Aortic Valve Transplant Via Carotid Artery at Hadassah – An Israel First
Curator and Reporter: Aviva Lev-Ari, PhD, RN
The transplant using the carotid artery as the point of entry was selected. The technique of trans-carotid access, Dr. Planer, Director of Hadassah’s Catheterization Department says, “is not performed in “the majority of medical centers worldwide.”
The Medical Case
A 76-year-old man with a history of critical stenosis of his aortic valve arrived at Hadassah Hospital Ein Kerem in severe cardiac shock. It was clear he needed a valve transplant urgently, but the traditional surgical options were not suitable for him because he also had severe vascular disease, anatomical limitations and had undergone previous heart bypass surgery.
Dr. Planer explains, “Until two decades ago, patients who required an aortic valve replacement had to have surgery that involved opening the chest. The recovery was long and difficult.”
This procedure, says Dr. Planer, “is performed using a hybrid approach, with catheterization specialists and cardiac surgeons.” Using this collaborative approach, Dr. Planer, Dr. Gabby Elbaz-Greener, senior catheterization specialist and head of the Structural Heart Intervention Program; Dr. Amit Korach, senior cardiac surgeon; Prof. Ronen Beeri, director of the Echocardiography Unit and senior anesthesiologist; and Dr. Tamer Abu Jreis, anesthesiology resident, successfully replaced the valve.
“Beyond choosing the right patient and the high technical capacity of the team, in a procedure such as this, it is of utmost importance for us to work harmoniously, despite coming from different disciplines,” says Dr. Planer. “Thankfully, the operation went smoothly and without complications. We are proud to be the first team in Israel to carry it out and pave the way for an additional therapeutic option for these seriously ill patients. Our patient has now been discharged to begin rehabilitation, and we wish him a full recovery.”
Transcarotid Compared With Other Alternative Access Routes for Transcatheter Aortic Valve Replacement
Originally published16 Nov 2018
https://doi.org/10.1161/CIRCINTERVENTIONS.118.006388 Circulation: Cardiovascular Interventions. 2018;11:e006388Abstract
Background
The optimal access for patients undergoing transcatheter aortic valve replacement (TAVR) who are not candidates for a transfemoral approach has not been elucidated. The purpose of this study was to compare the safety, feasibility, and early clinical outcomes of transcarotid TAVR compared with thoracic approaches.
Methods and Results
From a multicenter consecutive cohort of 329 alternative-access TAVR patients (2012–2017), we identified 101 patients who underwent transcarotid TAVR and 228 patients who underwent a transapical or transaortic TAVR. Preprocedural success and 30-day clinical outcomes were compared using multivariable propensity score analysis to account for between-group differences in baseline characteristics. All transcarotid cases were performed under general anesthesia, mainly using the left common carotid artery (97%). Propensity-matched groups had similar rates of 30-day all-cause mortality (2.1% versus 4.6%; P=0.37), stroke (2.1% versus 3.5%; P=0.67; transcarotid versus transapical/transaortic, respectively), new pacemaker implantation, and major vascular complications. Transcarotid TAVR was associated with significantly less new-onset atrial fibrillation (3.2% versus 19.0%; P=0.002), major or life-threatening bleeding (4.3% versus 19.9%; P=0.002), acute kidney injury (none versus 12.1%; P=0.002), and shorter median length of hospital stay (6 versus 8 days; P<0.001).
Conclusions
Transcarotid vascular access for TAVR is safe and feasible and is associated with encouraging short-term clinical outcomes. Our data suggest a clinical benefit of transcarotid TAVR with respect to atrial fibrillation, major bleeding, acute kidney injury, and length of stay compared with the more invasive transapical or transaortic strategies. Randomized studies are required to ascertain whether transcarotid TAVR yields equivalent results to other alternative vascular access routes.
Discussion
This is the first report of a multicenter propensity score-matched comparison between transcarotid and transthoracic access. The main findings are (1) transcarotid TAVR is safe and feasible in appropriately selected patients with a high rate of device success (87%); (2) compared with transapical and transaortic TAVR, the transcarotid approach was associated with no significant difference in rates of 30-day all-cause mortality, stroke, new pacemaker implantation, major vascular complications, and hemodynamic performance; (3) transcarotid TAVR is associated with significantly less new-onset atrial fibrillation, acute kidney injury, major or life-threatening bleeding, and shorter hospital stay.
TAVR technology has evolved considerably in the last few years allowing for the treatment of 85% to 90% of patients via the transfemoral route.4,15,16 Until recently, the transapical and transaortic approaches were considered the main alternative nontransfemoral routes, with comparable short- and long-term outcomes.17–19 Despite their advantage of simplifying valve positioning, major surgical manipulation of the chest wall is required. Furthermore, these techniques are limited by relative contraindications, such as significant respiratory failure in case of transapical, and porcelain aorta, as well as previous heart surgery, in cases of transaortic. Transcarotid TAVR was first performed in France in 2009,20 and then was subsequently adopted by several other centers.7–9,21,22 These experiences demonstrated that the surgical approach to the carotid artery is safe and relatively uncomplicated because of its superficial location, and operative experience with the carotid arteries is widespread among cardiovascular surgeons. We prefer performing transcarotid TAVR using the left common carotid because it allows superior coaxial alignment of the THV with the aortic annulus, although both sides can be used.9,10,21
In the current study, the 30-day crude stroke or TIA rate in the transcarotid group was 3% (2 disabling and 1 nondisabling stroke), with no significant difference compared with the transapical/transaortic group (as previously described in smaller studies).10,11 This stroke rate is lower than that observed in the cohort of patients included in the multicenter French Transcarotid TAVR Registry and others.8,9 As previously described,8,21 these neurological events are not always localized ipsilateral to the CCA used for TAVR. This suggests that there are other phenomena at play in addition to carotid arterial manipulation, such as new-onset postprocedural atrial fibrillation, periprocedural hypotension, inadequate contralateral carotid perfusion, and the THV deployment itself. Although the rates of preimplant and postimplant balloon valvuloplasty were significantly higher in the transapical/transaortic group even after adjustment, this did not translate to a higher risk of stroke or TIA among the transapical/transaortic patients. The low rate of stroke observed in this study may be attributed to careful patient selection and the intraoperative assessment of the functional integrity of the circle of Willis as used in one center in this study, using indirect methods, such as backflow blood pressure during carotid clamping and cerebral oximetry monitoring.7 However, the optimal preprocedural evaluation and periprocedural neurological monitoring during transcarotid TAVR are yet to be determined. Also, the optimal antithrombotic regimen and the role of embolic protection devices23–25 require further study to determine efficacy in the reduction of the risk of cerebral ischemia, specifically in patients undergoing transcarotid TAVR as literature is scarce in these patients.
Other major findings of this study were that transcarotid TAVR was significantly associated with a reduction in major or life-threatening bleeding and shorter LOS, compared with transapical/transaortic TAVR. This could be explained by (1) less-invasive access site exposure in the case of transcarotid TAVR compared with a minithoracotomy or hemisternotomy in the transapical/transaortic approach; (2) less ventilator use and shorter intensive care unit stay in transcarotid TAVR10; and (3) less pain during the postprocedural recovery and earlier patient mobilization. The lower incidence of new-onset atrial fibrillation among transcarotid TAVR patients may also partly explain shorter LOS. Any incision of the thoracic cavity is associated with various forms of supraventricular arrhythmia, most commonly atrial fibrillation, which may then translate to a prolonged hospital stay.26,27 A reduction of LOS is a critical component of current strategies to control overall costs associated with TAVR and may be the primary driver of reduced expenditure associated with transfemoral TAVR compared with alternative-access TAVR.28–30 Furthermore, severe bleeding may be associated with postprocedural hypovolemia and may explain, in part, the reduction in the rates of severe acute kidney injury in transcarotid cases compared with the transapical/transaortic approach.31,32 Similar findings were previously reported when comparing transapical or transaortic with transfemoral access. Blackstone et al33 reported their results in 501 propensity score-matched patients undergoing transapical versus transfemoral TAVR. More patients in the transapical group experienced adverse procedural events, longer length of stay, slower recovery, and higher transfusion rates. Similar results were published by Arai et al,34 who reported significantly higher rates of life-threatening bleeding when comparing transaortic (n=289) with transfemoral TAVR (n=467; 6% versus 3%, respectively; P=0.021) without a significant difference in other major outcomes. Our data also suggest that the risk of major vascular complications are decreased with a transcarotid TAVR approach (matched analysis, 3.2% versus 10.7%; P=0.05), although the study was underpowered for this specific end point and did not reach statistical significance.
Postoperative echocardiographic data showed favorable results in both groups, as either access provides direct aortic annular access and may allow superior positioning in particular anatomies (Figure). The observed 30-day mortality in the adjusted analysis (2.1% versus 4.6%; P=0.37; transcarotid versus transapical/transaortic, respectively) was also statistically comparable between groups and lower than that previously reported in transcarotid TAVR cohorts.8,9
Study Limitations
This report consists of a retrospective analysis of prospectively acquired data and is subject to the limitations inherent in this study design. Selection of patients was not random and may not be generalizable to other centers. Other alternative approaches, such as the subclavian route, were not evaluated because of the limited number of patients undergoing TAVR by subclavian access at the participating centers. The superficial position of the carotid artery coupled with the more complex exposure of the subclavian and its proximity to the brachial plexus, and the risks associated with its use if an ipsilateral internal mammary artery was used as a coronary bypass graft, have lead us to favor transcarotid over the subclavian approach. As well, specific end points, such as mortality, stroke, and major vascular complications, may have not reached statistical significance because of the small sample size and short-term follow-up. However, this is the largest multicenter study evaluating the transcarotid approach using a risk-adjusted comparator arm. Small numbers did not permit us to ascertain device-specific outcomes. However, adjusting the analysis for type of THV, we found that the association between decreased major bleeding and the transcarotid approach was modulated, in part, by the use of newer valve types with their lower profile delivery systems but was not entirely explained by this feature of the newer THVs (Appendix in the Data Supplement). Taken further, this association may also be access site specific and not entirely device specific. Accessing proximal high-pressure structures, such the left ventricular apex and ascending aorta, may be associated with less ability to adequately control bleeding compared with distal arterial sites, such as the carotid artery. Device-specific features of the newer TAVR prostheses, such as improved sealing skirts, did not influence postprocedural aortic regurgitation, need for a permanent pacemaker, pressure gradients, and overall procedural success rates in our study, which were similar between the transcarotid and transapical/transaortic groups.
Periprocedural cerebral monitoring was variable among institutions during transcarotid TAVR, reflecting a lack of consensus in the literature, and the rates of neurological events may have been underestimated because systematic evaluation by magnetic resonance imaging was not routinely performed following TAVR. However, the incidence of stroke/TIA was low and did not differ among centers (Table VII in the Data Supplement); the optimal perioperative neuromonitoring technique remains to be prospectively elucidated. However, all clinically significant neurological changes were identified, and all sites had a low-threshold trigger for consultation by a neurologist and the performance of neuroimaging post-TAVR. Preprocedural and postprocedural antiplatelet and anticoagulation therapy were not consistently captured across the study centers, which may confound the association between the approaches studied and outcomes, such as bleeding, cerebrovascular events, and mortality. However, all centers stopped the second antiplatelet agent at least 48 hours before the procedure for patients undergoing transapical or transaortic TAVR. We, therefore, cannot attribute the increased bleeding rates associated with transapical/transaortic solely to preoperative double antiplatelet therapy.
Conclusions
Transcarotid vascular access for TAVR is safe, feasible, and associated with encouraging short-term clinical outcomes in terms of mortality, stroke, and major vascular complications in patients who are not candidates to transfemoral TAVR. Furthermore, the transcarotid approach was associated with lower rates of major or life-threatening bleeding, new-onset atrial fibrillation, acute kidney injury, and shorter LOS compared with transapical or transaortic access. Larger prospective studies with longer follow-up are needed to confirm the safety and clinical efficacy of transcarotid TAVR compared with alternative approaches.
SOURCE
https://www.ahajournals.org/doi/10.1161/CIRCINTERVENTIONS.118.006388
Editorial
Transcatheter Aortic Valve Replacement via the Transcarotid Access
See Editorial by Chamandi et al
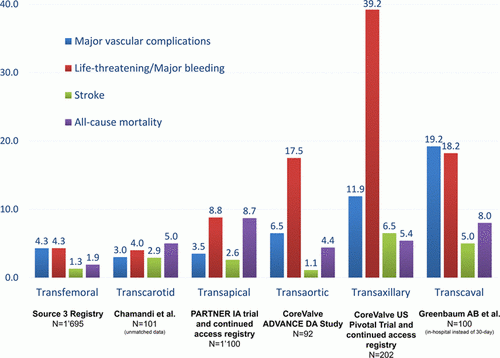
Figure. Comparative 30-day/in-hospital outcomes of different access routes for transcatheter aortic valve replacement ( TAVR) according to the VARC definitions.
SOURCE
https://www.ahajournals.org/doi/10.1161/CIRCINTERVENTIONS.118.007459
Other related articles published in this Open Access Online Scientific Journal Include:
90 articles on TAVR and TAVI
https://pharmaceuticalintelligence.com/?s=TAVR
Volume Six: Interventional Cardiology for Disease Diagnosis and Cardiac Surgery for Condition Treatment. On com since 12/24/2018 https://lnkd.in/e_CTb4R

Leave a Reply