humphreys
- 34% of study volunteers had evidence of a cTOD. Out of all biomarkers analyzed, BNP levels were significantly higher in those with cTOD compared with those without. BNP levels were also higher in those who had more than one form of cTOD compared with those who had a single form of cTOD.
- Hs-cTnT also performed well, but BNP levels had the highest correlation to imaging data. The gold standard diagnostic tool for cardiovascular disease is imaging studies, such as echocardiography.
- It is not standard practice to investigate healthy individuals for possible cTOD and would be costly and time consuming to perform imaging on these individuals.
- Biomarkers like BNP could be used as a primary screening tool with follow-up image studies performed, if necessary.
The eventual hope is to reduce the mortality of cardiovascular diseases and prevent silent cTOD from leading to more serious and potentially life-threatening cardiac events.
References
1. Roger, V.L. (2012) ‘AHA statistical update: Heart disease and stroke statistics-2012 update. A report from the american heart association‘, Circulation, 125 (2012), (pp. e2-e220)
2. Chiuve, S.E., et al., (2006) ‘Healthy lifestyle factors in the primary prevention of coronary heart disease among men: Benefits among users and nonusers of lipid-lowering and antihypertensive medications‘ Circulation, 114 (2006), (pp. 160-167)
3.De Vreede-Swagemakers, J.J., et al. (1997) ‘Out-of-hospital cardiac arrest in the 1990s: A population-based study in the Maastricht area on incidence, characteristics and survival‘, Journal of the American College of Cardiology, 30 (1997), (pp. 1500-1505)
4. Rutter, M.K., et al. (2002) ‘Significance of silent ischemia and microalbuminuria in predicting coronary events in asymptomatic patients with type 2 diabetes‘, Journal of the American College of Cardiology, 40 (2002), (pp. 56-61)
5. Tsang, T.S., et al. (2003) ‘Prediction of risk for first age-related cardiovascular events in an elderly population: The incremental value of echocardiography‘, Journal of the American College of Cardiology, 42 (2003), (pp. 1199-1205)
6. Gosse, P., (2005) ‘Left ventricular hypertrophy—the problem and possible solutions‘,The Journal of International Medical Research, 33 (Suppl 1) (2005), (pp. 3A-11A)
7. Benjamin, E.J., et al. (1995) ‘Left atrial size and the risk of stroke and death‘ The Framingham Heart Study Circulation, 92 (4), (pp. 835-41)
8. Redfield, M.M., et al. (2003) ‘Burden of systolic and diastolic ventricular dysfunction in the community: Appreciating the scope of the heart failure epidemic‘, JAMA, 289 (2003), (pp. 194-202)
9. Nadir, M.A., et al., (2012) ‘Improving the primary prevention of cardiovascular events by using biomarkers to identify individuals with silent heart disease‘, Journal of American College of Cardiology, 60 (11), (pp. 960-968) Tags: cardiovascular biomarker, cardiovascular disease, cardiovascular risk factors, cTOD
[B] Evaluating CHF patients in the emergency department
Congestive heart failure (CHF) is a severe cardiovascular disorder seen in the Emergency Department (ED). B-type Natriuretic Peptide (BNP) is usually ordered to evaluate the CHF severity.
However, it is difficult to interpret serum BNP level when different clinical entities existed.
The aim of this study is to illustrate the correlation between serum BNP level and
- relevant clinical variables and
- further determine the role of serum BNP in different CHF patients.
High variability of serum BNP levels exists in CHF patients with weak-to-moderate correlation effects particularly on obesity and diastolic/systolic HF.
Physicians should be cautious on interpreting BNP in different CHF populations.
Open Journal of Clinical Diagnostics scirp.org
[C] NT-proBNP compared with ECHO
Comparison of N-Terminal Pro B-Natriuretic Peptide and Echocardiographic Indices in Patients with Mitral Regurgitation. Shokoufeh Hajsadeghi1, Niloufar Samiei2, Masoud Moradi3, Maleki Majid2, et al. Corresponding author email: masoud_moradi65@yahoo.com
Abstract
Introduction: Echocardiographic indices can form the basis of the diagnosis of systolic and diastolic left ventricular (LV) dysfunction in patients with Mitral regurgitation (MR). However, using echocardiography alone may bring us to a diagnostic dead-end. The aim of this study was to compare N-Terminal pro B-natriuretic peptide (BNP) and echocardiographic indices in patients with mitral regurgitation.
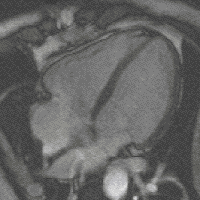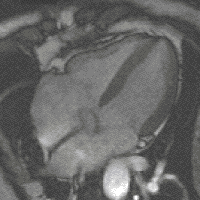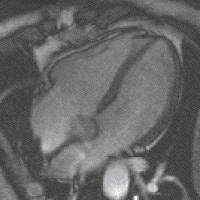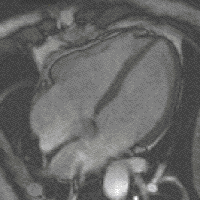
Methods: 2D and Doppler echocardiography and BNP serum level were obtained from 54 patients with organic mild, moderate and severe MR.
Results: BNP levels were increased with symptoms in patients with mitral regurgitation (NYHAI: 5.7 ± 1.1, NYHAII: 6.9 ± 1.5, NYHAIII: 8.3 ± 2 pg/ml, P , 0.001). BNP plasma level were significantly correlated with MPI (myocardial performance index)(r = 0.399, P = 0.004), and following echocardiographic indices: LVEDV (r = 0.45, P , 0.001), LVESV (r = 0.54, P , 0.001), LVEDD (r = 0.48, P , 0.001), LVESD (r = 0.54, P , 0.001), dp/dt (r = −0.32, P = 0.019) and SPAP (r = 0.4, P = 0.006).
Conclusion: The present study showed that BNP may be useful in patients with MR and may confirm echocardiographic indices.
Keywords: mitral regurgitation, N-Terminal pro-B natriuretic peptide, echocardiographic indices.
The hypothesis assumes that there is a linear sequence of most effective screening that comes out of this study, from a b-type natriuretic peptide to the imaging. It’s not clear that that is the case, and moreover, silent myocardial infarct is taken and lumped with other serious conditions affecting the myocardium, presumably through compromise of the end-artery circulation to the heart (R, L, and circumflex coronaries). There is no mention of whether the patients were screened out for peripheral, carotid, or other associated artery disease (superior mesenteric).
I’ll assume that that is the case. I see a problem with a linear, monothetic, “gold standard” approach, when the disease and the diagnosis of it is multivariate and requires a method that uses a classificatory approach. We’ll return to that.

English: A Wiggers diagram, showing the cardiac cycle events occuring in the left ventricle. (Photo credit: Wikipedia)
[D] reference normal for NT-proBNP
ABSTRACT
Background: The natriuretic peptides, B-type natriuretic peptide (BNP) and NT-proBNP that have emerged as tools for diagnosing congestive heart failure (CHF) are affected by age and renal insufficiency (RI).This study evaluates the reference value for interpreting NT-proBNP concentrations. Increasing concentrations of NT-proBNP are associated with co-morbidities, not merely CHF, resulting in altered volume status or myocardial filling pressures.
Methods: NT-proBNP was measured in a population with normal trans-thoracic echocardiograms (TTE) and free of anemia or renal impairment.
Selection of Patients: Study participants were seen in acute care for symptoms of shortness of breath suspicious for CHF.
Results: The median NT-proBNP for patients under 50 years is 27.6 pg/ml with an upper limit of 445 pg/ml, and for patients over 50 years the median was 142.3 pg/ml with an upper limit of 475.3 pg/ml. We introduce a transformed NT-proBNP that normalizes for decrease in glomerular filtration rate and eliminates the age factor.
Conclusion: We suggest that NT-proBNP levels can be more accurately interpreted only after removal of the major co-morbidities that affect an increase in this peptide in serum. The PRIDE study guidelines should be applied until presence or absence of comorbidities is diagnosed. With no comorbidities, the reference range for normal over 50 years of age can be reduced below 800 pg/ml. The effect shown in previous papers likely is due to increasing concurrent comorbidity with age.
Key Words: Congestive Heart Failure, Natriuretic peptides, Anemia, Chronic renal insufficiency
Statistical treatment:
The combined acute and blood donor study sets were kept separate and each analyzed for central tendency, distribution and variability. The two were combined after the comorbidities described above were extracted from the acute care study group. This resulted in a population that should be representative of an unaffected study population that could be used to establish a most representative reference range. The database was replicated several times and then patient rows were randomly deleted until there was an expanded combined and mixed data set with 6,700 entries. All of the database sets were used for analyses.
The results are reported in means with p < 0.05 as the measure of significance for difference between means. Independent Student’s t-tests were applied comparing NT-proBNP and anemia. Univariate ANOVAs were used to compare NT-proBNP levels with varying ranges of hemoglobin and age using SPSS 15.0 (SPSS, Chicago, IL). A linear regression analysis with linear fitting and confidence interval was performed using SYSTAT 12 (SYSTAT, San Jose, CA). The results are reported in means with p < 0.05 as the measure of significance for difference between means. Linear regression analysis, Independent Student’s t and Mann-Whitney tests were applied comparing NT-proBNP for age intervals. Reference range was determined using MedCalc 9.2.0.0 (Mariakerke, Belgium).
We observe the following changes with respect to NT-proBNP and age:
- Sharp increase in NT-proBNP at over age 50
- Increase in NT-proBNP at 7 percent per decade over 50
- Decrease in eGFR at 4 percent per decade over 50
- Slope of NT-proBNP increase with age is related to proportion of patients with eGFR less than 90
- NT-proBNP increase can be delayed or accelerated based on disease comorbidities
Adjustment of the NT-proBNP for eGFR and for age over 50 difference
We have carried out a normalization to adjust for both eGFR and for age over 50:
- Take Log of NT-proBNP and multiply by 1000
- Divide the result by eGFR (using MDRD[9] or Cockroft Gault[10])
- Compare results for age under 50, 50-70, and over 70 years
- Adjust to age under 50 years by multiplying by 0.66 and 0.56.
GFR (mL/min/1.73 m2) = 186 x (Scr)-1.154 x (Age)-0.203 x (0.742 if female) x (1.210 if African-American) (conventional units)
The equation does not require weight because the results are reported normalized to 1.73 m2 body surface area, which is an accepted average adult surface area.
Comparison of the mean + standard deviation of 607 blood donors and NYMH inpatients for the MDRD and Cockroft Gault (eCG), respectively gave 114.3, 43.7(MDRD); 105.0, 40.1 (eCG). The eCG is predicted by the regression: eCG = 0.059 + 0.918*MDRD. The mean + standard deviation for the age under 50 years and 50 or older is 106.5 + 14.7, 100.9 + 14.5 (MDRD); and 102.5 + 18.5, 98.4 + 20.8 (eCG). These differences are significant at < 0.0001, and 0.010, respectively.
The means comparison of the normalized NT-proBNP (NKLog[NT-proBNP]/eGFR) results in 23.4 and 18.7 for 307 non-donors and 300 donors, significant at p < 0.0001, assuming unequal variance). The difference is not significant for the MDRD normalized NT-proBNP (16.5, 6.6). The normalized by eCG result for 324 under age under 50 years and 283 age 50 years and older is 17.7 versus 18.2, significant at p = 0.0001. The MDRD calculated adjustment is 16.8 vs 16.9, which is not significant. The relationship between these is NKLog(NT-proBNP)/eCG = 4.47 + 0.948*NKLog(NT-proBNP)/MDRD. Figure 4 is a plot of the regression of NKLog(NTproBNP)/MDRD vs NKLog(NTproBNP)/eCG predicted over the full study population.
The reference range for the normalized Klog(NT-proBNP)/MDRD is described by a mean 13.99, median 13.12, and standard deviation 6.14 with a nonparametric upper limit of 24.7. A ROC curve is constructed comparing the NT-proBNP, the NKLog(NTproBNP)/MDRD and the ratio NTproBNP to NKLog(NTproBNP)/MDRD in the expanded full database. The area under the curve is 0.944 (0.938-0.950) for NKLog(NTproBNP)/MDRD with a base of 571 patients with early CHF and 6115 patients without. The reference range for NKLog(proBNP)/MDRD can be referenced to the percentiles as follows: 20, 8.78; 40, 11.92; 60, 14.85; 90, 21.10; 95, 24.73; 97.5, 29.54.
Conclusion: We suggest that NT-proBNP levels can be accurately assessed only after removal of the major confounding co-morbidities that increase this peptide in serum. We established our new range after establishing absence of co-morbidities. The value of this approach for screening purposes is an allowance for a considerably lower reference normal with a higher specificity based on the donor studies and the mixture model. This study finds that the reference range for NT-proBNP is age-dependent past age 50 years, mainly as the change relates to eGFR, and we introduce an age adjusted alternative measure, the normalized NT-proBNP using the MDRD transformation described.
NT-pro BNP reference range with blood donors and patients
Measure NT-proBNP (pg/ml) After trimming extremes
Highest 1110 599.4
Arithmetic mean 179.6 118.2
Geometric mean 68.7 54.4
Median 52.6 42.6
Standard deviation 250.5 150.6
D’Agostino-Pearson P = 0.0026 P = 0.0091
97.5%
< 50 years 526.9 445.0
> 50 years 1000 565.0
Upper Limit of Normal 772.9 475.3
95% confidence interval 637.1 – 873.73 442.7 – 531.0
Bernstein LH, Zions MY, Alam ME, Haq SA, Heitner JF, et al. What is the best approximation of reference normal for NT-proBNP? Clinical Levels for Enhanced Assessment of NT-proBNP (CLEAN)
Renal Effect on NT-proBNP
NT-proBNP is excreted by the kidney. Therefore, GFR has to be taken into account in adjusting the reference range. BNP, unlike the propeptide, is eliminated 80% by vascular endothelium. What would be the effect of vascular endothelium erosion? We don’t know.
The Cockroft Gault equation is widely used in hospitals for adjusting medication doses in hospital patients. The MDRD equation was developed for patients with renal insufficiency and has been shown to be comparable to CG for the population the MDRD is applied. However, the MDRD is only reported to a CLCR of only 60 ml/min and is not validated for age over 65 years. On the other hand, the body weight and BMI, necessary for calculating the CG formula are not routinely done for all patients or in all hospitals. We used 307 inpatients and calculated the MDRD up to 100 ml/min/m2, then used the results to predict the CG. The regression for MDRD versus the CG resulted in an r = 0.884, and a regression equation: CG = -21.1 + 1.172*(MDRD). The initial prediction of CG from MDRDe from 198 of the patients is defined by the regression: CGe = -64.6 + 1.866*MDRDe. (Deming)(95% CI: Intercept -84.5 to -42.8; slope 1.40 to 2.33). The means, medians, standard deviations, and 97.5th percentiles, respectively, of the age, MDRDe and CGe (calculated from weight data) for the 307 patients are: age- 61.2, 62.0, 17.4, 91.3; MDRD – 121.5, 107.5, 55.9, 212.3; CG – 111.7, 98.7, 51.4, 195.0.
The NT-proBNP was adjusted using a log transform and the estimated GFR (glomerular filtration rate by the original method of Levey et al. The result for reference corrected Nt proBNP is shown in Table 2.
Table 2.
Kruskal-Wallis test
| Data | KLOGNTPR |
| Factor codes | MDRD60 |
| Sample size |
440 |
| Factor |
n |
Average Rank |
| 0 |
344 |
174.11 |
| 1 |
96 |
386.73 |
| Test statistic |
209.8311 |
| Corrected for ties Ht |
209.8313 |
| Degrees of Freedom (DF) |
1 |
| Significance level |
P < 0.0001 |
[E] Mid-region proANP in Emergency Room
| Mid-region pro-hormone markers for diagnosis and prognosis in acute dyspnea: results from the BACH (Biomarkers in Acute Heart Failure) trial. |
| J Am Coll Cardiol 2010 May 11;55(19):2062-76 (ISSN: 1558-3597) |
| Maisel A; Mueller C; Nowak R; Peacock WF; Landsberg JW; Ponikowski P; Mockel M; Hogan C; Wu AH; Richards M; Clopton P; Filippatos GS; Di Somma S; Anand I; Ng L; Daniels LB; Neath SX; Christenson R; Potocki M; McCord J; Terracciano G; Kremastinos D; Hartmann O; von Haehling S; Bergmann A; Morgenthaler NG; Anker SD VA San Diego Healthcare System, San Diego, California 92161, USA. amaisel@ucsd.edu. |
| OBJECTIVES: Our purpose was to assess the diagnostic utility of mid–regional pro-atrial natriuretic peptide (MR-proANP) for the diagnosis of acute heart failure (AHF) and the prognostic value of mid–regional pro-adrenomedullin (MR-proADM) in patients with AHF. BACKGROUND: There are some caveats and limitations to natriuretic peptide testing in the acute dyspneic patient. METHODS: The BACH (Biomarkers in Acute Heart Failure) trial was a prospective, 15-center, international study of 1,641 patients presenting to the emergency department with dyspnea. A noninferiority test of MR-proANP versus B-type natriuretic peptide (BNP) for diagnosis of AHF and a superiority test of MR-proADM versus BNP for 90-day survival were conducted. Other end points were exploratory. RESULTS: MR-proANP (> or =120 pmol/l) proved noninferior to BNP (> or =100 pg/ml) for the diagnosis of AHF (accuracy difference 0.9%). In tests of secondary diagnostic objectives, MR-proANP levels added to the utility of BNP levels in patients with intermediate BNP values and with obesity but not in renal insufficiency, the elderly, or patients with edema. Using cut-off values from receiver-operating characteristic analysis, the accuracy to predict 90-day survival of heart failure patients was 73% (95% confidence interval: 70% to 77%) for MR-proADM and 62% (95% confidence interval: 58% to 66%) for BNP (difference p < 0.001). In adjusted multivariable Cox regression, MR-proADM, but not BNP, carried independent prognostic value (p < 0.001). Results were consistent using NT-proBNP instead of BNP (p < 0.001). None of the biomarkers was able to predict rehospitalization or visits to the emergency department with clinical relevance. CONCLUSIONS: MR-proANP is as useful as BNP for AHF diagnosis in dyspneic patients and may provide additional clinical utility when BNP is difficult to interpret. MR-proADM identifies patients with high 90-day mortality risk and adds prognostic value to BNP. (Biomarkers in Acute Heart Failure [BACH]; NCT00537628). [Copyright 2010 American College of Cardiology Foundation. Published by Elsevier Inc. All rights reserved.]. |
| Comment In: RefSource:J Am Coll Cardiol. 2010 May 11; 55(19):2077-9/PMID:20447529 |
II. CRP
[A] Predictor of benefit of lowering CRP with statin
Sever PS, Poulter NR, Chang CL, et al; ASCOT Investigators. Evaluation of C-reactive protein prior to and on-treatment as a predictor of benefit from atorvastatin: observations from the Anglo-Scandinavian Cardiac Outcomes Trial. Eur Heart J. 2012;33:486-494
The theory that lowering the C-reactive protein (CRP) level with statin therapy is predictive of cardiovascular outcomes independent of lowering the low-density lipoprotein (LDL) cholesterol level was first advanced by the JUPITER investigators.[1]
- This study further fueled the debate on whether CRP measurement should be routine for monitoring cardiovascular disease risk. The ASCOT investigators entered this debate when they analyzed data from their trial to determine whether on-statin C-reactive protein level was associated with cardiovascular outcomes.[4]
- The data in the nested case-control study were from persons recruited to ASCOT in the United Kingdom and Ireland, 9098 of whom were randomly assigned in the blood pressure-lowering arm to receive either amlodipine with or without perindopril or atenolol with or without bendroflumethiazide.[5] Within the whole blood-pressure-lowering group, 4853 persons with a total cholesterol level of 6.5 mmol/L or less (≤ 250 mg/dL) were further randomized to receive atorvastatin or placebo as part of the lipid-lowering arm.[6]
- For the case-control study, 485 cardiovascular cases were age- and sex-matched with 1367 controls. As expected, the investigators found that baseline LDL cholesterol and CRP levels both predicted cardiovascular events.
- However, neither the baseline nor the on-treatment CRP level was related to the magnitude of statin efficacy in the prevention of cardiovascular events, whereas the on-treatment LDL cholesterol level was strongly predictive. Including CRP in the Framingham model resulted in a “modest” (2.1%) improvement in risk prediction overall.
The investigators noted that this finding was in line with other prospective studies that showed statistically significant, but modest, absolute improvements with the use of CRP in clinical risk prediction.[7,8] They concluded that “in this hypertensive population selected on the basis of traditional, common coexisting risk factors, CRP did not usefully improve the prediction of cardiovascular events and, critically, reduction in CRP associated with statin therapy was not a predictor of cardiovascular outcome alone or in combination with LDL-cholesterol.”
Eugene Braunwald downplayed the ASCOT investigators’ conclusions in observing “the ASCOT results, albeit quite limited in size, are in fact remarkably similar to those of the [CARE, AFCAPS/TexCAPS, REVERSAL, A to Z], and JUPITER trials, especially in light of the fact that the dose of atorvastatin [in ASCOT] was only 10 mg, while some of the other trials used considerably larger equivalent doses of statins.”
My own take on this is that for at least two decades, there was a belief that the LDL lowering was the main effect of statins, until the (deep frozen) specimens were reexamined from the Framingham study using a hs CRP assay. The investigation was to determine whether there is a predictor of CVD that is present when the traditional features are not present (which would have to include diabetes and hypertension). The basis for the use of hsCRP became to identify patients who had sufficient risk to be treated with a statin. The essential focus seemed to turn on whether statin treatment has efficacy in view of the differential between the LDL or the CRP on the magnitude of the effect. The muscular effect of a statin then comes into view with the size dose and length of treatment. However, the CRP measurement identified a relationship between development of the vascular disease and the inflammatory process independently of the STATIN treatment benefit.
Prof. Sever (Medscape): The key result that we found in the initial paper was that CRP, although an independent predictor of cardiovascular events in the hypertensive population, was really only a weak predictor, which is confirmed by the meta-analyses. Furthermore, when you incorporate CRP into a Framingham-style model, it really does not add any benefit or give any more information than if it had not been included in the model. LDL cholesterol is a much more important biomarker. Our second important conclusion addressed the question of whether, after starting a patient on statin therapy, the magnitude of lowering CRP by the statin and the level to which CRP has been reduced predicts cardiovascular outcome. The simple answer from our analyses was that it did not and that the benefits were all related to lowering LDL cholesterol. Our population comprised patients with stable hypertension and no history of coronary disease; likewise, the diabetes population in CARDS had no history of coronary heart disease. Oddly, PROVE IT-TIMI 22 involved persons who were selected from a high-risk coronary heart disease population simply because they had a high level of an inflammatory marker. So, to a certain extent, this is like comparing apples and oranges, and to find some unifying hypothesis on the basis of widely heterogeneous patient populations seems to be a little naive.
[B] Predictor of cardiovascular disease
Acute Phase Reactants as Novel Predictors of Cardiovascular Disease M. S. Ahmed, A. B. Jadhav, A. Hassan, and Qing H. Meng SRN Inflammation 2012; Article ID 953461, 18 pages. doi:10.5402/2012/953461
- Acute phase reaction is a systemic response which usually follows a physiological condition that takes place in the beginning of an inflammatory process.
- This physiological change usually lasts 1-2 days. However, the systemic acute phase response usually lasts longer.
- The aim of this systemic response is to restore homeostasis.
- These events are accompanied by upregulation of some proteins (positive acute phase reactants) and
- downregulation of others (negative acute phase reactants) during inflammatory reactions.
Cardiovascular diseases are accompanied by the elevation of several positive acute phase reactants such as
- C-reactive protein (CRP),
- serum amyloid A (SAA),
- fibrinogen,
- white blood cell count,
- secretory nonpancreatic phospholipase 2-II (sPLA2-II),
- ferritin, and
- ceruloplasmin.
Cardiovascular disease is also accompanied by the reduction of important transport proteins such as
- albumin, transferrin,
- transthyretin,
- retinol-binding protein,
- antithrombin, and
- transcortin.
In this paper, we will be discussing the biological activity and diagnostic and prognostic values of acute phase reactants with cardiovascular importance.
The potential therapeutic targets of these reactants will be also discussed.
.
[C] CRP as an Inflammatory Biomarker
CRP is an acute phase protein [7, 8] produced in the liver in response to interleukin- (IL-) 6 which is stimulated, in turn, by tumour necrosis factor-α (TNF-α) and IL-1 [8, 9].
Recent studies suggest that CRP plays a pivotal role in many aspects of atherogenesis including
- LDL uptake by macrophage,
- release of proinflammatory cytokines,
- expression of monocyte chemotactic protein-1,
- intercellular adhesion molecule-1, and vascular cellular adhesion molecule-1 [10–12].
Activation of inflammation and the acute phase reaction appear to play an important role, not only in the pathogenesis of atherosclerosis, but also in the initiation of the acute coronary syndrome (ACS) [13,14]. Cesari et al. suggested that the inflammatory markers CRP, IL-6, and TNF-α are independent predictors of cardiovascular events in older persons [14].
Diagnostic Value
CRP is also an early ischemic marker and elevated CRP is predictive of future adverse events [22, 23]. High-sensitivity CRP (hs-CRP) rises acutely after tissue injury, including myocardial infarction (MI). Intense cytokine production and inflammatory cell infiltration occur in the area of ischemia and necrosis. This increase of hs-CRP levels, in part, correlates with infarct size [24, 25]
CRP can be also used for patients screening in the primary prevention population [36]. Ockene et al. indicated that CRP is generally expressed at low levels (<1 mg/L) in healthy adults and levels remain relatively stable in the absence of an acute inflammatory stimulus [37].
Patients with unstable angina and CRP >3 mg/L at discharge are more likely to be readmitted for recurrent cardiovascular instability or MI within 1 year [38].
Pietilä et al. indicated that hs-CRP measurement is the strongest correlative factor for future clinical events due to arterial inflammation, myocardial infarction, unstable angina, stroke, and peripheral vascular disease in both diseased and apparently healthy asymptomatic patients [40].
The CRP plasma level also is the best risk assessment in patients with
- either stable or unstable angina,
- long term after myocardial infarction, and
- in patients undergoing revascularization therapies [41].
- One study showed the only independent cardiovascular risk indicators using multivariate, age adjusted and traditional risk analysis were CRP and Total/HDL cholesterol ratio.
- If CRP, IL-6, and ICAM-1 levels are added to lipid levels, risk assessment can be improved over lipids alone.
- Moreover, serum CRP may indicate the vulnerability of the plaque [40].
Prognostic Value
- elevation of hs-CRP levels predicts a poor cardiovascular prognosis [42].
- The extent of the inflammatory response to injury appears to have prognostic significance, which is independent of the extent of myocardial injury.
- hs-CRP response after MI has been shown to predict future CHD morbidity and mortality independent of infarct size [43].
- CRP is also a predictor of incident type 2 diabetes. As well, it adds a prognostic information on vascular risk at all levels of the metabolic syndrome [44].
__________________________________________________________________________________________________________________________
III. Troponin(s) and hs-TnI/cTnT
Comparison of diagnostic accuracy between three different rules of interpreting high sensitivity troponin T results. Francesco Buccelletti; Leonarda Galiuto; Davide Marsiliani; Paolo Iacomini; et al. Intern Emerg Med 2012; 7, 365
Abstract
With the introduction of high sensitivity troponin-T (hs-TnT) assay, clinicians face more patients with ‘positive’ results but without myocardial infarction. Repeated hs-TnT determinations are warranted to improve specificity. The aim of this study was to compare diagnostic accuracy of three different interpretation rules for two hs-TnT results taken 6 h apart. After adjusting for clinical differences, hs-TnT results were recoded according to the three rules.
- Rule1: hs-TnT >13 ng/L in at least one determination.
- Rule2: change of >20 % between the two measures.
- Rule3: change >50 % if baseline hs-TnT 14-53 ng/L and >20 % if baseline >54 ng/L.
The sensitivity, specificity and ROC curves were compared. The sensitivity analysis was used to generate post-test probability for any test result. Primary outcome was the evidence of coronary critical stenosis (CCS) on coronary angiography in patients with high-risk chest pain.
183 patients were analyzed (38.3 %) among all patients presenting with chest pain during the study period. CCS was found in 80 (43.7 %) cases.
The specificity was 0.62 (0.52-0.71), 0.76 (0.66-0.84) and 0.83 (0.74-0.89) for rules 1, 2 and 3, respectively (P < 0.01). Sensitivity decreased with increasing specificity (P < 0.01).
Overall diagnostic accuracy did not differ among the three rules (AUC curves difference P = 0.12). Sensitivity analysis showed a 25 % relative gain in predicting CCS using rule 3 compared to rule 1. Changes between two determinations of hs-TnT 6 h apart effectively improved specificity for CCS presence in high-risk chest pain patients.
There was a parallel loss in sensitivity that discouraged any use of such changes as a unique way to interpret the new hs-TnT results.
Advances in identifying NSTEMI biomarkers [Published 31 August 2012 | Article by Excerpta Medica | Tags: elderly, ami, biomarkers, diagnosis]
In the run-up to the ESC conference at the end of August, we review some recently published research on the hot topic of biomarkers for NSTEMI.
Prompt and accurate diagnosis of acute non-ST elevation myocardial infarction (NSTEMI) can be particularly challenging in elderly patients, as they often present with
- atypical symptoms and/or have an inconclusive ECG.
- the diagnostic value of cardiac troponin T (cTnT), an established marker of cardiac injury, is often limited as there is often non-coronary troponin elevation caused by concomitant conditions such as acute congestive heart failure.
- Identifying new sensitive and specific biomarkers of NSTEMI in elderly patients is therefore important, and circulating microRNAs (miRs) are emerging as good candidates.
researchers evaluated the diagnostic potential of plasma levels of various miRs in elderly patients enrolled at presentation:
- 92 acute NSTEMI patients (complicated by congestive heart failure in three-quarters of cases),
- 81 patients with acute congestive heart failure without acute MI, and
- 99 age-matched healthy people (the control group).
The researchers, from centers in Italy, found that levels of miR-1, miR-21, miR-133a, and miR-423-5p were 3-10 times higher in the patients with NSTEMI, compared with controls. Levels of miR-499-5p, meanwhile, were more than 80 times higher in the NSTEMI patients compared with the patients in the control group.
- Levels of miR-499-5p and miR-21 were also significantly higher in the NSTEMI group compared with the group of patients with acute congestive heart failure without acute MI.
- The researchers also found that miR-499-5p was similar to cTnT in being able to distinguish NSTEMI patients from the other two groups.
- Also, a subgroup analysis of patients with a modest elevation in cTnT level at presentation (0.03-0.10 ng/mL) revealed that miR-499-5p had a diagnostic accuracy superior both to cTnT and to high sensitivity cTnT in differentiating NSTEMI from acute congestive heart failure.
International Journal of Cardiology
________________________________________________________________________________________________________________________________________________________________________
IV. Predicting cardiovascular mortality in NSTEMI patients
[A] Japanese researchers studied 258 consecutive patients hospitalized for unstable angina and NSTEMI within 24 hours of the onset of chest symptoms, and followed them up for a median period of 49 months after admission. During this period there were 38 cardiovascular deaths (14.7%).
They reported that high-mobility group- box 1 (HMGB1), a nuclear protein and signaller of tissue damage, was “a potential and independent predictor of cardiovascular mortality in patients hospitalized for unstable angina and NSTEMI.
- HMGB1,
- cardiac troponin I,
- Killip class greater than 1, and
- age
were each independently and significantly associated with cardiovascular mortality.
……………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………
[B] William LaFramboise et al. BMC Med. 2012 Dec 5;10(1):157)
see Report by Aviva Lev-Ari (pharmaceuticalintelligence.com) Coronary artery disease in symptomatic patients referred for coronary angiography: Predicted by Serum Protein Profiles
Significant differences were detected in circulating proteins from patients requiring revascularization including increased apolipoprotein B100 (APO-B100), C-reactive protein (CRP), fibrinogen, vascular cell adhesion molecule 1 (VCAM-1), myeloperoxidase (MPO), resistin, osteopontin, interleukin (IL)-1beta, IL-6, IL-10 and N-terminal fragment protein precursor brain natriuretic peptide (NT-pBNP) and decreased apolipoprotein A1 (APO-A1). Biomarker classification signatures comprising up to 5 analytes were identified using a tunable scoring function trained against 239 samples and validated with 120 additional samples. A total of 14 overlapping signatures classified patients without significant coronary disease (38% to 59% specificity) while maintaining 95% sensitivity for patients requiring revascularization. Osteopontin (14 times) and resistin (10 times) were most frequently represented among these diagnostic signatures. The most efficacious protein signature in validation studies comprised osteopontin (OPN), resistin, matrix metalloproteinase 7 (MMP7) and interferon gamma (IFNgamma) as a four-marker panel while the addition of either CRP or adiponectin (ACRP-30) yielded comparable results in five protein signatures.
______________________________________________________________________________________________________________________________________________________
V. Assessing Cardiovascular Risk
Agency for Healthcare Research and Quality (AHRQ)
Assessing Cardiovascular Risk: Guideline Synthesis
Agency for Healthcare Research and Quality (AHRQ) Authors and Disclosures Posted: 03/01/2012
- Guidelines Being Compared
- Areas of Agreement and Difference
- Comparison of Recommendations: Lipoprotein and Apolipoprotein Assessments
- Comparison of Recommendations: Inflammation Markers (CRP, Fibrinogen, White Blood Cell Count, Lp-PLA2)
- Comparison of Recommendations: Homocysteine Level
- Comparison of Recommendations: IMT, ABI, and Calcium Scoring Methods
- Comparison of Recommendations: Natriuretic Peptides
- Comparison of Recommendations: Metabolic and Renal Factors
- Strength of Evidence and Recommendation Grading System
- Methodology
- Source(s) of Funding
- Benefits and Harms
- Status
…………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………..
The Third MI Definition: An Expert Interview With Joseph Alpert In the new definition, the diagnosis of acute MI remains unchanged: That is, it applies where there is evidence of myocardial necrosis in a clinical setting consistent with acute myocardial ischemia. However, the criteria for diagnosis have been updated, with an emphasis on the biomarker cardiac troponin.
- The first essential criterion for diagnosis of MI is detection of a rise or fall in cardiac troponin, or CKMB if troponin is not available, with at least 1 value above the 99th percentile upper reference limit, plus at least 1 the following criteria:
- Symptoms of ischemia;
- ECG changes of new or presumed new ischemia (significant ST-segment T-wave changes or new left bundle branch block);
- Development of pathologic Q waves on ECG; or
- Imaging evidence of new loss of viable myocardium or new regional wall-motion abnormality.Other criteria include those for MI in sudden unexpected cardiac death and for MI during percutaneous coronary intervention (PCI) and coronary artery bypass graft surgery (CABG).
The guidance document supports the use of high-sensitivity cardiac troponin assays, especially for distinguishing myocardial injury not related to myocardial ischemia, such as that associated with heart failure or renal failure. These assays are available in Europe, and not in the United States. MI is designated as ST-segment elevation MI or non- ST-segment elevation MI, and as in the 2007 version, it is classified into 5 types on the basis of pathologic, clinical, and prognostic differences. These types have been updated in the latest version.
- Type 1 MI (spontaneous MI) is related to atherosclerotic plaque rupture or other event leading to thrombus formation in ≥ 1 of the coronary arteries, leading to decreased myocardial blood flow with ensuing necrosis;
- Type 2 MI arises from a condition other than CAD;
- Type 3 MI is deemed to have occurred when cardiac death occurs with symptoms suggestive of myocardial ischemia, but without biomarker values having been obtained; and
- Type 4 and 5 MIs are related to PCI and CABG, respectively, and have been redefined since 2007.
The new document also describes situations in which troponin levels are elevated in conditions where myocardial injury with necrosis is associated with predominantly nonischemic myocardial injury, such as heart failure, renal failure, myocarditis, arrhythmias, or pulmonary embolism.
__________________________________________________________________________________________________________________________________________________________________________
VI Statistical Problems
The normal or “bell shaped” curve is a plot of numerical values along the x-axis and the frequency of the occurrence on the y-axis. If the set of measurements occurs as a random and independent event, we refer to this as parametric, and the distribution of the values is a bell shaped curve with all but 2.5% of the values included within both ends, with the mean or arithmetic average at the center, and with 67% of the sample contained within 1 standard deviation of the mean. We view a reference range in terms of a homogeneous population. This means that while all values might not be the same, the values are scattered within a distance from the mean that becomes less frequent as the distance is larger so that we can describe a mean and a 95% confidence interval around the mean. In the problem we are discussing, the classic reference value could be determined with outliers removed, and it would most likely fit to a Receiver Operator Characteristic curve. This became blurred when the high sensitivity assay was introduced, which included NOISE, which is really not noise but heterogeneous elements related to [a] vascular events that are not caused by plaque rupture, or [b] ischemia related to “piecemeal necrosis” which continued might predict a serious future event. Hidden variables include – age, diurnal variation, racial factors, and disease (hypertension, CHF, type 2 diabetes, renal failure).
A majority have no ST elevation on EKG, considered definitive for AMI. This makes the finding of elevated and increasing cardiac specific enzyme or protein in serum of paramount importance for specifying damaged cardiac muscle in a context of insufficient circulation. We examine the classification of AMI using a combination of features of chest pain, EKG, and a sensitive cardiac marker, derived from the cardiac muscle filament. An optimum value for a test cutoff is, such as cTnT, can be derived without using a prior determination of disease status. This is an alternative to first carrying out a study with a training set, and then repeating it with a validation set, provided there is sufficient information for classifying the data.. We have to construct a self-classifying table of ordered classes that have assigned measurable risks. Haberman (4) discusses the underlying assumptions used by Magidson for association models of cross-classified data in calculating the maximum likelihood estimates (MLE) by using the log-likelihood ratio and a sum of squares representing deviations of parameters from their constraints. The Latent Class Analysis (LCA) developed by Magidson and Vermunt allows use of a traditional LCA or a regression model (Statistical Innovation. Belmont, MA). . The LCA model uses the variables – chest pain, EKG, and troponin T – to classify the data and to test the underlying structure using powerful fit measures, such as L2. Chest pain has the value of “typical” or “other”. EKG has the value ST depression or any other (for a non Q-wave study). “cTnT” has the value assigned by rank in the scaling intervals. The results of such an analysis are displayed in Table 1.
Table 1. This LCA classification was constructed using the troponin T before hsTnT was available.
| CTnT (mg/L) | MI (6%) | Not MI (94%) |
| 0-0.03 | 0.0008 | 0.8485 |
| 0.031-0.055 | 0.0009 | 0.0791 |
| 0.056-0.080 | 0.0009 | 0.0369 |
| 0.081-0.099 | 0.0010 | 0.0106 |
| 0.10-0.199 | 0.2026 | 0.0238 |
| > 0.20 | 0.7939 | 0.0012 |
Eugene Rypka. Syndromic classification: A process for amplifying information using S-Clustering. Nutrition 1996; 14(12: 827-829.
Stuart W Zarich, Keith Bradley, Inder Dip Mayall, Larry H Bernstein. Minor elevations in troponin T values enhance risk assessment in emergency department patients with suspected myocardial ischemia: analysis of novel troponin T cut-off values. Clin Chim Acta 2004; 343(1-2):223-229
Haberman SJ. Computation of maximum likelihood estimates in association models. J Am Stat Assoc 1995;90:1438-1446
Rudolph RA, Bernstein LH, Babb J. Information Induction for the Diagnosis of Myocardial Infarction. Clin Chem 1988; 34: 2031-8.
Vermoent JK, and Magidson J. Latent class cluster analysis. JA Hagenaars and AL McCutcheon (eds.), Advanced Latent Class Analysis. Cambridge, Cambridge University Press, 2000.
Bernstein LH, Qamar A, McPherson C, Zarich S. Evaluating a new graphical ordinal logit method (GOLDminer) in the diagnosis of myocardial infarction utilizing clinical features and laboratory data. Yale J Biol Med 1999; 72: 259-268.
__________________________________________________________________________________________________________________________________________________________________________
VII. Conclusions I have made a number of comments to follow up on. The diagnosis of myocardial infarct has been extended as a result of the emergence of the high sensitivity troponins, but the laboratory methods have not caught up with the technology as the identification of myocardial ischemia is broken down with fine granularity in order to
- identify the high risk patients early
- and manage them effectively at the earliest stage of disease evolution
We no longer ponder over
- ECG findings of new Q-qave, not previously seen
- ST elevation
- T-wave inversion
These are an indication of plaque rupture. There are strong associations between CRP, hyperhomocysteinemia, and then add the troponins and b-type natriuretic and the pro b-type peptides. These associations have to be analyzed by “syndromic classification”, described by Eugene Rypka. The study first described found great value in the BNP and proBNP. Despite having the creatinine clearance, the NT-proBNP can’t be adequately interpreted without adjusting for the estimated glomerular filtration rate, and using a log transform for the high fold-increase with age.
There is much more to be done with capturing the information from the data we are generating. The problem of classification requires accurate data measurement, but it also requires that features in scaled data are combined in meaningful ways. That job is far from completed.
…………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………….
Below I paste all discussions on this post that are taking place on LinkedIn Group: Innovations in Cardiology:
Kathy Dowd, AuD • I am an audiologist representing the Academy of Doctors of Audiology for an initiative of early identification of hearing loss in adults with chronic diseases, including cardiovascular disease, thyroid disease, diabetes, etc. I am working on a new product that will automatically screen hearing of patients with these conditions and route them to audiologists for evaluation, treatment and counseling. Hearing loss is unidentified for most adults for 7-10. The psychological impact of hearing loss includes depression, isolation, confusion and poor job performance. We are focused on educating healthcare professionals on the need to identify this ‘silent epidemic’ as a co morbidity with most major illnesses.
Aviva Lev-Ari, PhD, RN • Dr. William LaFramboise
Thank you for your comment above and the reference to your most recent publication. It is very helpful. We are on the same page on this topic.
May I bring to the attention of the readers three sources which are shading additional light on that matter.
To Stent or Not? A Critical Decision
Obstructive coronary artery disease diagnosed by RNA levels of 23 genes – CardioDx heart disease test wins Medicare coverage
Follow William
William LaFramboise • Thank you Aviva. The CardioDx approach is promising with heavy commercial support for use in a primary care practitioner’s office. However, RNA acquisition, purification and qRT-PCR expression analysis takes 2-3 days, is performed off-site, derives from a small subset of circulating inflammatory cells and is not yet directly correlated with functional proteomics. So its value in the Emergency Room and Chest Clinic is currently limited. The proteomics test we published revealed systemic serum changes in a small number of proteins known to be involved in atherosclerosis. It has a faster turnaround time (minutes to hours) that could be implemented in an emergency room or chest clinic. We are predominantly interested in using our test to “rule out” symptomatic patients who currently undergo coronary angiography but do NOT have clinically significant CAD. Our goal is to eliminate unecessary catheterizations while catching all patients that should undergo coronary angiography with a high probability of percutaneous intervention. Currently, the patients we are targeting all undergo catheterization; our test will hopefully allow us to identify at least some of these patients who do not have CAD and eliminate this expensive and risky procedure. However, we are in the pioneering stages of developing our test so there are miles to go before we establish and validate clinical efficacy.
Larry
Larry Bernstein • What you have indicated is practical proteomics. There is more to be done in line with what Dr Lev-Ari has indicated based on additional voluminous literature. What you have done with a not so large data set, and probably underpowered looks very interesting.
I f you were willing to share the data, now that it is publihed, I think that we can sharpen the results using a method of “identifying anomalies”, and even come up with estimated probabilities for meaningful classes. I think that the best you can get is defined by Kullback-Liebler distance.
Larry H Bernstein, MD
larry.bernstein@gmail.com
Biomarker classification signatures comprising up to 5 analytes were identified using a tunable scoring function trained against 239 samples and validated with 120 additional samples. A total of 14 overlapping signatures classified patients without significant coronary disease (38% to 59% specificity) while maintaining 95% sensitivity for patients requiring revascularization. Osteopontin (14 times) and resistin (10 times) were most frequently represented among these diagnostic signatures. The most efficacious protein signature in validation studies comprised osteopontin (OPN), resistin, matrix metalloproteinase 7 (MMP7) and interferon gamma (IFNgamma) as a four-marker panel while the addition of either CRP or adiponectin (ACRP-30) yielded comparable results in five protein signatures.
Proteins in the serum of CAD patients predominantly reflected (1) a positive acute phase, inflammatory response and (2) alterations in lipid metabolism, transport, peroxidation and accumulation.
Follow William
William LaFramboise • Our study (http://www.ncbi.nlm.nih.gov/pubmed/23216991) comprised discovery research using targeted immunochemical screening of retrospective patient samples using both Luminex and Aushon platforms as opposed to shotgun proteomics. Hence the costs constrained sample numbers. Nevertheless, our ability to predict outcome substantially exceeded available methods:
DISCUSSION
The Framingham CHD scores were statistically different between groups (P <0.001, unpaired Student’s t test) but they classified only 16% of the subjects without significant CAD (10 of 63) at a 95% sensitivity for patients with CAD. In contrast, our algorithm incorporating serum values for OPN, RES, CRP, MMP7 and IFNγ identified 63% of the subjects without significant CAD (40 of 63) at 95% sensitivity for patients with CAD. Thus, our multiplex serum protein classifier correctly identified four times as many patients as the Framingham index.
The addition of clinical variables to our scoring system should improve the acuity of our test as we move into the next phase. I appreciate your input and will contact you directly for further insights
Larry Bernstein • Bill La Fram..
our algorithm incorporating serum values for OPN, RES, CRP, MMP7 and IFNγ identified 63% of the subjects without significant CAD (40 of 63) at 95% sensitivity for patients with CAD
I think you can improve the algorithm with strong clinical features. The Goldman algorithm is stronger than the Framingham Index. Maybe its because the FI is epidemiological and is a measure of long term risk being present and does not indicate significant features at the time of presenting. The best features of the Goldman algorithm (without lab work) are – ECG (which may be arguable with NSEMI), but the presence of Afib or tachyarrhythmia could be added to that in weighting, and radiation actually should include symptoms of gall bladder (vagal nerve branch), and onset, characteristic and duration of pain, and SOB.
In your algorithm there isn’t any assessment of the hypercoagulable state, blood flow or Viscosity. There is a strong relationship between hyperhomocysteinemia and CVD, and the HHCys has ties to impaired methyl group transfers that maybe proinflammatory through more than one interaction: countering eNOS, related to Lp(a), un unknown relationship to iNOS (which becomes a counterpoise to eNOS), an effect on blood flow and viscosity, and a relationship to platelet aggregation.
Lp(a) was originally considered of less weight, except that it occurred in thin people from Asian Indian descent. The relationship to apo(B) and to dense LDL particles is now a factor. Sam Filligane uses Lp(a) in his ambulatory practice, and he also uses the PLAC test that Aviva has posted on.
The biggest problem we have is the amount of variability in the data physicians use. It makes metaanalysis a poor solution to the problem. The standardization of laboratory “panels” set up after CLIA 88 puts a real burden on the physician for unsubstantiated “cost benefits” in the light of today’s knowledge.
…………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………………….
Related articles
- Innovative Scientific Team Increases Cardiac Biomarker Product line For Cardiovascular Disease Management (virtual-strategy.com)
- Endothelial Function and Cardiovascular Disease (pharmaceuticalintelligence.com)
- Should You Take an Aspirin a Day? (everydayhealth.com)
- Exercise protects against heart failure even at advanced ages (medicalxpress.com)
- Modest Elevation in BNP in Asymptomatic Hypertensive Patients Reflects Sub-Clinical Cardiac Remodeling, Inflammation and Extracellular Matrix Changes (plosone.org)
- Chronic Activation of the G Protein-Coupled Receptor 30 with Agonist G-1 Attenuates Heart Failure (plosone.org)
- Nutrition supplements that help myocardial infarction (foodconsumer.org)
- Effects of a Novel Bradykinin B1 Receptor Antagonist and Angiotensin II Receptor Blockade on Experimental Myocardial Infarction in Rats (plosone.org)
- Altered Gene Expression Pattern in Peripheral Blood Mononuclear Cells in Patients with Acute Myocardial Infarction (plosone.org)
- Telomere Length Variation in Juvenile Acute Myocardial Infarction (plosone.org)
- 15 Novel Risk Loci for Coronary Artery Disease: found by International Consortium
- CABG or PCI: Patients with Diabetes – CABG Rein Supreme
- Cardiovascular Risk Inflammatory Marker: Risk Assessment for Coronary Heart Disease and Ischemic Stroke – Atherosclerosis.
- Artherogenesis: Predictor of CVD – the Smaller and Denser LDL Particles
- Recent Patents on Biomarkers
Other related articles on Assessing Cardiovascular Disease with Biomarkers published on this Open Access Online Scientific Journal, include the following:
Dr. Lev-Ari’s research on Assessing Cardiovascular Disease with Biomarkers includes
- Biomarkers in vascular biology,
- Biomarkers in molecular cardiology and
- circulating Endothelial Progenitor Cells (cEPCs) as a Biomarker for cardiovascular marcovascular disease risk
Lev-Ari, A., (2012U). Cardiovascular Outcomes: Function of circulating Endothelial Progenitor Cells (cEPCs): Exploring Pharmaco-therapy targeted at Endogenous Augmentation of cEPCs
Lev-Ari, A., (2012T). Endothelial Dysfunction, Diminished Availability of cEPCs, Increasing CVD Risk for Macrovascular Disease – Therapeutic Potential of cEPCs
Lev-Ari, A., (2012S). Vascular Medicine and Biology: CLASSIFICATION OF FAST ACTING THERAPY FOR PATIENTS AT HIGH RISK FOR MACROVASCULAR EVENTS Macrovascular Disease – Therapeutic Potential of cEPCs
Lev-Ari, A. (2012a). Resident-cell-based Therapy in Human Ischaemic Heart Disease: Evolution in the PROMISE of Thymosin beta4 for Cardiac Repair
http://pharmaceuticalintelligence.com/2012/04/30/93/
Lev-Ari, A. (2012b). Triple Antihypertensive Combination Therapy Significantly Lowers Blood Pressure in Hard-to-Treat Patients with Hypertension and Diabetes
http://pharmaceuticalintelligence.com/2012/05/29/445/
Lev-Ari, A. (2012h). Macrovascular Disease – Therapeutic Potential of cEPCs: Reduction Methods for CV Risk
Lev-Ari, A. (2012xx). Coronary artery disease in symptomatic patients referred for coronary angiography: Predicted by Serum Protein Profiles
Lev-Ari, A. (2013a) forthcoming, based on:
Part III: (2006c) Biomarker for Therapeutic Targets of Cardiovascular Risk Reduction by cEPCs Endogenous Augmentation using New Combination Drug Therapy of Three Drug Classes and Several Drug Indications. Northeastern University, Boston, MA 02115
Special Considerations in Blood Lipoproteins, Viscosity, Assessment and Treatment Larry Bernstein
New Insights on Nitric Oxide donors – Part IV Larry Bernstein
The Essential Role of Nitric Oxide and Therapeutic NO Donor Targets in Renal Pharmacotherapy Larry Bernstein
A second look at the transthyretin nutrition inflammatory conundrum Larry Bernstein
What is the role of plasma viscosity in hemostasis and vascular disease risk? Larry Bernstein
Biochemistry of the Coagulation Cascade and Platelet Aggregation – Part I Larry Bernstein
Laboratory, Innovative Technology, Therapeutics Larry Bernstein
Ubiquinin-Proteosome pathway, autophagy, the mitochondrion, proteolysis and cell apoptosis Larry Bernstein
Overview of new strategy for treatment of T2DM: SGLT2 inhibiting oral antidiabetic agents aviralvatsa
Mitochondrial dynamics and cardiovascular diseases ritusaxena
Nitric Oxide and it’s impact on Cardiothoracic Surgery tildabarliya
Telling NO to Cardiac Risk sjwilliamspa