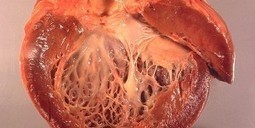
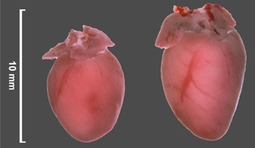
See on Scoop.it – Cardiovascular Disease: PHARMACO-THERAPY
This is one of those “good news, but” medical stories.
New treatments for heart failure have made it much less likely that people with this chronic condition will die suddenly.
But an analysis by researchers at UCLA finds that the death rate for people with advanced heart failure remains stubbornly high, with 30 percent of people dying within three years.
“They’re not dying suddenly, but their disease is still progressing,” says Dr. Tamara Horwich, an assistant professor of medicine at UCLA and a co-author of the study, which was published inCirculation Heart Failure.
Still, that’s a lot better than 50 years ago, when heart failure patients were pretty much sent home to die. Heart failure has many causes, including heart attack, diabetes, high blood pressure and viral infections. But the effect is the same: a heart that doesn’t move blood effectively.
About 6 million people in the United States have heart failure, according to the Centers for Disease Control and Prevention, and is the primary cause of 55,000 deaths a year.
In the past 20 years, medical care for heart failure has changed radically, with new medications and devices. Horwich and her colleagues wanted to see if these advances were helping patients in the real world.
The people in this study were referred the UCLA center in their early 50s, on average; this is not a disease just for the old. The study looked at 2,500 patients who had been treated at UCLA from 1993 to 2010.
They found that three drugs — ACE inhibitors, beta blockers, and aldosterone antagonists — had been widely adopted for treatment of heart failure between 1993 and 2010. At the same time, the number of people with implanted automatic heart defibrillators went from 11 percent to 68 percent. The implanted defibrillators correct abnormal heart rhythms, a big cause of sudden death.
Death rates were 42 percent lower for patients in the most recent treatment group, between 2005 and 2010, than for the patients in the 1990s. That was largely due to a drop in sudden cardiac deaths.
But deaths from progressive heart failure remained high, with 31 percent of patients dying in the latter part of the study, compared to 36 percent in the 1990s. People could be coming to UCLA sicker than in years past, Horvich speculates, having survived heart attacks and other problems that would have killed them in the past.
But it could also be because those people are ending up on implantable ventricular assist pumps or getting heart transplants, very expensive treatments that are difficult for many people to tolerate.
“We’re not curing the disease,” Horvich tells Shots. “We’re delaying the inevitable.” And that means, she says, that “we still have a lot of hard work ahead of us” in finding ways to prevent and treat heart failure.
See on www.npr.org
Like this:
Like Loading...